Is There A Timeline For Psoriasis Remission
Psoriasis is unpredictable, and psoriasis remission has no timeline. Sometimes, remission can be lengthy. You may not experience symptoms for months, even years. Remission can also be short-lived. You may start experiencing symptoms again within a few weeks of them disappearing.
One common psoriasis cycle involves having fewer symptoms and flares during summer months and more symptoms and flares during winter months. Thats likely because of how the two very different environments affect your skin. The weather in these two seasons can trigger psoriasis symptoms. Being aware of these triggers and others can help you reduce flare frequency and extend remission periods.
Although psoriasis may return on its own, something may prod its return. These things are called triggers. Being aware of the most common ones can help you reduce the likelihood of flares and possibly extend periods of remission.
Effective Treatments Can Clear The Way For Remission
Often, psoriasis remission may follow a successful course of treatment. Again, treatment plans and the results you might see will vary widely because each case of psoriasis is different. Recommended treatments also often must be tailored according to skin tone. Darker skin tends to produce thicker lesions and may respond better to treatments specifically made for those symptoms.
Some treatments that have been effective at helping to reduce or control symptoms for many people include:
- Topical medications. Corticosteroid ointments and creams are the topical treatments most often prescribed for mild to moderate psoriasis symptoms. Other topical treatments include salicylic acid and lab-made forms of vitamin D.
- Oral or injected medications. Steroids, retinoids, methotrexate, , and biologics are among the most commonly prescribed psoriasis medications taken by mouth or by injections. Retinoids can also come as a gel or cream.
- Light therapy. Some form of light therapy — which could mean sunlight or some type of UVB light exposure — is often included in a treatment plan for moderate to severe cases of psoriasis. If the UVB exposure doesnât work, some doctors will prescribe oral psoralen and brief UVA exposure. This treatment is called PUVA.
Some people with psoriasis also report getting relief of symptoms by using alternative therapies, such as essential oils, fish oil supplements, or aloe vera cream.
What To Discuss With Your Dermatologist
Be sure to tell your dermatologist if you:
-
Experience any health problem, even if it seems unrelated to taking methotrexate, such as fever, chills, body aches, bleeding, or bruising easily
-
Become pregnant
-
Feel uncertain about how to take methotrexate
-
Think the information that came with the medicine about how to take methotrexate differs from what your dermatologist told you
Images
Cordoro KM. Management of childhood psoriasis. Adv Dermatol. 2008 24:125-69.
Feldman SR. Treatment of psoriasis. UpToDate 2015 Jul, Wolters Kluwer Health. Last accessed November 2015.
Hugh J, Van Voorhees AS, et al. From the Medical Board of the National Psoriasis Foundation: The risk of cardiovascular disease in individuals with psoriasis and the potential impact of current therapies. J Am Acad Dermatol. 2014 70:168-77.
Menter A, Korman NJ, et al. Guidelines of care for the management of psoriasis and psoriatic arthritis Section 4. Guidelines of care for the management and treatment of psoriasis with traditional systemic agents. J Am Acad Dermatol2009 61:451-85.
All content solely developed by the American Academy of Dermatology
The American Academy of Dermatology gratefully acknowledges the support from Bristol Myers Squibb.
Read Also: Home Phototherapy Unit For Psoriasis
What Is Psoriatic Arthritis
Psoriatic arthritis is a type of autoimmune arthritis associated with joint and skin inflammation. PsA affects joints and surrounding structures. It can cause inflammation where tendons and ligaments attach to bone , inflammation of toes or fingers , inflammation of the peripheral joint lining , and inflammation of the spine .
PsA also affects the nails, causing pitting . PsA is usually connected to psoriasis, a condition where skin cells build and form scales and dry, itchy patches. These symptoms help to distinguish it from other types of inflammatory arthritis, such as rheumatoid arthritis , another autoimmune disease in which an overactive immune system mistakenly attacks the joints and, in severe cases, the organs.
According to data from the Cleveland Clinic, PsA prevalence varies from 0.3% to 1%, and people with pre-existing psoriasis have the highest risk for developing PsA. It is often diagnosed in middle age but anyone of any age can develop PsA. Women and men are equally affected, and people of Northern European descent have an increased risk. Genetics also play a role, especially family history of PsA or psoriasis.
Early diagnosis and treatment are vital for relieving pain and inflammation, preventing progressive joint involvement and damage, and increasing the possibility of disease remission.
What Is Psoriasis Symptoms Causes Diagnosis Treatment And Prevention
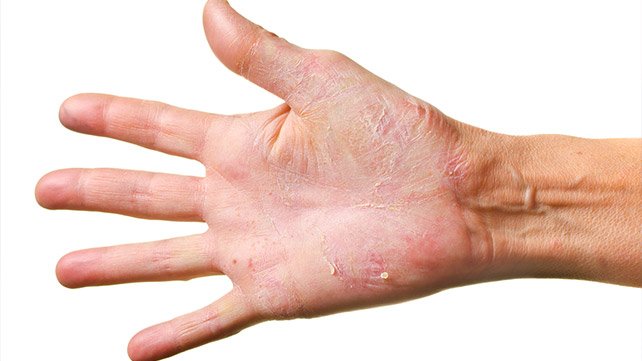
Psoriasis is an autoimmune disease that causes plaques, which are itchy or sore patches of thick, dry, discolored skin.
While any part of your body can be affected, psoriasis plaques most often develop on the elbows, knees, scalp, back, face, palms, and feet.
Like other autoinflammatory diseases, psoriasis occurs when your immune system which normally attacks infectious germs begins to attack healthy cells instead.
You May Like: When Do You Develop Psoriasis
Can Psoriasis Be Treated
Yes, there are many forms of treatment for psoriasis, which range from those you apply to the skin to tablets, and more recently injectable therapies, See Treatments for Psoriasis.
Many people who have psoriasis find that the sun and artificial ultraviolet light helps to improve their skins appearance. For some the change is dramatic. Be aware that exposure to the sun and artificial UV therapy can cause damage to the skin. See Psoriasis and the sun and Psoriasis and phototherapy
For some people, talking therapies such as cognitive behaviour therapy can also help them understand the psychological impact of psoriasis and provide a safe therapy which may help them cope with psoriasis. See our free online CBT programme
Your general practitioner or dermatologist will be best placed to advise you and keep you informed of all current and new treatments available and to recommend the best treatment programme for you personally.
Remember: Your treatment can only be as good as you allow it to be – that means if the treatment takes six weeks, you have to follow it as instructed for six weeks and no ducking out! Adherence to treatment instructions is an essential part of managing your psoriasis.
How To Achieve Remission In Psoriatic Arthritis
Learn how to work with your doctor to treat your psoriatic arthritis with medication to get it under control and keep it that way.
Getting psoriatic arthritis under control and achieving remission is possible with currently available medications.
Psoriatic arthritis is a form of inflammatory arthritis that affects both skin and joints. It is treated with conventional disease-modifying antirheumatic drugs and biologics. In some cases, these medications can lead to a near disappearance of symptoms, prompting patients to wonder if they still need to take them. But remission does not equal cure.
How Can I Reach Remission?
Some people may have a very mild form of PsA and get it under control relatively quickly, whereas others may have very severe disease and have to try several medications and combinations of medications to find relief. There are no clear criteria for defining remission in PsA, so it is difficult to say when you have gotten there. In general, rheumatologists talk about getting to a minimal disease activity state.
One of the best ways to help achieve low disease activity is through close collaboration with your rheumatologist. After the initial period they will re-evaluate your symptoms, examine your laboratory findings and then adjust the medication as needed. If youre not responding adequately, your doctor may change or increase the dose of your medication.
Treat-to-Target Strategy
Can I Stop My PsA Medication When I Feel Better?
Hello,
Don’t Miss: Best Remedy For Scalp Psoriasis
Psoriasis Beyond The Basics
There are many different types of psoriasis, including chronic plaque psoriasis, types of pustular psoriasis , guttate psoriasis, scalp psoriasis, flexural psoriasis, napkin psoriasis, nail psoriasis and erythrodermic psoriasis .
For those that have psoriasis around 1 in 4 may develop an associated psoriatic arthritis , which is about 325,000 people, or around 0.5% of the UK population. PsA causes pain and swelling in the joints and tendons, accompanied by stiffness particularly in the mornings. The most commonly affected sites are the hands, feet, lower back, neck and knees, with movement in these areas becoming severely limited.
Not all people will be affected in the same way and doctors will class the condition as mild, moderate or severe.
Remember, although psoriasis is a chronic condition, it can be controlled and go into remission .
The Fallout Of A Psa Flare
No one really knows why PsA symptoms can come and gobut experts say that inflammation rears its ugly head when the immune system mistakenly attacks healthy cells and tissues in the joints and skin. include skin trauma or injury, stress, alcohol, excess weight, smoking, and common infections that can all cause a surge in immune system activity.
The degree of inflammation one has determines how long a flare can last,” explains Minna J. Kohler, M.D., director of the Rheumatology Musculoskeletal Ultrasound Program at Massachusetts General Hospital and Harvard Medical School in Cambridge, MA. “The length of a flare related to PsA can vary from days to weeks.
If a flare remains uncontrolled, it can eventually translate into permanent damage to the joints and soft tissues, leading to bone loss, cartilage damage, and tendon tears. Eye inflammation, known as uveitis, can present, or be worsened, by a flare.
Adequate, early treatment of inflammation should be a goal in treatment of PsA to prevent permanent joint and tendon damage, Dr. Kohler advises.
Read Also: Best Treatment For Psoriasis And Psoriatic Arthritis
What Medications Or Treatments Are Used
Your healthcare provider may prescribe or recommend the following to help relieve your symptoms:
- Calcipotriene skin ointment. Calcipotriene is a form of vitamin D that helps reduce discoloration.
- Corticosteroid creams or ointments. Your healthcare provider may prescribe corticosteroid creams or ointments to reduce inflammation.
- Injectable medicines. Your healthcare provider may use a hypodermic needle to inject medicine under your skin or into your vein. Examples include adalimumab, etanercept and infliximab.
- Oral medicines. Oral medicines are pills or capsules taken by mouth. They treat severe forms of inverse psoriasis. Examples include acitretin capsules, and methotrexate tablets.
- Pimecrolimus skin creamortacrolimus ointment. These medicines typically treat eczema, but they may help treat inverse psoriasis, too.
- . Phototherapy uses ultraviolet light, usually ultraviolet B , from special lamps. The ultraviolet light waves found in sunlight can help certain skin disorders, including inverse psoriasis.
Before Stopping Psoriasis Treatment Talk With Your Dermatologist
Because psoriasis is a lifelong disease, its understandable that you may want to stop treatment at some point. Alwaystalk with your dermatologist before you stop treatment.
Some treatments can be stopped immediately. Others need to be discontinued slowly to prevent psoriasis from worsening .
When psoriasis rebounds, it may become a more serious type of psoriasis. A person who had plaque psoriasis may suddenly have pustular psoriasis or erythrodermic psoriasis.
The best way to prevent a rebound is to talk with your dermatologist. Your dermatologist can tell you whether you can stop the treatment abruptly or slowly. Sometimes, the best approach is to gradually switch to another treatment.
Don’t Miss: Who Is The Best Doctor For Psoriasis
Can I Have Sex If I Have An Inverse Psoriasis Flare
Inverse psoriasis isnt a sexually transmitted disease or infection . Still, it can look like an STD or STI. Its a good idea to be honest with your partner if you have a flare-up. If they have any questions, encourage them to talk to a healthcare provider before you have sex.
If you have inverse psoriasis on your genitals, you may experience discomfort or pain during sex. Sexual lubricants and condoms can help ease discomfort, pain or itching.
After sex, carefully clean and dry your genitals and reapply any inverse psoriasis medications.
Remission Is More Likely If You Avoid Triggers
Psoriasis has no cure, and thereâs no guaranteed way to get rid of symptoms for good. You cannot force psoriasis to go into remission. But, you can better your chances of going into remission, and staying in remission longer, by avoiding psoriasis triggers, including:
- Stress. This is one of the most common psoriasis triggers. For many people, avoiding stress completely can be almost impossible. Thatâs especially true if your psoriasis symptoms are causing you to feel stressed or anxious. Trying things like meditation, walking, or relaxation may help.
- Infections. Anything that stresses or affects the immune system can be a psoriasis trigger. People with psoriasis may have a flare-up after getting sick with strep throat, bronchitis, or an ear infection, among other things.
- Injuries to the skin. This could include anything from a scrape to a bug bite, even getting a tattoo.
- Weather. Some people with psoriasis say that cold, dry conditions are especially likely to cause symptoms.
Other possible triggers of psoriasis symptoms include smoking, drinking a lot of alcohol, allergies, and certain medications.
A few other steps you can try to make your time of remission last longer, or keep your symptoms under control:
Recommended Reading: What Is The Best Probiotic For Psoriasis
Your Nails Look Better
For some people, changes to their nails are the first sign a flare-up is occurring. You may notice your finger and toenails are pitted, discolored, or growing abnormally. Psoriasis can also cause your nails to become loose and break. If your psoriasis is going into remission, you may notice your nails returning to a normal color and becoming stronger, with less pits present.
Systemic And Biologic Treatment
People with severe psoriasis may need to use oral or injected medicines, which are systemic treatments. These medications include:
- cyclosporine, which suppresses the immune system
- methotrexate to slow down skin cell formation and reduce inflammation
- oral retinoids or vitamin A derivatives
Systemic treatments can have severe side effects, so people typically use them alongside topical creams or light therapy and only take them for short periods.
Biologics aim to reduce the impact of psoriasis by targeting a specific part of the immune system. They can help prevent flares and relieve symptoms, and they are part of a long-term treatment plan.
Also Check: Does Psoriasis Stay In One Spot
Can You Experience Remission Without Treatment
Its generally recommended to treat your psoriasis. Psoriasis has a chronic relapsing nature, and poorly controlled psoriasis may increase the risk of having other types of psoriasis.
However, if someone has achieved complete remission for at least one year, their doctor may recommend stopping therapy with careful follow-up. You should always talk to your health care provider for medical advice if youre interested in discontinuing your medications.
What Is The Difference Between Psoriasis And Inverse Psoriasis
Psoriasis and inverse psoriasis are both diseases that affect your skin.
Psoriasis features thick, discolored patches of skin covered with white or silvery scales. The thick, scaly patches are plaques.
Inverse psoriasis doesnt feature the thick, scaly plaques like other types of psoriasis, most likely because its present in moist areas of your body. An inverse psoriasis rash also looks shinier than a psoriasis rash.
Also Check: What Cream Do You Use For Psoriasis
What Does Psoriasis Remission Mean For Treatment
Once you reach near or full skin clearance, you may feel like stopping some or all psoriasis treatments. Depending on your health status, psoriasis history, and treatment plan, however, your dermatologist may recommend continuing therapy unchanged. The doctor may also suggest modifying dosages, or they may suggest stopping particular medications.
According to the American Academy of Dermatology, one of three things may happen if psoriasis treatment is stopped:
In general, dermatologists do not recommend stopping biologic therapy. Long-term, continuous therapy is ideal for maintaining remission. Once you reach remission, you should discuss a maintenance plan with your dermatologist. You may need close monitoring and regular adjustments to your treatment plan to help keep your psoriasis under control.
Future Of Psoriasis: Can Lasting Improvement Be Achieved In Psoriasis Care
Professor Carle Paul
Though many steps have been made in the past to improve psoriasis treatment, psoriasis management should focus on the need to decrease the treatment burden for patients, and to help patients achieve both long-term clearance and remission of psoriasis. Results from recent studies have shown that newer biologic therapies have resulted in increased efficacy in patients with psoriasis.43 Data from the BADBIR Registry and DERMBIO studies show that IL-12/23 inhibition results in higher levels of drug persistence and drug survival, compared with anti-TNF alpha or anti-IL-17 therapies.44,45 Furthermore, data from the PSOLAR study shows that drug persistence with ustekinumab was higher when given either as first, second, or third-line treatment, compared with infliximab, adalimumab, or etanercept.46
Figure 2: Predictors of drug-free remission after withdrawal from treatment with guselkumab.49PASI: Psoriasis Area Severity Index.Adapted from Liu et al.49
The GUIDE study will examine further maintenance treatment strategies with guselkumab by comparing several patient populations, including patients with short versus long disease duration and those with biomarkers identified as predictors of drug-free remission in the VOYAGE 2.50
Date of Preparation: October 2019. CP-120819
Read Also: Treatment Of Plaque Psoriasis Scalp
What Can I Do To Help Treat My Psoriasis
There may not be a cure yet but there is much you can do to help maintain and control your psoriasis. Psoriasis, regardless of location or type, is often irritated by contact, particularly tight clothing such as elasticated waistbands, socks, tights, and underwear. It may be useful to wear looser clothing where psoriasis is likely to be irritated either when flaring or during periods of treatment. Identifying factors that may cause your psoriasis to flare, using a diary, can be helpful.