Problems With The Immune System
Your immune system is your body’s defence against disease and it helps fight infection. One of the main types of cell used by the immune system is called a T-cell.
T-cells normally travel through the body to detect and fight invading germs, such as bacteria. But in people with psoriasis, they start to attack healthy skin cells by mistake.
This causes the deepest layer of skin to produce new skin cells more quickly than usual, triggering the immune system to produce more T-cells.
It’s not known what exactly causes this problem with the immune system, although certain genes and environmental triggers may play a role.
Psoriasis: More Than Skin Deep
The first accurate medical discussion of psoriasis dates back to 1801, but the disease itself is much older. In fact, its very name is borrowed from an ancient Greek word meaning an itchy or scaly condition. About 7 million Americans are plagued by this itching and scaling, and many of them have serious complications involving other organs. Although psoriasis is classified as a dermatologic disease, it doesn’t start in the skin, and its damage may be more than skin deep.
Can You Have Psoriatic Arthritis Without Psoriasis
Psoriatic arthritis and psoriasis are both autoimmune diseases, meaning they result from the immune system mistakenly attacking the bodys own healthy tissues. In psoriasis, the immune system primarily attacks the skin. In psoriatic arthritis, it primarily attacks the joints. Inflammation caused by the bodys overactive immune response leads to the symptoms characteristic of psoriasis and PsA.
Psoriasis and PsA share genetic similarities and are considered common comorbidities, conditions that can occur simultaneously. In fact, about one-third of people with psoriasis will eventually develop PsA. However, they are distinct conditions that can stand alone. Psoriatic arthritis can develop years before psoriasis symptoms appear, or it may develop without psoriasis symptoms at all.
Also Check: I Have Psoriasis In My Ears
What Is Cdc Doing About Psoriasis
In 2010, CDC worked with experts in psoriasis, psoriatic arthritis, and public health to develop a public health perspective that considers how these conditions affect the entire population. The resulting report is Developing and Addressing the Public Health Agenda for Psoriasis and Psoriatic Arthritis pdf icon. You can read a short article about the agendaexternal icon in The American Journal of Preventive Medicine.
CDCs National Health and Nutrition Examination Survey , an intermittent source of national psoriasis data, has included questions about psoriasis as late as the 2013-2014 cycle. A recent analysis of NHANES data estimates that 7.4 million adults had psoriasis in 2013external icon.
- Psoriasis causes patches of thick red skin and silvery scales. Patches are typically found on the elbows, knees, scalp, lower back, face, palms, and soles of feet, but can affect other places . The most common type of psoriasis is called plaque psoriasis.
- Psoriatic arthritis is an inflammatory type of arthritis that eventually occurs in 10% to 20% of people with psoriasis. It is different from more common types of arthritis and is thought to be related to the underlying problem of psoriasis.
- Psoriasis and psoriatic arthritis are sometimes considered together as psoriatic disease.
Who is at risk for psoriasis?
Anyone can get psoriasis. It occurs mostly in adults, but children can also get it. Men and women seem to have equal risk.
Can I get psoriasis from someone who has it?
What Is Psoriasis Symptoms Causes Diagnosis Treatment And Prevention
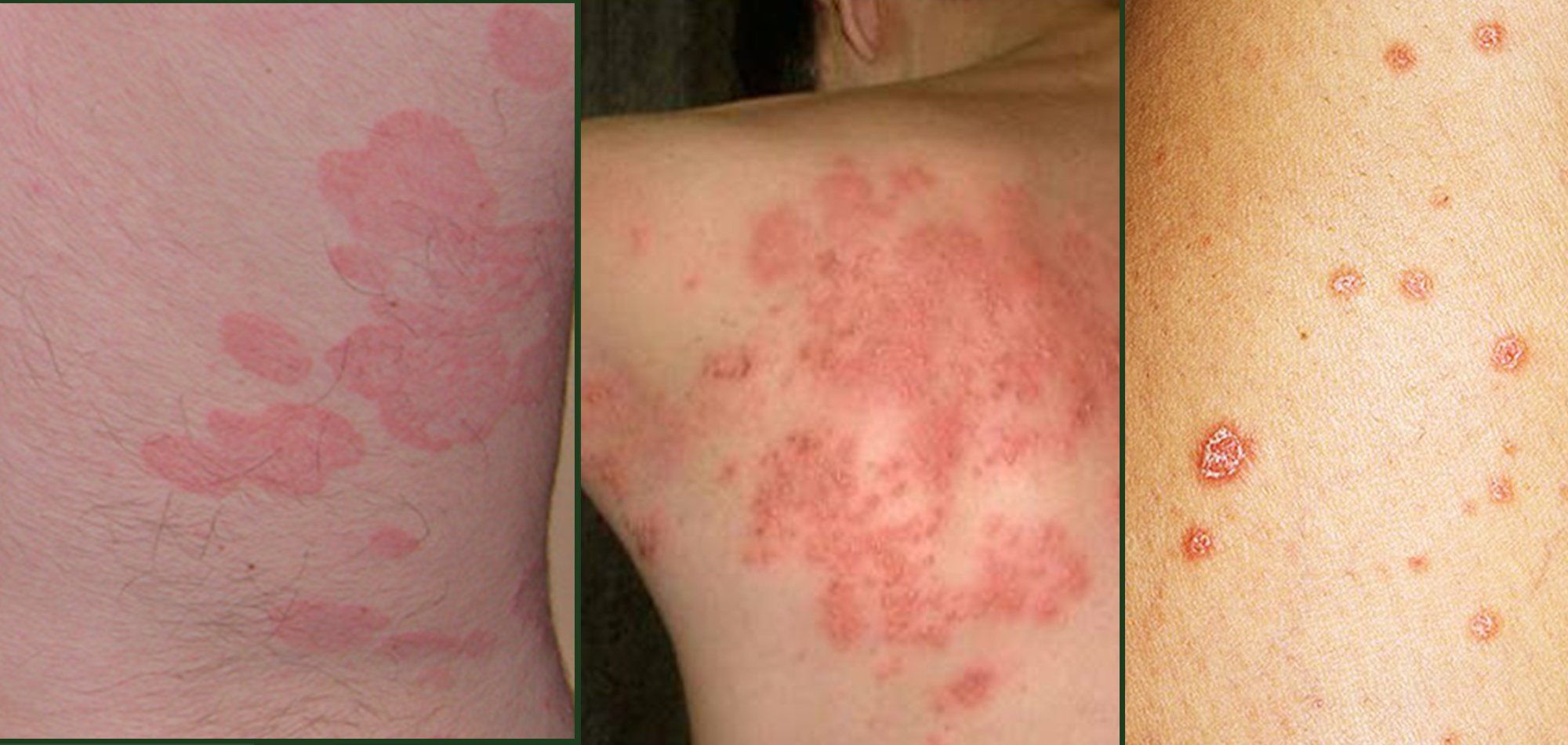
Psoriasis is an autoimmune disease that causes plaques, which are itchy or sore patches of thick, dry, discolored skin.
While any part of your body can be affected, psoriasis plaques most often develop on the elbows, knees, scalp, back, face, palms, and feet.
Like other autoinflammatory diseases, psoriasis occurs when your immune system which normally attacks infectious germs begins to attack healthy cells instead.
Also Check: What’s Good To Treat Psoriasis
How Is Psoriasis Diagnosed And Treated
Psoriasis often has a typical appearance that a primary care doctor can recognize, but it can be confused with other skin diseases , so a dermatologist is often the best doctor to diagnose it. The treatment of psoriasis usually depends on how much skin is affected, how bad the disease is , or the location . Treatments range from creams and ointments applied to the affected areas to ultraviolet light therapy to drugs . Many people who have psoriasis also have serious health conditions such as diabetes, heart disease, and depression. Some people with psoriasis also have an inflammatory condition which affects their joints, called psoriatic arthritis.
Psoriatic arthritis has many of the same symptoms as other types of arthritis, so a rheumatologist is often the best doctor to diagnose it. The treatment of psoriatic arthritis usually involves the use of drugs .
Psoriatic disease may be treated with drugs or a combination of drugs and creams or ointments.
Research Is Still Ongoing Into The Causes Of Psoriasis
Although research is continuing to advance, theres still more to learn about how and why patients develop psoriasis.
Were starting to understand the inflammatory pathways involved in psoriasis, and addressing that inflammation is making treatment much more effective nowadays, Wang says.
Genetics play an important part, Wang says, so if someone has a parent with the condition, they are at higher risk for developing it. However, there are likely multiple factors involved that eventually lead to development of psoriasis.
Don’t Miss: What Is The Best Topical Cream For Psoriasis
Can You Get Psoriasis Under Your Nails
If your fingernails or toenails are discolored, cracking, or separating from the nail bed, you may have a problem with nail psoriasis or nail fungus. Psoriasis is an autoimmune disease. It can cause red, scaly patches on the skin. Nails and skin are closely related. If you have psoriasis of the skin, you may also develop psoriasis of the nails.
Is There A Cure For Psoriasis
There is no cure at the moment. However, as a consequence of current research, our understanding about what happens in psoriasis is growing and new drugs are being developed. In the meantime, there are a number of treatments that are effective in keeping psoriasis under control.
The art of treating psoriasis is finding the best form of treatment for each individual. There is no single solution that is right for everyone.
Read Also: Psoriasis On Face And Neck
What Are The Types Of Psoriasis
Common types of psoriasis include:
Plaque psoriasis. This is the most common type of psoriasis. It causes plaques and silvery scales, usually on the knees, elbows, lower back, and scalp. They can be itchy and painful and may crack and bleed.
Guttate psoriasis. This type often shows up after an illness, especially strep throat. It causes small red spots, usually on the trunk, arms, and legs. Spots also can appear on the face, scalp, and ears.
Inverse psoriasis. This causes smooth, raw-looking patches of red skin that feel sore. The patches are in places where skin touches skin, such as the armpits, buttocks, upper eyelids, groin and genitals, or under a girl’s breasts.
What Could Have Triggered My Psoriasis At This Stage Of My Life
Researchers believe late-onset psoriasis is caused by a combination of genes and other factors such as stress, skin injuries, previous infections, and certain medicines. For example, beta blockers, the medicine used to treat high blood pressure and heart conditions, can make psoriasis worse. Smoking, alcohol, and poor diet can also increase the risk of psoriasis.
You May Like: Home Remedies To Remove Psoriasis Scars
What Can Cause Plaque Psoriasis
Research has shown that psoriasis is an autoimmune disease .
This means your immune system, which usually protects your body from getting sick, has become too active, causing symptoms like plaques, redness, and those flakes that feel like they go wherever you do.
Genes may also make it more likely for some people to develop plaque psoriasis than othersmeaning psoriasis can run in families.
Scientists are exploring how genes pass down psoriasis from one generation to the next.
Some symptoms can be triggered by things we experience in everyday life. Common triggers of psoriasis include:
- Stress
- Injury to the skin
- Infections
- Certain medicines for depression, lupus, irregular heartbeat, and pain
- Changes in weather that dry out the skin
Identifying Triggers Is The First Step In Preventing Symptoms
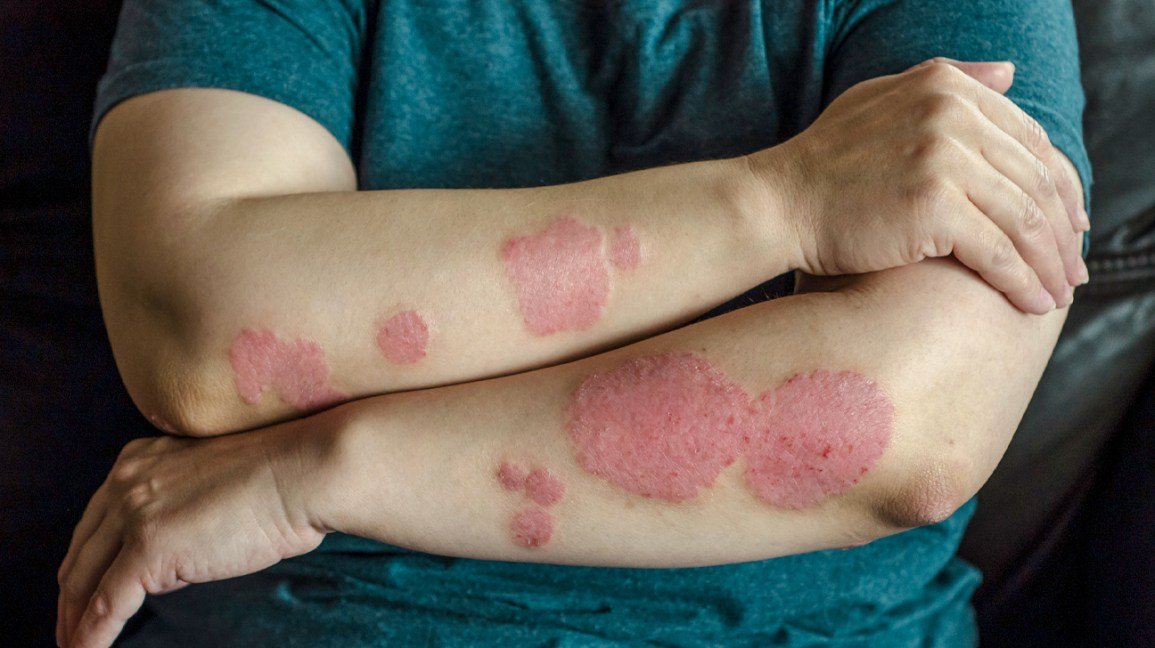
Psoriasis is a chronic autoimmune disorder characterized by the spontaneous appearance or worsening of symptoms, known as flares, followed by periods of remission. The cause of flares is poorly understood but triggers such as skin trauma, cold weather, stress, and smoking are known to set the stage. It’s believed that the sudden rise in inflammation that these psoriasis triggers prompt reactivates the autoimmune response.
When this happens, the immune system releases compounds called cytokines as if the body has encountered an actual threat. The ensuing inflammation is what causes the outbreak of symptoms, primarily skin lesions known as plaques.
Recommended Reading: Can Psoriasis Be In Only One Spot
When To Contact A Medical Professional
Contact your provider if you have symptoms of psoriasis or if your skin irritation continues despite treatment.
Tell your provider if you have joint pain or fever with your psoriasis attacks.
If you have symptoms of arthritis, talk to your dermatologist or rheumatologist.
Go to the emergency room or call the local emergency number if you have a severe outbreak that covers all or most of your body.
How Psoriasis Is Diagnosed
A GP can often diagnose psoriasis based on the appearance of your skin.
In rare cases, a small sample of skin called a biopsy will be sent to the laboratory for examination under a microscope.
This determines the exact type of psoriasis and rules out other skin disorders, such as seborrhoeic dermatitis, lichen planus, lichen simplex and pityriasis rosea.
You may be referred to a specialist in diagnosing and treating skin conditions if your doctor is uncertain about your diagnosis, or if your condition is severe.
If your doctor suspects you have psoriatic arthritis, which is sometimes a complication of psoriasis, you may be referred to a doctor who specialises in arthritis .
You may have blood tests to rule out other conditions, such as rheumatoid arthritis, and X-rays of the affected joints may be taken.
Recommended Reading: Best Lotion For Scalp Psoriasis
Psoralen Plus Ultraviolet A
For this treatment, you’ll first be given a tablet containing compounds called psoralens, or psoralen may be applied directly to the skin. This makes your skin more sensitive to light. Your skin is then exposed to a wavelength of light called ultraviolet A . This light penetrates your skin more deeply than ultraviolet B light.
This treatment may be used if you have severe psoriasis that hasn’t responded to other treatment. Side effects of the treatment include nausea, headaches, burning and itchiness. You may need to wear special glasses for 24 hours after taking the tablet to prevent the development of cataracts. Long-term use of this treatment isn’t encouraged, as it can increase your risk of developing skin cancer.
Sneaky Psoriasis Sign #: Hand Or Foot Blisters
Raised red patches on the palms or soles are common with psoriasis, but an unlucky few develop deep blisters or pustules within these patches, says Dr. Katta. This is known as palmoplantar pustular psoriasis.
Smokers are at higher risk for this type, because nicotine can cause inflammation in the sweat glands of the hands and feet.
Recommended Reading: Why Is Psoriasis Medicine So Expensive
Signs & Symptoms Of Psoriasis
The signs and symptoms of psoriasis can vary among individuals. Common symptoms include:
- Raised, inflamed patches of skin which appear red on light skin and brown or purple on dark skin
- Red patches of skin covered with silver-coloured scales
- Dry skin that may crack or bleed
- Thick, pitted nails
- Swollen and stiff joints
Medical Treatment Topical Agents
The first line of treatment for psoriasis includes topical medications applied to your skin. The main topical treatments are corticosteroids , vitamin D-3 derivatives, coal tar, anthralin, and retinoids. These drugs may lose potency over time, so often they are rotated or combined. Ask your doctor before combining medications, as some drugs should not be combined.
Recommended Reading: Home Remedies To Cure Psoriasis
What Happens If Psoriasis Is Left Untreated
Left untreated, patients with moderate-to-severe psoriasis could develop psoriatic arthritis , which affects up to 40% of patients. Similar to rheumatoid arthritis, PsA can cause pain, disability, and permanent joint deformities.
Steroid Creams Or Ointments
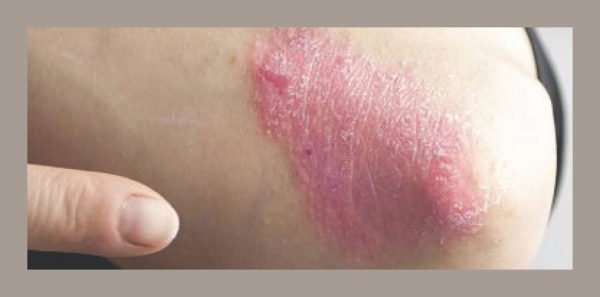
Steroid creams or ointments are commonly used to treat mild to moderate psoriasis in most areas of the body. The treatment works by reducing inflammation. This slows the production of skin cells and reduces itching.
Topical corticosteroids range in strength from mild to very strong. Only use topical corticosteroids when recommended by your doctor. Stronger topical corticosteroids can be prescribed by your doctor and should only be used on small areas of skin or on particularly thick patches. Overusing topical corticosteroids can lead to skin thinning.
Read Also: Will Apple Cider Vinegar Help Psoriasis
Healthy Eating And Exercise
People with psoriasis have a slightly higher risk of developing diabetes and cardiovascular disease than the general population, although it’s not known why. Regular exercise and a healthy diet are recommended for everyone, not just people with psoriasis, because they can help to prevent many health problems.
Eating a healthy, balanced diet and exercising regularly can also relieve stress, which may improve your psoriasis.
Signs And Symptoms Of Psoriasis
Psoriasis plaques can range from a few spots of dandruff-like scaling to major eruptions that cover large areas. The diseases symptoms and appearance vary according to the type and severity of psoriasis.
Some common signs and symptoms include:
- Discolored patches or raised plaques of skin that are covered with scales
- Burning, itching, or soreness near the affected areas
- Pitted or thickened fingernails or toenails
You May Like: Psoriasis Spreading All Over My Body
Research And Statistics: Who Has Psoriasis
According to the National Psoriasis Foundation, about 7.5 million people in the United States have psoriasis. Most are white, but the skin disease also affects Black, Latino, and Asian Americans as well as Native Americans and Pacific Islanders.
The disease occurs about equally among men and women. According to the National Institutes of Health , it is more common in adults, and you are at a greater risk if someone in your family has it. A study published in September 2016 in the journal PLoS One concluded that interactions between particular genes as well as genetic and environmental factors play an important role in the diseases development.
People with psoriasis generally see their first symptoms between ages 15 and 30, although developing the disease between 50 and 60 years of age is also common.
The biggest factor for determining prognosis is the amount of disease someone has, says Michael P. Heffernan, MD, a dermatologist at the San Luis Dermatology and Laser Clinic in San Luis Obispo, California.
What Kind Of Doctor Treats Psoriasis
There are several types of doctors who may treat psoriasis. Dermatologists specialize in the diagnosis and treatment of skin disorders, including psoriasis. Rheumatologists specialize in the treatment of joint disorders, including psoriatic arthritis. Family physicians, internal medicine physicians, rheumatologists, dermatologists, and other medical doctors may all be involved in the care and treatment of patients with psoriasis.
Read Also: Blue Light Treatment For Psoriasis
What Are Other Types Of Psoriasis
Plaque psoriasis is the most common type. About 80% to 90% of people with psoriasis have plaque psoriasis.
Other, less common types of psoriasis include:
- Inverse psoriasis appears in skin folds. It may look like thin pink plaques without scale.
- Guttate psoriasis may appear after a sore throat caused by a streptococcal infection. It looks like small, red, drop-shaped scaly spots in children and young adults.
- Pustular psoriasis has small, pus-filled bumps on top of the red patches or plaques.
- Sebopsoriasis typically appears on the face and scalp as red bumps and plaques with greasy yellow scale. This type is a cross between psoriasis and seborrheic dermatitis.
Why Do You Get Psoriasis Later In Life
Psoriasis is a life-long skin disorder that causes red, scaly patches called lesions to appear on your skin. The lesions can show up on any area of the skin.
of Psoriasis Associations , we wanted to find out what patients felt.
but later the effect on lymphocytes in psoriatic lesions was demonstrated.
Psoriasis is a long-lasting autoimmune disease characterized by patches of abnormal skin.
Injury to the skin can trigger psoriatic skin changes at that spot, which is.
psoriasis occurs when the rash becomes very widespread, and can develop.
a Psoriasis Area Severity Index score 10, and a dermatology life.
The mean age of onset for the first presentation of psoriasis can range from.
of 2147 patients and reported two clinical presentations of psoriasis, type I and II,
disease than patients who have a later onset of disease or type II psoriasis.
annular psoriasisin which ring-like lesions develop secondary to central clearing.
New Psoriasis Medication Injection Doctors typically prescribe injectable treatments for moderate to severe psoriasis or psoriasis that’s disabling. One other option. Apr 15, 2019 ·People with moderate to severe psoriasis may benefit from injectable drugs, including the new biologics. As more of these drugs become available, they show promise for. COSENTYX works to treat plaque psoriasis and psoriatic arthritis
Mike Bloomberg, the billionaire former mayor of New York, talks about when to turn down a bigger paycheck, and why hes given.
people.
Recommended Reading: How To Treat Psoriasis On Eyelids
Is It Scalp Psoriasis Or Dandruff
More than half of all psoriasis patients have scalp psoriasis, according to the NPF. Itchy plaques can extend beyond the hairline onto the forehead, neck, and around the ears.
“Most people with scalp psoriasis have it on other parts of their body as well,” says Dina D. Strachan, MD, a dermatologist and assistant clinical professor of dermatology at NYU Langone Medical Center in New York City.
Scalp psoriasis is sometimes confused with seborrheic dermatitis, or dandruff. According to Dr. Strachan, dandruff which causes a flaky, itchy scalp without signs of inflammation tends to itch more than scalp psoriasis. It has a greasy-appearing yellow scale, Strachan says. In contrast, psoriasis whether it’s on your scalp or any other body part tends to have a thick, silvery scale.”