When Psoriasis Affects The Feet
Psoriasis is a condition caused by an overactive immune system that triggers abnormal skin cell growth.
Normally, skin cells grow and shed in a monthly cycle. With psoriasis, the skin cells grow and build up on the surface of the skin, forming plaques and scales.
Foot psoriasis or palmoplantar psoriasis, which means psoriasis of the hands and feet is a less common type of psoriasis. It causes painful, itchy, red, dry patches of skin on the bottom or soles of your feet. A more rare form of the condition, called pustulosis, involves small, pus-filled blisters in the same area. In both cases, the psoriasis can crack and bleed, which can make everyday tasks like standing or walking difficult.
Forty percent of people who have psoriasis experience palmoplantar psoriasis, according to the National Psoriasis Foundation . In a study published in the August 2020 issue of the Journal of the American Academy of Dermatology, people with palmoplantar psoriasis were six times as likely to have mood disorders likely due to problems with mobility than those with psoriasis affecting other parts of the body.
In some cases, people with foot psoriasis cant even walk, says Abby S. Van Vorhees, MD, chair of dermatology at Eastern Virginia Medical School and emeritus chair of the NPF Medical Board. But the good news is that there are treatments available and theres a lot that can be done to make patients feel better.
When Psoriatic Disease Strikes The Hands And Feet
We take many common movements and activities for granted â until they become difficult or impossible to do. Get a grip on whatâs happening.
Our hands and feet are ultra-sensitive. Sensory neurons, which trigger pain sensations in the brain, cluster at the fingertips. The complex anatomical structure of hands and feet â with many joints, tendons and ligaments packed tightly together â gives us an acute sense of touch and lets us do precision movements. Our hands, particularly when used for communication through gesture, draw attention.Our feet are so important for our balance and mobility.
Thatâs why psoriatic disease, when it strikes the hands and feet, has an outsize effect. The symptoms can be more intense and more upsetting. Fingernail psoriasis, for instance, is often immediately noticeable and can make something as basic as a handshake feel uncomfortable. Pain and other symptoms of psoriasis and psoriatic arthritis in the hands and feet can make other routine tasks hard to accomplish.
Gary Bixby, who lost all his fingernails and toenails to severe psoriasis , says psoriatic nail disease makes it painful to chop fuel for his wood-burning stove, a frustrating problem during winters at his home in Blair, Wisconsin.
âIt was affecting more fingernails, then my toenails and large areas on my arms, legs and trunk,â says Bixby. âThatâs when I went to a podiatrist, who thought I had psoriasis, and then to a dermatologist, who confirmed it.”
Treatment For Psoriasis On The Feet
As yet, there is no cure for psoriasis, but there is a range of treatments that can help relieve symptoms and reduce flare-ups. The choice of treatment will often depend on the type, location, and severity of a persons psoriasis.
The three primary treatments are topical medications, light therapy, and systemic drugs.
Topical medications come in the form of creams, ointments, and oils that people apply directly to their skin. Examples include:
- emollients, which are non-cosmetic moisturizers
- steroids
- calcineurin inhibitors
- coal tar
A person can buy some topical treatments, such as emollients, mild steroids creams, and coal tar foams, over the counter. A doctor can prescribe stronger topical formulations.
Light therapy, also known as phototherapy, usually takes place in hospitals or clinics and involves doctors exposing a person to ultraviolet light. For light therapy to be effective, people may require 2 or 3 sessions a week.
Systemic treatments work throughout the body and include oral and injected drugs. Doctors typically only prescribe these medications for severe psoriasis due to the risk of serious side effect and the need for close monitoring.
Examples of systemic treatments include:
- immunosuppressants, such as methotrexate or cyclosporine
- steroids
- phosphodiesterase 4 inhibitors
- biologics
A doctor may recommend coal tar, light therapy, or systemic drugs for people with psoriasis on the feet that they find difficult to treat in other ways.
Recommended Reading: Is Neem Good For Psoriasis
Bright Future For Psoriasis Of The Feet:
- There Is No Cure, But There Are Amazing Treatments.
- They are getting better every year, in fact over the past 10 years research is showing drugs that display a decreased toxicity while achieving better results.
- Combine these systemic medication innovations with topical creams and UV therapy The future is very bright!
Foot Psoriasis Vs Athlete’s Foot
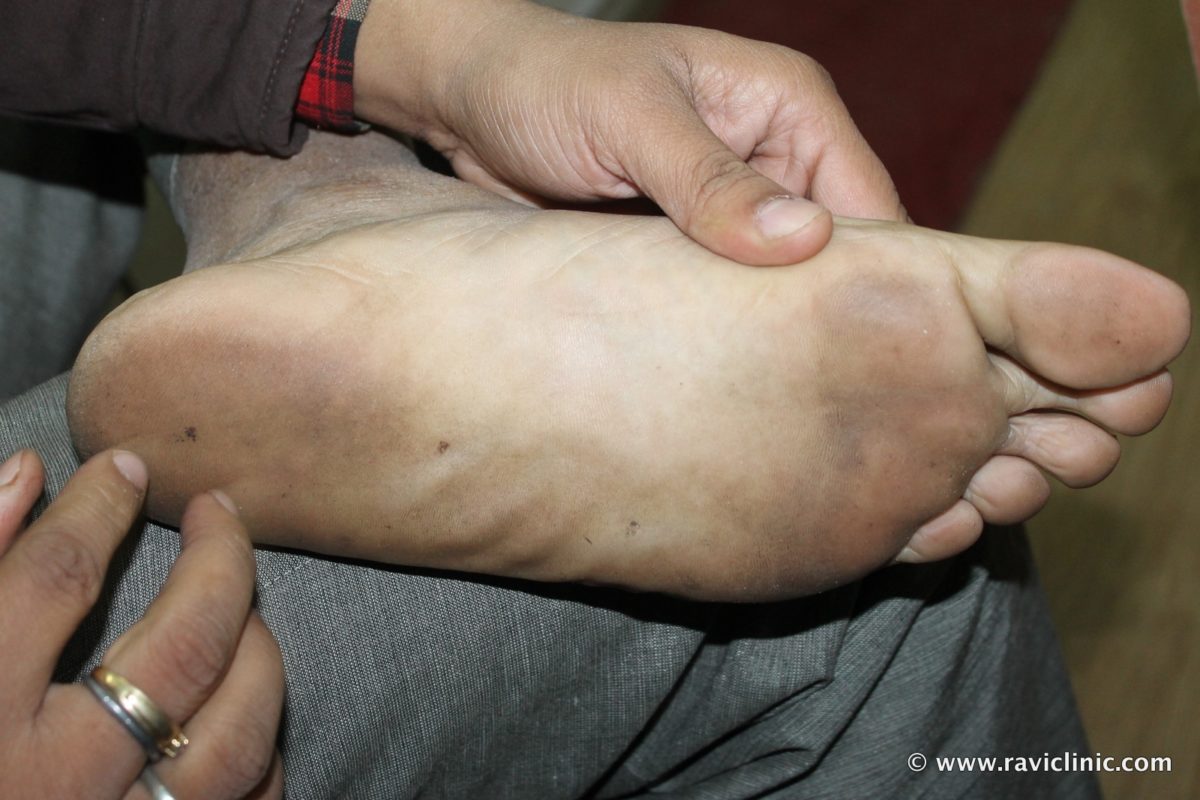
Other conditions may look a little like foot psoriasis, such as athlete’s foot and eczema. That’s why it’s smart to check in with your doctor.
Athlete’s foot is caused by a fungus, and symptoms like scaling or peeling skin, inflammation, or swelling usually occur between your toes. It may spread to the soles of your feet and to your toenails.
Treatments for these various conditions differ, so getting an accurate diagnosis is the first step toward relief.
Don’t Miss: Can You Have Multiple Types Of Psoriasis
Yoga For Psoriasis Treatment
Psoriasis can occur due to stress, and stress can happen due to psoriasis flares ups. Managing stress can provide you relief from psoriasis. Stress can affect your body in many ways, including increasing inflammation. Inflammation can also cause psoriasis, or make this disease more serious if you already have one.
Yoga is the best way to manage stress and there are many yoga asanas which you can perform at home. Perform below yoga to get rid of psoriasis. You can watch videos of all yoga asana at youtube.
Psoriasis is a skin disease that occurs because of the overgrowth of skin cells. This can be a very serious health condition and long-lasting. The exact cause of this problem is yet to find but mainly it occurs because of malfunction of the immunity system. Follow the above Home remedies to get rid of Psoriasis from the neck, feet, hand, and other parts of the body. If you have any other home remedy which we forget mention write in the comment box below.
Psoriasis Cuts On Feet
Psoriasis on Bottom of right foot. Left and hands are just as bad. Does anyone else get deep cuts and is super painful to walk in? Some days it takes so much energy just to make it to the bathroom.
I started cosentyx last august. My insurance company covered it but when the new year came around they decided they werent going to cover it anymore. I had just started seeing little bit of results at the very end of December. And I started taltz in January and have been religiously putting steroid creams 2x daily morning and evening and other ointments to keep skin moist between that time. I have tried every moisturizer and soap you can probably come up with. Plus the $300 if lamps online. Nothing works!!! The one thing I havent tried is epsom salt or dead sea salt because Im afraid it will burn like crazy.
Recommended Reading: Is Eating Oatmeal Good For Psoriasis
What Are The Causes Of Psoriasis
Medical science is still unsure about the causes of psoriasis. But many researchers believe that this problem is related to the immunity system, genetic disorder, or could be a problem of T cells and other WBC which are known as neutrophils.
Psoriasis may be triggered by a strep infection, skin infection. Other triggers may include:-
- Excessive sunburn
Ayurvedic Home Remedies For Psoriasis Treatment
- Sesame Seeds Soak 15-20 sesame seeds in a cup of water. Leave it for overnight then drink on this Sesame water empty stomach in the morning. Repeat this remedy until you get rid of psoriasis.
- Bitter Gourd Juice Extract 1-2 cup of fresh bitter gourd juice and drink empty stomach in the morning. Repeat this remedy for 5-6 months. You can add one tablespoon of lemon juice if you dont like the taste.
You May Like: Does Aloe Vera Help Psoriasis
Mild To Moderate Cases
Mild to moderate palmoplantar psoriasis may be treated with topical treatments, including:
- Emollient moisturizers: Apply thinly and frequently to treat dry, itchy, flaky skin and help prevent cracking.
- Salicylic acid: This keratolytic agent, available in lotions, soaps, foot balms, and shampoos, promotes the shedding of scales and reduces thickened plaques.
- Coal tar: Lotions, creams, and shampoos with this ingredient can reduce inflammation and slow skin growth.
- Anti-itch creams, containing ingredients like camphor, menthol, or benzocaine
- Calcipotriene: A vitamin D derivative, this appears to slow the hyperproduction of skin cells and reduce inflammation.
- Topical corticosteroids: Apply sparingly to temper local inflammation and reduce the size and appearance of plaques.
To improve absorption, a technique called occlusion may be used in which the hands or feet are covered with cling film, plastic gloves, or a plastic bag for several hours or overnight.
Speak with your healthcare provider about the appropriate use of occlusion to prevent skin irritation or the supersaturation of the skin .
A topical drug sometimes used to treat psoriasis, called anthralin, is not very successful for palmoplantar psoriasis. Anthralin is messy and impractical, requiring prolonged treatments, and may further dry and irritate delicate skin.
Psoriasis On Feet: Symptoms Causes And Treatments
Psoriasis is an autoimmune disease in which skin cells grow and build up faster than normal. Some people with psoriasis develop symptoms on their feet. Itching, rashes, and dry, thick skin can be particularly bothersome on the feet and make walking or standing uncomfortable.
If you think you have psoriasis on your feet, its important to get the right diagnosis and work with your dermatologist to find the best treatment for your skin.
Read Also: Blue Star Cream For Psoriasis
Small Area Big Impact
Your hands and feet make up only 4% of your body’s total surface area. But psoriasis here can still have a big effect on your quality of life. You might have pain, or you may just want to cover up the scales. If it affects your work, that could lead to a financial burden as well.
Hands and feet psoriasis can also cause your skin to:
- Crack or split
- Blister or have pimple-like spots
Response To Antifungal Treatment
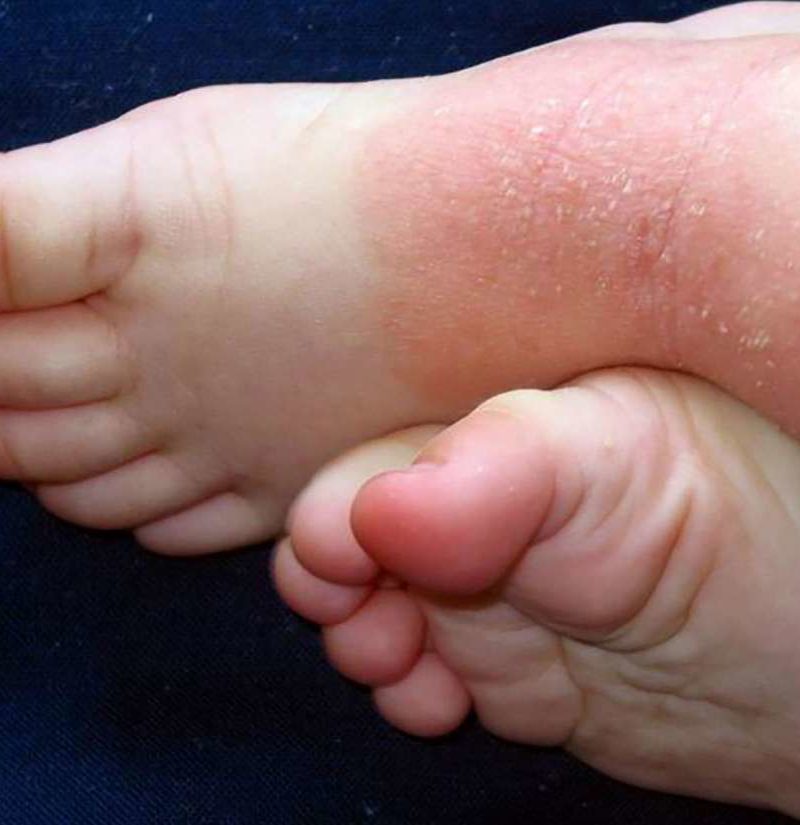
You can buy over-the-counter antifungal creams] and ointments at your pharmacy without a prescription.
Apply this medication to the affected areas. If the rashes begin to disappear, you likely have a fungal infection, or athletes foot. If the rashes dont disappear, you may be dealing with psoriasis or something else.
Recommended Reading: What Vitamins Can Help Psoriasis
Stay Dedicated To Your Treatment Plan
The main thing when dealing with psoriasis on the feet is realizing that it requires special attention. Not having full use of your feet and the mobility you need can impact your quality of life.
The physical aspects of pain, cracking and bleeding can make it harder to treat but not impossible. You must be diligent in your efforts and methods and stay dedicated to the process.
The emotional burdens are hard enough but sometimes disruption of work, walking and daily life can strain you emotionally.
What Are The Clinical Features Of Palmoplantar Psoriasis
Palms and soles affected by psoriasis tend to be partially or completely red, dry and thickened, often with deep painful cracks . The skin changes tend to have a sharp border and are often symmetrical, ie similar distribution on both palms and/or both soles. At times, palmar psoriasis can be quite hard to differentiate from hand dermatitis and other forms of acquired keratoderma. Plantar psoriasis may sometimes be similar in appearance to tinea pedis. There may be signs of psoriasis elsewhere.
Palmoplantar psoriasis tends to be a chronic condition, ie, it is very persistent.
Compared to chronic plaque psoriasis on other sites, palmoplantar psoriasis is more commonly associated with:
Don’t Miss: Why Do I Have Psoriasis
What Can I Do To Help My Feet
The most important action is to seek advice and help when you notice any changes in your foot, whatever they may be. You can talk to your GP or local pharmacist for advice. Some problems can be resolved simply. For issues that are more persistent you may be referred to a specialist, such as a dermatologist, rheumatologist, physiotherapist, surgeon or chiropodist/podiatrist.
For general foot care, personal hygiene is important, particularly in avoiding fungal and viral infections. Change shoes and socks regularly, avoid shoes which are ill-fitting or cause bad posture. If you are overweight, losing weight could relieve the pressure on your joints and improve your walking gait.
If you are diagnosed with psoriasis, develop a treatment regime that works for you often, applying treatment after a bath or shower, along with the use of an emollient, can make the process easier.
If you have nail involvement, keep nails trimmed and clean. If they are thick, try trimming them after soaking them in a bath or shower, as this makes them softer and easier to cut. Alternatively, seek an appointment with a chiropodist, which is often available via the NHS.
If you have psoriatic arthritis, it is important to rest inflamed joints. Sourcing footwear that supports the foot and helps to reduce the pressure on the inflamed areas can help, as can inner soles and orthotic supports. Once again, a chiropodist is best placed to advise you.
This article is adapted from The psoriatic foot leaflet.
What Is The Treatment For Palmoplantar Psoriasis
Improvement in general health can lead to an improvement in palmoplantar psoriasis.
- Weight loss, if overweight
- Investigation and management of associated health conditions
Mild psoriasis of the palms and soles may be treated with topical treatments:
- Emollients: thick, greasy barrier creams applied thinly and frequently to moisturise the dry, scaly skin and help prevent painful cracking.
- Keratolytic agents such as urea or salicylic acid to thin down the thick scaling skin. Several companies market effective heel balms containing these and other agents.
- Coal tar: to improve the scale and inflammation. Because of the mess, coal tar is often applied at night under cotton gloves or socks.
- Topical steroids: ultrapotent ointment applied initially daily for two to four weeks, if necessary under occlusion, to reduce inflammation, itch and scaling. Maintenance use should be confined to 2 days each week to avoid thinning the skin and causing psoriasis to become more extensive.
Calcipotriol ointment is not very successful for palmoplantar psoriasis. It may also cause an irritant contact dermatitis on the face if a treated area inadvertently touches it. Dithranol is too messy and irritating for routine use on hands and feet.
More severe palmoplantar psoriasis usually requires or systemic agents, most often:
You May Like: What Causes Psoriasis In Children
Ways To Treat Psoriasis At Home
Psoriasis is a recurring autoimmune disorder characterized by red, flaky patches on the skin.
Even though it affects your skin, psoriasis actually begins deep inside your body in your immune system.
It comes from your T cells, a type of white blood cell. T cells are designed to protect the body from infection and disease. When these cells mistakenly become active and set off other immune responses, it can lead to psoriasis symptoms.
Even though theres no cure, many treatments exist to ease the symptoms of psoriasis. Here are 12 ways to manage mild symptoms at home.
Could It Be Palmoplantar Pustulosis
When dealing with psoriasis of the foot you may also want to consider palmoplantar pustulosis. Severe pain when walking, plaque and scales on the soles of the foot or bleeding from cracks on the feet are all symptoms of palmoplantar psoriasis.
This makes it difficult to perform daily activities, including walking. Wearing shoes, driving and walking are horribly painful with flares.
You May Like: Il 17 Inhibitors For Psoriasis
Getting A Diagnosis Of Psoriatic Arthritis
The presence of psoriasis may provide an indication of psoriatic arthritis when someone develops joint symptoms. Psoriatic arthritis can develop in people with a lot or a little of psoriasis, and may be more common in people with nail psoriasis. As well as joint symptoms, psoriatic arthritis can lead to feeling tired. Many people become frustrated by a lack of diagnosis psoriatic arthritis tends to have periods of improvement and worsening, which may also be attributed to mechanical joint problems and not inflammatory arthritis.
If you have the symptoms of inflammatory arthritis, such as psoriatic arthritis, your doctor will often refer you to a rheumatologist. In some cases, further tests and imagery may be sought, although this will depend on the individual circumstances and level of confidence in the initial diagnosis.
How Does Psoriasis Impact The Feet
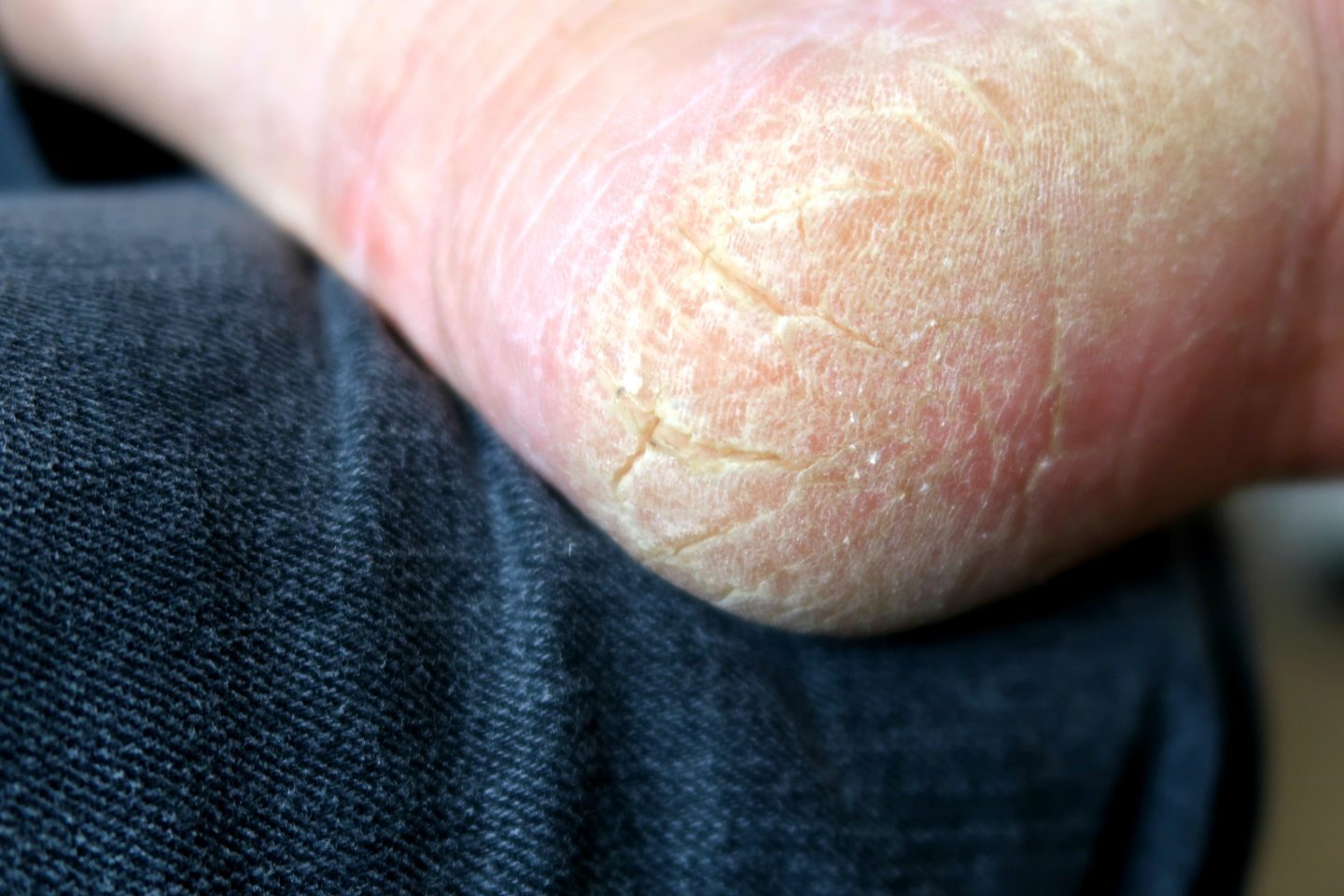
There are a few different ways psoriasis can disrupt your daily life by attacking your feet. If you have psoriasis theres already so much going on with your body, that you may not realize its affecting your feet too. You may think the pain in your feet is from standing too long or normal everyday fatigue.
It could be more severe than you think. Since Ive had these feet for almost 60 years Im thinking Im just getting old and my feet are old too. They hurt more than usual, but Im so used to pain that I just ignore it now.
Recommended Reading: How To Remove Psoriasis Black Marks
When Psoriasis Affects Your Feet And How To Treat It
View source:
Psoriasis is uncomfortable anywhere, but what if its on the soles of your feet? These tips will help you manage better.
Medically Reviewed by Sanjai Sinha, MD
The severe form of foot psoriasis is called palmoplantar pustulosis.
Your feet work hard. Theyre in almost constant use and as a result, they take a lot of wear and tear. Everyone gets the occasional blister or callous, but if you have psoriasis, the pain may not stop there. Psoriasis lesions can be uncomfortable wherever they occur, but they may be especially difficult to endure on the soles of your feet.
Psoriasis is a chronic autoimmune condition that affects as many as 7.5 million Americans. The most common type of psoriasis causes plaques red, raised patches on the skin that are covered by a silvery layer of dead skin.
Plaque psoriasis usually occurs on the elbows and knees, but other types of psoriasis can affect the soles of your feet and the palms of your hands, explains Rebecca Tung, MD, dermatologist at Loyola University Medical Center in Chicago and associate professor of medicine at Loyola University Chicago Stritch School of Medicine. There are two forms of psoriasis that can be seen on the palms of the hands and soles of the feet. A milder form causes the feet or hands to be dry and scaly, and a more severe form causes pustules to form on the feet or hands.