What Is Psoriasis Symptoms Causes Diagnosis Treatment And Prevention
Psoriasis is an autoimmune disease that causes plaques, which are itchy or sore patches of thick, dry, discolored skin.
While any part of your body can be affected, psoriasis plaques most often develop on the elbows, knees, scalp, back, face, palms, and feet.
Like other autoinflammatory diseases, psoriasis occurs when your immune system which normally attacks infectious germs begins to attack healthy cells instead.
How Common Is Psoriasis
Although it is difficult to estimate exactly how many people are living with psoriasis, it is thought that the disease affects at least 125 million people around the world. This means that about 2 percent to 3 percent of the global population have some form of psoriasis.1,2
Surveys suggest that around 3 percent of all people over age 20 living in the U.S. have been diagnosed with psoriasis, or 7 million adults.-3
However, researchers think that it is likely that many more than 7 million people in the United States have the disease. This is because many people may not have been diagnosed by a healthcare provider yet, or do not know for sure that they have psoriasis.3
How To Stay Safe
Having psoriasis and a compromised immune system is a good reason to want to stay healthy.
To minimize your risk for COVID-19, take the following CDC precautions:
- Stay home as much as you can.
- Avoid crowds, and limit close contact with others when out in public.
- Avoid touching your face, nose, and mouth when out.
- Avoid touching frequently touched surfacessuch as doorknobs and shopping cartswhen out in public. Carry disinfecting wipes for when you need to touch surfaces.
- Wear a mask when in a crowded place.
- Talk to your doctor about whether the COVID vaccine is an option for you, and if it is, get vaccinated as soon as you can.
- Wash your hands with soap and water for at least 20 seconds or use hand sanitizer after coming inside or after touching commonly touched surfaces.
Don’t Miss: What Does Psoriasis Look Like When It First Appears
Psoriasis And Cardiovascular Risk
- A recent study in the Journal of the American Academy of Dermatology2 noted several medical conditions or situations that increase the cardiovascular risk for individuals who have mild to severe psoriasis, including:
- Smoking.
- Hyperlipidemia .
- Increased Body Mass Index .
- Researchers who studied medical records of more than 680,000 British patients found that people in their 40s with severe psoriasis were more than twice as likely to suffer a heart attack than people without the skin disease.
- Mild psoriasis slightly raised the risk for heart attack by 20 percent for people in their 40s.
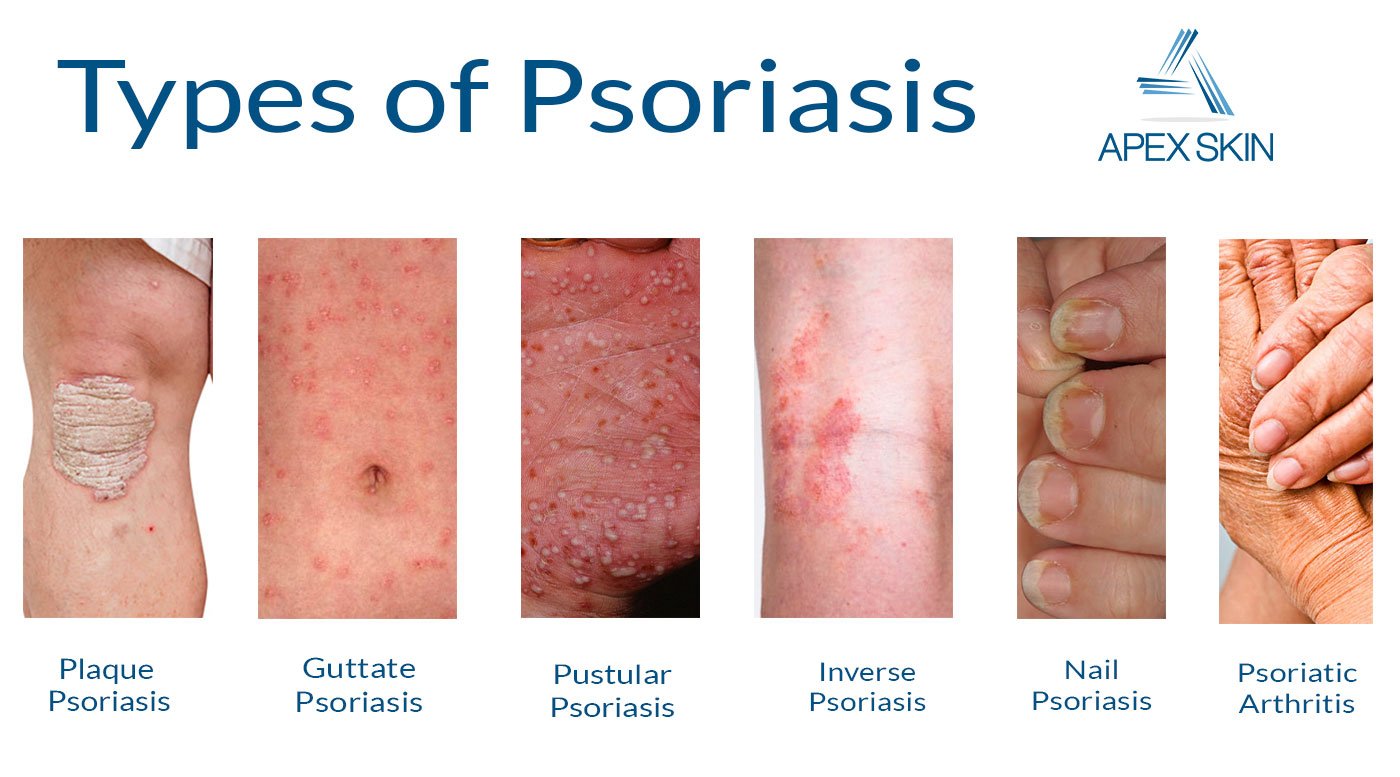
What Is Plaque Psoriasis
Plaque psoriasis, which is recognizable due to the scaly plaques it produces on the skin, is the most common type of psoriasis. An estimated 80 to 90 percent of people with psoriasis develop plaques.
Some people will have more than one type of psoriasis. People who have plaque psoriasis may later develop other forms of the condition, such as psoriatic arthritis.
Usually, the turnover of peoples skin cells takes 21 to 28 days. In people with psoriasis, the body attacks healthy skin cells, so new cells develop every 4 to 7 days.
Psoriasis damages patches of skin, leaving areas of redness and irritation. This damage causes the skin to appear scaly and gray and to peel off.
Plaque psoriasis is not an infection, and it is not contagious. However, irritated patches of psoriasis can become infected.
In some people, an infection or injury to the skin can trigger an outbreak of psoriasis. People experiencing their first psoriasis flare-up may mistake their symptoms for an allergic reaction or skin infection.
Recommended Reading: Does Aloe Vera Help Psoriasis
Leaving Abbvie Web Site
You are leaving the SKYRIZI site and connecting to a site that is not under the control of AbbVie. AbbVie is not responsible for the contents of any such site or any further links from such site. AbbVie is providing these links to you only as a convenience and the inclusion of any link does not imply the endorsement of the linked site by AbbVie. You should also be aware that the linked site may be governed by its own set of terms and conditions and privacy policy for which AbbVie has no responsibility.
Conversely, the presence of this link does not imply the linked site’s endorsement of SKYRIZI or AbbVie.
Do you wish to leave this site?
US-RISN-190090
How Do People Get A Second Type Of Psoriasis On Their Skin
While theres no way to predict who will develop a second type of psoriasis, some people may be more susceptible. For example, having severe psoriasis that isnt well controlled, stopping a strong medication too quickly, or getting strep throat may increase your risk.
The following explains how people who have plaque psoriasis, the most common type of psoriasis, can develop a second type of psoriasis on their skin.
Youll also find out how plaque psoriasis can turn into a different type of psoriasis.
Inverse psoriasis: Many people gain a lot of weight after getting plaque psoriasis. Researchers arent sure why this happens, but they have discovered that extra pounds can increase your risk of developing inverse psoriasis.
Inverse psoriasis only forms in areas where skin touches skin, such as the armpits, groin, or underneath the breasts. It causes smooth, bright-red patches of raw-feeling skin.
Guttate psoriasis: Some people with plaque psoriasis have developed guttate psoriasis after getting an infection, such as strep throat. Guttate psoriasis causes spots on the skin that are small, pink to salmon-colored, and scaly. These spots are often widespread, appearing on the torso, legs, and arms.
Erythrodermic psoriasis: Some people who have severe plaque psoriasis see their plaque psoriasis turn into erythrodermic psoriasis. This can happen when:
Different ways that psoriasis can affect the nails
Also Check: Wild Naturals Eczema & Psoriasis Cream
Is Psoriasis The Same As Eczema
Psoriasis and eczema are two different skin conditions. They differ in where the disease appears on the body, how much it itches and how it looks. Eczema tends to appear more often behind the knees and inside the elbows. Eczema also causes more intense itching than psoriasis. Many people, especially children, can get both eczema and psoriasis.
How Is Plaque Psoriasis Diagnosed
Plaque psoriasis is not your typical rash.
“There are various subtypes and forms that affect different locations of the body and depending on the location can come with its own impact on quality of life,” says Dr. Friedman.
While a biopsy of the skin is often not needed for diagnosis of psoriasis, Dr. Brodell says sometimes a dermatologist may choose to perform a biopsy to exclude other possible conditions that also include scaling, such as cutaneous T-cell lymphoma.
To diagnose psoriasis, doctors often examine your skin and look for characteristics of psoriasis on typical areas of the body where psoriasis occurs, such as the elbows, knees, and scalp.
“If people have scaly rashes in those areas, it is most likely psoriasis,” says Dr. Brodell.
Because eczema can often be mistaken for psoriasis and vice versa, he says it’s important that a dermatologist makes the diagnosis.
“For a dermatologist, looking at psoriasis and eczema is like the difference between a VW bug and a Porsche sports car. There are a lot of things about them that are the same, but we can detect some different things just looking at it,” Dr. Brodell says.
RELATED:Scalp Psoriasis Vs. Dandruff: How to Tell the Difference and What to Do to Relieve Your Scalp Itch
Recommended Reading: Best Conditioner For Scalp Psoriasis
Are Some People More Likely Than Others To Develop Psoriasis
People of all ages can develop psoriasis. About one-third of people with psoriasis are diagnosed with the disease before the age of 20, and around three-quarters of people are diagnosed before the age of 40. Some people who have never had the condition before will develop it for the first time between the ages of 50 and 60.1,3
Psoriasis affects men and women at equal rates.3
About one-third of people with psoriasis report having a relative with the condition. If a parent has psoriasis, their child has about a 10 percent chance of developing it too. If both parents have psoriasis, their child has about a 50 percent chance of developing the disease.2 Incident rates in children have more than doubled since 1970. Children also are more likely to have serious co-occurring health issues such as depression, anxiety, obesity, diabetes, high blood pressure, high cholesterol, and rheumatoid arthritis.4
Psoriasis can affect people of all ethnicities. In the U.S., research has shown that psoriasis is more common among people of certain ethnicities than others. For example, researchers estimate that in the United States, around 2.5 percent of non-Hispanic Caucasians have psoriasis compared to 1.3% of African Americans. About 80 percent, reported mild disease.1,3
People with psoriasis report more mental distress or mild to severe depression than those without psoriasis. They are also more likely to be obese and be a former smoker.3
What Else Should I Ask My Healthcare Provider
If you have psoriasis, ask your healthcare provider:
- How can I prevent outbreaks and control symptoms?
- What medication will work best for me?
- What else should I do to improve symptoms?
- What are my options if creams dont work?
- Will psoriasis ever go away?
A note from Cleveland Clinic
Psoriasis, an itchy skin condition, can come and go throughout your life. Its related to an overactive immune response and is not contagious. If you have skin changes that arent going away, talk to your healthcare provider. There is no cure for psoriasis, but psoriasis treatments can improve symptoms. Your provider may prescribe a special cream or moisturizer or medications. Other therapies are available if creams or medicines dont work. Maintaining your overall health will also help improve symptoms.
Last reviewed by a Cleveland Clinic medical professional on 10/17/2020.
References
You May Like: Early Stage Psoriasis On Face
What Causes Plaque Psoriasis
While it’s not exactly known why some people get psoriasis and others don’t, Dr. Friedman says the cause is believed to be a mix of nature and nurture.
“We know there is a genetic connection, but we don’t know enough about that yet, and we think there are certain triggers in the environment, so both might release psoriasis,” he says.
Robert T. Brodell, MD, chair of the Department of Dermatology at the University of Mississippi Medical Center, says a phenomenon called Koebnerization named for a 19th century dermatologistexplains some instances of plaque psoriasis. It occurs where the skin has been traumatized. “So, if you have surgery for your appendix, you may heal from your surgery, but psoriasis may develop all along that scar,” he tells Health.
While scientists can’t explain exactly why this might occur, they do know what’s happening in the body when plaque psoriasis develops. Essentially, people with plaque psoriasis have an overactive immune system that causes skin cells to develop too quickly. Instead of growing and shedding over the course of a month, new cells appear in a matter of three to four days. But they don’t fall off quickly they pile up on the surface of the skin, creating a buildup of plaque and scales.
How Is Plaque Psoriasis Treated
While there’s no cure for psoriasis, Dr. Friedman says there are many treatment options that can clear up these skin lesions.
“The question isn’t how are you going to treat psoriasis, it’s which are you going to pick because we have so many options,” he says. And there are more and better treatments all the time. “We used to be happy clearing someone by 75%, but now we treat to clear it. We have drugs that will get you 99% clear.”
Treatment options include:
- Topical creams and ointments, such as steroid creams
- Systemic treatments, meaning medications used to slow down the immune system
- Biologic medications, or drugs that target areas and are not systemic
- Alternative options, such as salt baths and aloe vera
Recommended Reading: Is Neem Good For Psoriasis
What Can I Do To Help
- Discuss your psoriasis and how it affects your life with your GP or dermatologist and identify treatment goals.
- Manage your risk factors for heart disease and stroke with your GP.
- Adopt a healthy lifestyle: eat a balanced diet, try to lose weight if you are overweight and exercise regularly.
- Stop smoking if you smoke.
- If you drink excessive alcohol, reducing your intake might be helpful.
- Reduce stress, where possible.
- Take your medications as recommended by your GP or dermatologist.
If you have pain in your joints discuss with your GP or dermatologist.
Enhancing Healthcare Team Outcomes
Plaque psoriasis is a complex life long disorder with enormous morbidity. Thus, it is best managed by an interprofessional team.
Insulin resistance and cardiovascular diseases are more common in psoriatic patients as are metabolic comorbidities. Obesity is the most common comorbidity observed in children with psoriasis. Many patients present with reduced quality of life and psychological manifestations and need special attention and counseling. Thus, primary care clinicians should advocate lifestyle modification such as reducing weight, reducing alcohol intake and smoking cessation may help control psoriasis, improve the results of treatment and prevent future complications.
Sudden onset, palmoplantar keratoderma, severe nail dystrophy, the involvement of skin folds should arouse suspicion of associated HIV infection in whom pustular forms are also more common with a higher frequency of arthritis.
Teaching Points
Outcomes
Read Also: What Shampoo Can I Use For Psoriasis
How Common Is Psoriatic Arthritis In People With Psoriasis
The prevalence of psoriatic arthritis among psoriasis patients is higher than previously thought, according to several international studies published between 2013 and 2015. In North America and Europe, between 18 and 42 percent of people with psoriasis, an inflammatory skin disease, also have psoriatic arthritis. In the United States, psoriasis affects about 2.2 percent of the population , making it the most prevalent autoimmune disease in the US. In addition to skin problems associated with psoriasis, psoriatic arthritis affects the joints and other parts of the body.
The Importance Of Early Diagnosis In Psoriatic Arthritis
Because PsA is progressive and can cause irreversible joint damage, early diagnosis and treatment are critical. The earlier your condition is identified, the more likely doctors can slow or stop joint damage with medication. Treatment options may include biologics such as etanercept and adalimumab , and disease-modifying antirheumatic drugs such as methotrexate and the newer apremilast .
There are several challenges in diagnosing PsA, including lack of standardized criteria and the wide range of doctors people with this condition might see. If you have symptoms of psoriatic arthritis, you may go to your primary care doctor, dermatologist or rheumatologist. We see a lot of patients coming in with a delayed diagnosis. And now that we have such great treatments to manage the symptoms and slow down progression, we really want to find these patients, says M. Elaine Husni, MD, vice chair of rheumatology at the Cleveland Clinic in Ohio.
Don’t Miss: What Are Symptoms Of Plaque Psoriasis
How Is Psoriasis Treated
Mild psoriasis is treated with topical treatments, including moisturizers and over-the-counter and prescription creams and shampoos. Moderate to severe psoriasis is usually treated with a combination of approaches, including topical treatments, , and systemic medications like biologic therapy.2 Some of the biologic therapies used to treat psoriasis are the same medications that are used to treat AS.
In addition to medications, many people with psoriasis incorporate lifestyle changes to help control their symptoms. Identifying and avoiding triggers can help reduce flares, and some people find that dietary changes, regular exercise, and stress management techniques help manage their condition.
How Can Psoriatic Arthritis Be Identified Earlier
A number of educational initiatives aimed at bringing together rheumatologists and dermatologists to learn from each other about psoriasis and psoriatic arthritis have been initiated. The good news is its possible to diagnose the majority of PsA patients based on history and a physical exam alone, prior to the results of the lab work and X-rays. Thus dermatologists who may not order lab work or X-rays can still feel confident about identifying patients who need to be referred to rheumatologists.
As a patient, you should be proactive and tell your doctor about any joint symptoms you may be experiencing. These may include joint pain of a noticeable duration , morning stiffness and joints that feel swollen or warm for days at a time.
Read Also: Mejor Tratamiento Para La Psoriasis
How Can Psoriasis Be Treated
Treatment of psoriasis depends upon your individual circumstances. Treatment applied to the surface of your skin is sufficient alone in most patients. For people with more extensive or difficult to treat psoriasis, ultraviolet light treatment , tablet treatment or injection treatment may be required.
How Will Psoriasis Affect Me
Psoriasis is a complicated condition that is very unique to each individual. Everyone has different ways in which they cope with their psoriasis, and the amount of skin affected by psoriasis can differ greatly from person to person.
It is important that both the physical signs of psoriasis and the psychological aspects of psoriasis are assessed together, and regularly, so that the most appropriate treatment can be prescribed. The psychological impact is not always related to the clinical severity of psoriasis, so do not be afraid to tell healthcare professionals how you are feeling.
If you are finding it difficult to cope with your psoriasis, please visit your GP, or get in touch with us for information and advice.
If you’d like to speak with others who have psoriasis, and share personal experiences and advice, feel free to register for our forums.
Don’t Miss: Is Eating Oatmeal Good For Psoriasis
Causes And Risk Factors Of Psoriasis
Psoriasis, in general, is a genetic condition passed down through families. “It’s likely that multiple genes need to be affected to allow psoriasis to occur and that it’s frequently triggered by an external event, such as an infection,” says James W. Swan, MD, professor of dermatology at the Loyola University Stritch School of Medicine in Maywood, Illinois.
Certain risk factors, such as a family history or being obese, may increase your odds of developing psoriasis.
According to the National Psoriasis Foundation , at least 10 percent of people inherit genes that could lead to psoriasis, but only 3 percent or less actually develop the disease. For this reason, it is believed that the disease is caused by a combination of genetics and external factors or triggers.
A psoriasis outbreak may be provoked by: