Plaque Psoriasis: Red Bumps And Silvery Scales
Plaque psoriasis is the most common form of the chronic skin condition, affecting about 80 percent of people with psoriasis. Usually starting as small red bumps on the skin, plaque psoriasis develops into red patches with a silvery, scaly coating these raised patches are called plaques. Plaques usually show up on elbows, knees, and the lower back, and they can last for months or even years without treatment.
What Can Prevent Someone From Getting A Second Type Of Psoriasis
Most types of psoriasis cannot be prevented.
That said, if you already have plaque psoriasis, it may be possible to reduce your risk of developing another type of psoriasis on your skin. Dermatologists recommend taking the following precautions:
-
Protect your skin to prevent sunburn
-
Take medication as directed and speak with your dermatologist before stopping a medication
-
Treat your psoriasis so that its well-controlled
-
Watch your weight so that you stay at a weight thats recommended for your age and height
Watching your weight may help prevent inverse psoriasis. This type of psoriasis is more common in people who are 20 or more pounds overweight.
Psoriasis And Mental Health
Skin conditions that affect your appearance naturally can make you self-conscious. Add the misconception that psoriasis is contagious, and it’s no wonder those with psoriasis are often embarrassed to show their skin. Because of this misconception, psoriasis can be very isolating and wear on mental health. “Its a real problem. A condition thats visible like this is a disease that can change how people view you,” Dr. Cather says. “It can change how you present yourself and even what you wear.”
Beyond that, research has shown that psoriasis can contribute to or worsen various mental health conditions, including depression, anxiety, bipolar disorder, eating disorders, and more. For more information, check out SELFs reporting on the complex connection between psoriasis and mental health here.
Also Check: How To Ease Psoriasis Itching
How Is Skin Cancer Treated
Treatment for skin cancer depends on the size and severity of the skin cancer. Typical treatments include the following:
- Surgery. The best way to prevent the skin cancer from spreading or growing is to surgically remove it.
- Radiation therapy.Radiation involves beams of high-powered energy that can destroy cancer cells. Its often used if your doctor cant remove all of the skin cancer during surgery.
- Chemotherapy. This intravenous drug treatment kills cancer cells. Some lotions and creams with cancer-killing medications may be used if you have skin cancer thats confined to the top layers of your skin.
- PDT is a combination of medication and laser light thats used to destroy cancer cells.
- Biologic therapy. Biologic therapy involves medication that boosts your bodys natural ability to fight cancer.
Treatments for skin cancer are most successful when the cancer is found early, particularly before it spreads to other organs in a process known as metastasis.
The cancer is more likely to grow and spread to nearby tissues and organs if its not detected and treated early.
Anyone can develop psoriasis. Certain risk factors increase the chances that youll develop the skin condition.
Heres My Diet And The List Of Products I Use:
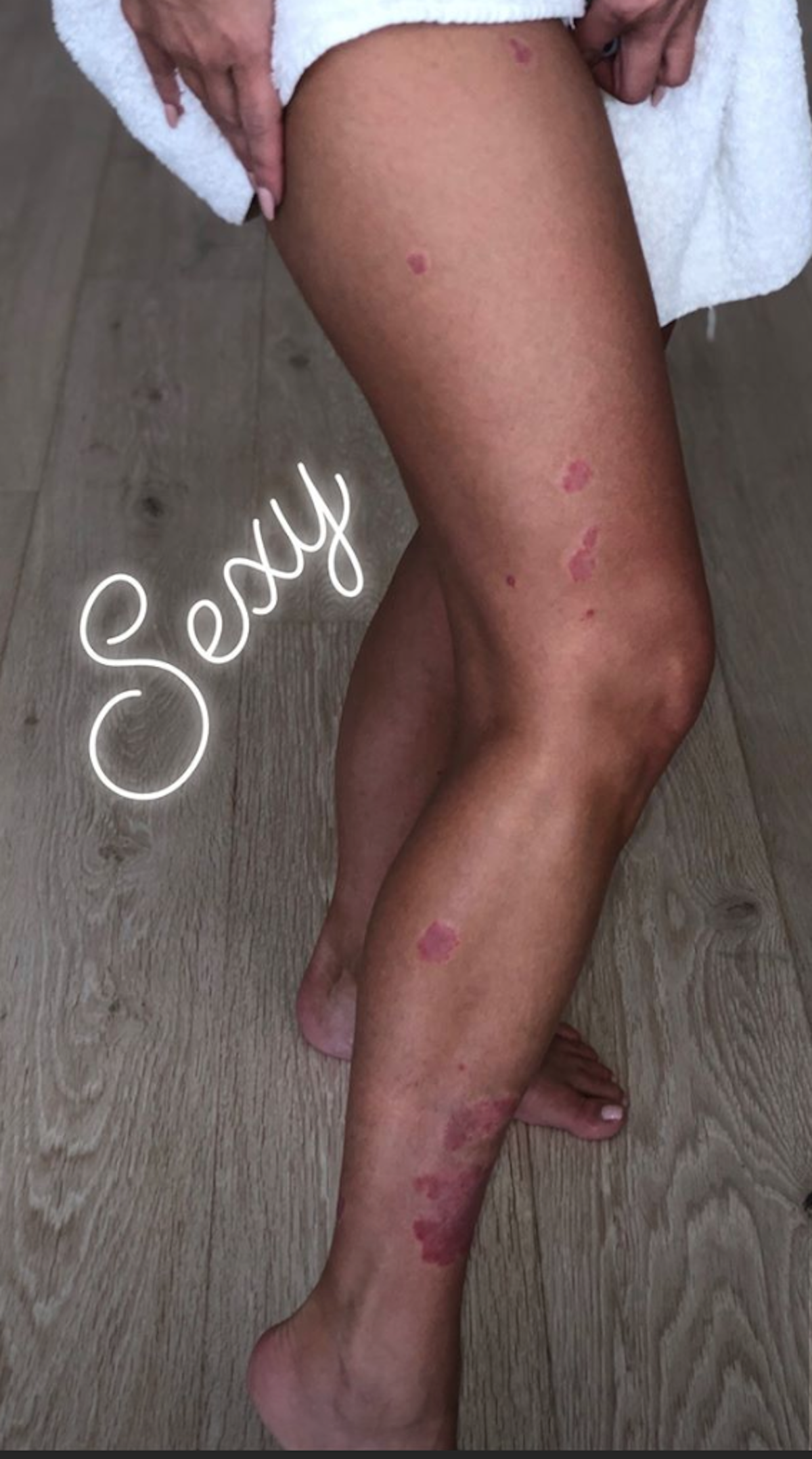
Nothing sold in a convenient store, all that is garbage.
No beef or cured pork.
No white bread.
Coffee thats diluted with an inch of milk. When Im at home, I use coconut milk.
IPAs and hard ciders are the only alcohols that dont trigger my psoriasis. I have read online other people who say IPAs do not cause outbreaks either. If I drink a Bud or Coors or whiskey, my skin gets bad immediately.
I drink one to two cups of detox tea a day.
Recommended Reading: Vitamin D Cream For Psoriasis
What Are The Clinical Features Of Genital Psoriasis
Psoriasis of the external genitalia and perianal area often presents as well-demarcated, bright red, thin plaques. These usually lack scale, as friction between the skin surfaces rubs it off. Scales may be seen on the outer parts of the genital skin. Scales can be easily scraped off, leaving pinpoint bleeding.
In women, vulval psoriasis appears symmetrical. It can vary from silvery, scaly patches adjacent to the labia majora to moist, greyish plaques or glossy red plaques without scaling in the skin folds.
In men, the penis and scrotum may be involved. The glans penis, the bulbous part of the end of the penis, and the corona are most commonly affected. In circumcised men, plaques can be more scaly than on the rest of the genital skin. In uncircumcised men, nonscaling plaques are more common.
Psoriatic napkin eruption presents as red and sometimes silvery plaques with well-defined borders in the nappy area of children under the age of 2 years. It usually clears up after a few months to a year, but may later generalise into plaque psoriasis.
Psoriasis in genital areas can be very itchy at times. The plaques may also be fissured and painful.
Psoriasis does not lead to scarring. The skin can return to a normal appearance with treatment or spontaneously.
See images of genital psoriasis.
Getting A Diagnosis Of Psoriatic Arthritis
The presence of psoriasis may provide an indication of psoriatic arthritis when someone develops joint symptoms. Psoriatic arthritis can develop in people with a lot or a little of psoriasis, and may be more common in people with nail psoriasis. As well as joint symptoms, psoriatic arthritis can lead to feeling tired. Many people become frustrated by a lack of diagnosis psoriatic arthritis tends to have periods of improvement and worsening, which may also be attributed to mechanical joint problems and not inflammatory arthritis.
If you have the symptoms of inflammatory arthritis, such as psoriatic arthritis, your doctor will often refer you to a rheumatologist. In some cases, further tests and imagery may be sought, although this will depend on the individual circumstances and level of confidence in the initial diagnosis.
Read Also: Psoriasis On Hands Home Remedy
What Is Genital Psoriasis
Psoriasis is a common, long-term scaly skin condition that affects approximately 2% of the population. Genital psoriasis affects the genital skin, which includes the pubic area, vulva or penis, skin folds including natal cleft, and buttocks. It is known as anogenital psoriasis when psoriasis also affects perianal skin. Psoriasis does not affect mucosal surfaces.
Psoriasis is one of the most common diseases affecting anogenital skin. It can be part of more generalisedplaque psoriasis, but it may also be the only affected area in 25% of cases. Rarely, generalised and localisedpustular psoriasis can also affect the genital skin.
Genital skin can also be affected in inverse or flexural psoriasis, psoriasis that mainly affects the skin folds. Genital psoriasis may be associated with considerable discomfort and embarrassment, and may severely impair the quality of life and sexual well-being of those affected.
What Type Of Psoriasis Treatment Will I Need
Several treatment options can relieve psoriasis. Creams or ointments may be enough to improve the rash in small areas of skin. If the rash affects larger areas, or you also have joint pain, you may need other treatments. Joint pain may be a sign that you have arthritis.
Your provider will decide on a treatment plan based on:
- Severity of the rash.
- Vitamin A or retinoid creams.
Don’t Miss: Best Treatment For Pustular Psoriasis
Causes Triggers And Risk Factors
Psoriasis develops when the body replaces skin cells too fast. Doctors do not fully understand what causes this skin condition, but they believe it to be an autoimmune disease. This means that the bodys immune system attacks healthy tissue, such as skin cells, by mistake.
A persons genes may play a role in the development of psoriasis, and it may run in families. People who have other autoimmune diseases are also more likely to develop psoriasis.
Many people with psoriasis find that certain things trigger or worsen their symptoms. Potential triggers can vary from person-to-person, but may include:
- a recent injury to the skin, such as a cut, insect bite, or sunburn
- weather changes, especially when they cause skin dryness
- an illness or infection
- certain medications
Some people first notice psoriasis after they have experienced a trigger, so may mistake their foot symptoms for an allergic reaction or an infection, such as athletes foot.
Athletes foot is a common fungal infection that occurs on the feet. Unlike psoriasis, it is contagious.
A person can get athletes foot from surfaces, towels, and clothes that have become infected with the fungus.
In most cases, athletes foot requires treatment. However, a person can usually treat the infection at home with over-the-counter antifungal medications.
Some differences between athletes foot and psoriasis include:
Who Gets Psoriasis That Affect The Joints
Years after developing psoriasis on their skin, some people get a type of arthritis called psoriatic arthritis, which affects the joints. Its also possible to develop psoriatic arthritis before getting psoriasis on your skin.
Its not possible to predict who will get psoriatic arthritis. For this reason, its important for people who have psoriasis to pay attention to their joints.
Without treatment, psoriatic arthritis can worsen and damage joints. This damage is irreversible and can cause a lifelong disability. Treatment can prevent psoriatic arthritis from worsening.
Early warning signs of psoriatic arthritis include:
-
A swollen and tender joint, especially within a finger or toe
-
Heel pain
-
Swelling on the back of your leg, just above your heel
-
Stiffness in the morning that fades during the day
Don’t Miss: Treating Plaque Psoriasis On Scalp
Acne: Blocked Pores That Lead To Pimples
Some forms of psoriasis appear as pus-filled blisters that may be confused with pimples. Pustular psoriasis forms white blisters that are filled with pus and surrounded by red skin. Far more common than psoriasis, acne also causes a pus-filled pimple eruption. However unlike psoriasis acne is caused by excess oil, blocked pores, and bacteria. Acne is common in teens and young adults and occurs on the face, neck, back, or chest. Pustular psoriasis is usually seen in adults and can occur anywhere on the body, but less likely on the face.
What Are The Symptoms Of Psoriasis
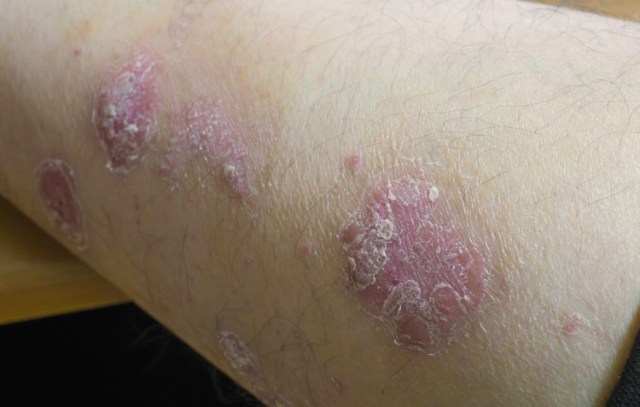
There are different types of psoriasis. The most common is chronic plaque psoriasis. This causes patches of red, raised skin, with white and silvery flakes.
It can occur anywhere on the skin, but most commonly at the elbows, knees, back, buttocks and scalp.
Psoriasis can cause small round dents in finger and toe nails, this is known as pitting. Nails can also change colour, become thicker and the nail may lift away from your finger.
Also Check: What Is Used To Treat Psoriasis
Whats Triggering Your Psoriasis Flare
Science isnt exactly sure what causes psoriasis. It seems to be a combo of genetics, environmental triggers, and your immune system going rogue against your skin cells.
If youre genetically predisposed to psoriasis , youll prob experience your first flare-up because of an environmental trigger.
Even folks with a tried-and-true treatment protocol can get flare-ups. Theres just no way to control *everything* around you and trying to control everything would be a lot of stress.
Most psoriasis flare-ups start as a small itchy patch that spreads pretty quickly. Scratching it wont speed up the spread, but it could lead to irritation and infection.
Ringworm: Fungal Infections Of The Skin And Nails
Tinea is a type of fungal infection that resembles some symptoms of psoriasis. Psoriasis can cause the thick fingernails symptomatic of fungal nail infections, and both can cause red, itchy skin rashes. When tinea grows on your skin, it can cause a scaly, red skin rash that clears in the middle, called ringworm . Fungal infections of the skin and nails can be hard to treat. Antifungal medications work, but you may need to take them for a long time.
Read Also: Psoriasis On Face And Neck
What Psoriasis Medications Can I Take
Systemic Medications
Biologics for Psoriasis
The following drugs are categorized under the term biologic because they are all proteins produced in the laboratory by industrial cell culture techniques and must be given either subcutaneously or intravenously. The frequency of treatment depends on the specific drug. All of these medications are very precise in that they block only one or two parts of the inflammatory reaction and are moderately immunosuppresive.
Biologics are expensive and do not cure psoriasis but as a group are quite effective and reasonably safe. If it is decided to start a patient on a biologic drug, the choice will depend on the particular physician’s expertise, as well as insurance coverage and payment issues.
What Can I Do To Help My Feet
The most important action is to seek advice and help when you notice any changes in your foot, whatever they may be. You can talk to your GP or local pharmacist for advice. Some problems can be resolved simply. For issues that are more persistent you may be referred to a specialist, such as a dermatologist, rheumatologist, physiotherapist, surgeon or chiropodist/podiatrist.
For general foot care, personal hygiene is important, particularly in avoiding fungal and viral infections. Change shoes and socks regularly, avoid shoes which are ill-fitting or cause bad posture. If you are overweight, losing weight could relieve the pressure on your joints and improve your walking gait.
If you are diagnosed with psoriasis, develop a treatment regime that works for you often, applying treatment after a bath or shower, along with the use of an emollient, can make the process easier.
If you have nail involvement, keep nails trimmed and clean. If they are thick, try trimming them after soaking them in a bath or shower, as this makes them softer and easier to cut. Alternatively, seek an appointment with a chiropodist, which is often available via the NHS.
If you have psoriatic arthritis, it is important to rest inflamed joints. Sourcing footwear that supports the foot and helps to reduce the pressure on the inflamed areas can help, as can inner soles and orthotic supports. Once again, a chiropodist is best placed to advise you.
This article is adapted from The psoriatic foot leaflet.
Read Also: Psoriasis En La Cabeza Tratamiento
What Is Plaque Psoriasis
Plaque psoriasis, also called psoriasis vulgaris, is the most common type.
Between 80 percent and 90 percent of people with psoriasis have this form, according to the American Academy of Dermatology.
Plaque psoriasis is characterized by raised, scaly patches of skin. On white skin, the patches, known as plaques, are often red or pink, with silvery-white scale. On skin of color plaques may appear salmon with silvery-white scale, or violet or dark brown with gray scale.
Plaques can crop up on any area of the body but are commonly found on the knees, elbows, scalp, or back.
The plaques can cause:
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Don’t Miss: Cual Es El Mejor Tratamiento Para La Psoriasis
Psoriasis Symptoms You Should Never Ignore
Psoriasis is known for symptoms you see on your skin, but this condition runs deeper than that. Psoriasis is an autoimmune disease that occurs when the immune system starts attacking healthy cells usually skin cells instead of targeting foreign bodies like bacteria and viruses.
This process can cause skin cells to turn over much more quickly than usual , which creates psoriasiss telltale scaly patches.
In most people with psoriasis, the disease goes through cycles, flaring for a few weeks or months, then subsiding for a time. It may also go into remission.
Psoriasis symptoms can vary from person to person and depend on the kind of psoriasis you have. Some people may have a few patches near their scalp or elbow others can have patches that cover much of their body.
One key thing to know about psoriasis is that its not contagious. You cant catch it by touching someone elses skin plaques.
Heres a look at the most common symptoms of psoriasis to be aware of.
What Is The Guttate Psoriasis Diet Does It Relieve Symptoms
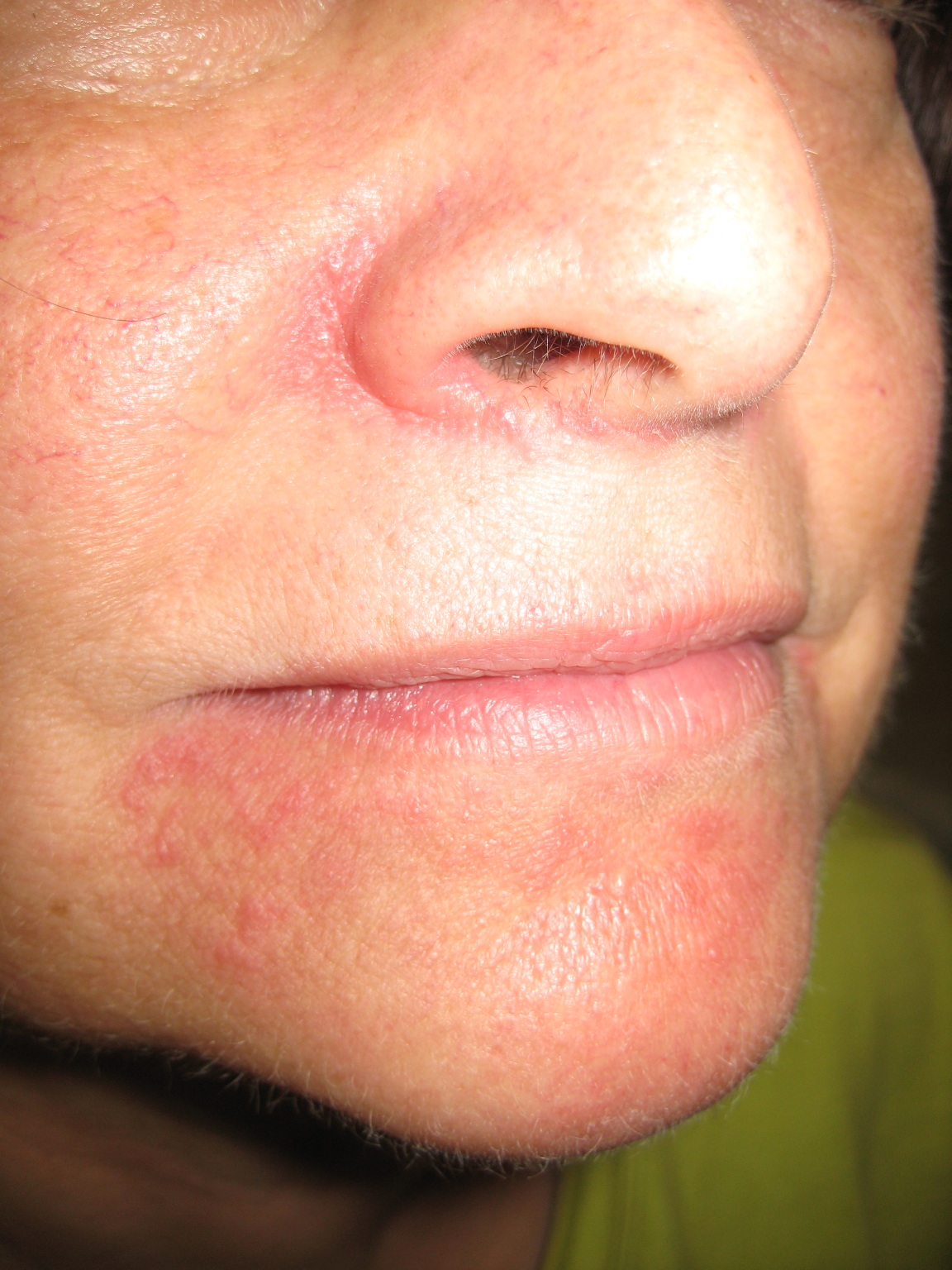
Researchers at the University of California-San Francisco School of Medicines Department of Dermatology surveyed psoriasis patients to probe linkages between diet and psoriasis symptoms. The most successful guttate psoriasis diet followed by patients, though differing vastly, had some common features:
- Reduced sugar intake.
- Avoided milk and many dairy products.
- Reduced or eliminated whole grain fiber, especially products rich in glutens. They settled for gluten-free foods such as buckwheat, corn, flax, and millets.
- Generally avoided vegetables of the nightshade family like potatoes, tomatoes, eggplant, and peppers. Pushed consumption of green leafy vegetables such as spinach and kale.
- Cut alcohol consumption substantially.
- Favored fish and lean meat to red meat.
- Took fish oil and Vitamin D supplements.
You May Like: What Are Symptoms Of Plaque Psoriasis