Will Psoriatic Arthritis Shorten Your Life Expectancy
Psoriatic arthritis is not life-threatening. However, due to the high possibility of comorbidities, other conditions that a person can have at the same time as PsA, such as cardiovascular and respiratory conditions, people with PsA may be associated with a reduced life span. But early treatment significantly improves a person’s prognosis.
Day Of Surgery: Meet Your Anesthesiologist
Make sure your anesthesiologist has reviewed your primary medical history, particularly any prior difficulties you may have had with anesthesia. For example, if you have had problems with intubation through the mouth, request intubation through the nose instead. If your surgery involves your lower extremities , discuss with your surgeon and the anesthesiologist the possibility of using a spinal block rather than intubation. Your normal cognitive function can quickly be restored, often as early as when the surgery is completed. A similar type of block, called an interscalene block, may be used with upper extremity surgery.
Diet And Psoriasis: What’s The Connection
Can your diet help keep psoriasis under control? Maybe. An observational study published online July 25, 2018, by JAMA Dermatology found that people with psoriasis who followed a Mediterranean diet an eating pattern rich in fruits and vegetables, legumes, whole grains, fish, fruit, nuts, and extra-virgin olive oil experienced fewer severe flare-ups. This was only an association and more research is needed, but experts believe the Mediterranean diet contains many foods that have an anti-inflammatory effect in the body and may offer extra protection against psoriasis triggers.
Read Also: Scalp Psoriasis Hair Loss Treatment
How Should You Care For Your Surgical Wound
Your surgeon and care team will give you exact instructions.
To lower your chances of getting an infection, be sure to ask your surgeon how theyâd like you to clean your skin while your surgical wound is healing, Davis says.
And if the skin around your incision is itchy due to psoriasis, resist the urge to scratch. Instead, talk to your surgeon and your dermatologist. They may decide to treat the psoriasis patch with a topical steroid, Madan says. Even though thatâs not a typical step to take when it comes to wound healing after surgery, he says, your dermatologist will weigh the pros and cons to figure out if itâs right for you.
What Is Plaque Psoriasis
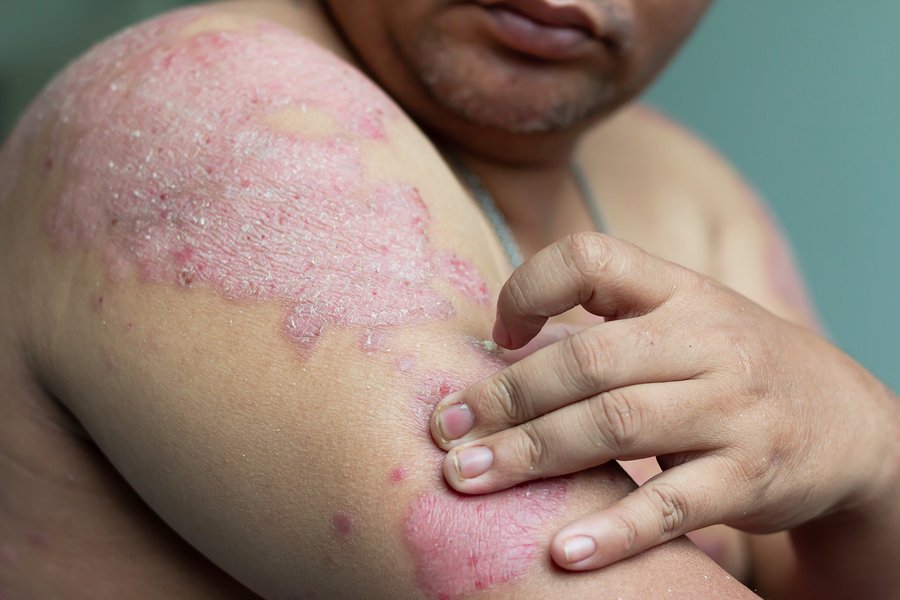
Plaque psoriasis is an inherited systemic inflammatory disease of immune dysfunction that causes plaques of elevated, scaling, inflamed skin that is often quite itchy. The plaques are characteristically found on the scalp, elbows, and knees. Plaque psoriasis is relatively common about 2%-3% of population of the United States is affected. It is not contagious.
Don’t Miss: How To Stop Itching Scalp Psoriasis
Topical Treatments For Psoriasis
For patients with mild to moderate psoriasis, the use of creams and ointments may be all that is necessary. Here are some of the options we use:
- Topical corticosteroids These drugs are the first choice for treating psoriasis. They reduce inflammation and relieve itching, and they can be combined with other treatments. Long-term use can cause the skin to thin, however, so its best to use these as a short-term treatment during flare-ups.
- Vitamin D analogues These synthetic forms of vitamin D slow the growth of the patients skin cells.
- Anthralin This drug helps slow skin cell growth and it can remove scales and make the skin smoother.
- Topical retinoids These vitamin A-based medications decrease inflammation, but they can also irritate the skin and make the skin light sensitive.
- Calcineurin inhibitors These reduce inflammation and plaque build-up, but are not good for long-term use.
- Salicylic acid Commonly used in chemical peels, salicylic acid promotes sloughing of dead skin cells and reduces scaling.
- Coal tar Coal tar reduces scaling, itching, and inflammation, but it is messy, stains clothing and bedding, and has a strong odor.
Different Types Of Psoriasis
- Plaque psoriasis This is the most common form of psoriasis, where dry, raised, red skin lesions covered with silvery scales form. Areas may be small or large, and they can occur anywhere on the body, even inside the mouth.
- Nail psoriasis Psoriasis can affect the fingernails and toenails, causing abnormal nail growth and discoloration, pitting, and even causing the nail to loosen from the nail bed or crumble.
- Guttate psoriasis This type of psoriasis is usually triggered by a bacterial infection such as strep throat, and it usually affects children and teens. Small water-drop-shaped, scaly lesions form on the trunk, arms, legs, and scalp. These lesions arent as thick as most other plaques. This type may occur just a single time, or it may have repeated episodes.
- Inverse psoriasis Its thought that fungal infections trigger this type of psoriasis. It mainly affects the skin in the armpits, groin, under the breasts, and around the genitals. Smooth patches of red, inflamed skin form, without the isolated plaques of other types. These patches worsen with friction and perspiration.
- Pustular psoriasis This is a rare form that affects the hands, feet, or fingertips. Pus-filled blisters develop quickly, appearing just hours after the skin first becomes red and tender.
- Erthrodermic psoriasis This is the least common form of psoriasis. The entire body is covered with a red, peeling rash that can itch and burn intensely.
Also Check: How To Cure Psoriasis At Home
Recovering From Psoriatic Arthritis Surgery
After surgery, your doctor may prescribe pain medications to ensure you are comfortable while you recover. You generally remain in the hospital overnight for observation.
When you are discharged, your doctor will give you a supportive splint to wear for at least two weeks. If your ankle joint is replaced, you will also need crutches during recovery to avoid putting weight on your foot and ankle.
Your doctor will schedule a follow-up appointment after 10â14 days to assess how well the affected joint is healing and to determine whether you need to continue to wear the splint. After the joint heals, your doctor may recommend four to eight weeks of physical therapy.
Depending on your health and abilities prior to surgery, the affected joints, and the success of surgery, recovery may be longer for some people than others. Joint replacement surgery recovery also depends on the job a person is returning to. If they need to be rehabilitated for physical, labor-intensive work, they may take longer to recover than a person returning to office work.
Additionally, PsA surgery can cause lingering pain. It is normal to have pain in the joint where surgery was performed. The pain can last a few weeks or months.
The Most Common Surgery For Psoriatic Arthritis: Joint Replacement
A number of surgical options are available for psoriatic arthritis, depending on the joints affected and a persons unique circumstances.
Joint replacement, also known as arthroplasty, may be the best choice when there’s severe joint damage in the hips and knees. Very often, people with psoriatic arthritis have hip and knee involvement that gets worse over time, says Bekele.
Hip replacement otherwise known as total hip arthroplasty is the most common surgery for people with psoriatic arthritis, according to the Danish review, followed by knee replacement.
Patients usually do well after allowing time for recovery and rehabilitation. Joint replacement can help people regain mobility for a decade or more, according to Bekele.
But, he warns, its best to delay surgery until absolutely necessary. Thats because these artificial joints have a 20- to 30-year shelf life. And since young people can often get PsA, you dont want to do the surgery so early that, at some point, those artificial joints wear out and a second surgery is needed.
One potential way to delay joint replacement is to first turn to a procedure called synovectomy, or removal of the synovium a layer of tissue that lines and lubricates the joints.
When psoriatic arthritis aggravates this lining, it creates an excessive amount of fluid that erodes the cartilage. This causes pain and stiffness and eventually bone rubbing against bone. A synovectomy can help stop this joint pain.
Also Check: Best Treatment For Psoriasis In Hair
Prevalence Of Nonadherence In Psoriasis
Prevalence of nonadherence in psoriasis
EMR Electronic Medical Records, UVB Ultravioler B, TNF- Tumor necrosis factor-alpha
Psoriasis patients had the lowest rate of primary adherence compared to other chronic dermatologic conditions, with 44% of psoriasis patients failing to fill their prescriptions . In a study assessing adherence to both topical and oral psoriasis treatments, mean medication adherence was 60.6% when assessed by pill count and medication weight while self-reported adherence rates by patient interview were 92.0%. Both self-reported measures and medication weights tend to overestimate adherence rates compared to electronic monitoring . Electronic monitoring may consists of a microchip installed into the medication cap to record the opening and closing of the bottles. Electronic monitoring measured an adherence rate of 67% compared to 92% as recorded by psoriasis patient diaries .
Adherence rates also vary widely depending on treatment modality. In a self-reported questionnaire, adherence rates were 100% for biologics, 96% for oral medications, 93% for phototherapy, and 75% for topical therapies however, these rates are likely inflated given that the measurements were self-reported and subjective .
What Does The Koebner Phenomenon Look Like
Koebner lesions tend to have the same features as a persons existing psoriasis plaques. The new lesions can be raised, discolored, scaly, itchy, and painful. They can also crack and bleed.
These new psoriatic lesions also tend to follow the lines or shape of the injury itself, Soleymani notes. Psoriasis can be itchy, and you can often see clear linear streaks of psoriasis plaques develop where the nails frequently scratch, he explains.
In many cases, Koebnerization will occur within days of an injury in other cases, new plaques might not show up until years later. As a result, you might not make the association between a scratch, scrape, or chronic irritation and a new flare.
How quickly the Koebner phenomenon occurs seems to depend on the degree of irritation or trauma, Soleymani says. With a deep scratch, surgical wound, or sunburn, the Koebner phenomenon can occur a few days or a week later. With milder injuries, such as chronic rubbing or irritation, it could be many years before you see new plaques develop.
RELATED: Is That Rash Psoriasis, or Is It Something Else?
Recommended Reading: How To Loosen Psoriasis Scales On Scalp
Your Temporary Nighttime Routine
For the first few days after surgery, you may need the assistance of another person to lift your legs onto the bed. Try to sleep at least 6 inches from the edge of the bed. For the first week or two after surgery, sleep on your back and not on the side that was repaired.
When getting into bed, use the non-repaired leg to lift the repaired leg, or pull up on the repaired leg gently to swing the leg into the bed. Use the non-repaired leg to slide the repaired leg farther into the bed. Sleeping with a pillow between your legs and a pillow under your arm helps minimize some of the movements that occur during sleep and may allow for a better nightâs sleep.
Place a pillow under your legs only if recommended by the surgeon.
Before getting out of bed, sit on the side of your bed to check for dizziness. When you first stand up, you can stand or march in place for a few seconds to ensure you have your balance before starting to walk. You may need a walker or cane at first.
Use Gentle Chemical Exfoliants
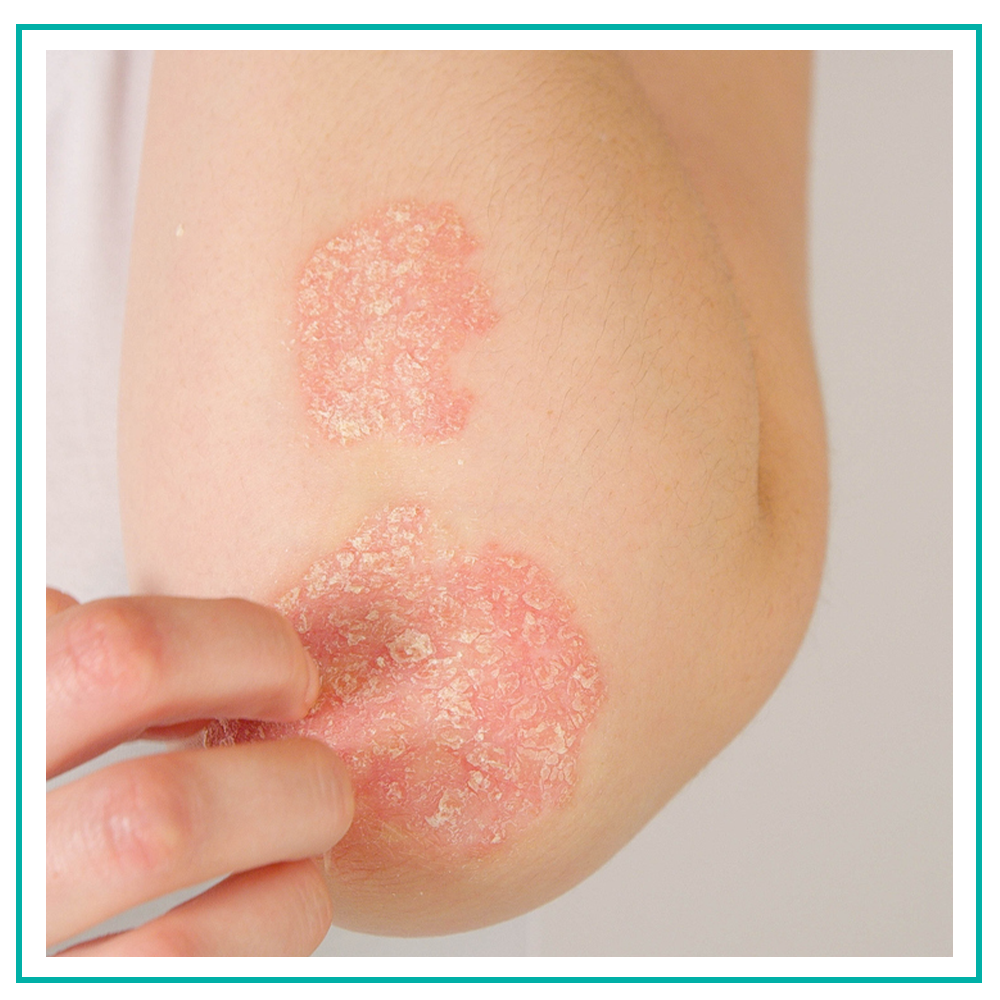
The American Academy of Dermatology stresses the importance of using active ingredients to remove scales from your skin. This is important because they soften the attachment of the scale to the skin, making the scales easier to remove.
Locate the scales that you want to remove
Your approach will be different if the scales are hidden under hair, sitting right at your hairline, or behind your ears.
Choose a spot treatment or shampoo
If your scales are surrounded by hair, its best to use a medicated shampoo to soften them. Although shampoos have milder ingredients than topical spot treatments, they provide the added benefit of gentle physical exfoliation.
A spot treatment might have stronger ingredients and should be applied directly onto hairless skin.
Choose your ingredients
Look for the following ingredients, either in shampoos or topical creams:
- Salicylic acid is a powerful exfoliating ingredient that can be found in shampoos and creams. It helps lift and soften scaling and is best as a spot treatment. Shampoos with salicylic acid should be used sparingly, as they can dry your scalp and may lead to more flaking.
- Coal tar is one of the most common ingredients in psoriasis shampoos. It helps soften any scaling on the scalp.
- Lactic acid and urea work similarly to salicylic acid. Theyre scale lifters that soften and break down the thickness of your flakes. They can be found in shampoos or spot treatments.
Don’t Miss: Guttate Psoriasis Vs Pityriasis Rosea
How Successful Are The Treatments
Anti-inflammatory drugs can help to reduce pain, swelling and stiffness. Unfortunately, however, they can make skin symptoms worse in some people. Steroid injections to joints may give relief. Diseasemodifying drugs such as methotrexate can dampen down both skin and joint symptoms, as can targeted biologic agents.
In some cases, surgery to remove a thickened synovial membrane , realign a joint or to fuse a joint may stop pain which results from movement.
Sometimes it is possible to remove the painful end of a bone .
Remember: All treatments may have unwanted side effects or require special precautions . Always make sure you have all the information before embarking on any course of therapy this includes reading the patient information leaflets provided with your medicines.
Benefits And Risks Of Psoriatic Arthritis Surgery
Surgery offers significant pain relief for severe cases of PsA. It can repair the damage the condition has done and allow you to participate in day-to-day life with improved symptoms.
Many prosthetic joints last for years. However, a prosthetic joint can wear out and become unstable. Your surgeon may schedule annual follow-up appointments to monitor the implanted joint and, if necessary, explore surgical options to repair or replace aging parts.
However, sometimes a joint replacement doesn’t improve symptoms as much as expected. This is an unfortunate but possible circumstance and should be taken into account before you decide to get surgery. Also, while rare, there is a chance the replacement will have issues like dislocation.
Other things to consider before surgery are recovery time and postsurgical care. Recovery time depends on the extent of your surgery, the joint operated on, and your daily tasks. If you have a sedentary lifestyle and career rather than physically demanding ones, recovery periods can be shorter. A hip replacement surgery, for example, may take two to four weeks to recover, but times can vary.
To benefit the most from replacement surgery, pre- and postsurgical physical therapy is required. PT before surgery allows the therapist to get a better understanding of your needs and capabilities and how best to treat you after your operation.
Also Check: Home Remedies For Psoriasis On Your Head
Dermatologists Located In Brookline Ma & Andover Ma
Psoriasis is a chronic, inflammatory disease that causes your skin cells to grow much faster than usual. Plaque psoriasis, the most common type, causes red, raised patches of skin covered with silvery-white scales. The skin disease experts at Integrated Dermatology of Brookline provide advanced management strategies for people of all ages with psoriasis. Call your nearest office in Brookline or Andover, Massachusetts, today, or book an appointment with Dr. Rockoff or Dr. Wang online at any time.
Psoriasis And Elective Foot Surgery
The authors present a brief overview of the dermatologie condition, psoriasis. Special attention is given to a review of the literature as it addresses surgery and the psoriatic patient. The authors conclude that psoriatic patients are somewhat more susceptible to postoperative infection, but with proper precautions, complications can be avoided. Therefore, the condition of psoriasis is not an absolute contraindication to elective foot surgery.
- Previous article in issue
You May Like: Cuã¡l Es La Mejor Crema Para La Psoriasis
Hair Transplant Psoriasis Aftercare
In general, follow the aftercare instructions that your surgeon provides following a hair transplant psoriasis. You have to be extra careful in avoiding all those things that can trigger scalp psoriasis, such as infection, itching, smoking, stress, prolonged sun exposure, etc. Other than that, the surgeon may prescribe you some corticosteroids to avoid a flare-up.
You should also wear sunblock. You might need to use a special shampoo, the usage of which you can discuss with your surgeon. Well closely follow your hair transplant psoriasis recovery. If any flare-up occurs, you should inform us. Make sure that you keep your scalp clean at all times.
Youll be requested to share your pictures with our Aftercare team during your recovery. Our hair transplant surgeons can suggest you see your dermatologist if any flare-ups occur after hair transplant psoriasis. Looking after your transplanted areas well if you suffer from psoriasis is important in maintaining good results.
More Than Skin Troubles
A 2017 study from the Journal of the American Academy of Dermatology found that people with psoriasis that covers 10% of their body or more are 64% more likely than those without psoriasis to develop type 2 diabetes. “About 30% of people with psoriasis also might develop psoriatic arthritis, which causes destructive inflammation in your joints,” says dermatologist Dr. Gideon Smith. Psoriasis also may signal a higher risk for fatty liver disease and heart attacks.
Also Check: Mejor Medicina Para La Psoriasis
Is There A Treatment For Psoriasis
Before treatment comes the diagnosis. For that, youd need to go to a doctor for a physical examination. You might get a diagnosis through a physical exam, or the doctor might send a small piece of your skin, in a medical test called a biopsy, for testing in a laboratory. This can help the doctor determine the type of psoriasis that the person is suffering from.
Psoriasis is a chronic, lifelong condition. It has no cure. However, there are treatments available for it. Topical treatments include:
- Creams
- Salicylic acid
- Vitamin D analogues
These are part of the treatment for many people with psoriasis. Some people also need to get injections or take oral medications.
Psoriasis can significantly impact the quality of life of a person. The appearance of the skin can also become a cause for low confidence among individuals with psoriasis. Different treatments can help them better manage their condition.
Moreover, there are some tips suggested for scalp psoriasis. To make sure that the scalp doesnt get dry, a conditioner can help. Similarly, avoid any products that can dry out the scalp. This includes various hair-styling products. Ice packs can also help with irritation on the scalp.