Integrative Approaches To Care
The use of natural treatment options can be effective for some individuals when used in conjunction with traditional treatment options. The National Psoriasis Foundation suggests that you talk with your health care provider before trying any integrative treatment approaches, and especially before taking any herbal remedies to avoid dangerous interactions with your medications. Also, you should not take some herbal remedies if you are pregnant or breastfeeding or if you have pre-existing medical conditions such as diabetes, high blood pressure or mood disorders. Stop usage and consult your health care provider immediately if you experience side effects.
What Are The Clinical Features Of Palmoplantar Psoriasis
Palms and soles affected by psoriasis tend to be partially or completely red, dry and thickened, often with deep painful cracks . The skin changes tend to have a sharp border and are often symmetrical, ie similar distribution on both palms and/or both soles. At times, palmar psoriasis can be quite hard to differentiate from hand dermatitis and other forms of acquired keratoderma. Plantar psoriasis may sometimes be similar in appearance to tinea pedis. There may be signs of psoriasis elsewhere.
Palmoplantar psoriasis tends to be a chronic condition, ie, it is very persistent.
Compared to chronic plaque psoriasis on other sites, palmoplantar psoriasis is more commonly associated with:
Animal Models For Pustular Psoriasis
Psoriasis is a disease unique to humans. However, certain aspects of the disease, such as activation of specific inflammatory pathways or infiltration of specific leukocyte populations such as neutrophils, can be modeled in mice. These models can be transgenic, xenografts, or induced via intradermal cytokine injection or via topical application of the TLR7 agonist imiquimod . We will address some of the mouse models that may have applicability for the study of GPP. No models currently exist to model PPP or ACH.
As discussed above, IL-36 activation is central to pustular psoriasis pathogenesis. Transgenic mice directing overexpression of the Il36a gene to the epidermis with the keratin 14 promoter were found to be small and showed flaky skin. Histology revealed a thickened epidermis, with leukocyte infiltration and increased expression of neutrophil chemokines. Interestingly, this phenotype peaked at postnatal day 5 and resolved by postnatal day 21. However, when these mice were backcrossed to Il36rn/ mice, they developed a dramatically more severe skin phenotype characterized histologically by intracorneal and intraepithelial pustules, parakeratosis and dilated superficial dermal blood vessels. Intradermal injection of Il-36 into mouse skin, has been used to induce an inflammatory phenotype, but this phenotype is less robust than the transgenic Il36rn/ model.
Recommended Reading: Fastest Way To Get Rid Of Psoriasis
Von Zumbusch Pustular Psoriasis
von Zumbusch psoriasis, or acute generalized pustular psoriasis, is the most severe type of pustular psoriasis. Its very rare.
It begins with painful areas of red skin. Pustules form within hours and dry up in 1 or 2 days.
von Zumbusch psoriasis can recur in cycles, returning every few days or weeks. Its rare in children, but when it does occur the outcome is better than when it appears in adults. In children, the condition often improves without treatment.
Symptoms may include:
Immediate medical care is necessary for this condition. Over time, von Zumbusch psoriasis can cause weight loss and exhaustion.
Potential complications include hair and nail loss, secondary bacterial infection, and liver damage. If left untreated, it can lead to cardiorespiratory failure.
What Are Causes And Risk Factors Of Pustular Psoriasis
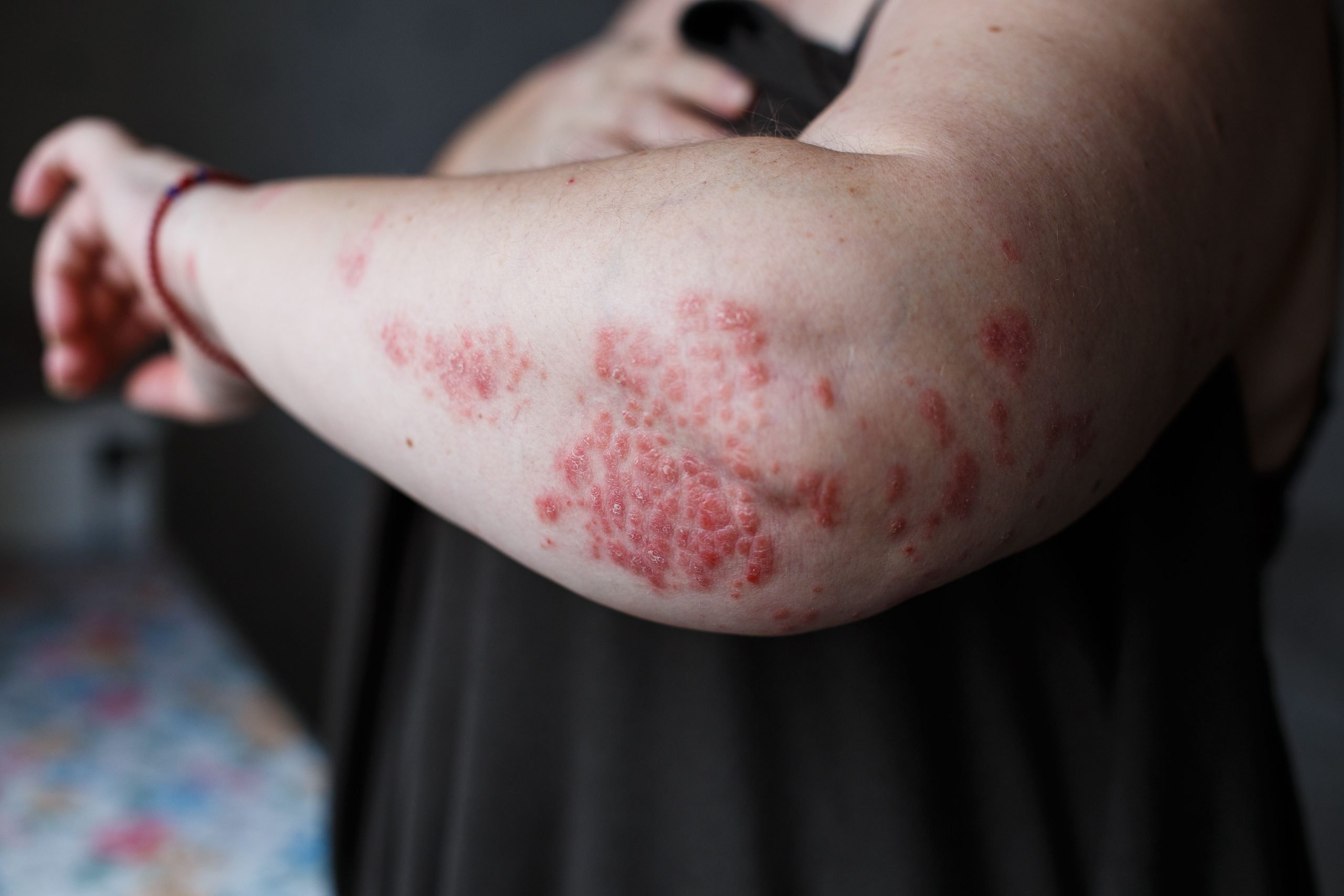
To understand pustular psoriasis, one must recognize aspects of classical plaque-type psoriasis. It is generally agreed that a combination of genetics and environment induces psoriasis, including this pustular subtype. Below is a list of factors that are known to exacerbate pustular psoriasis:
- Acutely stopping high-dose systemic steroids
- Various medications have been associated with exacerbations of psoriasis, including the following:
- Oral iodides
- Interferon alfa and recombinant interferon-beta injections
In most people, a trigger for the disease is never identified.
You May Like: Medical Treatment For Scalp Psoriasis
Best For Skin Tears: Emuaid Over The Counter Ointment For Psoriasis
If you often find yourself scrambling for convenient and suitable ointment, Emuaid Over The Counter Ointment For Psoriasis is your solution. The emuaid over the counterointment forpsoriasis is allergic, found in nature and it is absolutely amazing. It has a unique delivery system that helps carry powerful healing ingredients deep into your nails and skin. These statements on this page have not been evaluated by the fda.
The ointment can deal with flare-ups and it works on nail fungus. Further, it is ideal for trouble spots, is best for coconut oil and it is great for apple cider. Finally, the emuaid over the counter ointment for psoriasis is used for painful conditions and it works very well.
Most buyers find that the ointment it takes for these marks to disappear depends on the severity and cause of your condition. In addition, a few strongly agree that the ointment is good for some things, over-sold for others.
Top Customer Quotes:
Read Also: Cosentyx Dosing Schedule For Psoriasis
Finding The Right Psoriasis Treatment:
Heres one of the challenging things about treating psoriasis: Your body can build up a tolerance to a certain medications, so something that seemed magical in its ability to bring you relief could suddenly stop working. On the other hand, a treatment that didnt work for you years ago could suddenly work wonders.
Thats why trial and error is a necessary part of psoriasis treatment. Finding the right treatment for psoriasis is much like finding the right partner. It may take some dating until the right one finally comes along, says Dr. Gohara. Some may work for a bit, but then efficacy fizzles. Topical steroids are the most common culprit of this phenomenon, although it may happen with other topical or systemic medication as well.
Read Also: Castor Oil For Psoriasis On Scalp
Derma Ced Deep Therapy Cream
The main ingredient of this product is its active ingredient of colloidal oatmeal. This type of oatmeal has been for centuries in the immediately calming itchy skin, and help soothes down skin irritation upon contact. It also has a high concentration of beta-glucan, which creates a water-holding barrier that draws in moisture to protect your skin.
The beta-glucan also simultaneously reduces your skin inflammation, softens skin with anti-oxidants, provides the great anti-itch effect, and can even trigger your immune cells to start up its healing process.
The oils that are in this product moisturize your skin better, as it needed a lot of moisture more than anything. Not only is this cream great for those who have psoriasis, but they also work great for eczemas.
What Is Palmoplantar Pustulosis
Palmoplantar pustulosis causes blister-like sores on the palms of your hands and the soles of your feet. It can also cause cracked skin or reddened, scaly patches. It’s an autoimmune disorder, which means your immune system attacks healthy parts of your body.
There’s no cure for PPP, but a dermatologist can treat it. Sometimes it comes back. But it could go away and never return.
Recommended Reading: Halobetasol Propionate Ointment For Psoriasis
Enhancing Healthcare Team Outcomes
Palmoplantar psoriasis is best managed by an interprofessional team that also includes the nurse and pharmacist. There is no cure for this disorder and at some point, drug treatment is required. The constant itching and pain and results in a poor quality of life, hence, healthcare workers should take steps to reduce triggers and educate patients on medication compliance. In addition, patients should be encouraged to discontinue smoking. The pharmacist should emphasize the importance of medication compliance. A wound care nurse should educate the patient on the importance of skincare.
The outcomes for most patients with palmoplantar psoriasis are guarded relapses are common and eventually most patients require the potent biological agents, which have their own adverse reactions.
Conditions Associated With Palmoplantar Pustulosis
Certain conditions have been reported to occur in patients with palmopustular pustulosis more often than in unaffected patients.
- Chronic plaquepsoriasis
- Autoimmune diseases particularly gluten sensitive enteropathy , thyroid disease and type 1 diabetes.
- Streptococcal tonsillitis.
- Rarely, synovitisacnepustulosishyperostosisosteomyelitis syndrome.
Palmoplantar pustulosis may rarely be provoked by the tumournecrosis factor -alpha inhibitors .
Recommended Reading: Is Plaque Psoriasis An Autoimmune Disease
What Is Pustular Psoriasis With Respect To Palmoplantar Pustular Psoriasis & Palmoplantar Pustulosis
There is an argument concerning this entity is it one and the same disease? According to studies, there is no real answer at the moment. However, the clinical features are very similar. Therefore, they are defined together. In general, the condition presents itself with one or more plaques. The resulting pustules are either greenish or yellowish. You can best understand this argument by checking pustular psoriasis pictures. Some systematic symptoms can actually be associated with palmoplantar Pustulosis the popular ones being hyperostosis and acne.
What Is The Treatment For Palmoplantar Psoriasis
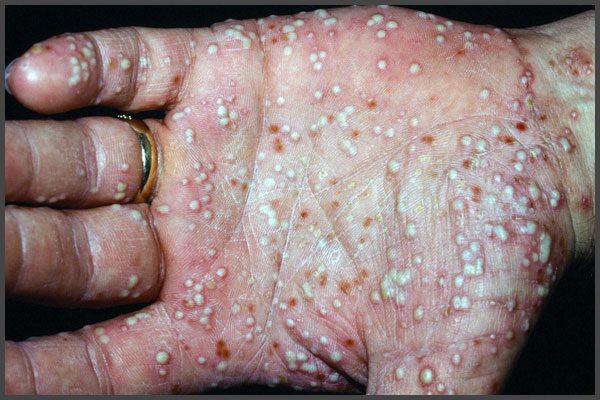
Improvement in general health can lead to an improvement in palmoplantar psoriasis.
- Weight loss, if overweight
- Investigation and management of associated health conditions
Mild psoriasis of the palms and soles may be treated with topical treatments:
- Emollients: thick, greasy barrier creams applied thinly and frequently to moisturise the dry, scaly skin and help prevent painful cracking.
- Keratolytic agents such as urea or salicylic acid to thin down the thick scaling skin. Several companies market effective heel balms containing these and other agents.
- Coal tar: to improve the scale and inflammation. Because of the mess, coal tar is often applied at night under cotton gloves or socks.
- Topical steroids: ultrapotent ointment applied initially daily for two to four weeks, if necessary under occlusion, to reduce inflammation, itch and scaling. Maintenance use should be confined to 2 days each week to avoid thinning the skin and causing psoriasis to become more extensive.
Calcipotriol ointment is not very successful for palmoplantar psoriasis. It may also cause an irritant contact dermatitis on the face if a treated area inadvertently touches it. Dithranol is too messy and irritating for routine use on hands and feet.
More severe palmoplantar psoriasis usually requires or systemic agents, most often:
You May Like: Tea Tree Oil For Psoriasis Reviews
Supplements And Alternative Treatments
The National Psoriasis Foundation suggest some herbs and natural remedies that may help with psoriasis in general.
- Tea tree oil: Always dilute with a carrier, such as almond oil, before applying. Do not take by mouth. Some people may have an allergic reaction.
- Epsom or Dead Sea salts: Add these to lukewarm water to soak the hands or feet.
- Oats: You can add these to a soak or a bath.
- Apple cider vinegar: Apply directly to the skin or dilute in equal parts with water. You can also add it to salads to take it by mouth.
- Capsaicin: Some people find that applying a cream containing the spicy ingredient in chili peppers to the skin may help reduce itching and burning.
- Mahonia Aquifolium: Also known as Oregon grape, applying a 10-percent topical cream may help reduce mild to moderate symptoms of psoriasis.
- Turmeric: Adding this spice to food or taking supplements may help with some types of psoriasis.
Ask a health professional before using any of these, to make sure they are safe and suitable for you to use.
Apply a small amount to a small area of skin to check your reaction, in case you have an allergy or the treatment makes symptoms worse.
A Blend Of Coconut Oil & Aloe Vera
Melt half a cup of virgin coconut oil extract. Add the melted coconut to a third cup of aloe Vera gel, and stir for a few minutes to mix. Then add to the mixture three drops of peppermint, rose, and lavender essential oils. Pour the blend in a clean, dark-colored, airtight glass bottle, and store it for a few hours. Do a patch test by applying small amount of the mixture on your skin. If there is no reaction, go ahead and apply the mixture on the affected parts of your skin, and leave it overnight. When you wake up the following morning, wash off the mixture off your skin with lukewarm water. Repeat the application as necessary.
Read Also: Does Psoriasis Get Worse Before It Gets Better
World Psoriasis Day 29 Octobre 2022
You may have palmoplantarpustular psoriasis if you are experiencing pustular-type blisters and scalingon the palms of your hand or on the soles of your feet. Of course, you need toget a true diagnosis, but sometimes knowing what youre dealing with can helpyou know when its actually time to make that doctors appointment.
Acrodermatitis Continua Of Hallopeau
Acrodermatitis continua of Hallopeau is another rare type of palmar-plantar pustular psoriasis. It is characterised by skin lesions on the ends of the fingers, including the nails which can sometimes become completely destroyed, and sometimes on the toes. The eruption sometimes starts after localised physical trauma. Often the lesions are painful and disabling, with the nails deformed, and bone changes may occur. This condition is quite hard to treat satisfactorily.
Don’t Miss: How To Stop Itching Skin From Psoriasis
Is It Possible To Prevent Pustular Psoriasis
- Avoiding environmental factors that trigger psoriasis, such as smoking, sun exposure, and stress, may help prevent or minimize flare-ups of psoriasis. Sun exposure may help in many cases of psoriasis and aggravate it in others.
- Alcohol is considered a risk factor for psoriasis in young to middle-aged men. Avoid or minimize alcohol use if one has psoriasis.
- There are no specific dietary restrictions or supplements for psoriasis, other than to consume a well-balanced and adequate diet.
How Is Psoriasis Diagnosed And Treated
Psoriasis often has a typical appearance that a primary care doctor can recognize, but it can be confused with other skin diseases , so a dermatologist is often the best doctor to diagnose it. The treatment of psoriasis usually depends on how much skin is affected, how bad the disease is , or the location . Treatments range from creams and ointments applied to the affected areas to ultraviolet light therapy to drugs . Many people who have psoriasis also have serious health conditions such as diabetes, heart disease, and depression. Some people with psoriasis also have an inflammatory condition which affects their joints, called psoriatic arthritis.
Psoriatic arthritis has many of the same symptoms as other types of arthritis, so a rheumatologist is often the best doctor to diagnose it. The treatment of psoriatic arthritis usually involves the use of drugs .
Psoriatic disease may be treated with drugs or a combination of drugs and creams or ointments.
Also Check: Psoriasis Treatment Center Of Central New Jersey
Read Also: How To Cure Psoriasis Permanently
Why The Heck Do I Have Psoriasis On My Hands
In March 2019, I noticed a small red irritated patch on my right palm. I ignored it for some time, thinking that I had simply gotten into something that irritated my skin.
It took me about a month or more to realize what it was pustular psoriasis. My old friend is back to teach me another lesson.
The National Psoriasis Foundation notes the following about Pustular Psoriasis:
Symptoms
Pustular psoriasis is primarily seen in adults. It may be limited to certain areas of the body for example, the hands and feet. Generalized pustular psoriasis also can cover most of the body. It tends to go in a cycle with reddening of the skin followed by pustules and scaling.
Triggers
- Emotional stress
- Sudden withdrawal of systemic medications or potent topical steroids
Palmoplantar pustulosis causes pustules on the palms of the hand and soles of the feet. It commonly affects the base of the thumb and the sides of the heels. Pustules initially appear in a studded pattern on top of red plaques of skin, but then turn brown, peel and become crusted. PPP is usually cyclical, with new crops of pustules followed by periods of low activity.
Going through the checklist, the most likely culprits are stress and sudden withdrawal of systemic medication.
Pustular Psoriasis Of Pregnancy
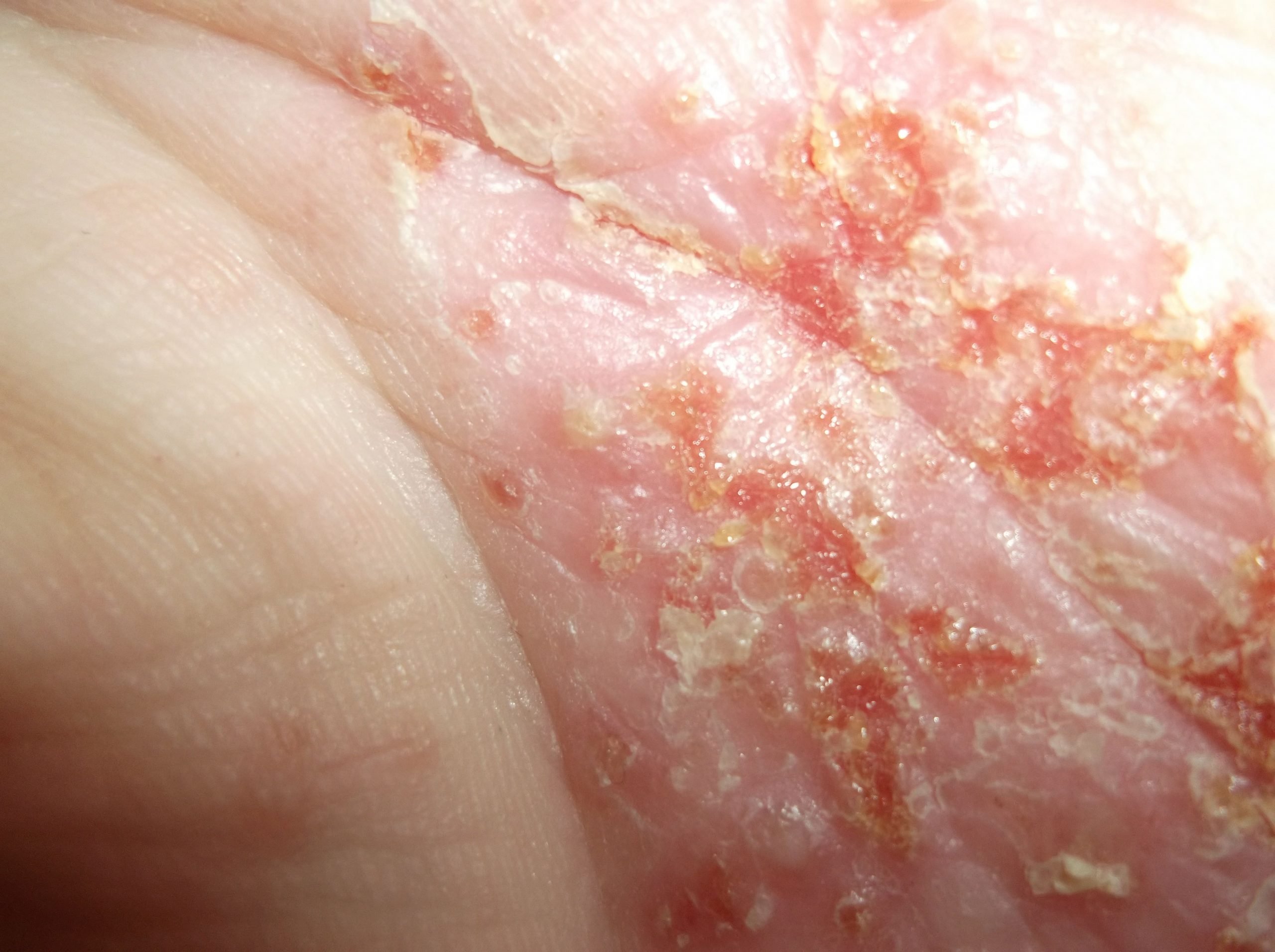
Pustular psoriasis of pregnancy, also called impetigo herpetiformis, is a very rare variant. It can be life threatening for the mother and fetus if its not treated.
Pustular psoriasis of pregnancy most often appears early in the third trimester. It can reappear in future pregnancies, usually at an earlier stage.
Symptoms may include:
- pus-filled bumps on the inner thighs and groin that join together and spread
- pustules in the mouth and under the nails
Although the exact cause is unknown, some possible risk factors may be a family history of psoriasis or a gene mutation triggered by increasing levels of progesterone.
Your treatment will depend on the type of pustular psoriasis you have and how serious it is. Sometimes it takes several tries or a combination of treatments to find the most effective approach.
Your doctor will probably prescribe ointments first because they can soothe your skin and reduce inflammation.
UV light, both natural and artificial, is used to treat psoriasis. PUVA therapy is a combination of UV light and psoralen, an oral medication that makes your skin more sensitive to it. PUVA stands for psoralen plus ultraviolet A.
Your doctor may also prescribe medications like:
- acitretin , an oral retinoid
- cyclosporine
- tumor necrosis factor-alpha blockers like infliximab , adalimumab , and etanercept
- interleukin-12/23 inhibitors like ustekinumab
TNF-alpha blockers and interleukin-12/23 inhibitors belong to a group of powerful drugs known as biologics.
You May Like: What Does Psoriasis Look Like On A Black Person
Supporting Acts: Indispensable Players In The Ensemble Of Psoriasis Immunology
Autoantigen presentation alone does not suffice to induce the psoriatic cascade in genetically predisposed individuals. Rather, costimulatory effects of various gene products orchestrate the activation of the actual autoimmune response. Such risk gene variants modulate inflammatory signaling pathways , peptide epitope processing and/or Th/c17 differentiation .
Table 1. Genetic factors implicated in psoriasis.
These genetic variations create costimulatory signals which modulate innate and adaptive immune mechanisms and shape the proinflammatory environment. In sum and in conjunction with the appropriate HLA molecules and autoantigens, they may eventually exceed the thresholds for activation and maintenance of pathogenic autoimmune and autoinflammatory responses in psoriasis . Likewise, regulatory mechanisms involving programmed death -1 signals have emerged recently as modulators of chronic inflammation in psoriasis . However, the complex interactions of various players are by no means fully understood. Therefore, they are listed here only as a whole.
The autoantigens described so far cannot fully explain the genesis of psoriasis. To give just one example of the latter notion: Psoriatic lesions can also occur in vitiligo foci that do not contain melanocytes . Alterations of resident cell types such as vascular endothelial cells or the cutaneous nervous system are also involved in the disease process . Further research is certainly needed here.