Psoriasis And Your Genes
Psoriasis is often diagnosed in people ages 15 to 35, but it can affect anyone regardless of age, including children. According to the National Psoriasis Foundation, about one-third of the people who get psoriasis are under age 20, and around 20,000 new diagnoses every year are children under the age of 10.
Genetics becomes important when one parent has psoriasis. According to the National Psoriasis Foundation, having a parent with the condition gives you a 28% chance of having psoriasis. If both of your parents have the condition, your risk jumps to 65%.
Researchers believe that mutated genes, in combination with environmental triggers, must interact to cause a person to develop psoriasis.
While rare, it is possible to get psoriasis without a family history, but the chance applies to a small group. In this case, a person has spontaneous gene mutations that can lead to psoriasis when triggered by environmental factors.
What Should You Do If You Develop Another Type Of Psoriasis
Life-threatening signs and symptoms, such as redness that covers most of your body, fever, and chills, require immediate medical care.
When signs and symptoms are not life threatening, you should see a board-certified dermatologist for a diagnosis. Youll find pictures of the different types of psoriasis and learn more about the possible signs and symptoms at Psoriasis: Signs and symptoms
ImagesImage 1: Getty ImagesImage 2: J Am Acad Dermatol 2013 69:245-52.
ReferencesBrummer GC, Hawkes JE, et al. Ustekinumab-induced remission of recalcitrant guttate psoriasis: A case series. JAAD Case Rep. 2017 3: 4325.
Egeberg A, Thyssen JP, et al. Prognosis after hospitalization for erythroderma. Acta Derm Venereol. 2016 96:959-92.
Gottlieb A, Korman NJ, et al. “Guidelines of care for the management of psoriasis and psoriatic arthritis: Section 2. Psoriatic arthritis: Overview and guidelines of care for treatment with an emphasis on the biologics. J Am Acad Dermatol 2008 58:851-64.
Gudjonsson JE and Elder JT. Psoriasis. In: Wolff K, Goldsmith LA, et al. Fitzpatricks Dermatology in General Medicine. McGraw Hill Medical, New York, 2008:178-81.
Khosravi H, Siegel MP, et al. Treatment of Inverse/Intertriginous Psoriasis: Updated Guidelines from the Medical Board of the National Psoriasis Foundation. J Drugs Dermatol. 2017 16:760-6.
Navrotski BRF, Nihi FM, et al. Wet wrap dressings as a rescue therapy option for erythrodermic psoriasis. An Bras Dermatol. 2018 93:598-600.
What Makes Psoriasis Worse
Speaking of making a bad situation worse, if you already have the chronic condition, certain things can increase its severity or trigger a recurrence, even if youve been in remission for a while. The most common triggers are:
-
Medications: If you already have psoriasis, certain prescription meds may make it worse or bring on a flare while youre taking them, or after you stop. These drugs include:
-
Antimalarial medications
-
Inderal for high blood pressure
-
Indomethacin, a nonsteroidal anti-inflammatory used for arthritis
-
Lithium
-
Prednisone, prescribed for various conditions that cause inflammation
-
Quinidine, a heart medication
If you have psoriasis, talk to your doctor before taking a new prescription drug to see if there is a skin-friendly alterative. It’s not always an option, and unfortunately, even if you do discontinue a medication that appears to be worsening your skin condition, that doesnt guarantee flares wont occur in the future.
Its important to note that what sets off one persons psoriasis might not affect anothers at all. Be your own detective to ID your specific triggers. If your psoriasis acts up before your wedding, an important job interview, or a big presentation, stress is likely a trigger for you. If it rears its ugly head while youre taking certain medications, they could be a cause. Knowing your personal triggers so you can avoid them may help you ward off a future flare-upor at least lessen its severity.
Also Check: How To Get Psoriasis Out Of Ears
Possible Causes For Psoriasis Remission
The goal of psoriasis treatment is to reduce the symptoms and hopefully end the flare. If treatments are successful, psoriasis may go into remission.
Even without treatment, psoriasis may disappear. Spontaneous remission, or remission that occurs without treatment, is also possible. In that case, its likely your immune system turned off its attack on your body. This allows the symptoms to fade.
This doesnt mean that you wont ever have another flare. Watch for symptoms of psoriasis so that you can begin treating them if they reappear.
Is There A Timeline For Psoriasis Remission

Psoriasis is unpredictable, and psoriasis remission has no timeline. Sometimes, remission can be lengthy. You may not experience symptoms for months, even years. Remission can also be short-lived. You may start experiencing symptoms again within a few weeks of them disappearing.
One common psoriasis cycle involves having fewer symptoms and flares during summer months and more symptoms and flares during winter months. Thats likely because of how the two very different environments affect your skin. The weather in these two seasons can trigger psoriasis symptoms. Being aware of these triggers and others can help you reduce flare frequency and extend remission periods.
Although psoriasis may return on its own, something may prod its return. These things are called triggers. Being aware of the most common ones can help you reduce the likelihood of flares and possibly extend periods of remission.
Recommended Reading: Cerave Psoriasis Moisturizing Cream Walgreens
Psoriatic Arthritis: What Is The Connection
Psoriatic arthritis : 1 in 4 of people with psoriasis may develop an associated arthritis called psoriatic arthropathy, which causes pain and swelling in the joints and connective tissue, accompanied by stiffness particularly in the mornings and when rising from a seat. Most commonly affected sites are the hands, feet, lower back, neck and knees, with movement in these areas becoming severely limited. Chronic fatigue is a common complaint linked with this condition. If you are experiencing mild aches and pains and have psoriasis, even very mildly, consult your dermatologist for further advice and if necessary a referral to a rheumatologist for further assessments. For more detailed information on psoriatic arthritis see What is Psoriatic Arthritis?
An Overactive Immune System
Psoriasis is considered an autoimmune condition. This means your immune system is a bit overzealous, causing immune cells to start attacking healthy tissuein this case, your skinas if it was an invader. The attack causes an inflammatory cascade as white blood cells go to war with skin cells, causing them to grow more quickly and thickly than they should. In turn, this results in the formation of those painful psoriatic patches.
Also Check: Will Vitamin C Make Psoriasis Worse
How Many People Have Psoriasis
Psoriasis is a fairly common skin condition and is estimated to affect approximately 1%-3% of the U.S. population. It currently affects roughly 7.5 million to 8.5 million people in the U.S. It is seen worldwide in about 125 million people. Interestingly, African Americans have about half the rate of psoriasis as Caucasians.
Psoriasis And Complications From Live Vaccines
Despite lots of research, there is no evidence that any vaccine makes psoriasis worse. The reason you want to avoid live vaccines though is that they may be too strong for your bodys defense system, or your immune system, to handle.
This is especially true if you are taking medications that blunt your immune system like steroids or biologics. If your immune system is suppressed, you may actually get symptoms of the disease you are trying to prevent.
To prevent psoriasis vaccine complications while on treatment, your doctor may give you a series of vaccinations before you start a biological drug. This could include vaccinations for diseases like the flu, pneumonia, and hepatitis.
The most common live virus vaccine is the one for the childhood diseases mumps, measles, and rubella, called MMR. Fortunately, most people with psoriasis are adults so they dont have to worry, said Dr. Moore.
A common live virus you should talk to your doctor about is the vaccination for herpes zoster, or shingles. Although this vaccine should be used with caution in psoriasis, some recent research suggests it can still be worth taking. A 2011 study published in the journal Arthritis Research and Therapy found that the live virus for shingles can be safe, even for people taking biologic drugs.
Don’t Miss: Psoriasis On African American Skin
Are There Home Remedies For Late
While home remedies will not make psoriasis go away, many people with mild to moderate psoriasis manage their symptoms using natural and alternative remedies. Tea tree oil and apple cider vinegar can relieve itching and loosen plaques especially in scalp psoriasis. An oatmeal bath or Epsom salts can soothe irritated skin. Adding omega-3 fatty acids to your diet can help reduce inflammation.
What Are The Symptoms Of Guttate Psoriasis
Guttate psoriasis causes tiny bumps called papules. Guttate means resembling drops. So, the papules are drop-like bumps or raised spots. Guttate psoriasis does not occur in stagesthe papules usually appear suddenly on the arms, legs or torso. Less frequently, the bumps affect the face, scalp and ears. The bumps may itch and have the following appearance:
-
Raised and slightly thickened
You May Like: Can Econazole Nitrate Cream Be Used For Psoriasis
How Can Psoriasis Flare
While you cant change your genes, you can prevent psoriasis flare-ups by controlling your symptoms through regular treatments. These include applying topical medications, taking oral medications, or receiving injections to reduce uncomfortable psoriasis symptoms.
or light treatment can also reduce the incidence of psoriasis. This type of treatment involves using natural or artificial ultraviolet light to slow skin growth and inflammation.
Aside from medical treatments, making certain lifestyle adjustments can also reduce your risk for a psoriasis flare-up. These include:
Psoriasis: More Than Skin Deep

The first accurate medical discussion of psoriasis dates back to 1801, but the disease itself is much older. In fact, its very name is borrowed from an ancient Greek word meaning an itchy or scaly condition. About 7 million Americans are plagued by this itching and scaling, and many of them have serious complications involving other organs. Although psoriasis is classified as a dermatologic disease, it doesn’t start in the skin, and its damage may be more than skin deep.
You May Like: Is There Treatment For Psoriasis
Psoriasis Can Cause Arthritis
For an unknown reason, psoriasis can cause a form of arthritis known as psoriatic arthritis. Symptoms include:
- discomfort, throbbing or swelling in one or many joints
- tenderness in any joint
- pain caused by inflammation in the joints, which stimulates nerve endings.
- The joints most likely to be affected are the last joint in the fingers or toes, the sacrum , wrists, knees or ankles.
Psoriasis Affects Nearly Three Percent Of The World’s Population Or Approximately 125 Million People Worldwide
Women and men of all ages and ethnicities are affected by psoriasis. Psoriasis has a variety of forms, though plaque psoriasis is most common, comprising approximately 80% to 90% of all cases. Several other serious diseases have been associated with psoriasis, including diabetes, heart disease, and psoriatic arthritis, a chronic disease that causes inflammation, swelling, and pain in the joints.As research continues to demonstrate the serious, systemic effects of psoriasis, new research approaches to understand effective treatment options are needed to improve the health and lives of psoriasis patients.
The cause of psoriasis isn’t fully knownPsoriasis is thought to be related to an immune system problem with cells in the body. More specifically, one key cell is a type of white blood cell called a T lymphocyte or T cell. Normally, T cells travel throughout the body to detect and fight off foreign substances, such as viruses or bacteria. In psoriasis, however, the T cells attack healthy skin cells by mistake, as if to heal a wound or to fight an infection.
Overactive T cells trigger other immune responses. The effects include dilation of blood vessels in the skin around the plaques and an increase in other white blood cells that can enter the outer layer of skin. These changes result in an increased production of both healthy skin cells and more T cells and other white blood cells.
Factors that may trigger psoriasis include:
Don’t Miss: Will A Tanning Bed Help Psoriasis
Knowing Your Risk For Psoriasis
For those genetically predisposed to the disease, Dr. Cohen says that there are certain risk factors that can increase the odds of developing it.
“Cigarette smoking, alcohol use, certain medications are environmental factors that might bring out psoriasis in someone who’s genetically susceptible,” says Dr. Cohen. And while genes or environmental factors can play a role in causing some people to develop the disease, the “exact mechanism” of why people get it remains a mystery, he adds.
As sufferers know, flare-ups can come and go with little-to-no warning, but any number of possible triggers are thought to contribute to bouts with the disease. “When flares of psoriasis occur, the first thing that needs to be done is to identify the cause and rule out an infection as the triggering event,” says Dr. Gelfand.
RELATED:6 Things That Can Make Psoriasis Better
What Causes Psoriasis
The exact cause of psoriasis isnt known. Some medical researchers have theories about why people develop psoriasis. According to the National Psoriasis Foundation, an estimated 10 percent of people inherit genes that increase their likelihood of getting psoriasis. Of those 10 percent, however, only about 2 to 3 percent actually develop the disorder.
Scientists have identified about 25 gene variants that can increase your risk for psoriasis. These genetic variants are believed to cause changes in the way the bodys T cells behave. T cells are immune system cells that normally fight off harmful invaders, such as viruses and bacteria.
In people with psoriasis, T cells also attack healthy skin cells by mistake. This immune system response results in a range of reactions, including:
- the enlargement of blood vessels in the skin
- an increase in white blood cells that stimulate the skin to produce new cells more quickly than usual
- an increase in skin cells, T cells, and additional immune system cells
- an accumulation of new skin cells on the surface of the skin
- the development of the thick, scaly patches associated with psoriasis
Typically, these effects occur in response to a trigger.
- having another autoimmune disorder, such as HIV or rheumatoid arthritis
- infections that cause a weakened immune system, such as strep throat
- a skin injury, such as a cut, bug bite, or sunburn
- excessive stress and tension
- certain medications, including lithium, beta-blockers, and antimalarial drugs
Read Also: Treating Scalp Psoriasis And Seborrheic Dermatitis
Where Will It Appear
Often plaque psoriasis will appear on your body in places like your elbows, your knees, or your back. These lesions arent picky though they may appear anywhere on your body. Its also quite common for plaque psoriasis to appear on your scalp, and even your upper body, palms, and feet.
On a personal level, I have found that by making sure I moisturise the places on my body I know are susceptible to psoriasis flare-ups, I can nip any flare-ups in the bud before they get out of control.
If you know of the areas on your body that you mainly get psoriasis, Id definitely advocate for this preventative measure.
Natural Skin Treatments For Plaque Psoriasis
Because its a chronic condition, many people with plaque psoriasis will try alternative and natural treatment methods. One method that has gained significant attention in the psoriasis community is the mud and salt of the Dead Sea.
Thousands of people a year invest in expensive Dead Sea skin treatments or vacations to attempt to heal their psoriasis. Although the scientific evidence is limited regarding the effectiveness of these treatments, many believe it can help treat plaque psoriasis.
You May Like: Short Course Of Prednisone For Psoriasis
Why Do People Get It
The reasons behind why people get psoriasis isnt an easy diagnosis.
Many factors contribute to why the autoimmune condition is caused, including environmental conditions or hereditary factors. Psoriasis is known to run in families, even if it might skip a generation or two.
A psoriasis flare-up is common if you go through a stressful experience. Its also known to appear if you end up with strep throat.
Being an autoimmune condition, it makes sense that if your throat is sore, as a result of an infection, your body is already running overtime trying to get rid of the infection, and it could throw your body into overdrive on the skin production front but Im no doctor!
Stress is also a huge factor even if you dont feel emotionally stressed, your body tends to know more about how much strain youre putting it through before you are mentally aware.
Psoriasis could be a way of your body letting you know that youre putting a little too much strain on it and to take some time out. A little-enforced break time never hurt anyone, surely!
What Are The Types Of Psoriasis
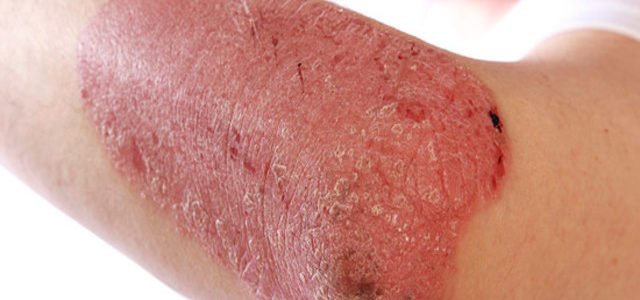
Common types of psoriasis include:
Plaque psoriasis. This is the most common type of psoriasis. It causes plaques and silvery scales, usually on the knees, elbows, lower back, and scalp. They can be itchy and painful and may crack and bleed.
Guttate psoriasis. This type often shows up after an illness, especially strep throat. It causes small red spots, usually on the trunk, arms, and legs. Spots also can appear on the face, scalp, and ears.
Inverse psoriasis. This causes smooth, raw-looking patches of red skin that feel sore. The patches are in places where skin touches skin, such as the armpits, buttocks, upper eyelids, groin and genitals, or under a girl’s breasts.
Read Also: Long Term Effects Of Psoriasis
Be Mindful Of Alcohol Consumption
Alcohol and Psoriasis
Some studies show a link between heavy drinking and psoriasis flares. It seems that men who drink heavily are more likely to suffer from psoriasis than men who do not drink alcohol. Alcohol consumption negatively impacts treatment and reduces the likelihood of remission. Alcohol may interact with certain psoriasis medications. Ask your doctor if it is safe for you to consume alcohol if you have psoriasis.
Tips to Stop Drinking
If you’re trying to cut back or stop drinking all together, managing triggers can help you reach your goal. In general, avoid high-risk situations where you anticipate it will be difficult to avoid temptation. If you can’t avoid a situation where you are concerned you might be triggered, have some strategies in place to help you stay on track and cope.
- Distract yourself by calling or texting a friend or watching a funny video online. Go for a walk or take a few minutes to practice deep breathing or meditation.
- Review your reasons for not wanting to drink. Write the reasons on a card that you keep in your purse or wallet to revisit when you need to.
- Talk to a trusted friend when you’re tempted to drink and discuss the reasons you’re trying to abstain.