More Than Skin Troubles
A 2017 study from the Journal of the American Academy of Dermatology found that people with psoriasis that covers 10% of their body or more are 64% more likely than those without psoriasis to develop type 2 diabetes. “About 30% of people with psoriasis also might develop psoriatic arthritis, which causes destructive inflammation in your joints,” says dermatologist Dr. Gideon Smith. Psoriasis also may signal a higher risk for fatty liver disease and heart attacks.
Treatment With Topical Corticosteroids
Corticosteroids reduce inflammation and slow the rapid production of skin cells. They are applied to the skin in the form of a cream, solution, ointment or for the treatment of psoriasis on the scalp a foam or shampoo.
There are big differences between corticosteroids in terms of the strength of their effect . In Germany and other countries they are divided up into four groups based on their potency:
- Low-potency corticosteroids
- High-potency corticosteroids
- Ultra-high-potency corticosteroids
Ultra-high-potency corticosteroids are often needed for the treatment of very scaly areas of skin and psoriasis on hair-covered areas of the scalp. Weaker corticosteroids or other drugs are used on sensitive areas of the body, such as the face or in skin folds. The symptoms usually improve within one to two weeks of starting treatment.
Psoriasis flare-ups are often treated with stronger medications such as mometasone. These medications are generally applied to the affected areas of skin once or twice a day for the first three weeks. After that they are gradually applied less frequently for instance, every other day in the fourth week, and every three days in the fifth week. Treatment with topical steroids is stopped gradually because an abrupt stop can make psoriasis come back again.
Studies have shown high-potency corticosteroids to be effective. They found the following after a few weeks:
What Are The Signs Someone Has It
People with psoriasis will probably notice one or more of these things:
- raised red patches of skin that can have silvery scales on them
- dry, cracked skin that may bleed at times
- itching, soreness, or a burning feeling in the affected area
- thick fingernails that have indents or pits
There are different types of psoriasis:
Read Also: Best Treatment For Psoriasis On Head
How Do You Treat Plaque Psoriasis
There are several treatments that target plaques. Your physician will decide which one is right for you based on your general health, any underlying conditions, and the severity of your plaque psoriasis. Your options include:
-
Topical ointments and creams such as cortisone cream, oral or injectable corticosteroids
-
Light therapy
-
Systemic drugs such as Gengraf and Sandimmune and Rasuvo and Rheumatrex
-
Biologic medications, which are made from living organisms and work by slowing down your overactive immune system
Research suggests that biologics for psoriasis might help with those other inflammatory diseases linked to the skin condition, too. A study in Cardiovascular Research found that treating psoriasis with biologics helps reduce the plaque buildup in the arteries, which leads to heart attacks and strokes.
However, once your skin plaques disappear, youre not necessarily in the clear. Exposure to your triggers can bring on a new bout of plaque psoriasis. Only 10% of people are lucky enough to have whats called spontaneous remission, when your skin clears up forever and you never have a flare up again.
Can Psoriasis Go Away
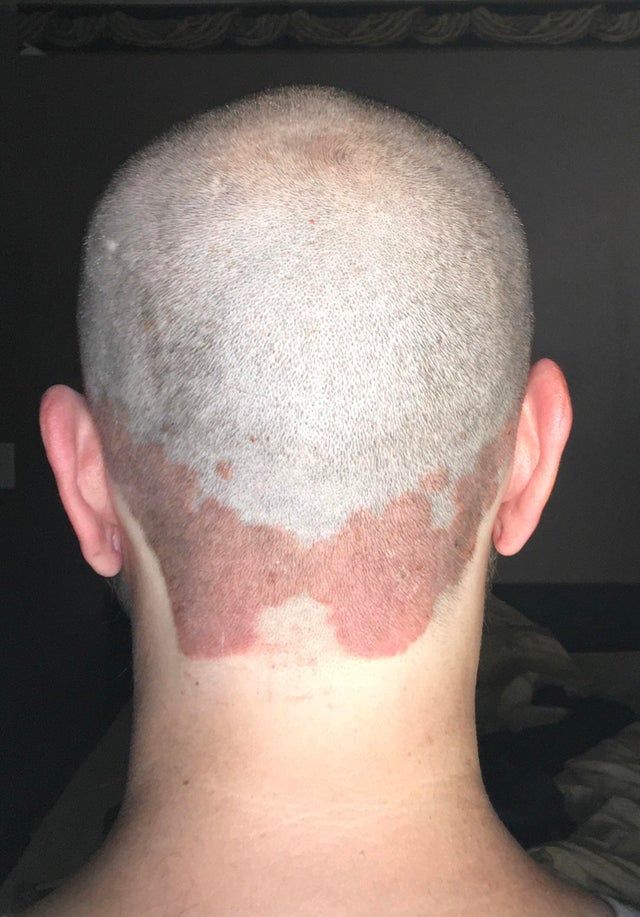
Psoriasis is a skin disease that develops due to changes in genetic makeup, and most often, it is passed from your parents . It may also occur due to changes in the immune system, autoimmune response, in which your own antibodies start attacking the cells of your body.
Psoriasis is a chronic inflammatory condition that has no definite cure and only the symptoms can be managed. At times, treatment can make psoriasis symptoms disappear and give you clear skin for a while.
This symptom-free period is referred to as remission. A remission is followed by the reappearance of the symptoms and this period is known as relapse.A remission can last for months or years ranging from one to 12 months.
The course of psoriasis is unpredictable, varying considerably among patients, so it’s impossible to know if you will have a remission and how long it will last.
You May Like: Best Over The Counter Scalp Psoriasis Treatment
What Are The Signs & Symptoms Of Psoriasis
The main symptom of psoriasis is red, thickened patches of skin called plaques. These can burn, itch, or feel sore. Often, silvery scales cover the plaques.
Plaques can happen anywhere. In children, they’re most common on the:
- face
- areas where skin touches skin
- diaper area
Other symptoms of psoriasis include:
- dry, cracked skin that may bleed at times
- thick, pitted nails
- arthritis
Before Stopping Psoriasis Treatment Talk With Your Dermatologist
Because psoriasis is a lifelong disease, its understandable that you may want to stop treatment at some point. Alwaystalk with your dermatologist before you stop treatment.
Some treatments can be stopped immediately. Others need to be discontinued slowly to prevent psoriasis from worsening .
When psoriasis rebounds, it may become a more serious type of psoriasis. A person who had plaque psoriasis may suddenly have pustular psoriasis or erythrodermic psoriasis.
The best way to prevent a rebound is to talk with your dermatologist. Your dermatologist can tell you whether you can stop the treatment abruptly or slowly. Sometimes, the best approach is to gradually switch to another treatment.
Read Also: What Does Psoriasis Look Like When It First Appears
How To Prevent Psoriasis From Returning
Psoriasis is a chronic, long-term condition, so flares will usually return even after remission. However, certain treatments and lifestyle changes may help people prolong their remission periods.
Experts believe that psoriasis occurs due to a combination of genetic factors and external triggers, but not everyone who inherits one or more of the specific psoriasis-causing genes goes on to develop the skin condition.
Therefore, avoiding triggers may be key to reducing the risk of psoriasis development and the return of symptoms following remission. Triggers vary from person to person, but some of the most common are:
How Can I Be Sure That Its Psoriasis And Not Something Else
For people with plaque or nail psoriasis, a primary care doctor can diagnose and treat the condition. People with unusual symptoms may need to see a dermatologist to rule out other conditions that can be mistaken for psoriasis. These include eczema, fungal infections, drug reactions, pityriasis rubra pilaris, and a form of skin cancer called cutaneous T cell lymphoma.
You May Like: Psoriasis En La Cabeza Tratamiento
Day 21 June 29 2020 Transformed
It has now been three weeks since I began my new treatment.
My body has, to lift a word from this websites home page, been transformed.
Its astonishing how rapidly and thoroughly it has occurred.
In seemingly the blink of an eye, decades of psoriasis have pretty much just disappeared.
Here are pictures of my shins: 5 days before treatment, 7 days after treatment began, and 21 days into treatment. Not bad, eh?
And here are my arm pics. Where did all the psoriasis go? Its fascinating to me how smooth my skin could be, so soon after having been so scratchy.
Im going to close with a story. I was at the beach several years ago, wearing a swim shirt, and looking around at other beach-goers to pass the time.
As I looked around at other people, I suddenly thought to myself: Why do I cover up my psoriasis, when all these people have their own how shall we put it? less-than-perfect elements of their own physical appearance?! How did they have the courage to enjoy themselves just as they are, and I was hiding behind a shirt I didnt want to wear?
So I took my swim shirt off, went into the ocean, and never wore one again.
After that, did I ever think people were looking askance at my psoriasis, perhaps wondering if it was contagious? Sure. But it no longer had significant power over me.
ADDENDUM 7/2: Lets take a look at my calves, shall we?
Im really starting to get used to the new me. It feels good.
Day 28 July 6 2020 Freedom
So lets take stock after four weeks. Scalp is clear, not itchy Im back to regular shampoo.
Body is largely free of psoriasis, and not itchy though my skin still shows, via its different colors, where the psoriasis used to be. Check out the shin photo below the one done without the flash to see the funky borders still visible, outlining former psoriasis zones. But note how clear those legs are! Im still not getting calls to be a leg model , but trust me when I say they are silky smooth.
I should also note that I am free of psoriatic arthritis pain. And I am not aware of any side effects.
The bottom line is I am starting to forget completely about psoriasis. Even the moisturizer I had used after showering I often skip now. Who puts moisturizer on soft, smooth skin?! If I wasnt doing these updates I might completely forget Ive battled psoriasis often getting my tail kicked for decades.
Hubris? Overconfidence? Pride cometh before the fall as my mom sometimes says ? Could be. And perhaps if I was doing daily Instagram selfies in swim trunks I might be less fascinated by the pinks, and whites, and browns that form those cool maps on my skin.
But I am officially letting myself get used to life basically psoriasis-free, and I feel like it might just last. Simply amazing. So get ready for my closing line that will make you groan on this Independence Day I am truly celebrating my freedom!
Don’t Miss: What Does Psoriasis Come From
Key Points About Psoriasis
- Psoriasis is a chronic skin condition. It causes inflamed, red, raised areas of skin that often develop dry, silvery scales called plaques.
- Psoriasis is not contagious. It is an autoimmune skin disease.
- Psoriasis is a long-term disease. You will have flare-ups that come and go over time.
- There is no cure, but treatments can help relieve symptoms. Treatment can include creams, light therapy , and oral or injected medicine.
- Psoriasis is a chronic condition. But you can manage it by working with your healthcare provider to create a long-term treatment plan and self-care routine that includes attention to both physical and emotional needs.
Debate Over Complete Clearance Goals Ends In Draw
byCharles Bankhead, Senior Editor, MedPage Today March 6, 2016
WASHINGTON — Dermatologists agreed that complete clearance should represent the treatment goal for all patients with psoriasis, but they remained divided over the best standard for good, but incomplete, responses, following arguments here.
The emergence of biologic and targeted therapies has made complete clearance of psoriasis a reality for more patients than ever, and results with new agents still in clinical evaluation suggest a potential for complete clearance in most patients.
When a response falls short of complete clearance, 75% improvement in the psoriasis area and severity index represents a familiar and useful standard, Robert Bissonnette, MD, of Innovaderm Research in Montreal, argued during a debate at the American Academy of Dermatology meeting.
PASI 90 represents incremental improvement over PASI 75 but remains statistically inferior to PASI 100 .
Stating a case for PASI 90 as the new standard, Robert J. Pariser, MD, of Eastern Virginia Medical School in Norfolk, said the availability of more potent therapies that attain higher rates of complete clearance also argues for a higher standard for a good response.
Case for PASI 75
Though used most often in education and clinical trial settings, the issue of the most appropriate PASI score for good response goes beyond academic arguments.
Case for PASI 90
More Opinions
Disclosures
Primary Source
American Academy of Dermatology
You May Like: Causes Of Psoriasis And Eczema
What You Should Know About Psoriatic Arthritis
An estimated 30% of people with psoriasis also have or will develop psoriatic arthritis, or PsA, a chronic autoimmune condition that affects 2-3% of the population. While psoriasis affects the skin, psoriatic arthritis affects the joints and some parts of the body where ligaments and tendons are attached to the bone, particularly in the fingers, toes, wrists, knees and spine. The result is stiffness, swelling, pain and, if not caught early, irreversible damage, which is why early diagnosis and treatment are important.
Topical Treatments For Psoriasis
Mild psoriasis can usually be treated effectively using medication applied directly to the skin . Corticosteroids and vitamin D analogues have proven to help and be well tolerated.
The treatment options for psoriasis include medication applied to the skin, phototherapy, and medication that is swallowed or injected. Topical treatments are often effective in mild to moderate cases of psoriasis. The medications are applied to the affected areas of skin in the form of ointments, creams, solutions or foams. The type of product used will depend on various factors, including the location of the plaque and the condition of the skin.
Some people only use the medication during acute episodes of psoriasis, while others use it regularly as a long-term treatment. It is then applied to the affected areas of skin during “quieter” phases too, with the aim of preventing further flare-ups. In order to avoid side effects, steroid medications aren’t applied every day, but rather on two days per week for instance at weekends.
In addition to using medicated topical treatments, people are advised to take good care of their skin, for instance by using lipid-replenishing ointments or creams to moisturize it. The aim of this continuous basic treatment is to relieve itching and prevent the skin from drying out.
Don’t Miss: Does Psoriasis Flare Up In Heat
Lifestyle Changes And Home Remedies
The most important lifestyle change that people with psoriasis can make is to avoid triggers, which might include cold weather, stress, or smoking.
People may also wish to try the following home remedies. While they will not cure psoriasis, they may reduce itching, dryness, and other types of discomfort:
- applying aloe vera gel to reduce redness and itching
- avoiding alcohol and tobacco
How Do You Treat Psa
If you have this condition, youll want to see a rheumatologist, a doctor who specializes in arthritis. Treatments can range OTC non-steroidal anti-inflammatory drugs such as Advil to disease-modifying antirheumatic drugs , including methotrexate, that work by slowing your immune system and your bodys inflammatory response. If those dont work, biologics may be considered.
Also Check: I Have Psoriasis In My Ears
Day 7 June 15 2020 Kim Kardashians Psoriasis Journey And Mine
Before I give you my update, I want to break some news here. Its not even up on the Psoriasis Cure Now News section yet, its so hot off the presses. Turns out Kim Kardashian West still more famous than I am, but just wait til my abs go viral talked about groin psoriasis on her show the other night. Documenting her psoriasis journey on her familys TV show, she even unveiled some gizmo that directs ultraviolet light right where its, um, needed. Here she is trying it on her face. Kim, if you are reading this, stay tuned. I have a feeling that my new treatment can blow your gizmo out of the water.
OK, now back to my psoriasis journey.
As you may have heard, the tentative plan is for me to update you folks about my treatment for 12 to 16 weeks, so well know one way or another how I did.
Well.
You gotta laugh: its Day 7 and it is already EXTRAORDINARY!
Its making me want to put an exclamation point after every sentence!
Holy Toledo!
This is one of the more impressive things Ive witnessed. My skin is smoother than its been in many, many years. My neck, behind my ears, my belly, my back: its simply unbelievable.
Did I mention its just Day 7 of my new treatment?
Im a lousy photographer, but there are already visual changes can you tell? Less redness. The psoriasis is more flush with the skin, its flattened a bunch already. Wow.
Then on Wednesday, Ill post legs.
Any questions or comments, please submit them below, and Ill reply in a future post.
Is There A Timeline For Psoriasis Remission
Psoriasis is unpredictable, and psoriasis remission has no timeline. Sometimes, remission can be lengthy. You may not experience symptoms for months, even years. Remission can also be short-lived. You may start experiencing symptoms again within a few weeks of them disappearing.
One common psoriasis cycle involves having fewer symptoms and flares during summer months and more symptoms and flares during winter months. Thats likely because of how the two very different environments affect your skin. The weather in these two seasons can trigger psoriasis symptoms. Being aware of these triggers and others can help you reduce flare frequency and extend remission periods.
Although psoriasis may return on its own, something may prod its return. These things are called triggers. Being aware of the most common ones can help you reduce the likelihood of flares and possibly extend periods of remission.
Don’t Miss: Does Celery Juice Help Psoriasis
Is Psoriasis Remission Possible
There’s no cure for psoriasis, but it’s possible that your symptoms could simply disappear, either with effective treatment or without any treatment at all.
The news that you have a chronic disease like psoriasis is understandably hard to handle. And a lifetime of psoriasis symptoms skin that’s often red, scaly, flaky, itchy, and painful probably seems like an unfair burden to bear for the 7.5 million Americans with psoriasis.
But some people have long periods with no symptoms, known as psoriasis remission, when their psoriasis treatment is successful.
Spontaneous remission, or when your symptoms clear up without treatment, is also possible. Your immune system attacks the skin cells mistakenly, which is what triggers psoriasis in the first place, but in some cases, the body relents and allows the cells to heal.