Psoriatic Arthritis: What Is The Connection
Psoriatic arthritis : 1 in 4 of people with psoriasis may develop an associated arthritis called psoriatic arthropathy, which causes pain and swelling in the joints and connective tissue, accompanied by stiffness particularly in the mornings and when rising from a seat. Most commonly affected sites are the hands, feet, lower back, neck and knees, with movement in these areas becoming severely limited. Chronic fatigue is a common complaint linked with this condition. If you are experiencing mild aches and pains and have psoriasis, even very mildly, consult your dermatologist for further advice and if necessary a referral to a rheumatologist for further assessments. For more detailed information on psoriatic arthritis see What is Psoriatic Arthritis?
Psoriasis Beyond The Basics
There are many different types of psoriasis, including chronic plaque psoriasis, types of pustular psoriasis , guttate psoriasis, scalp psoriasis, flexural psoriasis, napkin psoriasis, nail psoriasis and erythrodermic psoriasis .
For those that have psoriasis around 1 in 4 may develop an associated psoriatic arthritis , which is about 325,000 people, or around 0.5% of the UK population. PsA causes pain and swelling in the joints and tendons, accompanied by stiffness particularly in the mornings. The most commonly affected sites are the hands, feet, lower back, neck and knees, with movement in these areas becoming severely limited.
Not all people will be affected in the same way and doctors will class the condition as mild, moderate or severe.
Remember, although psoriasis is a chronic condition, it can be controlled and go into remission .
What You Should Know About Scalp Psoriasis
If youre scratching your head over an itchy scalp condition that wont clear up with a traditional dandruff shampoo, you may have scalp psoriasis. This type can go hand-in-hand with plaque psoriasis , or even appear in those who dont have any history of the skin disorder at all.
Its often confused with dandruff, because, well, it itches and causes flakes, only these flakes are typically silvery-white and scaly. You might also have painful red scales or silver plaques on your head. In severe cases, scalp psoriasis appears as thickened, crusty patches of skin not only on the hairline, but also on the forehead, back of the neck and near the ears.
You May Like: Home Phototherapy Unit For Psoriasis
How Do You Treat Scalp Psoriasis
Mild cases can be nipped in the bud or improved with salicylic-, coal-tar-, or clobestasol propionate-containing shampoos. More severe cases may require systemic or biologic drugs, oral treatments, light therapy, or a combination of treatments. Unfortunately, you may lose some hair with some of these treatments, which is usually temporary.
Main Symptoms Of Psoriasis
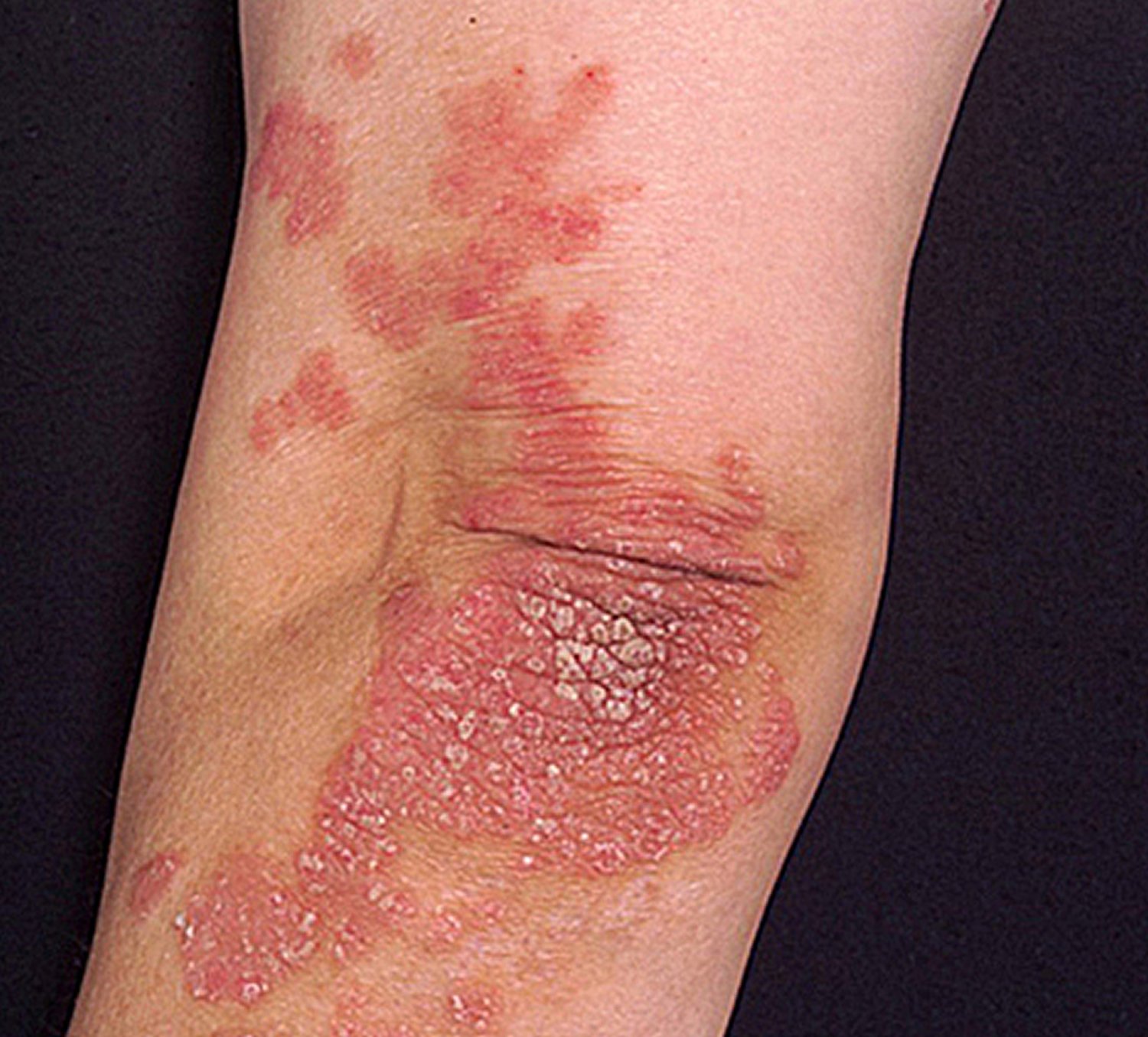
Psoriasis typically causes patches of skin that are dry and covered in scales.
On brown, black and white skin the patches can look pink or red, and the scales white or silvery. On brown and black skin the patches can also look purple or dark brown, and the scales may look grey.
Some people find their psoriasis causes itching or soreness.
There are several different types of psoriasis. Many people have only 1 type at a time, although you can have 2 different types together. One type may change into another or become more severe.
Most cases of psoriasis go through cycles, causing problems for a few weeks or months before easing or stopping.
You should see a GP if you think you may have psoriasis.
Read Also: Uv Light Lamp For Psoriasis
Can Psoriasis Be Treated
Yes, there are many forms of treatment for psoriasis, which range from those you apply to the skin to tablets, and more recently injectable therapies, See Treatments for Psoriasis.
Many people who have psoriasis find that the sun and artificial ultraviolet light helps to improve their skins appearance. For some the change is dramatic. Be aware that exposure to the sun and artificial UV therapy can cause damage to the skin. See Psoriasis and the sun and Psoriasis and phototherapy
For some people, talking therapies such as cognitive behaviour therapy can also help them understand the psychological impact of psoriasis and provide a safe therapy which may help them cope with psoriasis. See our free online CBT programme
Your general practitioner or dermatologist will be best placed to advise you and keep you informed of all current and new treatments available and to recommend the best treatment programme for you personally.
Remember: Your treatment can only be as good as you allow it to be – that means if the treatment takes six weeks, you have to follow it as instructed for six weeks and no ducking out! Adherence to treatment instructions is an essential part of managing your psoriasis.
How Do People Get A Second Type Of Psoriasis On Their Skin
While theres no way to predict who will develop a second type of psoriasis, some people may be more susceptible. For example, having severe psoriasis that isnt well controlled, stopping a strong medication too quickly, or getting strep throat may increase your risk.
The following explains how people who have plaque psoriasis, the most common type of psoriasis, can develop a second type of psoriasis on their skin.
Youll also find out how plaque psoriasis can turn into a different type of psoriasis.
Inverse psoriasis: Many people gain a lot of weight after getting plaque psoriasis. Researchers arent sure why this happens, but they have discovered that extra pounds can increase your risk of developing inverse psoriasis.
Inverse psoriasis only forms in areas where skin touches skin, such as the armpits, groin, or underneath the breasts. It causes smooth, bright-red patches of raw-feeling skin.
Guttate psoriasis: Some people with plaque psoriasis have developed guttate psoriasis after getting an infection, such as strep throat. Guttate psoriasis causes spots on the skin that are small, pink to salmon-colored, and scaly. These spots are often widespread, appearing on the torso, legs, and arms.
Erythrodermic psoriasis: Some people who have severe plaque psoriasis see their plaque psoriasis turn into erythrodermic psoriasis. This can happen when:
Different ways that psoriasis can affect the nails
Recommended Reading: Pictures Of What Psoriasis Looks Like
Can Psoriasis Affect My Joints
Yes, psoriasis is associated with inflamed joints in about one-third of those affected. In fact, sometimes joint pains may be the only sign of the disorder, with completely clear skin. The joint disease associated with psoriasis is referred to as psoriatic arthritis. Patients may have inflammation of any joints , although the joints of the hands, knees, and ankles tend to be most commonly affected. Psoriatic arthritis is an inflammatory, destructive form of arthritis and needs to be treated with medications in order to stop the disease progression.
The average age for onset of psoriatic arthritis is 30-40 years of age. Usually, the skin symptoms and signs precede the onset of arthritis.
Common Types Of Psoriasis
Plaque psoriasis is the most common form of psoriasis.
Its symptoms are dry skin lesions, known as plaques, covered in scales.
They normally appear on your elbows, knees, scalp and lower back, but can appear anywhere on your body.
The plaques can be itchy or sore, or both. In severe cases, the skin around your joints may crack and bleed.
Also Check: How Do I Get Psoriasis
What Is Guttate Psoriasis
Guttate psoriasis is the second most common psoriasis type.
It affects about 10 percent of people with psoriasis, according to the National Psoriasis Foundation .
Guttate psoriasis, from the Latin for raindrop shaped, causes small, dot-like spots on the body. These lesions frequently appear on the upper arms, trunk, thighs, or scalp.
Often, this form of psoriasis starts in childhood or young adulthood.
Guttate psoriasis can be triggered by a strep infection, tonsillitis, stress, a skin injury, or certain medication . Sometimes genetic factors are to blame.
Guttate psoriasis may clear up on its own, but certain cases require treatment. Some patients may experience guttate psoriasis just once, while others may find it leads to plaque psoriasis.
Pustular Or Exudative Psoriasis
This type is manifested through the most severe pathological changes. Characteristic signs of this type are purulent lesions of the skin. Pustular psoriasis can be caused by infections, pathologies of the hormonal background or by improper treatment of common psoriasis. This disease often causes a fever, an increase in blood leukocytes. Skin lesions form purulent lakes which is accompanied by burning and painful sensations. Patients with exudative psoriasis have the need for hospitalization during exacerbations. The process of treating this form of ailment is very complex, long and it requires special attention. However, the cyclicity of the disease implies the possibility of remission. There are two forms of pustular psoriasis: generalized and localized.
Generalized form of pustular psoriasis is dangerous for human life. Rapidity of the symptoms development is typical for this type. At first, you can see inflamed foci, in the form of purple spots on the skin. Over time, they are transformed into purulent lesions and merge into large-scale skin lesions. If these lesions are injured, there are wounds and ulcers. This form of the disease is accompanied by severe itching, burning and febrile syndrome. The disease aggravation can last almost 2 months. As a consequence, the skin shows symptoms typical for common psoriasis. Localization: elbow and knee folds, skin folds, genitalia and sometimes head and nails.
Also Check: Drugs Used To Treat Psoriasis
What You Should Know About Erythrodermic Psoriasis
The rarest of all psoriasis types, erythrodermic psoriasis affects only 2% of those with psoriasis. This type causes redness from head to toe, as if your skin has been burned. Even worse, its possible that your skin could peel off in sheets.
As with the pustular type, erythrodermic psoriasis severely compromises the skins protective barrier, so swift medical attention is a must. You can also develop fever, chills, swollen, painful joints, and rapid heart rate.
Who Gets Psoriasis
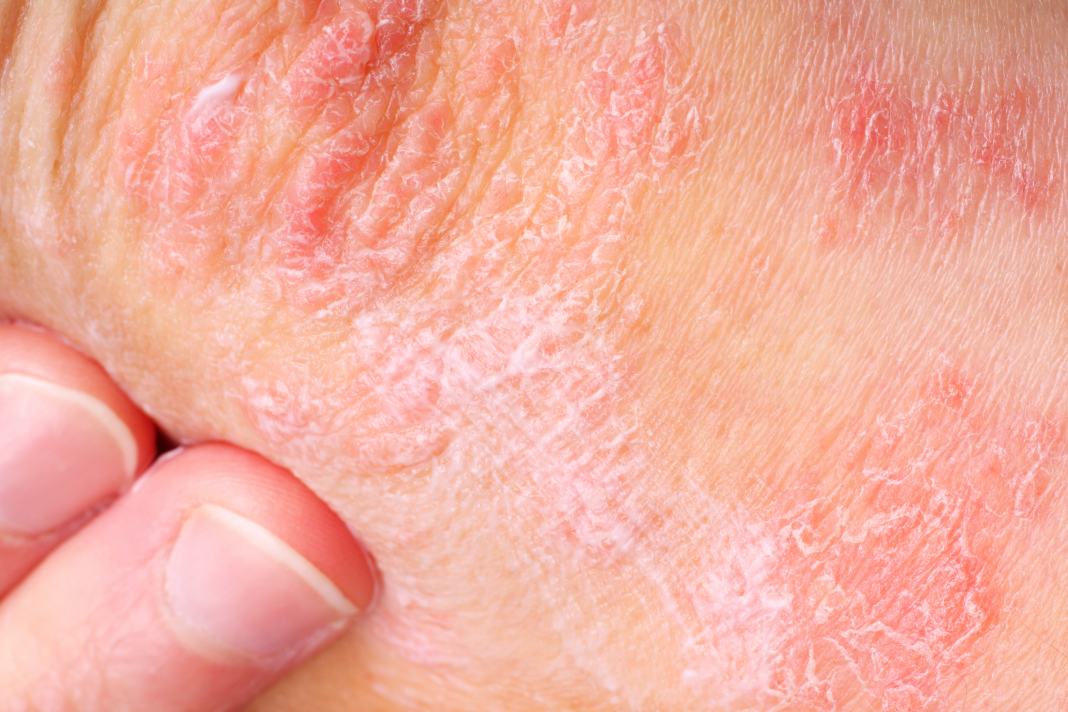
Psoriasis is a long-term scaling disease of the skin which affects around 1 in 50 people, which is about 1.3 million, or around 2% of the UK population. IT IS NOT CONTAGIOUS and you cannot catch psoriasis from someone else. It usually appears as red, raised, scaly patches known as plaques. Any part of the skin surface may be involved but the plaques most commonly appear on the elbows, knees and scalp. It can be itchy but is not usually painful. Nail changes, including pitting and ridging, are present in nearly half of all those who have psoriasis.
Read Also: Anti Inflammatory Drugs For Psoriasis
What You Can Do
Most people who get plaque psoriasis have it for the rest of their lives. You can do a few things to deal with it better:
Avoid triggers. Things like stress and smoking don’t cause psoriasis. But they can make it worse. Try to figure out what triggers your flare-ups. You may be affected by:
- Alcohol
- Cold, dry weather
- Hormones
Watch your diet. There’s no proof that specific foods make a difference with psoriasis. But losing weight may keep your symptoms at bay, so it makes sense to eat healthy. And a diet low in fatty meat and dairy products and high in fish and colorful fruits and vegetables may help with inflammation. Read more on psoriasis and your diet.
Take care of your skin. A good moisturizer can keep plaques soft and make you less itchy. Avoid harsh soaps.A bath with colloidal oatmeal or Epsom salts can also soothe your skin. Try using medicated shampoo for scales on your scalp. Learn about more skin care tips for psoriasis.
Get support. Plaque psoriasis can take an emotional toll. You may feel self-conscious about the way it looks or overwhelmed by what it takes to manage it. Many people with psoriasis become depressed. If you think you need some help, talk with your doctor about therapy or medication. It also helps to talk with people who understand what you’re going through and can offer strategies for coping. Find out how to get emotional support during psoriasis treatment.
Show Sources
What Is Scalp Psoriasis
Scalp psoriasis shows up as itchy, scaly patches on the scalp that may bleed if you try to remove them.
About half of people who have psoriasis have it on their scalp.
At the onset, scalp psoriasis often is confused with seborrheic dermatitis . Dandruff is a flaky, itchy scalp without signs of inflammation .
Scalp psoriasis can spread beyond the hairline and affect the forehead, back of the neck, and areas around the ears.
Often psoriasis in kids is first found on the scalp.
Additional reporting by George Vernadakis
You May Like: Can Psoriasis Cause Other Health Problems
Home Treatment For Psoriasis
There are some home remedies that may help minimize outbreaks or reduce symptoms of psoriasis:
- Exposure to sunlight.
- Apply moisturizers after bathing to keep skin soft.
- Avoid irritating cosmetics or soaps.
- Do not scratch to the point you cause bleeding or excessive irritation.
- Over-the-counter cortisone creams can reduce itching of mild psoriasis.
A dermatologist may prescribe an ultraviolet B unit and instruct the patient on home use.
What You Should Know About Psoriatic Arthritis
An estimated 30% of people with psoriasis also have or will develop psoriatic arthritis, or PsA, a chronic autoimmune condition that affects 2-3% of the population. While psoriasis affects the skin, psoriatic arthritis affects the joints and some parts of the body where ligaments and tendons are attached to the bone, particularly in the fingers, toes, wrists, knees and spine. The result is stiffness, swelling, pain and, if not caught early, irreversible damage, which is why early diagnosis and treatment are important.
Recommended Reading: Severe Psoriasis And Psoriatic Arthritis
What Should You Do If You Develop Another Type Of Psoriasis
Life-threatening signs and symptoms, such as redness that covers most of your body, fever, and chills, require immediate medical care.
When signs and symptoms are not life threatening, you should see a board-certified dermatologist for a diagnosis. Youll find pictures of the different types of psoriasis and learn more about the possible signs and symptoms at Psoriasis: Signs and symptoms
ImagesImage 1: Getty ImagesImage 2: J Am Acad Dermatol 2013 69:245-52.
ReferencesBrummer GC, Hawkes JE, et al. Ustekinumab-induced remission of recalcitrant guttate psoriasis: A case series. JAAD Case Rep. 2017 3: 4325.
Egeberg A, Thyssen JP, et al. Prognosis after hospitalization for erythroderma. Acta Derm Venereol. 2016 96:959-92.
Gottlieb A, Korman NJ, et al. “Guidelines of care for the management of psoriasis and psoriatic arthritis: Section 2. Psoriatic arthritis: Overview and guidelines of care for treatment with an emphasis on the biologics. J Am Acad Dermatol 2008 58:851-64.
Gudjonsson JE and Elder JT. Psoriasis. In: Wolff K, Goldsmith LA, et al. Fitzpatricks Dermatology in General Medicine. McGraw Hill Medical, New York, 2008:178-81.
Khosravi H, Siegel MP, et al. Treatment of Inverse/Intertriginous Psoriasis: Updated Guidelines from the Medical Board of the National Psoriasis Foundation. J Drugs Dermatol. 2017 16:760-6.
Navrotski BRF, Nihi FM, et al. Wet wrap dressings as a rescue therapy option for erythrodermic psoriasis. An Bras Dermatol. 2018 93:598-600.
What Else Should I Ask My Healthcare Provider
If you have psoriasis, ask your healthcare provider:
- How can I prevent outbreaks and control symptoms?
- What medication will work best for me?
- What else should I do to improve symptoms?
- What are my options if creams dont work?
- Will psoriasis ever go away?
A note from Cleveland Clinic
Psoriasis, an itchy skin condition, can come and go throughout your life. Its related to an overactive immune response and is not contagious. If you have skin changes that arent going away, talk to your healthcare provider. There is no cure for psoriasis, but psoriasis treatments can improve symptoms. Your provider may prescribe a special cream or moisturizer or medications. Other therapies are available if creams or medicines dont work. Maintaining your overall health will also help improve symptoms.
Last reviewed by a Cleveland Clinic medical professional on 10/17/2020.
References
Don’t Miss: Best Cortisone Cream For Psoriasis
What Is Cdc Doing About Psoriasis
In 2010, CDC worked with experts in psoriasis, psoriatic arthritis, and public health to develop a public health perspective that considers how these conditions affect the entire population. The resulting report is Developing and Addressing the Public Health Agenda for Psoriasis and Psoriatic Arthritis pdf icon. You can read a short article about the agendaexternal icon in The American Journal of Preventive Medicine.
CDCs National Health and Nutrition Examination Survey , an intermittent source of national psoriasis data, has included questions about psoriasis as late as the 2013-2014 cycle. A recent analysis of NHANES data estimates that 7.4 million adults had psoriasis in 2013external icon.
- Psoriasis causes patches of thick red skin and silvery scales. Patches are typically found on the elbows, knees, scalp, lower back, face, palms, and soles of feet, but can affect other places . The most common type of psoriasis is called plaque psoriasis.
- Psoriatic arthritis is an inflammatory type of arthritis that eventually occurs in 10% to 20% of people with psoriasis. It is different from more common types of arthritis and is thought to be related to the underlying problem of psoriasis.
- Psoriasis and psoriatic arthritis are sometimes considered together as psoriatic disease.
Who is at risk for psoriasis?
Anyone can get psoriasis. It occurs mostly in adults, but children can also get it. Men and women seem to have equal risk.
Can I get psoriasis from someone who has it?
What You Should Know About Guttate Psoriasis
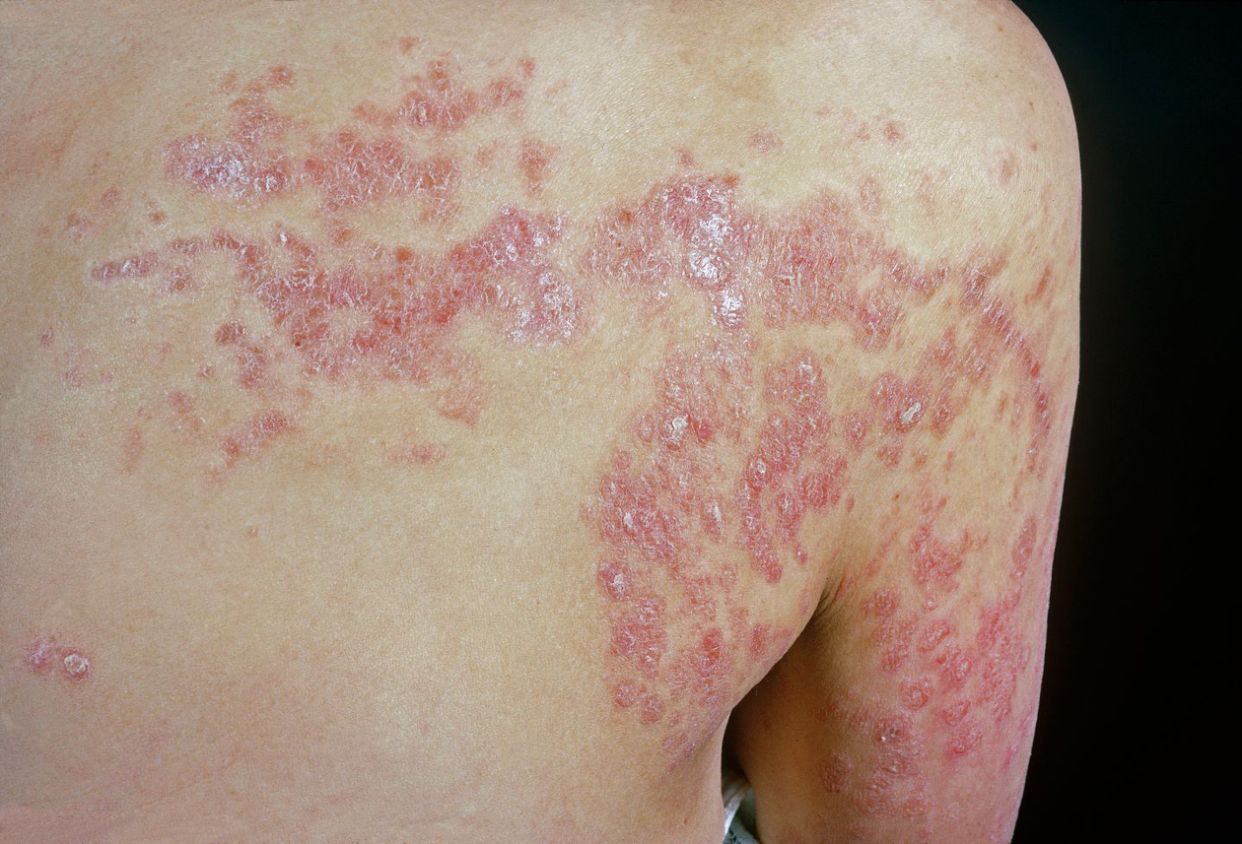
This type doesnt bring large plaques, but instead little red bumps smaller than a fingertip. You can wind up with hundreds of them scattered on your arms, legs, and torso.
About 10% of all psoriasis cases are the guttate type. You can have a mild case with just a few spots in one area, a moderate case that covers up to 10% of your body, or a severe breakout that leaves most, or even all, of your body covered in bumps.
Recommended Reading: Psoriasis On Face African American
Who Gets Nail Psoriasis
After developing a type of psoriasis on your skin, its common for psoriasis to affect the nails. Nail psoriasis becomes more common with age. Its also more common if youve had psoriasis on your skin for some time or have severe psoriasis.
Signs of nail psoriasis include tiny dents in your nails , discoloration under one or more nails, and a nail lifting away from the nail bed so that its no longer completely attached. Some people have a buildup of skin under one or more of their nails, which can also cause a nail to lift up.