Psoriasis: More Than Skin Deep
The first accurate medical discussion of psoriasis dates back to 1801, but the disease itself is much older. In fact, its very name is borrowed from an ancient Greek word meaning an itchy or scaly condition. About 7 million Americans are plagued by this itching and scaling, and many of them have serious complications involving other organs. Although psoriasis is classified as a dermatologic disease, it doesn’t start in the skin, and its damage may be more than skin deep.
What Exactly Is An Autoimmune Disease
When you have an autoimmune disease, your body mistakes normal, healthy tissues for foreign invaders. Basically, it goes to war with itself, causing damage and inflammation.
Not so fun fact: There are 100+ autoimmune diseases. Some of them, like psoriasis, only affects one body part . Others are system-wide, leaving your body exhausted and achy almost 24/7.
Regardless of your autoimmune diagnosis, your body is doing its war-waging thing because of some mysterious perfect storm of genetics and environmental factors.
Supplements And Alternative Treatments
The National Psoriasis Foundation suggest some herbs and natural remedies that may help with psoriasis in general.
- Tea tree oil: Always dilute with a carrier, such as almond oil, before applying. Do not take by mouth. Some people may have an allergic reaction.
- Epsom or Dead Sea salts: Add these to lukewarm water to soak the hands or feet.
- Oats: You can add these to a soak or a bath.
- Apple cider vinegar: Apply directly to the skin or dilute in equal parts with water. You can also add it to salads to take it by mouth.
- Capsaicin: Some people find that applying a cream containing the spicy ingredient in chili peppers to the skin may help reduce itching and burning.
- Mahonia Aquifolium: Also known as Oregon grape, applying a 10-percent topical cream may help reduce mild to moderate symptoms of psoriasis.
- Turmeric: Adding this spice to food or taking supplements may help with some types of psoriasis.
Ask a health professional before using any of these, to make sure they are safe and suitable for you to use.
Apply a small amount to a small area of skin to check your reaction, in case you have an allergy or the treatment makes symptoms worse.
Don’t Miss: Is There Treatment For Psoriasis
Shades Of Gray: Crosstalk Between Adaptive And Innate Immunity In Psoriasis
In addition to the antigen-specific facilitation of inflammation in psoriasis, there are several strong connections to components of the innate immune system. The crosstalk between the innate and adaptive branches of the immune system in psoriasis is complex and can only be highlighted by a few selected examples. Its fine-tuning arguably determines the actual clinical correlate within the spectrum of the disease. Indeed, there is accumulating circumstantial evidence that in patients with stable and mild disease, mechanisms of adaptive immunity are more likely to be in the foreground, while innate mechanisms seem to be more important in patients with active severe disease, systemic involvement and comorbid conditions . The impact on systemic comorbid diseases has been interpreted, at least in part, as a systemic spillover of innate inflammatory processes in severe psoriasis . Of course, such factors are not specific for psoriasis, but appear to account for a general inflammatory state in patients with severe psoriasis.
Patients with severe psoriasis have increased levels of inflammatory cytokines, CRP, fibrinogen, 2 macroglobulin or PAI-1 in the blood , they show transcriptomic, proteomic and metabolomic abnormalities and there are connections with chronic stress and biophysical properties of the skin .
How Does Psoriatic Disease Affect The Immune System
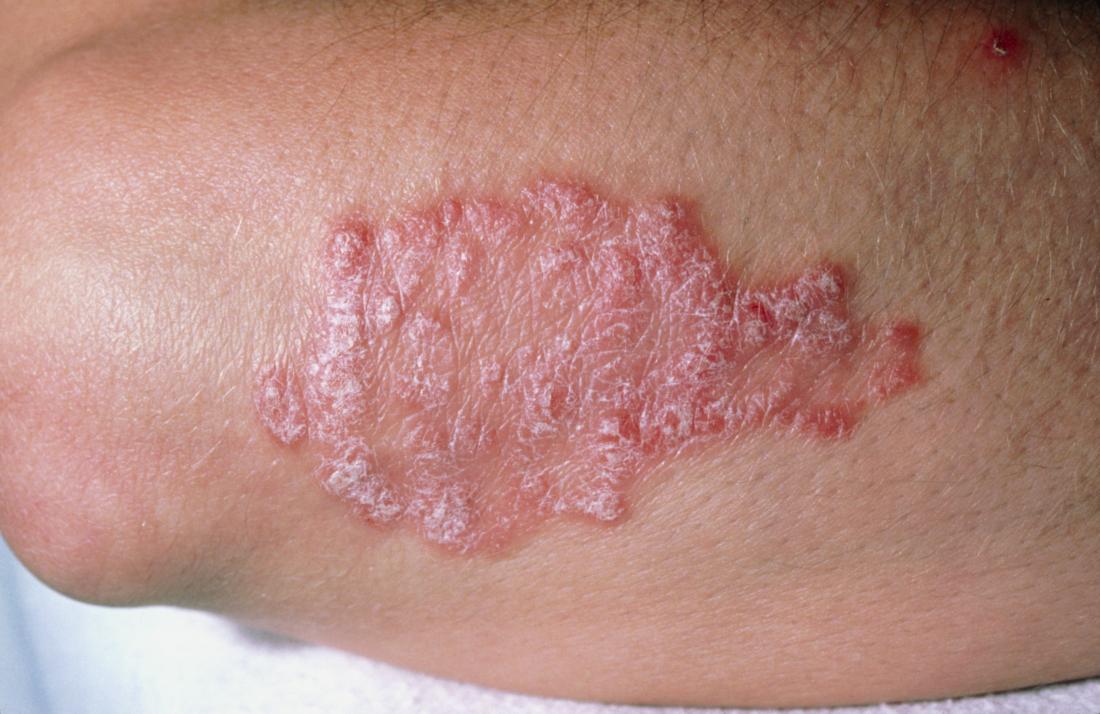
Psoriatic disease is an immune-mediated disease that includes psoriasis, along with other comorbidities such as psoriatic arthritis and related systemic inflammation. In people living with psoriasis and/or PsA, the immune system is triggered and activated, acting as though there are harmful pathogens attacking the body.
This inflammation can present with noticeable signs such as discoloration of the skin or swelling around joints. However, the overactive immune system may also lead to inflammation a person cannot see. It can affect in the body, organs and systems and lead to other health conditions associated with psoriatic disease. Comorbidities of psoriatic disease include cardiovascular disease, metabolic syndrome, obesity, hypertension , type 2 diabetes, anxiety and depression, and more.
Researchers who study psoriatic disease are still working to identify the substances inside the body that trigger this immune response. One possibility could be certain kinds of bacteria acting as antigens . For example, sometimes streptococcal infection can trigger a case of guttate psoriasis. Another possible antigen could be antimicrobial peptides, molecules made by the body that are a part of the immune system and that work as antibiotics. *
Recommended Reading: Is Hydrocortisone Cream Good For Psoriasis
How Are Autoimmune Diseases Diagnosed
Diagnosing an autoimmune disease usually takes healthcare providers longer than it does to diagnose other diseases. This is because many autoimmune diseases have similar symptoms with each other and with other diseases. You can help your healthcare provider with the diagnosing process by bringing the following to your appointment:
- A detailed list of any symptoms and how long youve had them.
- A record of your familys health history. Note if anyone in your family has an autoimmune disease.
In addition to interviewing you about your symptoms, your healthcare provider may do some blood tests to check for autoimmune diseases, including:
- Antinuclear antibody test .
Specific symptoms combined with specific blood markers may prove that you have an autoimmune disease.
Complications Of Psoriasis And Covid
If you test positive for COVID-19, have symptoms, or think you have been exposed to the virus, you should reach out to your primary doctor right away. Be sure to tell them you are taking immunosuppressive drugs to treat psoriasis.
If you test positive, you should also reach out to the doctor who treats your psoriasis so they can tell you how to manage your psoriasis care while you are recovering. They might suggest you alter or delay your next dose or treatments that suppress your immune system.
Your doctor will also give you information about treatment options for preventing a flare-up during this time.
There isnt enough evidence on how COVID-19 affects people with psoriasis or if they might be affected differently than people without psoriasis. Regardless, COVID-19 is highly transmissible and spreads rapidly, which means everyone is at risk. Even if you dont have symptoms, you can still spread COVID-19.
Complications of COVID-19acute respiratory distress, cardiac injury, blood clots, and morecan affect anyone who contracts the infection, especially those with a higher risk for the condition.
But it is unknown whether people with psoriasis have an elevated risk for these types of complications. The small amount of research available seems to indicate that their risk isnt different from others in the general population.
Recommended Reading: Scalp Eczema Vs Scalp Psoriasis
Monocytes Macrophages And Myeloid
Monocytes
Monocytes are known precursors for DCs and macrophages and as such, they have been described to be important cellular contributors to psoriatic pathology. It has been suggested that psoriatic monocytes engulf low density lipoprotein leading to overproduction of inflammatory cytokines. Additionally, psoriatic monocytes have also been described to possess increased phagocytic capabilities due to an imbalance in the ratio of cAMP/cGMP found in lesional skin. More recently an increase in CD14+ CD16+ intermediate monocytes termed Mon2 has been described in a cohort of human psoriatic patients., Interestingly, Mon2 monocytes also have been shown to be linked to an increased risk of CVD and to be predictive of myocardial infarction and death.
Macrophages
Myeloid-derived suppressor cells
What Are The Symptoms Of Psoriasis
The following are the most common symptoms of psoriasis. Psoriasis comes in several forms and severities. Symptoms may include:
-
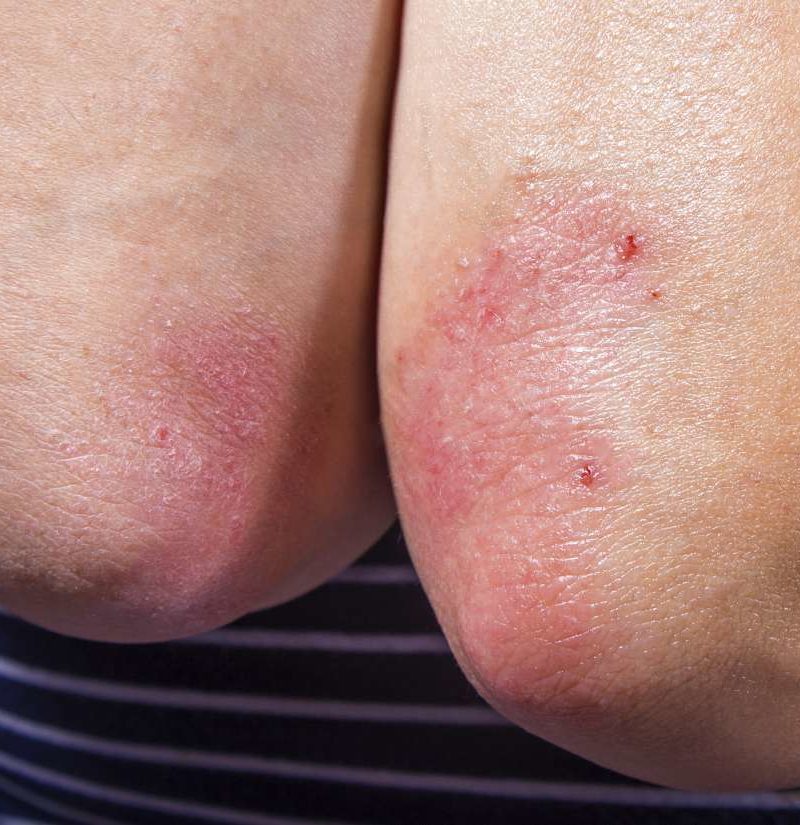
Plaque psoriasis. This type of psoriasis is the most common. Symptoms may include patches of red, raised skin on the trunk, arms, legs, knees, elbows, genitals, and scalp. Nails may also thicken, become pitted, and separate from the nail beds.
-
Guttate psoriasis. This type of psoriasis affects mostly children. Symptoms may include many small spots of red, raised skin. A sore throat usually proceeds the onset of this type of psoriasis.
-
Pustular psoriasis. Symptoms may include small pustules all over the body or just on the palms, soles, and other small areas.
The symptoms of psoriasis may look like other skin conditions. Always talk with your healthcare provider for a diagnosis.
Also Check: What Causes Psoriasis Of The Liver
Psoriasis Association With Other Autoimmune Diseases
Association of psoriasis with other autoimmune diseases is an ongoing research area. Previous studies have shown that there is a higher frequency of autoimmune diseases among psoriasis patients than observed in the general population potentially stemming from cytokine pathways dysregulation., Based on a retrospective study using MEDLINE data from January 1, 1980 to June 1, 2011, the major autoimmune disorders associated with psoriasis include RA, celiac disease, IBD, especially CD, multiple sclerosis, SLE, and autoimmune thyroid disease. However, anecdotal reports of other autoimmune diseases associated with psoriasis include Sjögrens syndrome and alopecia areata. In addition, a new meta-analysis of a single mutation of CD226, Gly307Ser has suggested that this modification is associated with an increased risk of developing various autoimmune disorders including psoriasis.
When To See A Doctor
See a doctor if you have symptoms of an autoimmune disease. You might need to visit a specialist, depending on the type of disease you have.
- Rheumatologists treat joint diseases, like rheumatoid arthritis as well as other autoimmune diseases like Sjögrens syndrome and SLE.
- Gastroenterologists treat diseases of the GI tract, such as celiac and Crohns disease.
- Endocrinologists treat conditions of the glands, including Graves disease, Hashimotos thyroiditis, and Addisons disease.
- Dermatologists treat skin conditions, such as psoriasis.
The Healthline FindCare tool can provide options in your area if you need help finding a specialist.
Recommended Reading: Dosage Of Methotrexate For Psoriasis
When Should I Go To The Emergency Department
Go to the emergency department if any of the following autoimmune disease symptoms get severe:
- Trouble breathing/shortness of breath. Remember that some people with an autoimmune disease can experience this when theyre pregnant.
- Severe chest pain/pressure to your chest.
- A headache that starts suddenly and feels like the worst headache youve ever had.
- Sudden weakness, especially if you cant move.
- Dizziness that doesnt stop.
- Pain so severe that you cant stand it.
A note from Cleveland Clinic
Living with an autoimmune disease can be complicated. Diseases like lupus, rheumatoid arthritis and multiple sclerosis are complex and serious. Although there are no cures for these diseases, many of their symptoms can be treated, and sometimes they go into remission. Stay in touch with your healthcare provider about any advances in understanding and treating autoimmune diseases.
If you think you may have an autoimmune disease, see your healthcare provider as soon as possible for diagnosis and treatment. Your symptoms will be easier to control if the condition is treated promptly.
Last reviewed by a Cleveland Clinic medical professional on 07/21/2021.
References
How Are Autoimmune Diseases Treated
There are no cures for autoimmune diseases, but symptoms can be managed. Everyones immune system, genetics and environment are different. That means that your treatment must be unique.
Some examples of medications used to treat autoimmune diseases include:
- Painkillers.
- Limiting processed foods from your diet.
Don’t Miss: Best Contraceptive Pill For Psoriasis
Adenoid Cystic Carcinoma With A Leptomeningeal Dissemination In A ‘wash’ Patternyour Browser Indicates If You’ve Visited This Link
A 39-year-old woman was referred to the neurology department due to headache, instability and difficulty walking for 5months. Several ancillary tests were performed. The blood test showed leucocytosis and the cerebrospinal fluid revealed an increased total protein and glucose consumption.
The Other Side: Antigen Presentation By Hla Molecules In Psoriasis
While most, if not all, autoimmune diseases are linked with certain HLA alleles , HLA-C*06:02 is the predominant psoriasis risk gene . HLA class I molecules present short peptide antigens to TCRs of CD8+ T cells. Such antigenic peptides are usually derived within the antigen presenting cell from parent proteins by proteasomal cleavage and loaded onto HLA-class I molecules. The HLA/peptide complex is then transported to the cell membrane where it can be recognized by CD8+ T cells . Thus, HLA-class I-restricted immune responses are usually directed against target cells which produce the antigenic peptide.
HLA-C*06:02-presented non-apeptides possess anchor amino acids at residues 2 and 9 , along with a putative anchor at residue 7 . HLA-C*06:02 features very negatively charged pockets and thus binds to distinct positively charged peptides. Given that between 1,000 and 3,000 different self-peptides have been detected on HLA-C*06:02 under experimental conditions, multiple cellular proteins should be, in principle, presented by this HLA molecule and recognizable by CD8+ T cells .
Recommended Reading: What Cream Do You Use For Psoriasis
The Bodys Defenses Gone Rogue
Researcher Nehal N. Mehta, M.D., MSCE, is a senior investigator in the Section of Inflammation and Cardiometabolic Diseases at the National Heart, Lung, and Blood Institute in Bethesda, Maryland. For the past six years, he and other scientists in his NHLBI lab have followed a group of 350 people with plaque psoriasis, looking into how chronic inflammation affects their risk of heart disease and metabolic conditions such as diabetes.
âInflammation is simply a collection of immune cells trying to put out a fire, and that fire is usually an infection or some sort of virus,â says Dr. Mehta, a cardiologist and internist.
Setting off this inflammatory response, infiltration of immune cells and release of factors, is what the immune system evolved to do. In psoriatic disease, however, this primal defense has gone awry.
âIn psoriasis, immune cells attack places they shouldnât,â Dr. Mehta says. âThey go to the skin and cause psoriatic plaques, but they can also go to the joints and cause psoriatic arthritis. When they infiltrate blood vessels of the heart, they inflame the cells that line blood vessels. These fill with immune cells that donât belong there and cause inflammation. Thatâs the beginning of cardiovascular disease.â
Psoriasis Linked To Autoimmune Diseases
Patients with psoriasis are more than 50% more likely than patients without psoriasis to have at least 1 other autoimmune disease and are nearly twice as likely to have at least 2 other autoimmune diseases, Jashin J. Wu, MD, director of dermatology research and associate residency program director in the Department of Dermatology at Kaiser Permanente Los Angeles Medical Center, California, and colleagues report in an article June 4 and in the November print issue of the Journal of the American Academy of Dermatology.
Dr. Wu told Medscape Medical News, “Psoriasis patients were more likely also to have other autoimmune diseases, and that the strongest association was with rheumatoid arthritis .”
Dr. Wu and colleagues conducted a retrospective cohort study among 25,341 Kaiser patients, each of whom had 2 or more diagnosis codes for a psoriatic disease and was treated between January 2004 and February 2011. Each was matched with 5 Kaiser members without this case definition but with similar age, sex, and length of plan enrollment. The analysis included Crohn’s disease, ulcerative colitis, type 1 diabetes mellitus, alopecia areata, hemolytic anemia, giant cell arteritis, multiple sclerosis, systemic lupus erythematosus, vitiligo, Graves disease, Hashimoto disease, chronic glomerulonephritis, pulmonary fibrosis, Sjogren syndrome, Addison disease, immune thrombocytopenia, chronic urticaria, celiac disease, and primary biliary cirrhosis.
Send comments and news tips to .
Also Check: Foods To Avoid With Psoriasis Arthritis
Setting The Stage: Psoriasis As An Immune
Figure 1. Complex fine-tuning of innate and adaptive immune mechanisms determines onset, course, and activity of psoriasis. As detailed in the text, intricate interactions between components of the innate with components of the adaptive immune system lie at the core of the pathophysiology of psoriasis. Once established, the relative contribution and fine-tuning of various mediators of adaptive and innate immunity determine the clinical manifestation toward chronic stable vs. highly inflammatory and/or pustular psoriasis.
Supporting Acts: Indispensable Players In The Ensemble Of Psoriasis Immunology
Autoantigen presentation alone does not suffice to induce the psoriatic cascade in genetically predisposed individuals. Rather, costimulatory effects of various gene products orchestrate the activation of the actual autoimmune response. Such risk gene variants modulate inflammatory signaling pathways , peptide epitope processing and/or Th/c17 differentiation .
Table 1. Genetic factors implicated in psoriasis.
These genetic variations create costimulatory signals which modulate innate and adaptive immune mechanisms and shape the proinflammatory environment. In sum and in conjunction with the appropriate HLA molecules and autoantigens, they may eventually exceed the thresholds for activation and maintenance of pathogenic autoimmune and autoinflammatory responses in psoriasis . Likewise, regulatory mechanisms involving programmed death -1 signals have emerged recently as modulators of chronic inflammation in psoriasis . However, the complex interactions of various players are by no means fully understood. Therefore, they are listed here only as a whole.
The autoantigens described so far cannot fully explain the genesis of psoriasis. To give just one example of the latter notion: Psoriatic lesions can also occur in vitiligo foci that do not contain melanocytes . Alterations of resident cell types such as vascular endothelial cells or the cutaneous nervous system are also involved in the disease process . Further research is certainly needed here.
Recommended Reading: Difference Between Dry Skin And Psoriasis
What Is An Autoimmune Disorder
Your body’s immune system is responsible for fighting foreign invaders threatening your health: bacteria, viruses, and fungi are just a few examples. Your good health depends partly on two important features of the immune system:
Unfortunately, when you have an autoimmune disease, your body’s immune system mistakenly confuses what is “self” with what is “other.” Instead of protecting your body, the immune system produces cells and chemicals that attack your own body, causing damage and disease.
There are many different autoimmune diseases, including psoriasis, rheumatoid arthritis, some types of thyroid diseases, some forms of anemia, lupus, celiac disease, and type 1 diabetes.