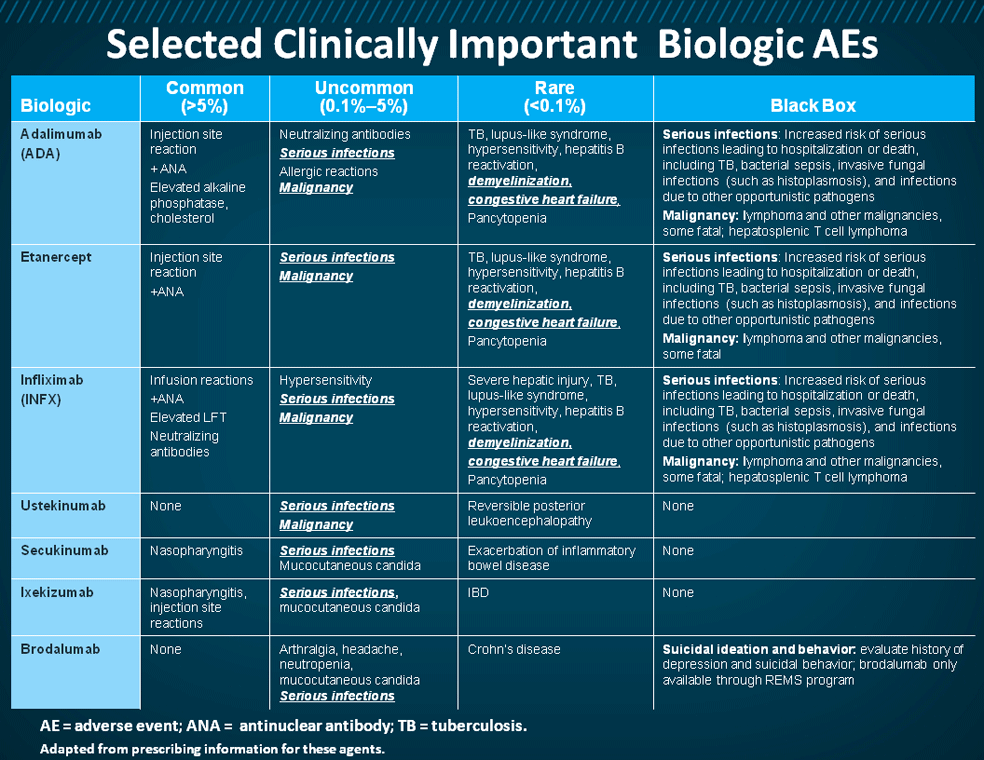
What Are The Possible Side Effects Of Biological Agents
To date, biological agents for psoriasis appear to have very few side effects. Because of their precise targets, they appear not to damage the entire immune system the way that general immunosuppressants do. However, biological agents should still be considered immunosuppressive and may increase the risk of infection and reactivation of tuberculosis . Uncommon infections with organisms such as listeria and legionella may be more common and more serious in patients on biological agents. Infections are more common in older patients on biologics.
Screening for latent TB and other infections should be undertaken prior to commencing a TNF inhibitor and other biological agents.
Biological agents may also increase the risk of skin cancer, especially squamous cell carcinoma and some lymphomas.
On the other hand, mortality may be reduced in patients taking TNF inhibitors compared to that in patients with psoriasis that are not taking them. This is due to a marked reduction in myocardial infarction. Some of the newer biological agents may also be associated with lower rates of malignancy than arise in matched patients that are not taking them.
Emerging Biological Therapies For Psa
Many treatment options are now available for PsA management considering all its clinical subtypes and comorbidities. However some patients have an inadequate response or a relative contraindication to first-line biologic therapy, advocating the development of novel medications with different mechanisms of action, such as T-cell modulators and anti-CD20.
Who Needs This Medication
The biologics do not cure psoriasis or arthritis caused by psoriasis, but they can relieve symptoms and may help prevent further joint damage.
Some medications such as creams, salves, lotions, sprays, or gels are safer and less expensive than the biologics. Or, if a large part of the body is affected, ultraviolet phototherapy or light therapy may be used.
Some people might not get enough relief with those treatments or they might have joint pain that requires other medications. Other options for treating psoriasis include: acitretin , cyclosporine , and methotrexate . These options also cause serious side effects, and doctors disagree about whether it is better to use one of them before trying a biologic.
Another option is apremilast . This is a new type of medication that was approved by the FDA for treating psoriatic arthritis in early 2014, shortly before this report was being prepared for publication. Unlike biologics, Otezla does not suppress the immune system. Since it is brand new, its long-term safety has not been established. If your doctor recommends any of these drugs, you should ask about the advantages and disadvantages compared with a biologic.
Don’t Miss: How To Stop Itching Skin From Psoriasis
Things To Consider When Taking A Biologic
Biologics are a type of medication that can be prescribed for some forms of inflammatory arthritis .
This sheet gives you general information about how biologics work, why they are used, as well as tips on the safe use of these medications.
This resource does not provide advice about the specific biologic you may be prescribed to manage your arthritis. It does not cover all the side effects and safety precautions that can occur with each biologic. You should discuss this with your doctor, rheumatology nurse or pharmacist, or see the For more information section at the end of this resource.
From The Academyguidelines Of Care For The Management Of Psoriasis And Psoriatic Arthritis: Section 2 Psoriatic Arthritis: Overview And Guidelines Of Care For Treatment With An Emphasis On The Biologics
Psoriasis is a common, chronic, inflammatory, multisystem disease with predominantly skin and joint manifestations affecting approximately 2% of the population. In this second of 5 sections of the guidelines of care for psoriasis, we give an overview of psoriatic arthritis including its cardinal clinical features, pathogenesis, prognosis, classification, assessment tools used to evaluate psoriatic arthritis, and the approach to treatment. Although patients with mild to moderate psoriatic arthritis may be treated with nonsteroidal anti-inflammatory drugs and/or intra-articular steroid injections, the use of disease-modifying antirheumatic drugs, particularly methotrexate, along with the biologic agents, are considered the standard of care in patients with more significant psoriatic arthritis. We will discuss the use of disease-modifying antirheumatic drugs and the biologic therapies in the treatment of patients with moderate to severe psoriatic arthritis.
- Previous article in issue
Don’t Miss: Can Psoriasis Spread To Face
Biological Dmards Other Than Tnfi
Although TNFi therapy remains central in the management of PsA, new insights into its pathogenesis led to identification of new therapeutic targets, including IL-12, IL-23, and IL-17. The IL-17 signaling pathway plays a relevant role in the pathogenesis of PsA. This proinflammatory cytokine is richly expressed in psoriatic skin lesions and in the synovial fluid of patients and can induce activation and proliferation of keratinocytes and endothelial cells. On the other side, IL-23 has been shown to play an important role in the polarization of CD4+ T-cells to become IL-17 producers. In the last few years, therapeutic agents targeting the IL-23/IL17 axis have been studied for the treatment of PsA.
Pooled meta-analysis was conducted by Mourad et al identifying RCTs evaluating the efficacy of TNF-i, anti-IL12/23 , and anti-IL17 in treating PsA and conducting a meta-analysis of these agents for treatment of dactylitis and enthesitis. Their results showed that TNF-i and IL inhibitors brought dactylitis to a significant resolution at week 24, with pooled risk ratios versus placebo of 2.57 and 1.88 respectively. For resolution of enthesitis at week 24, RR for TNF-i was 1.93 versus 1.95 for IL inhibitors. According to these results, TNF-i demonstrated the same efficacy of IL inhibitors in treating the two PsA manifestations.
Biological Agents For Other Types Of Skin Disease
Other biological agents used for severe skin diseases include:
- Dupilumab , which blocks the IL-4 receptor alpha subunit and is used for atopiceczema
- Rituximab , which is a CD20 antagonist and was initially used for B-cell lymphoma and now for rheumatoid arthritis and granulomatous polyangiitis
- Anakinra , which is an interleukin -1 antagonist registered for rheumatoid arthritis but also found to be helpful for autoinflammatory syndromes such as Schnitzler syndrome, cryopyrin-associated periodic syndrome and adult Still disease
- Omalizumab , which blocks the high-affinity receptor binding site on human immunoglobulin E and is used for asthma and chronic spontaneous urticaria in adolescents and adults > 12 years
- Lanadelumab is a monoclonal antibody that inhibits kallikrein and is used to treat hereditaryangioedema.
There are many other promising biological agents under investigation for skin conditions.
Recommended Reading: Why Do People Get Psoriasis
Other Possible Adverse Effects
It is known that RA itself, and recently a spondyloarthropathy are associated with a higher prevalence of lymphoma. In the case of RA, it has been shown that the risk is two to eight times the risk of the general population. In clinical trials, the standardised incidence ratio with the different anti-TNF agents has been within the SIR of patients with RA. Thus, when a lymphoma arises in the context of anti-TNF therapy, it is not known whether this occurred because of the therapy, as a result of having the underlying disease, or if it is completely unrelated to disease and treatment. We do not know the background incidence of lymphoma in a PsA population.
A small number of patients have developed or have exacerbated multiple sclerosis temporally coincident with anti-TNF therapy. TNF inhibitors should be avoided in patients with multiple sclerosis.
Are There Potential Side Effects I Should Expect From Biologics
When you take any medication, including biologics, you have to weigh its risks against its benefits , according to Dr. Keller. He says the vast majority of his psoriasis patients have no problems when taking these medicines.
But side effects can happen, so its important to have this discussion with your doctor. One of the most common is a skin reaction like localized inflammation or bruising at the injection site. These symptoms should improve within a day or two, and after youve had a few shots they may stop altogether.
When National Psoriasis Foundationvolunteer Jaime Lyn Moy first went on a biologic, her biggest concern was that it might suppress her immune system and make it harder for her body to fight infections. Shed already seen that happen to her son, who also has psoriasis. He would get infections pretty easily and he would have a more difficult time overcoming them. I was wondering if my outcome would be similar to his, she says. As suspected, she did see an uptick in infections like bronchitis and the flu, and she was slower to get over them than she was before going on biologics.
Thats because biologics dial down the immune system, meaning an increased chance of infection is a real risk. So your doctor will carefully screen you before putting you on one of these drugs to make sure you dont have a latent tuberculosis or hepatitis infection in your body that the biologic might reignite, according to Johns Hopkins Medicine.
Recommended Reading: Is Castor Oil Good For Scalp Psoriasis
Why Do Dermatologists Prescribe A Biologic To Treat Psoriasis
A biologic is an important treatment option for people with moderate-to-severe psoriasis, psoriatic arthritis, or both. For many people, taking a biologic was life changing because it helped control their symptoms when other treatments failed.
Benefits of biologics
Using a biologic to treat psoriasis is life changing for some people.
Biologics work by blocking reactions in your body that cause psoriasis and its symptoms.If you have psoriatic arthritis, a biologic can stop the pain, stiffness, and swelling in your joints. It can prevent the arthritis from worsening and causing more damage to your joints. The US Food and Drug Administration has approved the following biologics to treat adults with psoriasis or psoriatic arthritis. In many cases, these biologics have been approved to treat both diseases.
| Drug |
|---|
| X |
1Approved to treat adults when other psoriasis treatments fail to work or stop working.
Sometimes, a biologic is prescribed to treat a child who has psoriasis. This can be very effective for a child who has severe psoriasis. The FDA has approved usetekinumab to treat people 12 years of age and older who have moderate-to-severe psoriasis.
Efficacy And Safety Of Biologics
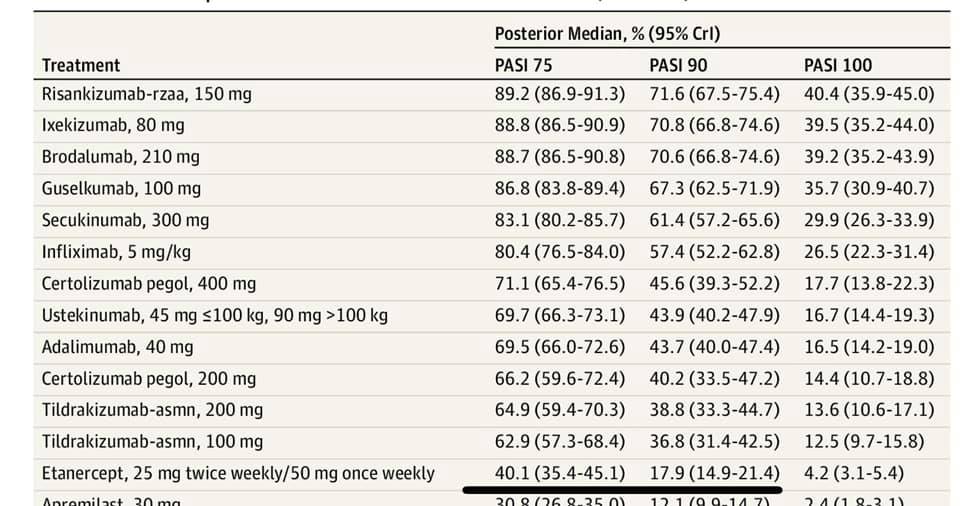
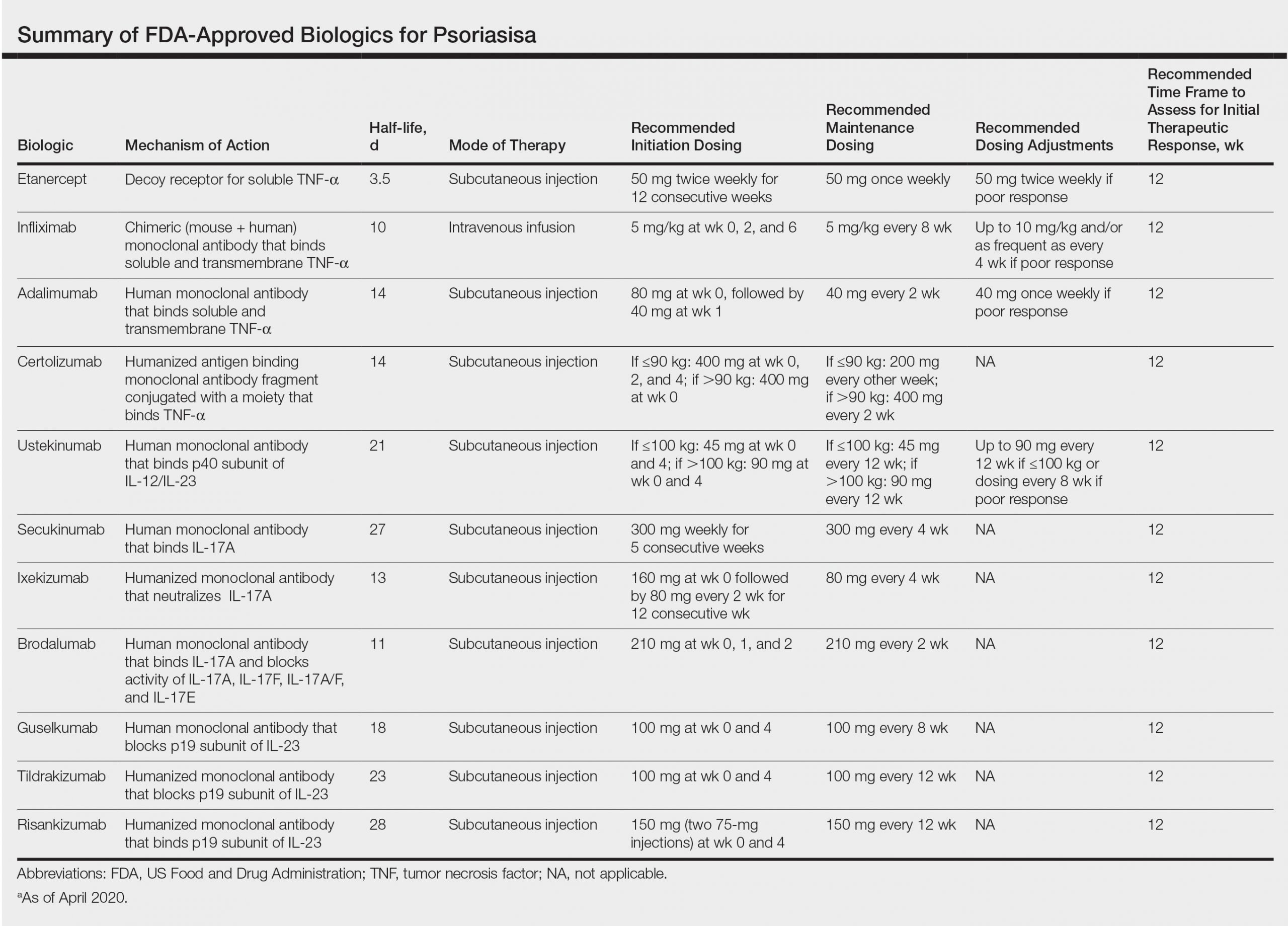
Although approved biologic agents differ by countries, biologic agents commonly used for the treatment of psoriasis are categorized into three groups, tumor necrosis factor – inhibitors, interleukin -23 inhibitors, and IL-17 inhibitors, as shown in . Infliximab, adalimumab, etanercept, certolizumab-pegol, and golimumab are TNF- inhibitors. Golimumab is used only for PsA. Ustekinumab is an anti-IL-12/23p40 antibody. Guselkumab, risankizumab, tildrakizumab, and mirikizumab are anti-IL-23p19 antibodies. Secukinumab, and ixekizumab are anti-IL-17A antibodies. Brodalumab is an anti-IL-17RA antibody. Bimekizumab is an anti-IL-17A/F antibody, which blocks both IL-17A and IL-17F. Many randomized controlled trials were conducted, and they demonstrated that the drugs are efficacious for moderate-to-severe plaque psoriasis. Recently, network meta-analyses enabled indirect comparison among those agents.
Read Also: How To Stop Plaque Psoriasis
Can Biosimilars Be Used With Other Treatments
It is important to tell your health care provider about all treatments, medicines, vitamins or supplements that you are taking.
Like all biologics, biosimilars can be used with other treatment options including topicals and phototherapy. The biologics Enbrel, Humira and Remicade are shown to be safe and effective when taken with methotrexate. This means that their biosimilars, including Erelzi, Amjevita, and Inflectra, may be safe and effective when taken with methotrexate.
- With Inflectra being the biosimilar to Remicade, its use in combination with phototherapy may increase the risk for skin cancer.
- No drugs that interact with biologics should be combined with their respective biosimilars.
Key Points For Decision Makers
| This CEA compares ixekizumab and secukinumab in PsA in the UK this comparison to secukinumab was considered particularly relevant in a decision-making context . |
| In both bDMARD-naïve and -experienced patients with PsA and concomitant moderate-to-severe psoriasis, ixekizumab provided more QALYs at a lower cost than secukinumab. |
| Although gains with ixekizumab were modest, the findings of this CEA, along with patient preferences and other factors, may be helpful in clinical decision-making. |
Recommended Reading: Light Therapy For Scalp Psoriasis
How Much Improvement Can I Expect
This is where all that agonizing decision-making can pay off. Todays biologics work so well that most people see significant improvement or even complete skin clearance. More than half of people who take newer generation biologics see 100% skin clearance within five months on the drug, according to a 2020 study published in the International Journal of Molecular Sciences.4
Half of the patients I put on a biologic are clear or close to clear. Those patients either dont get any psoriasis at all anymore, or they only have an occasional psoriasis plaque, say, in the wintertime or in times of significant stress, Dr. Keller says.
What Is The Best Biologic For Psoriatic Arthritis
New psoriatic arthritis treatment guidelines from the American College of Rheumatology say that most people with active psoriatic arthritis should choose an anti-TNF drug, such as adalimumab or infliximab , as their first line of therapy.
Considering this, Is TREMFYA better than Stelara? Patients receiving TREMFYA had a significantly greater number of visits from week 28 to week 40 with an Investigators Global Assessment score of 0 or 1 and 2-grade improvement from week 16 vs patients receiving STELARA .
What is the new drug for psoriatic arthritis? is a new kind of drug for long-term inflammation diseases like psoriatic arthritis. Its a pill that works by blocking a specific enzyme, a kind of protein, called PDE-4. That helps to slow other reactions that lead to inflammation.
Furthermore, What is the safest drug to take for psoriatic arthritis? What Is the Safest Drug for Psoriatic Arthritis?
- Over-the-counter Ibuprofen Naproxen Aspirin.
- Prescription. Celecoxib
Also Check: Psoriasis Medications Covered By Medicare
How Are Biologics Used To Treat Psa
Inflammation typically causes the swelling, stiffness, and joint pain that defines PsA.
Biologics used to treat PsA specifically target different pathways in the body that create inflammation. This is different from traditional drugs, which target many steps in the immune system.
Depending on your psoriatic arthritis symptoms and medical history, your doctor may recommend one of several biologics for relief.
What Are The 5 Types Of Psoriatic Arthritis
Psoriatic arthritis is categorized into five types: distal interphalangeal predominant, asymmetric oligoarticular, symmetric polyarthritis, spondylitis, and arthritis mutilans.
What aggravates psoriatic arthritis? Saturated fats, sugar, alcohol, and simple carbohydrates can add pounds, cause inflammation, and trigger psoriatic arthritis flares. Try to avoid foods such as: Processed meats like hot dogs, sausages, and bacon. Sugary drinks.
Is Celebrex good for psoriatic arthritis?
Both doses of celecoxib were well tolerated. Conclusions: Celecoxib 400 mg and 200 mg qd were efficacious and well tolerated in treating the signs and symptoms of PsA in flare after 2 weeks of treatment.
Can CBD help with psoriatic arthritis? Psoriasis and psoriatic arthritis are painful, chronic conditions that can cause stress and anxiety. CBD is an alternative treatment that may help reduce pain and inflammation and relieve anxiety related to PsA.
Also Check: Can You Have Psoriasis In Your Mouth
Types Of Psoriasis Medication
Treatments for autoimmune conditions focus on reducing or controlling the immune system response in your body. Sometimes, localized psoriasis treatments are used to treat a small patch of affected skin. Other times, systemic therapies are required to manage psoriasis.
Systemic treatments are those that work throughout the body, reaching all areas by traveling through the bloodstream. Systemic psoriasis drugs can be grouped into two categories: biologics and pharmaceuticals. Your healthcare team will consider your situation and discuss different treatment options.
Systemic therapy usually is reserved for people with severe psoriatic disease. “Severe” is defined as psoriasis covering more than 5% of the body’s surface or involves high-impact areas like the face or genitals.
Generally, psoriasis medications decrease the symptoms of active psoriasis and help reduce the risk of long-term comorbidities . Comorbidities include:
In the United States, the Food and Drug Administration regulates the manufacturing of both pharmaceuticals and biologics.
How Well Do The Biologic Drugs Work To Relieve Arthritis Caused By Psoriasis
All six biologic drugs included in our analysisadalimumab , certolizumab , etanercept , golimumab , infliximab , and ustekinumab are FDA-approved to treat psoriatic arthritis. The biologic drugs reduce joint pain and inflammation and improve the quality of life in up to 80 percent of people with this condition.
There are no head-to-head trials of biologic drugs to treat arthritis caused by psoriasis. Other studies that attempted to compare them indirectly had mixed results, but most found no difference in effectiveness among Humira, Enbrel, and Remicade. Simponi was approved after these studies were done. In the only major study of Simponi, about half of people who received it had at least a 50 percent improvement in joint pain, swelling, and function.
Don’t Miss: Como Se Cura La Psoriasis
How I Cured My Psoriatic Arthritis Naturally
Natural remedies
- Turmeric. Curcumin, which is an ingredient in turmeric, appears to have anti-inflammatory properties.
- Capsaicin. Capsaicin is the compound that makes chili peppers hot.
- Epsom salts.
- Massage therapy.
Can Skyrizi cause death?
Adverse events leading to discontinuation of the study drug were 1.2 percent in the SKYRIZI group and 4.9 percent in the COSENTYX group. There were no deaths in either treatment group.
Is Taltz better than Tremfya? Patients treated with Taltz demonstrated statistically significantly higher improvements than those treated with TREMFYA as measured by PASI 100 at Week 12 . Additionally, all major secondary endpoints up to Week 12 were achieved .
Is Tremfya better than Cosentyx? from Novartis, according to recent data published in the Journal of Dermatological Treatment.
Usage With Psoriasis Treatments
In addition to DMARDs like methotrexate, current biologics can be used in conjunction with these psoriasis therapies:
Topical treatments, whichare applied directly to the skin and are a first-line treatment for psoriasis. They slow down or normalize excessive skin cell growth and reduce skin inflammation.
, also called light therapy, which exposes skin to ultraviolent light under medical supervision. Exposure needs to be consistent to penetrate skin and slow skin cell growth. Phototherapy may, however, increased the risk of skin cancer if a person is taking TNF-inhibitors or vice versa. This is because photosensitivity is a side of effect of these medications.
Recommended Reading: Best Skin Moisturizer For Psoriasis