What About Physical Contact
Before doctors knew what caused psoriasis, they often confused it with leprosy — and people who had it were considered contagious. But now we know that you cannot catch the condition by brushing up against someone who has it. You also can’t get it from kissing, having sex, or swimming in the same water.
People get psoriasis because of their genes, not because of bad hygiene, their diet or lifestyle, or any other habits. They didnât get it from someone else, and they cannot infect others.
Even so, thereâs a lot of stigma around the condition, which can be hard for people who have it. They might feel uncomfortable when people stare at their lesions or avoid touching them, and they may try to hide their outbreaks under long clothing.
If you have psoriasis, you can help put an end to confusion and misunderstandings about the disease by talking openly with friends, family, and co-workers. And if you know people who have it, make sure they know that their condition doesn’t affect your opinion of them or make you not want to be around them.
What’s The Difference Between Psoriasis And Eczema
Psoriasis and eczema are skin conditions that can be red, itchy, and annoying, and both are rooted in a family history. But the similarities essentially stop there. Here are a few key ways theyre different:
-
Psoriasis is usually thick, scaly, and raised, and sometimes silvery or purplish. Eczema looks more like dry flaky skin.
-
Eczemaoften called atopic dermatitis, its most common typeis more prolific, affecting more than 7% of adults and 8-12% of children. Only around 3% of the population has psoriasis, and it usually appears later in life rather than during childhood.
-
Psoriasis is an autoimmune condition that can lead to more debilitating health issues, such as psoriatic arthritis, while eczema is just about skin.
-
Eczema can often be remedied with over-the-counter treatments and creams, but psoriasis often requires Rx medications and sometimes injections and laser therapy.
Is There A Cure For Psoriasis
Unfortunately, there is no cure for psoriasis. However, there are multiple ways to manage the disease. Medications, light therapy, stress reduction, adjunctive therapy sessions, moisturizers with salicylic acid, and sunlight are treatments. Some treatments can be used together. For best results, many clinicians suggest psoriasis be managed by a dermatologist skilled in treating this chronic disease.
Recommended Reading: Blue Star Cream For Psoriasis
Risk Factors For Psoriasis That Spreads
Psoriasis is more likely to spread and become severe when it is left untreated. So treatment from a doctor who specializes in psoriasis can significantly reduce the risk that psoriasis will spread, or that the next flare-up will be worse than the last.
A family history of psoriasis, having another immune system disorder, smoking, trauma to the skin, and exposure to many psoriasis triggers are additional risk factors that might cause psoriasis to spread.
It is essential to moisturize the skin because it can speed the healing process and prevent itching. A range of moisturizing lotions that are suitable for psoriasis are available without a prescription.
Tar shampoo and soap may also help. Ingredients that encourage old skin cells to fall off, such as salicylic acid, can reduce the appearance of flaky plaques. However, some of these products can be harsh on the skin, so getting advice from a professional can help determine the most suitable lotion.
Steroid creams, such as hydrocortisone, are also safe and effective for most people. They help with itching and can speed healing. Using steroid creams for a very long time may cause side effects, however, so talk to a doctor about the safe use of steroids.
Th World Health Assembly Recognizes Psoriasis As A Serious Non
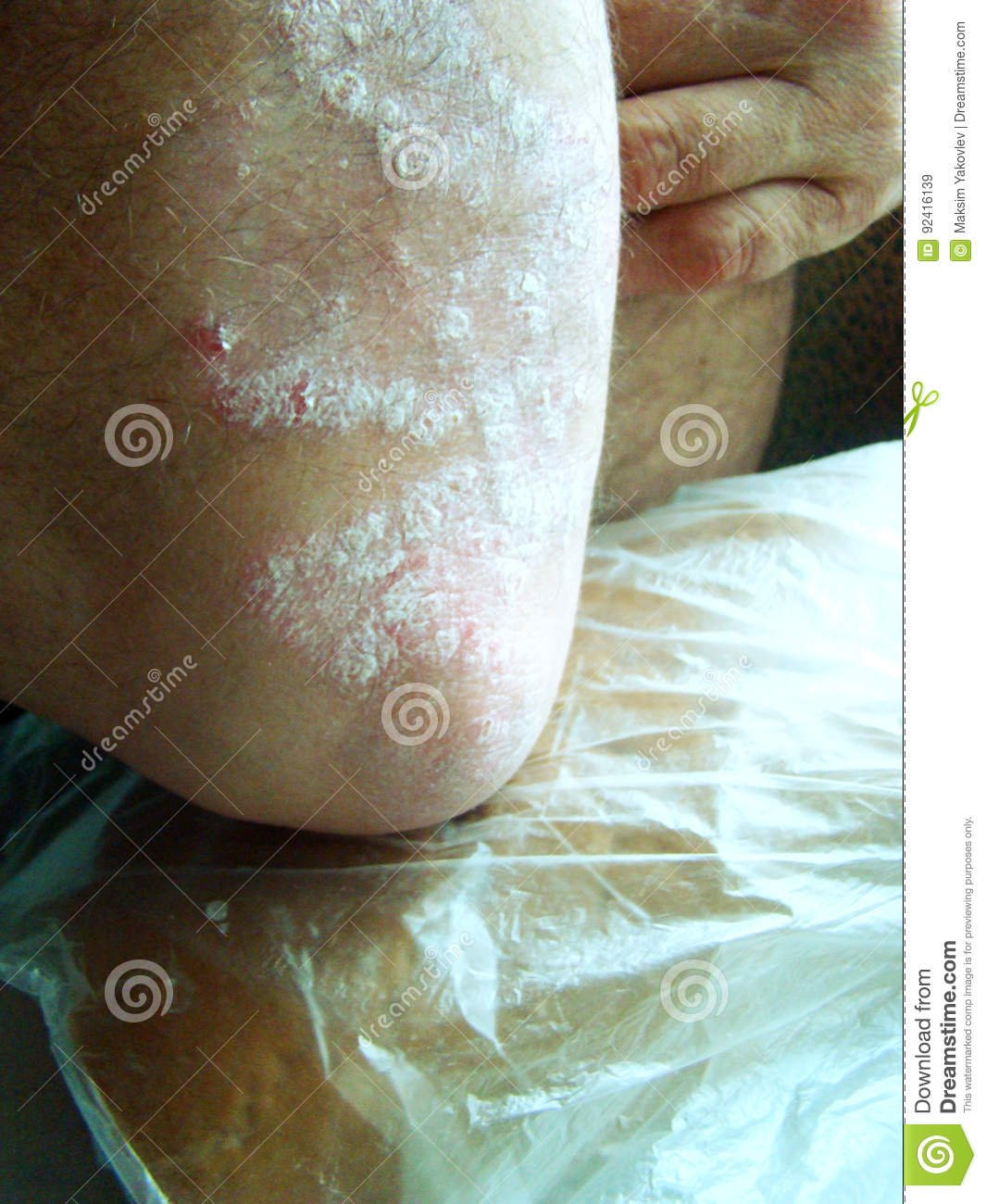
istoric day for the global psoriasis community, as WHO resolution on psoriasis is adopted by World Health Assembly
At the 67th World Health Assembly, the WHO member states adopted a resolution on psoriasis, recognizing it as a chronic, non-communicable, painful, disfiguring, and disabling disease for which there is no cure. The resolution also acknowledges the psychosocial burden of the disease and that many people with psoriasis suffer due to lack of awareness and access to sufficient treatment.
Lars Ettarp, President of the International Federation of Psoriasis Associations comments:IFPA, together with its member associations and leading medical societies, has long called for the WHO and its member states to recognize the serious nature of psoriasis. Finally, the voices of the more than 125 million people who live with psoriasis have been heard, and on this historic day for the global psoriasis community we wish to express our great appreciation for all the stakeholders involved in bringing about this important resolution, especially all the WHO member states that have shown their support for our cause.
Link to the WHO resolution EB133.R2
AcknowledgmentsIFPA wishes to thank the following for their invaluable support and commitment to the global psoriasis community:
About:
You can read more about IFPA, our members and our activities on our website www.ifpa-pso.org.
Tags:
You May Like: Light Therapy For Psoriasis At Home
What Are The Types Of Psoriasis
According to the Mayo Clinic1, there are several types of psoriasis:
Plaque psoriasis is common and appears as dry, raised patches of skin covered with scales. Generally, these plaques happen on your elbows, knees, lower back, and scalp.
Nail psoriasis affects your fingernails and toenails. You may have many different symptoms including pitting, abnormal nail growth, discoloration, or separation of your nail from the nail bed.
Guttate psoriasis is more common in young adults and children. It can happen after you get an infection like strep throat and produces lesions that look like small drops on your abdomen, arms, or legs.
Inverse psoriasis primarily affects the groin, butt, and breast areas. The patches are smooth and tend to get worse when you sweat a lot or experience a lot of friction.
Pustular psoriasis is rare and causes sores that are filled with pus. You may get them on your palms or the soles of your feet.
Erythrodermic psoriasis is uncommon and causes a peeling, burning rash that can appear on your entire body.
You may read articles or hear other people discuss psoriatic arthritis in conjunction with psoriasis. Psoriatic arthritis is another autoimmune condition that causes painful, swollen joints. Having psoriasis increases your risk of developing psoriatic arthritis, so its important to let your doctor know of any joint symptoms you develop, according to the Cleveland Clinic.
When Is Psoriasis Typically Diagnosed
According to the National Psoriasis Foundation, psoriasis often develops between the ages of 10 and 35. It may appear at any age, though. Up to 15 percent of people with psoriasis are diagnosed before age 10. In rare cases, infants can develop the condition.
Dermatologists usually diagnose psoriasis, although many primary care physicians will recognize it. Most doctors diagnose psoriasis by performing a visual skin exam and assessing family medical history. Youre considered at risk of developing psoriasis if you have one parent with the disease. If you have two parents with psoriasis, this risk is higher.
In some cases, a doctor can perform a skin biopsy to confirm the diagnosis and the type of psoriasis you have.
No cure for psoriasis is available yet. The disease may go into remission, however. The goal of psoriasis treatment is to stop or slow the appearance of any lesions, and then discover any triggers to mitigate outbreaks. This is done through slowing the growth of skin cells, reducing inflammation and scaling, and smoothing the skin. You may be able to accomplish this through medication, topical treatments, and light therapy.
You May Like: How To Cure Psoriasis On Feet
What’s The Difference Between Contact Dermatitis And Psoriasis
Psoriasis is a chronic skin condition caused by genetics and a hyperactive immune system, and it can flare at any time. Once you have these red, scaly patches of skin, you usually have ’em for good.
While contact dermatitis can also be itchy, red, swollen, and sore, it isnt raised and thick like psoriasis most often is. Its also not chronic: As its name implies, contact dermatitis only occurs when your skin comes into contact with a substance that causes a reaction. This can include anything from laundry detergent to jewelry made with nickel.
How Do You Develop Psoriasis
The exact cause of psoriasis isnt fully understood. Its thought that overactive T cells, which are cells that fight off viruses and bacteria in your body, are involved. In people with psoriasis, T cells attack healthy skin cells and activate other immune responses. This increases the production of healthy skin cells, T cells, and other white blood cells.
As a result, too many skin cells accumulate on the skins outer layer. This is why some types of psoriasis cause the skin to have a scaly appearance. It normally takes weeks for new skin cells to form, but in people with psoriasis, skin cells form within days. The body doesnt shed the excess cells and psoriasis lesions occur.
People with a compromised immune system, including those with HIV or those who get repeated infections, have a higher risk of getting psoriasis.
Many environmental and lifestyle factors may trigger psoriasis flares. Not everyone with psoriasis has the same triggers. Common triggers are:
- sun exposure
- skin trauma, such as cuts, bug bites, and burns
- stress
- certain medications, such as lithium, blood pressure medications, and iodides
- heavy alcohol use
Smoking isnt just a psoriasis trigger. It may also be involved in its development and increase the severity of the disease.
Research shows that smoking may cause one in five cases of psoriasis and doubles your risk of getting the condition. This may be due to the effects of nicotine on skin cells, skin inflammation, and your immune system.
Also Check: Mejor Tratamiento Para La Psoriasis
Causes And Risk Factors Of Psoriasis
Psoriasis, in general, is a genetic condition passed down through families. “It’s likely that multiple genes need to be affected to allow psoriasis to occur and that it’s frequently triggered by an external event, such as an infection,” says James W. Swan, MD, professor of dermatology at the Loyola University Stritch School of Medicine in Maywood, Illinois.
Certain risk factors, such as a family history or being obese, may increase your odds of developing psoriasis.
According to the National Psoriasis Foundation , at least 10 percent of people inherit genes that could lead to psoriasis, but only 3 percent or less actually develop the disease. For this reason, it is believed that the disease is caused by a combination of genetics and external factors or triggers.
A psoriasis outbreak may be provoked by:
Biologics Target Cell Growth
Many of the recent advancements in the treatment of psoriasis have been in the introduction of new oral and injectable medications for moderate-to-severe psoriasis. These medications, called biologics, are protein-based drugs developed from living cells that target specific parts of the immune system to control the rapid growth and movement of skin cells. The biologics approved for the treatment of moderate-to-severe psoriasis include etanercept , infliximab , adalimumab , ustekinumab , golimumab , apremilast , secukinumab , and ixekizumab . Most of these drugs are injections used for people who have failed to respond to traditional therapy or who also have psoriatic arthritis. If you have any questions about psoriasis or about the medications used to manage it, speak with your trusted local pharmacist or another healthcare provider.
Don’t Miss: Safe Psoriasis Treatment While Pregnant
What Is Psoriasis Symptoms Causes Diagnosis Treatment And Prevention
Psoriasis is an autoimmune disease that causes plaques, which are itchy or sore patches of thick, dry, discolored skin.
While any part of your body can be affected, psoriasis plaques most often develop on the elbows, knees, scalp, back, face, palms, and feet.
Like other autoinflammatory diseases, psoriasis occurs when your immune system which normally attacks infectious germs begins to attack healthy cells instead.
What Are Psoriasis Causes And Risk Factors
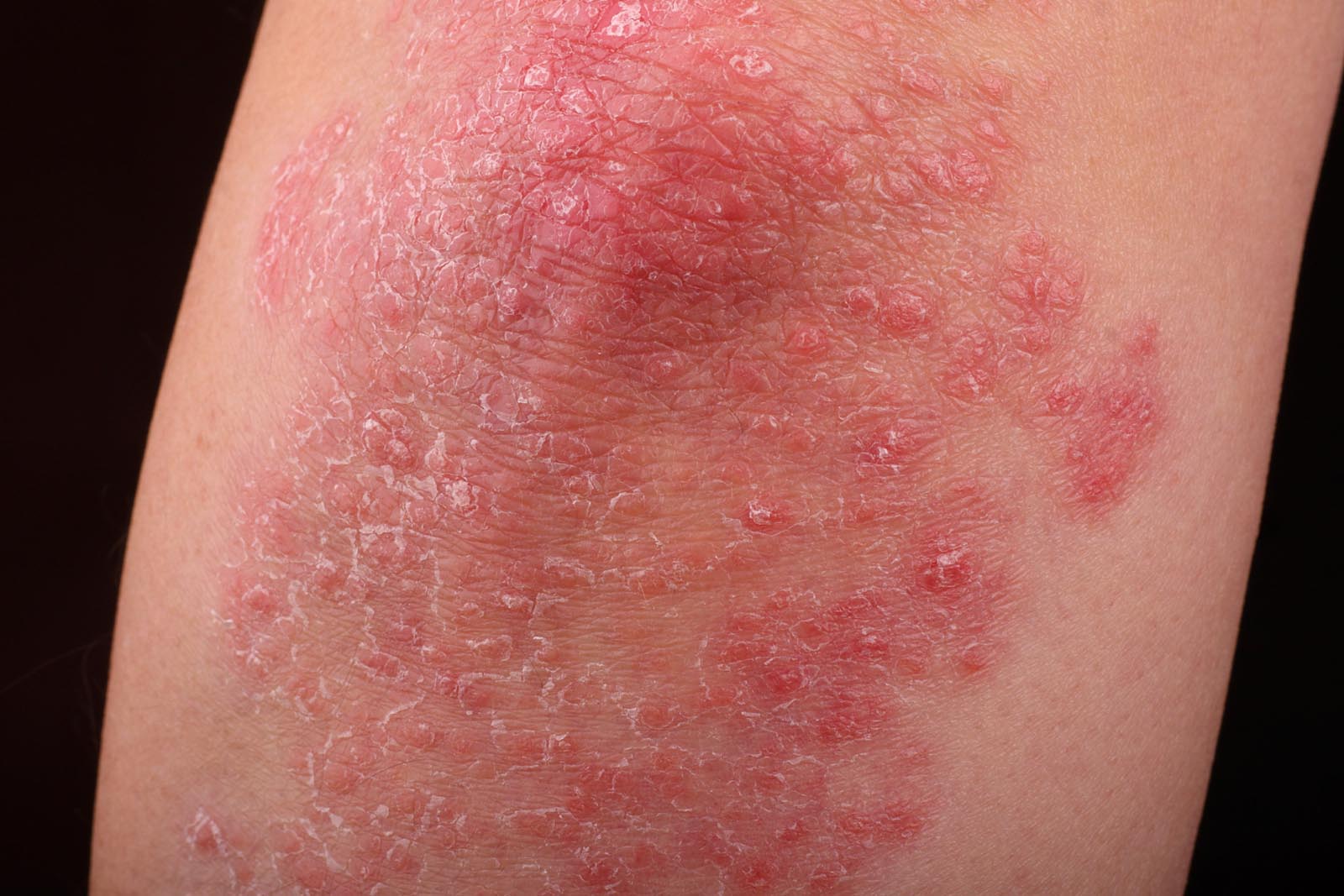
The immune system plays a key role in psoriasis. In psoriasis, a certain subset of T lymphocytes abnormally trigger inflammation in the skin as well as other parts of the body. These T cells produce inflammatory chemicals that cause skin cells to multiply as well as producing changes in small skin blood vessels, resulting ultimately in elevated scaling plaque of psoriasis.
Psoriasis has a genetic basis and can be inherited. Some people carry genes that make them more likely to develop psoriasis. Just because a person has genes that would make him more likely to have psoriasis doesn’t mean he will have the disease. About one-third of people with psoriasis have at least one family member with the disease. Certain factors trigger psoriasis to flare up in those who have the genes.
Environmental factors such as smoking, sunburns, streptococcal sore throat, and alcoholism may affect psoriasis by increasing the frequency of flares. Injury to the skin has been known to trigger psoriasis. For example, a skin infection, skin inflammation, or even excessive scratching can activate psoriasis. A number of medications have been shown to aggravate psoriasis.
Psoriasis flare-ups can last for weeks or months. Psoriasis can go away and then return.
Plaque psoriasis is the most common type of psoriasis and is characterized by red skin covered with silvery scales and inflammation. Plaques of psoriasis vary in shape and frequently itch or burn.
Also Check: What Happens If You Pick Psoriasis
How Do You Get A Psoriasis Diagnosis
Your physician will do a physical exam if they think you have psoriasis. They will probably also ask if you have any symptoms like itchy skin in addition to getting your medical history so they can learn if you have blood relatives with the condition or if youve experienced possible psoriasis triggers.
Your doctor may also remove a very small piece of your skin that can be analyzed to confirm that you have psoriasis, according to the AAD3. A biopsy can also help your doctor rule out other skin disorders and diagnose your specific form of psoriasis, according to the Mayo Clinic1.
For people of color, getting diagnosed with psoriasis can be really frustrating. Often, people with dark skin are misdiagnosed with other skin conditions because theres not enough medical awareness about how psoriasis looks on skin of color.
The length of time youve have psoriasis, any treatments you are using to help your symptoms, and scratching your flare can change the way psoriasis looks, according to Dr. Wassef. So, your physician might do a biopsy just to confirm that you do have psoriasis if they cant tell visually.
Whats Triggering Your Psoriasis Flare
Science isnt exactly sure what causes psoriasis. It seems to be a combo of genetics, environmental triggers, and your immune system going rogue against your skin cells.
If youre genetically predisposed to psoriasis , youll prob experience your first flare-up because of an environmental trigger.
Even folks with a tried-and-true treatment protocol can get flare-ups. Theres just no way to control *everything* around you and trying to control everything would be a lot of stress.
Most psoriasis flare-ups start as a small itchy patch that spreads pretty quickly. Scratching it wont speed up the spread, but it could lead to irritation and infection.
You May Like: Il 17 Inhibitors For Psoriasis
Patient Discussion About Communicable Disease
Q. Is psoriasis infectious? Last week I and my friends from high-school went to the pool. One of my friend has psoriasis on his back, and when the lifeguard noticed it he asked him to leave the pool because he has skin disease that may spread to the other people swimming in the pool. We told him it is psoriasis and not some fungus, but he told us that psoriasis is also infectious. Is that true? Can psoriasis infect people who come in touch with people with psoriasis? Can I go swimming with him or should be more cautious?
A.
Q. Is leukemia contagious? A friend of mine got leukemia , can I get it from him if he bleeds and I touch the blood? Like HIV I mean.
A.
Q. Is psoriasis contagious? My wife got psoriasis and I dont want to get infected
A.
So Who Can Get Psoriasis And Why
Psoriasis is whats called a multifactorial traitthis means that we inherit genes which confer risk for, or protection from, psoriasis from each of our parents, which gives us a relative predisposition to develop psoriasis, says Keith Choate, MD, a Yale Medicine dermatologist in New Haven, Connecticut. Basically, your parents pass it down to you.
But even if you have the gene, it doesn’t necessarily mean you’ll develop psoriasisit has to then be set off by an environmental trigger. “A persons genetic likelihood plus his or exposure to an environmental trigger ultimately determines when and if that person will develop psoriasis,” says Dr. Choate.
You May Like: What Is Guttate Psoriasis Pictures
Myth #: Itching Your Skin Will Cause Psoriasis To Spread
Psoriasis isnt a skin infection and cant be spread through touching or itching. However, a person can develop the Koebner phenomenon. This is the appearance of new skin lesions on areas of trauma, such as scratches or cuts. It is also known as the isomorphic response.Some experts suggest that 25% of people with psoriasis may experience the Koebner phenomenon.Sometimes, it is not possible for a person to avoid a cut or scrape. However, people can take some measures to reduce the potential of skin irritations. These include avoiding:
- Getting sunburned: Use sunscreen, stay in the shade, or wear sun protective clothes that cover the body.
- Contact with irritants: Products ranging from beauty treatments to household chemicals can irritate the skin.
- Scratching: Use topical treatments during a psoriasis flare to reduce itching.
- Injuries and bites: Wear clothes that cover the body when gardening, camping, and so on.
- Rubbing the skin: When bathing or showering, use products that a doctor recommends. Use lukewarm water, wash gently with the palms of the hands, and pat the skin dry after bathing. Avoid abrasive substances and sponges and try not to rub the skin.
- Stress
- Oral medications
- Medications by injection or through an intravenous infusion
- A doctor who specializes in dermatology, or treating skin disorders, can assess the severity of psoriasis and recommend the best treatment.