There Are Many Treatment Options Available To People With Psoriasis And Psoriatic Arthritis It Can Seem Overwhelming But It Sure Beats Not Having Enough Options
Mild psoriasis is typically treated with creams, ointments, and lotions applied directly to the skin, most often with topical steroids. Mild psoriasis treatments are examined here. Those with moderate or severe psoriasis also sometimes use such topical treatments, particularly for stubborn psoriasis patches or other hard-to-treat areas.
But most moderate to severe psoriasis and psoriatic arthritis is treated with treatments that impact the whole body: ultraviolet lights directed at the skin, pills that are taken by mouth, injections made under the skin, and infusions directly into the bloodstream.
Today patients can select treatments that are more effective, more safe, and able to be used longer than ever before. We review these options below.
Could It Be An Allergy
Many patients Ive seen over the years experience various kinds of allergies. The question is, could it be an allergy or could your symptoms be more indicative of psoriasis, rheumatoid arthritis or both? There are many different kinds of signs and symptoms as well as reactions that are common both to allergies as well as psoriasis and RA. Symptoms that are typical of an auto-immune disorder are light sensitivity, dry eyes and mouth, recurrent headaches and swollen glands.
One good tip that will allow you to distinguish between seasonal allergies and auto-immune disease is just that seasonal. Do your symptoms seem to get worse in spring or fall as opposed to being there all the time? If you experience typical seasonal allergic-type of symptoms then it is much more likely to occur at certain times of the year. Do your symptoms appear randomly, unexpectedly or are continuous without a break? Then its time to see your health-care professional for a more formal diagnosis.
Papers Of Particular Interest Published Recently Have Been Highlighted As: Of Importance
This is large, high quality randomised controlled trial of an adalimumab biosimilar
Recommended Reading: Shampoo For Eczema And Psoriasis
What Happens To Patients With Psoriatic Arthritis
Genes implicated in the pathogenesis of PsA include Cw6,IL-23 R alleles and Act1, a molecule in the IL-17R signaling pathway and other MHC Class I alleles , Class I major histocompatibility complex chain-related gene A . Environmental events have also been associated with the onset of psoriatic arthritis, including rubella vaccination, injury sufficient to require a medical consultation, recurrent oral ulcers, moving house and fracture requiring hospitalization.
From a clinical perspective, PsA patients can present with features of RA or spondyloarthritis . The synovial pathology is more akin to findings in spondyloarthritis than RA with infiltrating neutrophils, CD163+ macrophages, and the lack of an antibody response to the shared epitope as observed in RA.The importance of local biomechanical properties in disease pathogenesis, particularly as it relates to the enthesis, has been emphasized. The model of the synovio-entheseal complex delineates an innate immune response triggered by biomechanical and inflammatory events at the enthesis, which subsequently involve adjacent synovium and cartilage.
Mortality rates for PsA were higher than age-matched controls but recent evidence indicates that mortality may not be higher than observed in the general population. PsA patients do have higher rates of mortality from cardiovascular disease than controls.
Pharmacologic considerations
Psoriatic Arthritis Presentation Classification And Diagnosis
Prevalence of PsA is not known, but it is estimated to be from 0.3% to 1% of the U.S. population. In the psoriasis population, PsA is reported to range from 7% to 42%, although more recently, these numbers have been found to be in the 15% to 25% range . This type of inflammatory arthritis can develop at any age but usually is seen between the ages of 30 and 50 years, with men being affected equally or a little more than are women. Clinical symptoms usually include pain and stiffness of affected joints, > 30 minutes of morning stiffness, and fatigue.
The presentation of joint involvement can vary widely. Five subtypes of arthritis were identified by Moll and Wright in 1973, which included arthritis with predominant distal interphalangeal involvement, arthritis mutilans, symmetric polyarthritis , asymmetric oligoarthritis , and predominant spondylitis . Patients with PsA may also have evidence of spondylitis or sacroiliitis with back pain > 3 months, hip or buttock pain, nighttime pain, or pain that improves with activity but worsens with rest. The cervical spine is more frequently involved than is the lumbar spine in patients with PsA.
Radiograph of the Right Hand and Right Foot
Read Also: Best Bath Soak For Psoriasis
Symptoms Of Psoriatic Arthritis
The severity of the condition can vary considerably from person to person. Some people may have severe problems affecting many joints, whereas others may only notice mild symptoms in 1 or 2 joints.
There may be times when your symptoms improve and periods when they get worse .
Relapses can be very difficult to predict, but can often be managed with medicine when they do occur.
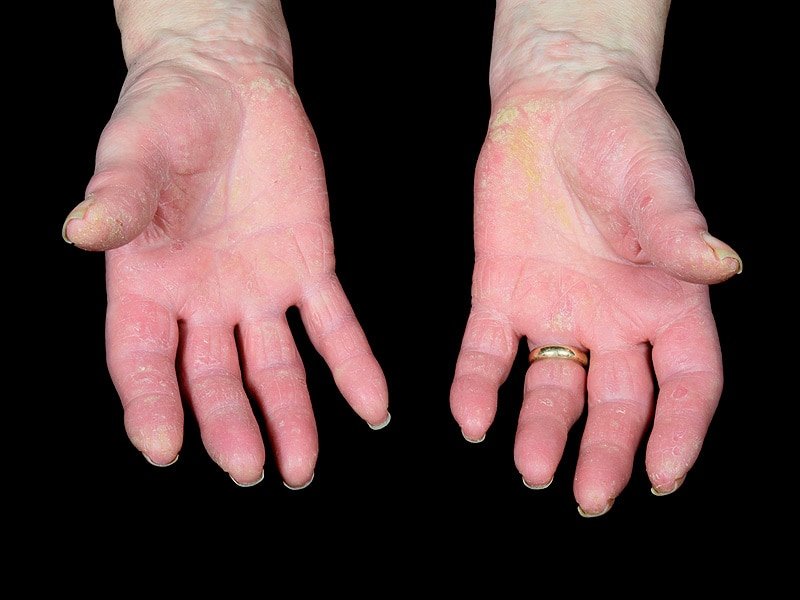
Fingers Toes And Skin
Another telling clue is the presentation of the disease on the fingers and toes. With PsA, the distal joints will be the focus of pain, swelling, and stiffness. By contrast, RA primarily involves the proximal joints .
With severe PsA, the fingers can also take on a sausage-like appearance , making it difficult to ball your fist. While this can occur with RA, it is not the hallmark that it is with PsA.
Around 85% of people of PsA with also have the most typical form of psoriasis, characterized by dry, flaky skin plaques. Moreover, half will have nail psoriasis at the time of their diagnosis. Neither of these occurs with RA.
Read Also: Beginning Stages Of Scalp Psoriasis
Does This Patient Have Psoriatic Arthritis
Psoriatic arthritis is an inflammatory arthritis that is characterized by a diversity of clinical manifestations and a highly variable disease course. This disorder was not recognized as a discrete entity until 1964, and it was Moll & Wrights landmark paper in 1973 that outlined the cardinal clinical features followed by familial studies a year later that documented the contribution of genetic factors in disease etiology.
Innovative translational studies and clinical trials over the last fifteen years have uncovered new disease mechanisms and fostered the development and validation of novel therapies, which have been incredibly effective for the varied clinical features of this disease. Recent attention has focused on the extra-articular manifestations and comorbid conditions associated with PsA because they may lessen function and quality of life and increase mortality.
Diagnosis
In the assessment of a patient for possible PsA, it is important to focus on the history and physical examination of the five key domains of this disease, which include integument manifestations of psoriasis, inflammatory peripheral arthritis, spondylitis, enthesitis, and dactylitis.
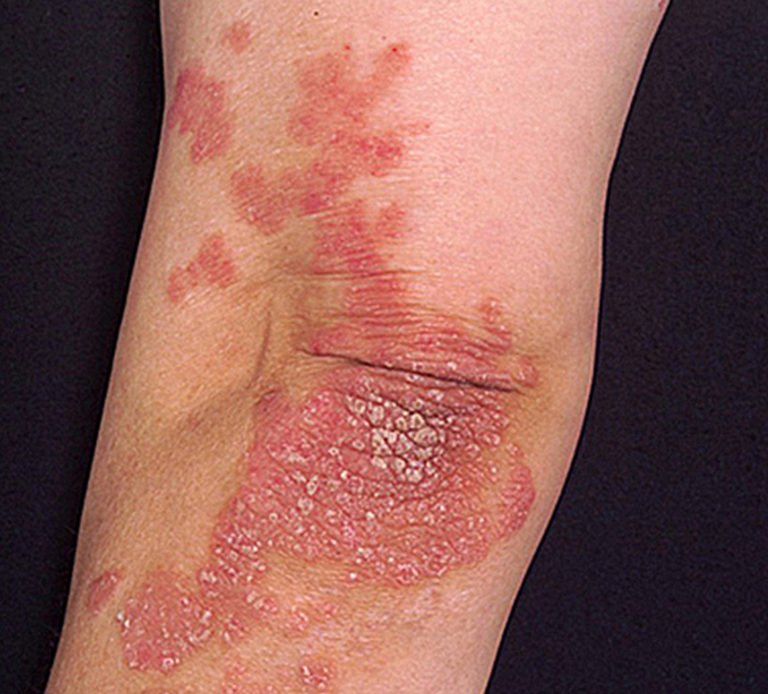
Psoriasis
Peripheral arthritis
Spondylitis
Enthesitis
Dactylitis
Some patients may not have psoriasis but will recall a family history of psoriasis or psoriatic arthritis, which is important to document. Other important elements in the history are symptoms of enthesitis .
Joint Pain Or Stiffness
Psoriatic arthritis causes inflammation in the joints, which can cause pain, tenderness, and stiffness. You might feel this in just one joint or in several.
Psoriatic arthritis usually affects the knees, fingers, toes, ankles, and lower back. Symptoms of pain and stiffness may disappear at times, and then return and worsen at other times. When symptoms subside for a time, its known as a remission. When they worsen, its called a flare-up.
Don’t Miss: Average Age Of Psoriasis Diagnosis
Is It Rheumatoid Arthritis Or Psoriatic Arthritis
Dr. Natalie Azar
I recommend to all my psoriasis patients that if they experience regular joint aches and pains that they talk to their health-care professional, because RA and PsA are both very real potential autoimmune diseases that may occur in addition to their already diagnosed psoriasis. Tests to confirm the diagnosis are available from your doctor, and determining the diagnosis can be most challenging for your health-care professional but it is very important to make the definitive diagnosis. Dr. Natalie E. Azar, assistant Clinical Professor of Medicine and Rheumatology at the NYU Langone Medical Center in New York City explains that the potential for organ involvement is significantly greater for those who have RA as opposed to those who have PsA. Patients who have RA are at a much greater risk of developing osteoporosis, heart and lung conditions, eye diseases and anemia which are all more frequently encountered in rheumatoid arthritis.
Almost one in three who have psoriasis have the potential to develop PsA, and there is no highly specific test that can be performed to determine if a patient has it, so it is essentially through a process of elimination. Some experts say that swollen fingers and toes are more likely to mean a higher incidence of the condition being PsA, but others disagree. The presence of nail and skin changes along with arthritis-like pain are more suggestive of PsA.
Psoriatic Arthritis Is A Lot Like Rheumatoid Arthritis But With A Nasty Skin Rash This Probably Sounds Terrible But I Was Secretly Happy When I Heard Phil Mickelson The Golfer Was Diagnosed With Psoriatic Arthritis Not That I Would Wish
Psoriatic arthritis is a lot like rheumatoid arthritis but with a nasty skin rash.
This probably sounds terrible but I was secretly happy when I heard Phil Mickelson the golfer was diagnosed with psoriatic arthritis. Not that I would wish the diagnosis on anyone! But I thought, wow, maybe it will increase awareness and maybe, just maybe, more studies and treatment options will become available.
I had worked for a rheumatologist/internal medicine doctor back in the early years of my nursing career. We had patients with rheumatoid arthritis, osteoarthritis, lupus, Sjogrens, a few cases of temporal arteritisI even saw my first HIV positive patient working in that clinic in the mid 80s. But I never once heard of psoriatic arthritis. I dont even remember hearing about it in nursing schooland I still hadnt heard of psoriatic arthritis when I was diagnosed in my late 40s. I was baffled by my diagnosis partly because I had no idea what it was but also it never even occurred to me since the psoriasis I had on my scalp had been diagnosed as just a bad case of dandruff and my sausage toes had been diagnosed as Mortons Neuroma.
Recommended Reading: Dawn Dish Soap For Scalp Psoriasis
Treatment For Psoriatic Arthritis Differs From Other Forms Of Arthritis
The main goals of all arthritis treatment are to reduce symptoms and improve quality of life. Methods vary depending on the type of arthritis.
Rheumatoid arthritis can be very destructive if its not treated, which is why we treat it aggressively with biologics, says Ruderman. But psoriatic arthritis doesnt manifest that way. Fewer than half of people with psoriatic arthritis develop a particularly aggressive form, which makes treatment challenging because we dont want to over-treat it.
Even so, the pain and discomfort associated with psoriatic arthritis can be significant. A study published in 2015 in the journal PLoS One found that the overall pain, joint pain, and fatigue reported by psoriatic arthritis patients was significantly greater than that reported by people with rheumatoid arthritis.
Unless someone has an existing condition, such as elevated blood pressure or kidney disease, nonsteroidal anti-inflammatory drugs are recommended for joint symptoms in milder forms of psoriatic arthritis, says Husni.
Topical creams, ointments, and lotions are often used to address the scaly, itchy skin rashes that occur with psoriasis.
If there are signs of joint damage, doctors treat psoriatic arthritis more aggressively with medications like the ones used to treat rheumatoid arthritis, says Ruderman. These include disease-modifying anti-rheumatic drugs and biologics.
Additional reporting by Becky Upham.
Cannabinoids And Rheumatoid Arthritis
RA is one of the most prevalent autoimmune diseases and one of the main causes of disability globally, causing pain, joint malformation and joint destruction.10 Preliminary evidence suggests that cannabinoids have a role in the future treatment of RA.
In one study,11 protein and mRNA expression of endocannabinoids, AEA and 2-AG, and cannabinoid receptors, CB1 and CB2, were found in synovial tissue obtained from 13 patients diagnosed with RA and undergoing arthroplasty whilst synovial tissue obtained from healthy volunteers was negative for the same endocannabinoids. Another study of synovial tissue from patients with RA12 found that of inflammatory cytokines, IL-6 and IL-8, which are stimulated by synovial cells, were attenuated by low concentrations of the synthetic cannabinoid WIN 55,212-2.
Furthermore, three different research groups achieved improvement in mice with collagen-induced arthritis , following treatment with various cannabinoids 13 The use of cannabinoids for the treatment of pain associated with RA has been assessed in only one 2006 clinical trial, where 58 patients with RA were allocated either nabiximols or a placebo.14 Compared with placebo, patients treated with nabiximols exhibited decreased pain along with improved sleep quality.15
Recommended Reading: Types Of Biologics For Psoriasis
Following The First Two Articles That Discussed The Treatment Of Cancer And Pain This Third Piece Will Focus On The Use Of Cannabinoids To Treat Psoriasis And Rheumatoid Arthritis
Endocannabinoids, as well as several phytocannabinoids, have been shown to influence immune functions, regulating inflammation, autoimmunity, antitumourigenesis, antipathogenic responses and other processes.1 Numerous in vitro and in vivo studies have examined the therapeutic potential of cannabinoid signalling in inflammation-associated diseases and attempted to dissect the complex immunological effects of cannabinoids.
Pattern Of Joint Involvement
With PsA, the pattern of joint involvement is often asymmetricalthe joints affected on one side of the body will not necessarily be affected on the other. Only 15% of people with PsA will have symmetrical arthritis, a condition considered more advanced and severe than asymmetrical arthritis.
In contrast, the pattern with RA is characteristically symmetricalthe same joints on both sides of the body are affected.
Recommended Reading: How To Loosen Psoriasis Scales On Scalp
Symptoms Of Ra And Psa
Both RA and PsA cause joint swelling, stiffness, and pain. Although both conditions affect joints in the fingers and toes, they do it in slightly different ways. And each one can cause other symptoms, too.
Rheumatoid arthritis:
- Often starts in the smaller joints, like the ones in your fingers and toes over time, it may affect other joints, too, like your wrists, knees, hips, and ankles.
- Usually shows up on the same joints on both sides of your body that means it’s symmetric.
- Often makes joints feel stiffer in the morning
- Can lead to fatigue, low-grade fever, and weight loss
Psoriatic arthritis:
- Can affect joints in the back and pelvis in addition to the ones in fingers and toes
- Often affects only one side of your body that means it’s asymmetric.
- Sometimes causes foot pain, especially on the sole of your foot or the back of your heel
- May make your fingers swell up like sausages
- May make your nails pit and flake
- Tends to affect entheses, areas where tendons or ligaments attach to bones
With both conditions, you’ll probably have times when your symptoms get worse. These are called flares. In between these flares are times without symptoms called remissions.
When To Get Medical Advice
See a GP if you have persistent pain, swelling or stiffness in your joints even if you have not been diagnosed with psoriasis.
If you’ve been diagnosed with psoriasis, you should have check-ups at least once a year to monitor your condition. Make sure you let the doctor know if you’re experiencing any problems with your joints.
You May Like: Small Psoriasis Spots On Legs
Rheumatoid Arthritis And Psoriatic Arthritis: The Similarities And Differences
All forms of arthritis involve tenderness and swelling of the joints. And, at first glance, psoriatic arthritis can be very hard to differentiate from other common types of arthritis, including rheumatoid arthritis and osteoarthritis.
Because psoriatic arthritis symptoms can overlap with those of rheumatoid arthritis and osteoarthritis not just swollen, achy joints but also stiffness and chronic fatigue diagnosing this autoimmune disease can be tricky.
Unlike rheumatoid arthritis, there is no blood test that can determine if a person has psoriatic arthritis, says M. Elaine Husni, MD, MPH, a rheumatologist at the Cleveland Clinic in Ohio.
Psoriatic arthritis can also affect the body in different ways depending on the person and how advanced the disease is, says Dr. Husni. As a result, a rheumatologist may need to examine a patient several times and run a number of tests before having enough information to make a definitive diagnosis.
One unique symptom of psoriatic arthritis that doctors look for is the presence of psoriasis, a condition that causes thick, discolored, scaly skin patches known as plaques, as well as pitted nails or nails that separate from the nail bed, according to the American Academy of Dermatology.
Like psoriatic arthritis, psoriasis stems from a faulty immune response, in which the immune system mistakenly attacks healthy cells and tissues.
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Don’t Miss: What Happens If You Pick Psoriasis