Psoriasis And Joint Pain
As a chronic autoimmune disorder, psoriasis can impact skin, joints and nails, and symptoms can vary from intermittent to chronic and from mild to debilitating. Symptoms develop as the immune system attacks the body, rather than protecting it from foreign intruders, which leads to inflammation. On the skin, this can manifest as sensitive, red patches and flaky skin.
Although both psoriasis and psoriatic arthritis can cause joint pain, stiffness and swelling, the signs of psoriatic arthritis often resemble those of rheumatoid arthritis. Common psoriatic arthritis symptoms include:
- Swollen fingers and toes which is often a precursor to significant joint symptoms
- Foot pain, particularly at the back of your heel or in the sole of your foot
- Lower back pain called spondylitis which causes inflammation of the joints between your spinal vertebrae and in the joints between your pelvis and spine.
There are several different types of psoriatic arthritis that are identified based on how symptoms are affecting your body. For example, symmetric psoriatic arthritis affects both sides of the body whereas asymmetric psoriatic arthritis only affects one side of the body. There are other types of psoriatic arthritis that are diagnosed based on the location of your inflammation.
What Are Eczema And Psoriasis
Many people around the world have aggravating and uncomfortable skin conditions. Two of the most common of these rashes are eczema and psoriasis.
It’s essential to understand the symptoms and causes of each of the conditions so that you can talk to your doctor about them when they are diagnosing them.
Both of these skin conditions can look the same. Eczema and psoriasis are different in that they can mean other things about your body or your environment.
One is triggered by allergies and skin reactions. The other triggers because your body is reacting abnormally.
What is eczema?
Roughly 30% of all people are affected by eczema. Eczema is a skin condition that affects mostly adolescents and children.
It can affect adults as well. It is often triggered by an allergic reaction to something you came into contact with. The skin reacts by turning red, swelling, and itching.
What is psoriasis?
Around 7 million people have psoriasis. Psoriasis appears on your skin in the same way that eczema does. The difference between psoriasis and eczema is that psoriasis is triggered by things that are not allergies.
Psoriasis starts beneath the skin. It then grows into patches of thick and red itchy skin that shed scaly dead skin cells.
The Link Between Psoriasis And The Immune System
No one ever really considered that the immune system had any real role in psoriasis, or its painful outbreaks. Not until a new drug Cyclosporine was offered to arthritis patients. What happened next was both surprising and unexpected. Patients who were prescribed the immune suppressing drug for their arthritis symptoms , began to report a decrease in their skin attacks. Without warning, researchers were faced with the theory that the immune system could be causing psoriasis.
It didnt take long before researchers began to figure out the mystery of psoriasis in regards to how the immune system can impact it.
The Role of the Immune System on the Skin
The immune system is responsible for standing guard and attacking any invaders which penetrate the body. Since the skins main job is to act as the bodys first defense mechanism against invasion, it is no wonder that the immune system works in close connection with each layer of the skin. Heres how it all works:
1. Immune cells patrol the entire body for dangers. Whats the Difference Between Psoriasis and Plaque Psoriasis
2. When an invader is detected, these immune send out chemical and nervous system messages to the immune system to ready itself for an attack
Read Also: Wild Naturals Eczema Psoriasis Shampoo
What Is The Difference Between Guttate Psoriasis And Plaque Psoriasis
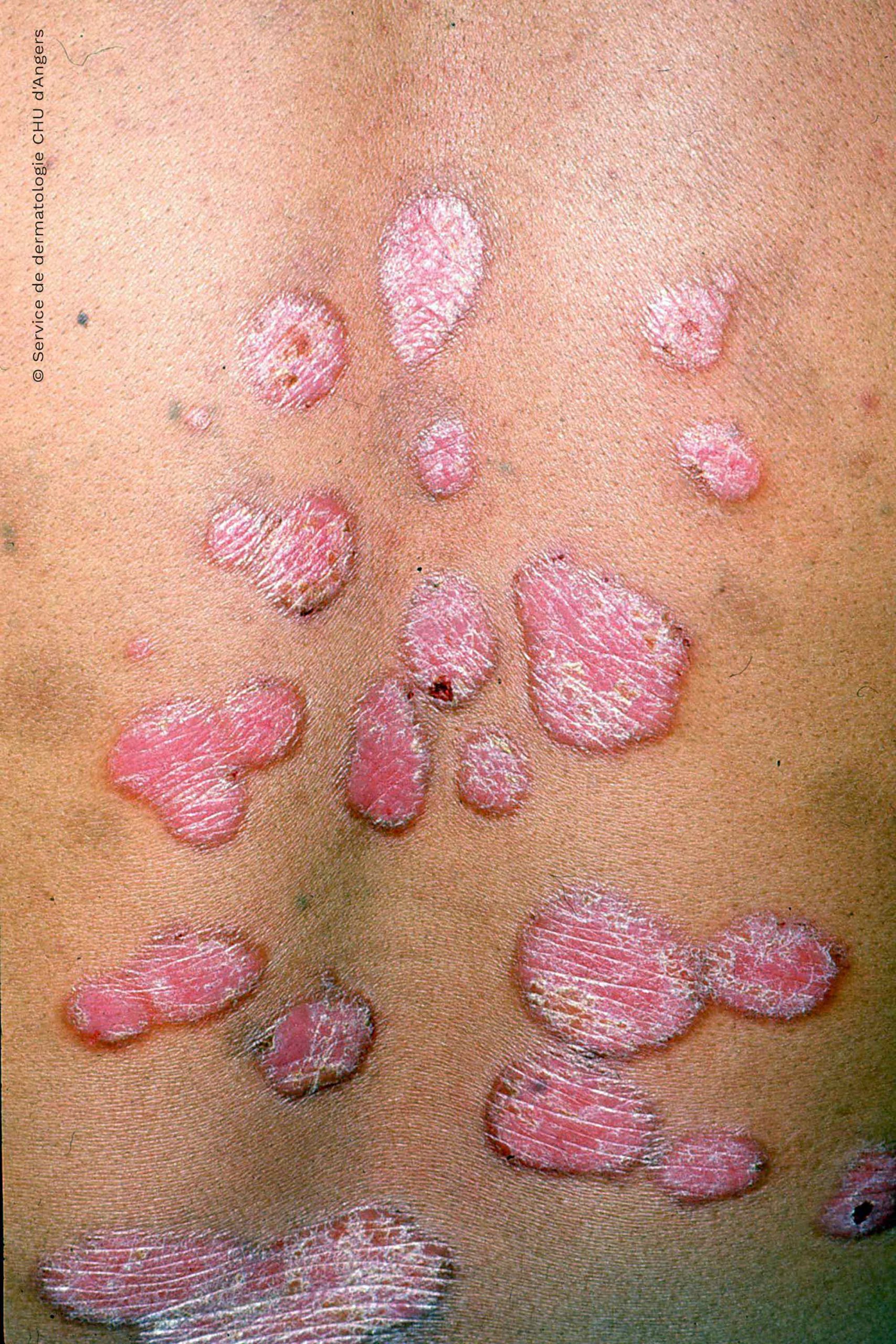
Guttate psoriasis and plaque psoriasis look different. Guttate psoriasis looks like small, discolored, drop-shaped scaly spots and usually appears in children and young adults. It typically appears after a sore throat caused by a streptococcal infection. It often goes away after several weeks, even if you dont seek treatment.
> > > Best Psoriasis Cure Available
3. To help safeguard the skin, the immune system release chemicals that can cause nerves to itch and blood vessels to dilate to prepare the skin for a sudden rush of immune cells
4. When the immune cells arrive at the scene, most work to kill off the pathogens causing the distress, but a few capture some of the invaders and take them back to the heart of the immune system, where other soldier cells are produced in a way to recognize and attack the invading cells on contact
5. Inflammation is the bodys way of opening blood vessels to allow more soldier cells to rush to the battlefield.
While this entire process is completely normal, people with psoriasis tend to overproduce these soldier cells when the body feels threatened. This overabundance of killer immune cells can actually be dangerous to the skin since they begin to attack good cells along with the bad ones.
While it is great to finally understand the impact an improperly working immune system can have on your skin and cause psoriasis more research is needed to pinpoint the exact cause for the over-firing of the cell messages. Whats the Difference Between Psoriasis and Plaque Psoriasis
You May Like: Can Dandruff Shampoo Help Psoriasis
What Can Prevent Someone From Getting A Second Type Of Psoriasis
Most types of psoriasis cannot be prevented.
That said, if you already have plaque psoriasis, it may be possible to reduce your risk of developing another type of psoriasis on your skin. Dermatologists recommend taking the following precautions:
-
Protect your skin to prevent sunburn
-
Take medication as directed and speak with your dermatologist before stopping a medication
-
Treat your psoriasis so that its well-controlled
-
Watch your weight so that you stay at a weight thats recommended for your age and height
Watching your weight may help prevent inverse psoriasis. This type of psoriasis is more common in people who are 20 or more pounds overweight.
Assessment Of Tissue Levels Of Cytokines In Relation To Psoriasis Phenotype
The tissue mRNA level of IFN- was significantly higher in the acute guttate psoriasis than chronic plaque psoriasis groups. The tissue protein levels of IL-12 and IL-17A were significantly higher in the chronic plaque psoriasis than acute guttate psoriasis groups .
Comparisons of tissue cytokine levels among chronic plaque psoriasis patients, acute guttate psoriasis patients, and healthy controls. IL: interleukin, IFN: interferon, RT-PCR: real-time reverse-transcription polymerase chain reaction. *p< 0.05, **p< 0.01.
Read Also: Can Psoriasis Make You Feel Unwell
Main Symptoms Of Psoriasis
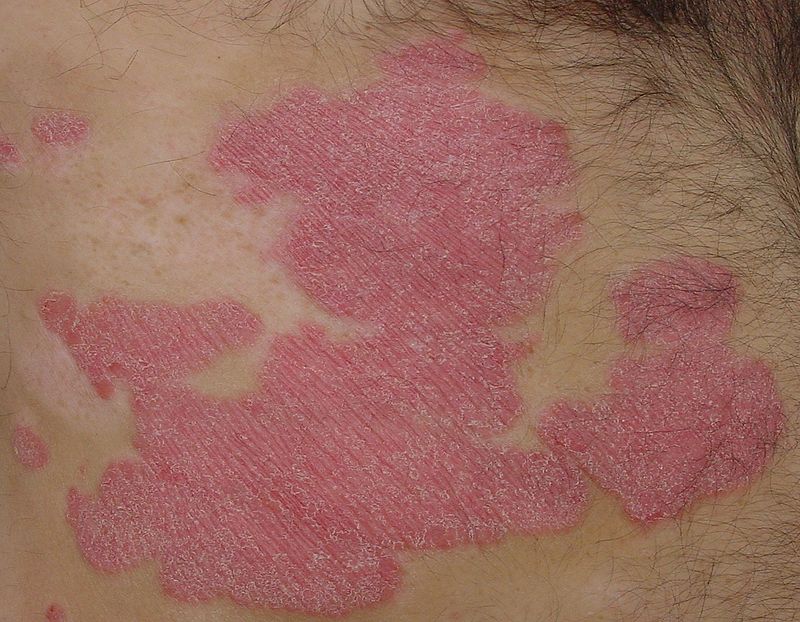
Psoriasis typically causes patches of skin that are dry, red and covered in silver scales. Some people find their psoriasis causes itching or soreness.
There are several different types of psoriasis. Many people have only 1 form at a time, although 2 different types can occur together. One form may change into another or become more severe.
Most cases of psoriasis go through cycles, causing problems for a few weeks or months before easing or stopping.
You should see a GP if you think you may have psoriasis.
Articles On Types Of Psoriasis
Knowing which kind of psoriasis you have helps you and your doctor make a treatment plan. Most people have only one type at a time. Sometimes, after your symptoms go away, a new form of psoriasis will crop up in response to a trigger.
In general, most types of psoriasis result from the same triggers:
- Diet
- Weather
Here’s how you can spot the 7 types of psoriasis and what you can do to treat them.
Also Check: Early Stages Of Psoriasis On Scalp
Are People With Psoriatic Arthritis At Greater Risk For Covid
This is an ongoing area of research.
The National Psoriasis Foundations guidance says that it is not known with certainty if having psoriatic disease meaningfully alters the risks of contracting SARS-CoV-2 or having a worse course of COVID-19 illness. It notes that existing data, with some exceptions, generally suggest that patients with psoriasis and/or psoriatic arthritis have similar rates of SARS-CoV-2 infection and COVID-19 outcomes as the general population.
The ACRs guidance says that autoimmune and inflammatory rheumatic disease patients are at higher risk for being hospitalized due to COVID-19 and having worse outcomes compared to the general population.
However, this is likely affected by factors such as age, other comorbidities such as heart disease or obesity, which is common in PsA, and taking steroid medications, rather than simply having psoriatic arthritis alone.
Some data suggests that patients with inflammatory rheumatologic diseases who get COVID-19 may have higher risk of developing serious complications, depending on their disease activity and other medical conditions such as high blood pressure, diabetes, and chronic kidney and lung disease, adds Dr. Zhu.
For more information, check out this summary of research on inflammatory arthritis and rheumatic disease patients and their risk for COVID-19 complications.
Also Check: Can Psoriasis Spread To Face
What Causes Psoriasis And Psoriatic Arthritis
The symptoms of both psoriasis and psoriatic arthritis arise when the bodys immune system malfunctions, leading to inflammation.
In psoriasis, the faulty reaction causes skin cells to grow too fast, promoting a buildup of skin cells on the surface. These cells appear as a scaly rash.
In psoriatic arthritis, the inflammation affects the joints. Permanent damage can result if the person does not seek treatment.
Doctors do not yet know the exact causes of psoriasis and psoriatic arthritis. However, they do know that genetics contribute to both conditions.
An estimated 1 out of 3 people with psoriasis say that they have a family member with psoriasis. Also, around 40 percent of people with psoriatic arthritis have a family member with psoriatic disease.
Still, many people have genes for psoriatic disease and never develop it. To develop psoriatic disease, a person must have the specific genes for it, as well as a trigger that activates it.
Possible triggers for psoriatic disease include:
- an infection, such as strep throat or a cold
- use of tobacco or smoking
- heavy alcohol use
These triggers may bring on psoriasis, and they can also cause flares. Flares are cycles during which symptoms become worse. Triggers vary from person to person and may change over time.
Psoriasis and psoriatic arthritis symptoms often come and go in cycles. They may get worse during a flare and then improve. Symptoms may also move around, affecting different areas of the body at different times.
Don’t Miss: How Long Can You Live With Psoriasis
What Medications Or Treatments Are Used To Treat Plaque Psoriasis
Your healthcare provider may prescribe the following as a cream, lotion or gel to treat mild cases of plaque psoriasis:
Salicylic acid shampoo treats plaques in your scalp.
In more severe or widespread cases of plaque psoriasis, your healthcare provider may prescribe:
- Medicine injections. Your healthcare provider will use a thin needle to inject medicine into your skin or a vein in your arm. These medicines may include adalimumab, etanercept or ustekinumab.
- Oral medicines. Oral medicines are pills or tablets that you swallow with water. These medicines may include acitretin, cyclosporine or methotrexate.
- . Phototherapy uses ultraviolet light, usually ultraviolet B , from special lamps. The ultraviolet light waves in sunlight can help certain skin disorders, including plaque psoriasis.
Though Psoriasis And Eczema Are Different Conditions Treatment For The Two Is Often Similar
While theres no cure for either condition, they can be treated. If youre diagnosed with psoriasis or eczema, your doctor may recommend:
- Over-the-counter moisturizers
- Topical medications to reduce inflammation, like corticosteroids, calcineurin inhibitors, and retinoids
- Oral steroids, like prednisone, which can help calm a severe case when used for a short period of time
- Wet dressings, which involve wrapping the area with a wet bandage to soothe the itchiness
Although psoriasis and eczema are both frustrating, irritating conditions, they shouldnt be life-ruiners. If youre struggling with managing your psoriasis or eczema, see a dermatologist, who can help determine the best treatment plan for you.
Related:
Don’t Miss: Mg217 Psoriasis Coal Tar Gel
Summary Plaque Psoriasis Vs Psoriasis
Psoriasis is a chronic multisystem disease with skin and joint manifestations. Plaque psoriasis is the commonest form of psoriasis which is characterized by the appearance of reddish well-demarcated plaques with silver scales usually on the extensor surface of the knees and elbows. Accordingly plaque psoriasis is one manifestation of the broad spectrum of dermatological and systemic manifestations which are identified as psoriasis. This can be identified as the difference between plaque psoriasis and psoriasis.
What Are Symptoms Of These Conditions
Visually, it can sometimes be difficult to tell one condition from the other. You need to look at various aspects of the rash to distinguish themboth manifest as dry, itchy scales, red patches, and plaques. At times, psoriasis causes thicker plaque, and eczema could produce a serous exudate or leaking fluid. In most cases, though, medical professionals have to perform biopsies to be sure.
Also Check: Best Drugstore Cream For Psoriasis
What Else Should I Ask My Healthcare Provider
If you have psoriasis, ask your healthcare provider:
- How can I prevent outbreaks and control symptoms?
- What medication will work best for me?
- What else should I do to improve symptoms?
- What are my options if creams dont work?
- Will psoriasis ever go away?
A note from Cleveland Clinic
Psoriasis, an itchy skin condition, can come and go throughout your life. Its related to an overactive immune response and is not contagious. If you have skin changes that arent going away, talk to your healthcare provider. There is no cure for psoriasis, but psoriasis treatments can improve symptoms. Your provider may prescribe a special cream or moisturizer or medications. Other therapies are available if creams or medicines dont work. Maintaining your overall health will also help improve symptoms.
Last reviewed by a Cleveland Clinic medical professional on 10/17/2020.
References
Ready To See If Cosentyx Can Help You Feel Real Relief From Your Symptoms
Find a dermatologist in your area who has experience prescribing biologics as well as other treatments for moderate to severe plaque psoriasis.
COSENTYX® is a prescription medicine used to treat:
-
people 6 years of age and older with moderate to severe plaque psoriasis that involves large areas or many areas of the body, and who may benefit from taking injections or pills or phototherapy
-
people 4 years of age and older with active enthesitis-related arthritis
-
people 2 years of age and older with active psoriatic arthritis
-
adults with active ankylosing spondylitis
-
adults with active non-radiographic axial spondyloarthritis and objective signs of inflammation
Do not use COSENTYX if you have had a severe allergic reaction to secukinumab or any of the other ingredients in COSENTYX. See the Medication Guide for a complete list of ingredients.
COSENTYX is a medicine that affects your immune system. COSENTYX may increase your risk of having serious side effects such as:
Infections
COSENTYX may lower the ability of your immune system to fight infections and may increase your risk of infections, sometimes serious.
Before starting COSENTYX, tell your doctor if you:
After starting COSENTYX, call your doctor right away if you have any signs of infection listed above. Do not use COSENTYX if you have any signs of infection unless you are instructed to by your doctor.
Inflammatory bowel disease
Serious allergic reactions
Before starting COSENTYX, tell your doctor if you:
You May Like: Can Psoriasis Cause Itching Without Rash
The Differences In Appearances
Eczema makes your skin red and inflamed. It may be scaly, oozing, or crusty. You may see rough, leathery patches that are sometimes dark. It can also cause swelling.
Psoriasis can also cause red patches. They may be silvery and scaly — and raised. But if you look closely, the skin is thicker and more inflamed than with eczema.
How To Differentiate Eczema And Psoriasis
Psoriasis is a chronic condition of the immune system. It causes red, scaly patches on the scalp or the skin of the elbows and knees, though it can occur anywhere on the skin. Meanwhile, eczema or atopic dermatitis is an inflammationcommon triggers include dry skin or chemicals. Neither of these is contagious, though people with either condition can pass it down to their children.
Recommended Reading: Difference Between Ichthyosis And Psoriasis
Traditional Treatment Cautions Whats The Difference Between Psoriasis And Plaque Psoriasis
You make an appointment to see your doctor because your psoriasis is flaring. He takes a look and then whips out his prescription pad to order one of the following:
. A prescription strength topical treatment
. phototherapy
. oral and injection therapy
. over the counter drugs
Any of these treatments may work fine to relieve your symptoms and make you feel better for now. The trouble with conventional treatment methods is that they rarely work to cure the underlying cause of this skin condition and that can leave you suffering repeat attacks. Still it is important to know what helps are available, and how they may help or hurt your chance of treatment success.
Topical Ointments Whats the Difference Between Psoriasis and Plaque Psoriasis
Topical ointments are used at the first sign of psoriasis. If caught early enough they can sometimes stave off a full-blown attack. Unfortunately, most people report becoming immune to them when used often, which makes them useless for long term use. Still, using the occasional cream or gel can help relieve some of your symptoms. Steroids
Both topical and internal steroids can be prescribed to help ease psoriasis swelling inflammation and itching. Immunomodulators
An immune suppressing drug that was originally used to help transplant patients beat organ rejection, Cyclosporine helps to inhibit T lymphocyte production so that scaly plaque is unable to grow on the surface of the skin.
. stretch marks
. loss of effect over time