Psoriasis: More Than Skin Deep
The first accurate medical discussion of psoriasis dates back to 1801, but the disease itself is much older. In fact, its very name is borrowed from an ancient Greek word meaning an itchy or scaly condition. About 7 million Americans are plagued by this itching and scaling, and many of them have serious complications involving other organs. Although psoriasis is classified as a dermatologic disease, it doesn’t start in the skin, and its damage may be more than skin deep.
How High Is My Risk Of Being Exposed To Covid
COVID-19 has made treating serious health conditions like psoriasis more challenging, but even so, you still need to communicate with your doctor and attend regular appointments.
Even in a pandemic, you can go to inpatient appointments because your doctor and their staff are doing everything to keep you safe when you come to their offices.
Precautions being taken include limiting the number of people coming in and out of their spaces, practicing masking, creating ways to physically distance, screening for COVID-19, disinfecting frequently touched surfaces, and sanitizing stations for staff and patients.
If you dont feel like coming into your doctors office or you are not feeling well, you have the option of telemedicine. That way, you can still meet with your doctor and get treatment using various videoconferencing technologies in real time, including Zoom and FaceTime.
Studies have found that people with psoriasis who received treatment via telemedicine had similar outcomes to people who saw their dermatologists in person.
The information in this article is current as of the date listed. As new research becomes available, well update this article. For the latest on COVID-19, visit our coronavirus news page.
Can Psoriatic Arthritis Attack Other Organs Of The Body
Apart from the skin, nails and joints, increased cardiovascular morbidity is considered part of psoriatic disease, as is the association with inflammatory bowel disease. An itchy, red eye due to conjunctivitis is more common in people with psoriatic arthritis and some people occasionally develop a painful, red eye caused by inflammation around the pupil of the eye, which is called iritis or uveitis. Anaemia may also be found but this is the result of long-term inflammation and is not a specific feature of psoriatic arthritis.
Recommended Reading: How To Stop A Psoriasis Flare Up
Healthy Eating And Exercise
People with psoriasis have a slightly higher risk of developing diabetes and cardiovascular disease than the general population, although it’s not known why. Regular exercise and a healthy diet are recommended for everyone, not just people with psoriasis, because they can help to prevent many health problems.
Eating a healthy, balanced diet and exercising regularly can also relieve stress, which may improve your psoriasis.
Biological Mechanisms Of Fatigue
A highly relevant model for fatigue may be sought in the so-called sickness behaviour, which represents an adaptive and complex response in humans and animals during the course of an infection.- Sick individuals demonstrate loss of appetite, initiative, grooming and interest in other individuals. They develop sleepiness and withdraw from normal social activities. Fatigue is a prominent and dominant feature of this response. Sickness behaviour seems to be deeply conserved throughout evolution and, as such, it is not a maladaptive response but a subconscious strategy for the survival of the individual and the species during viral and bacterial infections.
Activation of the innate immune system, which is found in all plant and animal life and which provides the immediate host immune response to infection and other immunological danger, may be a key regulator of fatigue in both acute and chronic conditions. A number of studies show that sickness behaviour is associated with proinflammatory cytokines such as IL-1, IL-6 and tumour necrosis factor -., Among these cytokines, IL-1 seems to have a pivotal role. IL-1 possesses an early and strong proinflammatory effect and is secreted mainly by activated monocytes, macrophages and dendritic cells.- IL-1 also reaches neuronal cells in the brain where it binds to specific IL-1 receptors not causing inflammation, but instead triggering the behavioural response.,
Read Also: Tea Tree Oil And Psoriasis
Day : Can Oil Pulling Really Make You Feel Better
A while back, I was reading a magazine and saw an article about Oil Pulling. I don’t remember all of the details, but I do remember the gist: Amazingly sick woman, hardly able to walk, starts swishing her mouth daily with coconut oil and gets cured in two weeks.
“HMMMM,”I thought, very skeptical of the whole thing. Still, you never know, so I filed the info away for future reference. Fast forward another two months. I’m feeling lousy and VERY, VERY tired of being sick. After making a horrible video talking about how hard it seems right now, I go back on line to do some research. Again, hidden deep in a Lyme’s message board, more people discuss how oil pulling has helped. Then, a third website , brings up the same thing.
“OK,” I think. Bowing to some unwritten code about hearing things in threes. “I’ll look into to it.”
Toted as an Indian folk remedy , Oil Pulling involves swishing oil in the mouth for 20 minutes to remove bacterial and draw out toxins. Practitioners swear by its ability to heal chronic and acute illnesses, including, but not limited to: yeast over growths, psoriasis, acne, gum disease, hormone imbalances, migraines, bronchitis, arthritis, insomnia, aids, and even cancer.
At worst, users excitedly talk about how the method makes their skin better and their teeth whiter. At best, the lame can now walk. The blind can see .How do you do it?
To start, you need a tablespoon of oil .
Will it work? Time will tell.
What Are The Symptoms Of Psoriasis
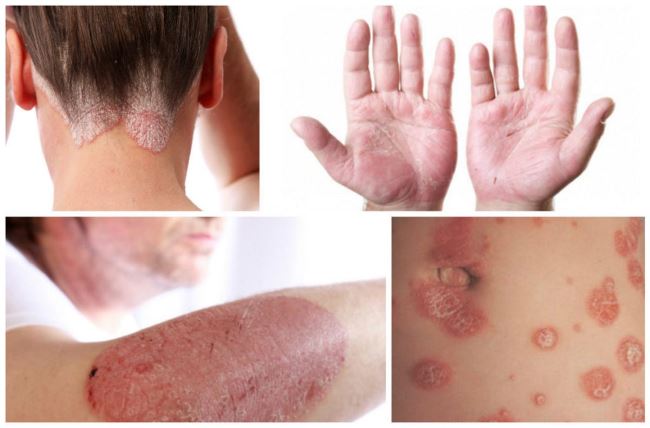
There are different types of psoriasis. The most common is chronic plaque psoriasis. This causes patches of red, raised skin, with white and silvery flakes.
It can occur anywhere on the skin, but most commonly at the elbows, knees, back, buttocks and scalp.
Psoriasis can cause small round dents in finger and toe nails, this is known as pitting. Nails can also change colour, become thicker and the nail may lift away from your finger.
You May Like: Cura Para La Psoriasis En El Cuero Cabelludo
Does Guttate Psoriasis Make You Feel Ill
- Usually the appearance of the spots is the worst thing about it.
- It doesn’t usually make you feel ill or feverish.
- The spots are not usually painful, but they can be a tiny bit itchy .
- You can imagine that coming up in spots all over your body in just a few days can be pretty distressing: a lot of people are quite upset when they see their doctor.
What Psoriatic Arthritis Fatigue Feels Like: What Patients Say
We asked several of our CreakyJoints Psoriatic Arthritis Patient Council members to help us paint a picture of what PsA fatigue feels like. Read on and see which descriptions resonate with you.
Fatigue is:
- Overwhelming the littlest tasks take the most effort. Ashley K.
- A really heavy feeling that I cant shake. Im awake, I cant focus, and I cant fall asleep. Jaime H.
- Like getting a blood draw, but instead of taking blood, the energy slowly gets pulled from my body. Diane T.
Fatigue makes me:
- Just sit in my chair for two hours. I cant summon the will to get up and move. Eddie A.
- Not have control of my day and my body. You wake up and you dont know if youre going to be functional, or do what you had planned for, and that in itself is a journey that Im still working through. Ashley
- Feel guilty, like I should have been there for this or that, I should have left earlier, or I should have done more. Eddie A.
- Feel like I have the flu. Im utterly tired and have to lie down or sleep. Frances D.
If fatigue were an animal, it would be:
To live without fatigue would mean:
Read Also: Psoriasis En La Cabeza Tratamiento
How Will Psoriatic Arthritis Affect Me
Starting the right treatment as soon as possible will give you the best chance of keeping your arthritis under control and minimise damage to your body.
Psoriatic arthritis can vary a great deal between different people. This makes it difficult to offer advice on what you should expect.
It will usually have some effect on your ability to get around and your quality of life, but treatment will reduce the effect it has.
Psoriatic arthritis can cause long-term damage to joints, bones and other tissues in the body, especially if it isnt treated.
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Read Also: List Of Biologics For Psoriasis
How Does Melanoma Make You Feel
Melanoma can cause pain in the bones where its spread, and some peoplethose with very little body fat covering their bonesmay be able to feel a lump or mass. Metastatic melanoma can also weaken the bones, making them fracture or break very easily. This is most common in the arms, legs, and spine.
What Happens After The First Outbreak

Usually it comes and goes and then that’s all there is to it. In about 80% of people the spots will fade in three weeks to three months and never come back. But in some people it carries on to be long-term plaque psoriasis. Sometimes you can get a second outbreak, particularly if the streptococcus germ is still in your throat or tonsils.
Recommended Reading: What Is The Difference Between Psoriasis And Psoriatic Arthritis
How To Stay Safe
Having psoriasis and a compromised immune system is a good reason to want to stay healthy.
To minimize your risk for COVID-19, take the following CDC precautions:
- Stay home as much as you can.
- Avoid crowds, and limit close contact with others when out in public.
- Avoid touching your face, nose, and mouth when out.
- Avoid touching frequently touched surfacessuch as doorknobs and shopping cartswhen out in public. Carry disinfecting wipes for when you need to touch surfaces.
- Wear a mask when in a crowded place.
- Talk to your doctor about whether the COVID vaccine is an option for you, and if it is, get vaccinated as soon as you can.
- Wash your hands with soap and water for at least 20 seconds or use hand sanitizer after coming inside or after touching commonly touched surfaces.
Psoriasis Treatments And Covid
People who are immunocompromised are believed to have a higher risk for COVID-19. While this usually applies to people with cancer on chemotherapy and those with poorly controlled HIV/AIDS, it can also apply to people who take medications that affect the function of their immune systems.
People with psoriasis will use different immunosuppressive drug therapies, including methotrexate, biologics, cyclosporine, and . Taking these medicines can partially inhibit your immune system, which adds to your infection risk.
The current guidelines of the American Academy of Dermatology recommend that people who take immunosuppressive drugs continue to take them unless they test positive or if they have symptoms of COVID-19.
Further, most recent research suggests people with psoriatic disease, including those on biologic drug therapy, are at no additional risk for contracting or being seriously harmed by COVID-19 from their psoriasis treatments.
According to the National Psoriasis Foundation COVID-19 Task Force, the overall existing data suggest that most treatments for psoriasis do not meaningfully alter the risks of contracting SARS-CoV-2 or having a worse course of COVID-19 illness.
The effects of immunosuppressive therapy on the immune system arent a reason to stop treatment. Your doctor is the best person to answer questions about your treatment plan. They can also best advise you on how the pandemic might affect your health situation and current treatment plan.
Also Check: What Oil Is Good For Scalp Psoriasis
Does Psoriasis Get Worse With Age
Aging doesnt make psoriasis worse. But as you get older, you may need to adjust your treatment plan. Your body may react differently to drugs youve taken over time. Or, it may no longer be safe for you to continue taking certain drugs.
According to the American Academy of Dermatology, some of the following factors can affect your treatment plan once you turn 65:
- It may be harder to reach areas of the body where you need to apply topical treatment.
- Skin may become thin, or it may bruise or tear more easily when you apply a topical corticosteroid.
- Light therapy may be challenging because of the time spent on your feet while standing in a light box.
- Skin may be sensitive to light due to medications youre taking for other health conditions, which makes light therapy more challenging.
- Some systemic drugs may be riskier to take because of differences in kidney function as you age.
Keep an open line of communication with your healthcare provider about your psoriasis treatment plan and whether it should be adjusted as you age.
What About Hair Loss
During autumn, many women experience hair loss. In fact, the hair is usually the first thing to suffer from a bodily upset. Yes, this is a type of seasonal hair loss and is only temporary. If the problem is severe, you may need to consult a hair loss specialist.
Massaging your scalp with lukewarm oil helps stimulate the hair follicles and improves blood circulation in the scalp.
Recommended Reading: Does Psoriasis Affect The Face
Four Main Types Of Psoriatic Arthritis
There are 78 major joints in the body and psoriatic arthritis can affect any one of these. Usually, however, certain joints are more likely to be affected . Different patterns are found. Sometimes just one or two joints are a problem but often several joints, both large and small and on both sides of the body, are involved. About a third of people with psoriatic arthritis also have spondylitis which can result in a painful, stiff back or neck. Psoriasis can affect the nails with pitting, discolouration and thickening and this may be associated with inflammation in the joints at the end of the finger or toe. Another way in which psoriatic arthritis can be recognized is the finding of a sausage-like swelling of a finger or toe, called dactylitis. This is caused by inflammation occurring simultaneously in joints and tendons, painful heels and other bony prominence can also occur and this is caused by inflammation where gristle attaches to bone.
How Is It Diagnosed What Should I Do Who Should I See
If you feel you may have psoriatic arthritis you should firstly talk to your GP and explain to him your concerns and why you feel you may have psoriatic arthritis.
You may be lucky in that your GP spots all the early warning clues to your aches and pains, and diagnoses you correctly for prompt treatment options. However, there are still many people who are diagnosed much later due to lack of knowledge. This is not a criticism, but merely that GPs have to have such a wide knowledge of many conditions and with psoriatic arthritis, it is not always as simple or obvious to diagnose.
A review of your medical history by your GP, symptoms, and blood tests to rule out certain other conditions are needed. Absence of rheumatoid factor in the blood often helps to distinguish psoriatic arthritis from rheumatoid arthritis.
Pitting of the finger nails, discolouration of the nail due to abnormalities in the growth of the tissue in the nail bed are always a certain clue of psoriatic arthritis presence. People with psoriatic arthritis almost always have nail involvement.
You May Like: Best Lotion For Psoriasis On Hands
Who Is Affected By Guttate Psoriasis
- Usually young people get guttate psoriasis, in their teens or twenties. Men and women are affected equally.
- It seems to occur all over the world.
- No one really quite knows how common it is. In general, a GP in the UK would have heard of it and probably know how to diagnose it, but they may not have seen a case themselves for many years.
Will Drug Treatments For Psoriatic Arthritis Make My Psoriasis Worse

Some drug treatments may make psoriasis worse, but then again, some can also make it better too. Before you start any treatments offered, discuss this both with your dermatologist and rheumatologist. DONT FORGET to politely request that both consultants let each other know of your treatment regimes, this helps both of them evaluate your treatment and any side effects that you may be likely to experience. Some people find that when their psoriasis is bad their arthritis is also bad and as one improves, so does the other. This most often occurs when the skin and joint disease start simultaneously. Some of the arthritis treatments also help the skin and this is can help the doctors decide which is the best drug to use.
Also Check: At What Age Can You Get Psoriasis