Psoriasis And Granulomatous Diseases
Non-infectious granulomatous conditions such as granuloma annulare and sarcoidosis are rarely associated with psoriasis . Th1 type cytokines are favored in the initial phase of sarcoidosis. In particular, TNF- is important in the formation of sarcoidal granuloma . A shared TNF–mediated pathogenesis between psoriasis and sarcoidosis may exist. TNF- activates Th17 cells to lead IL-17 production, and the IL-17 inflammatory pathway has been suggested to be important in psoriasis. Moreover, recent studies have suggested an important role of IL-17 in sarcoidosis, and enhanced expression of IL-17A+IFN-+ and IL-17A+IL-4+ memory T-cells was shown in sarcoidal lungs . Thus, Th17 profile has been implicated to play a role in sarcoidosis, possibly by inducing granuloma formation via suppression of regulatory T-cells . Another study showed upregulation of IL-23 and IL-21 in the lesions of cutaneous sarcoidosis . In addition, pso p27 is a protein detected in mast cells in psoriatic lesions and extractable from psoriatic scales. Pso p27 is abundantly expressed in psoriatic lesional skin, and also expression of pso p27 is increased in the lungs of pulmonary sarcoidosis . Further study is needed to determine the role of pso p27 in sarcoidosis.
Newly Reported Mental Comorbidity Of Psoriasis
An increased risk of Parkinson disease and migraine, especially migraine with aura was reported in patients with psoriasis while a higher risk of psoriasis was found in patients with schizophrenia, and Th17 and pro-inflammatory cytokines may act as a link between these two diseases . There is a relationship between psoriasis and alexithymia and dental fear , and impulse control proved to be the strongest predictor to psoriasis disability .
A meta-analysis showed significant, small-to-medium effects of psychosocial interventions on quality of life and anxiety , but a not significant effect on depression .
How Is Psoriasis Diagnosed And Treated
Psoriasis often has a typical appearance that a primary care doctor can recognize, but it can be confused with other skin diseases , so a dermatologist is often the best doctor to diagnose it. The treatment of psoriasis usually depends on how much skin is affected, how bad the disease is , or the location . Treatments range from creams and ointments applied to the affected areas to ultraviolet light therapy to drugs . Many people who have psoriasis also have serious health conditions such as diabetes, heart disease, and depression. Some people with psoriasis also have an inflammatory condition which affects their joints, called psoriatic arthritis.
Psoriatic arthritis has many of the same symptoms as other types of arthritis, so a rheumatologist is often the best doctor to diagnose it. The treatment of psoriatic arthritis usually involves the use of drugs .
Psoriatic disease may be treated with drugs or a combination of drugs and creams or ointments.
Don’t Miss: How Do I Get Rid Of Psoriasis In My Ears
What Are The Complications Of Psoriasis
People with severe psoriasis have an increased risk of developing diabetes, cardiovascular disease, arthritis, obesity, some types of cancer, inflammatory bowel disease and other immuneârelated disorders, and liver and kidney disease.
The condition can affect the nails and joints, and can seriously affect someone’s emotional and social wellbeing. It may affect their ability to work, go to school or participate in physical activities.
Plaque Psoriasis Is The Most Common Type Of Psoriasis
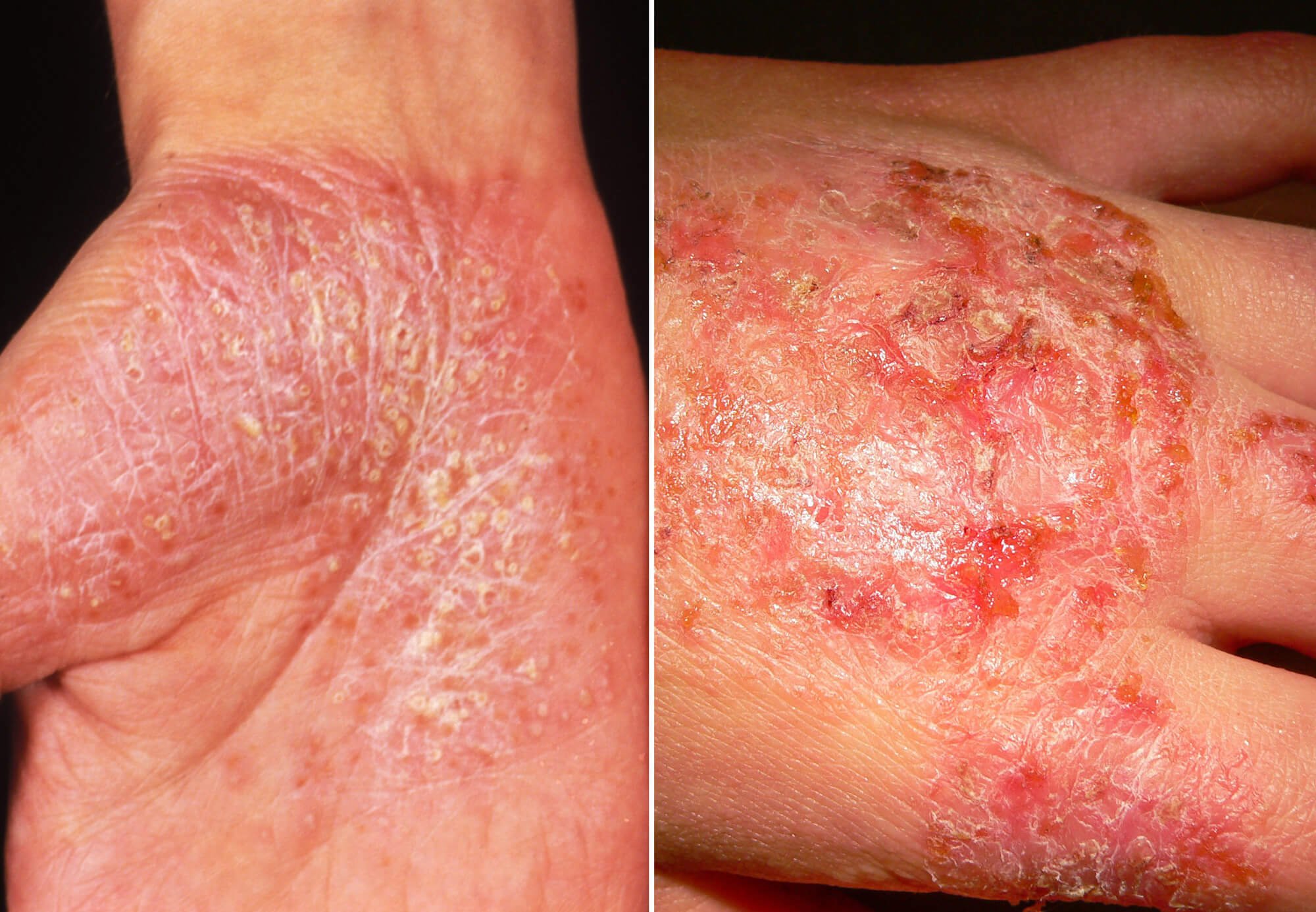
Those thick, scaly patches that develop on the skin are called plaques . About 80% to 90% of people living with psoriasis get plaques, so they have plaque psoriasis1.
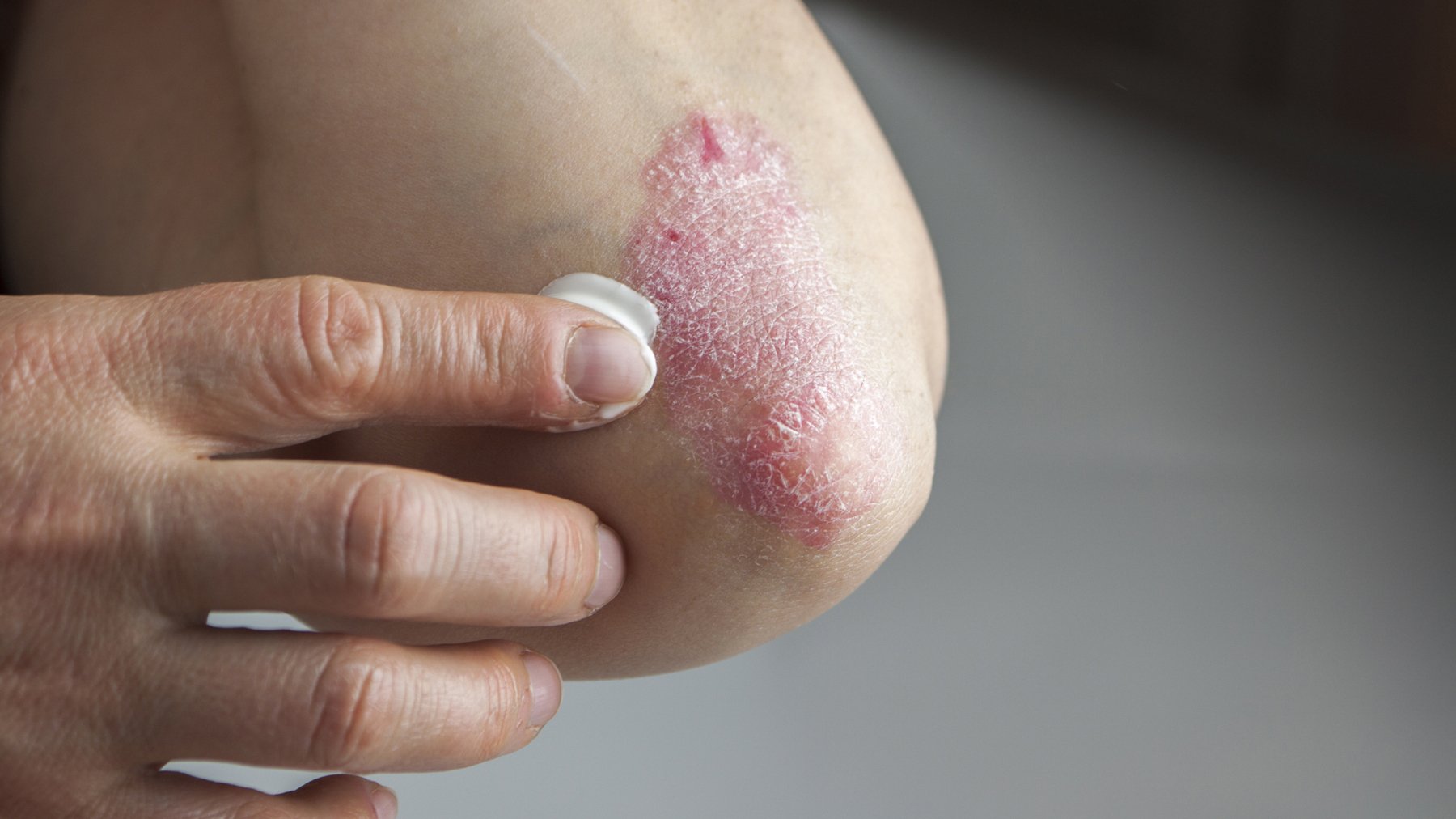
Plaque psoriasis on an elbow
When someone has plaque psoriasis, youll often see raised patches coated with a silvery-white scale.
Plaques can appear anywhere on the skin, but youre most likely to find them on the:
-
Knees
-
Lower back
-
Scalp
Plaques tend to vary in size. They may appear on the skin as a single patch or join together to cover a large area of skin.No matter the size, plaques tend to be itchy. Without treatment, the itch can become intense. Some people notice that their skin stings, burns, or feels painful and tight.
Read Also: Which Treatment Is Better For Psoriasis Homeopathy Or Allopathy
Articles On Types Of Psoriasis
Knowing which kind of psoriasis you have helps you and your doctor make a treatment plan. Most people have only one type at a time. Sometimes, after your symptoms go away, a new form of psoriasis will crop up in response to a trigger.
In general, most types of psoriasis result from the same triggers:
- Diet
- Weather
Here’s how you can spot the 7 types of psoriasis and what you can do to treat them.
What Are The Clinical Features Of Psoriasis
Psoriasis usually presents with symmetrically distributed, red, scaly plaques with well-defined edges. The scale is typically silvery white, except in skin folds where the plaques often appear shiny with a moist peeling surface. The most common sites are scalp, elbows, and knees, but any part of the skin can be involved. The plaques are usually very persistent without treatment.
Itch is mostly mild but may be severe in some patients, leading to scratching and lichenification characterised by thickened leathery skin and increased skin markings. Painful skin cracks or fissures may occur.
When psoriatic plaques clear up, they may leave brown or pale marks that can be expected to fade over several months.
Also Check: Best Cream For Psoriasis On Face
Is Psoriasis The Same As Eczema
Psoriasis and eczema are two different skin conditions. They differ in where the disease appears on the body, how much it itches and how it looks. Eczema tends to appear more often behind the knees and inside the elbows. Eczema also causes more intense itching than psoriasis. Many people, especially children, can get both eczema and psoriasis.
How Psoriasis Is Diagnosed
A GP can often diagnose psoriasis based on the appearance of your skin.
You may be referred to a specialist in diagnosing and treating skin conditions if your doctor is uncertain about your diagnosis, or if your condition is severe.
In rare cases, a small sample of skin called a biopsy will be sent to the laboratory for examination under a microscope.
If your doctor suspects you have psoriatic arthritis, which is sometimes a complication of psoriasis, you may be referred to a doctor who specialises in arthritis .
You may have blood tests to rule out other conditions, such as rheumatoid arthritis, and X-rays of the affected joints may be taken.
Don’t Miss: Rose Water For Scalp Psoriasis
Symptoms Causes Diagnosis And More
Psoriatic disease is an autoimmune disease that includes two specific inflammatory conditions. These two conditions, psoriasis and psoriatic arthritis , are a result of an overactive immune system. Psoriasis and PsA primarily affect the joints and skin throughout the body.
What If Those Psoriasis Treatments Dont Work
If psoriasis doesnt improve, your healthcare provider may recommend these treatments:
- Light therapy: UV light at specific wavelengths can decrease skin inflammation and help slow skin cell production.
- PUVA: This treatment combines a medication called psoralen with exposure to a special form of UV light.
- Methotrexate: Providers sometimes recommend this medication for severe cases. It may cause liver disease. If you take it, your provider will monitor you with blood tests. You may need periodic liver biopsies to check your liver health.
- Retinoids: These vitamin A-related drugs can cause side effects, including birth defects.
- Cyclosporine: This medicine can help severe psoriasis. But it may cause high blood pressure and kidney damage.
- Immune therapies: Newer immune therapy medications work by blocking the bodys immune system so it cant jumpstart an autoimmune disease such as psoriasis.
Recommended Reading: What Are The Symptoms Of Psoriasis
What Are The Symptoms Of Psoriasis
The following are the most common symptoms of psoriasis. Psoriasis comes in several forms and severities. Symptoms may include:
-
Plaque psoriasis. This type of psoriasis is the most common. Symptoms may include patches of red, raised skin on the trunk, arms, legs, knees, elbows, genitals, and scalp. Nails may also thicken, become pitted, and separate from the nail beds.
-
Guttate psoriasis. This type of psoriasis affects mostly children. Symptoms may include many small spots of red, raised skin. A sore throat usually proceeds the onset of this type of psoriasis.
-
Pustular psoriasis. Symptoms may include small pustules all over the body or just on the palms, soles, and other small areas.
The symptoms of psoriasis may look like other skin conditions. Always talk with your healthcare provider for a diagnosis.
What Else Should I Ask My Healthcare Provider
If you have psoriasis, ask your healthcare provider:
- How can I prevent outbreaks and control symptoms?
- What medication will work best for me?
- What else should I do to improve symptoms?
- What are my options if creams dont work?
- Will psoriasis ever go away?
A note from Cleveland Clinic
Psoriasis, an itchy skin condition, can come and go throughout your life. Its related to an overactive immune response and is not contagious. If you have skin changes that arent going away, talk to your healthcare provider. There is no cure for psoriasis, but psoriasis treatments can improve symptoms. Your provider may prescribe a special cream or moisturizer or medications. Other therapies are available if creams or medicines dont work. Maintaining your overall health will also help improve symptoms.
Last reviewed by a Cleveland Clinic medical professional on 10/17/2020.
References
Also Check: Does Psoriasis Affect Your Immune System
Introduction To Psoriasis And Scaling Diseases
, and lichen sclerosus Lichen Sclerosus Lichen sclerosus is a disorder that tends to cause itching and can cause scarring in the area around the anus and genitals. The cause of lichen sclerosis is unknown, but it may involve the immune… read more are different skin disorders that have been grouped together because the bumps, rashes, scales, and skin discoloration they cause have similar characteristics. That is, the rashes and bumps have well-defined borders, and the scales usually do not crust, crack, or weep with fluid.
Doctors tell these disorders apart by examining the bumps, rashes, scales, and skin discoloration and noting where they appear on the skin.
Causes And Risk Factors Of Psoriasis
Psoriasis, in general, is a genetic condition passed down through families. “It’s likely that multiple genes need to be affected to allow psoriasis to occur and that it’s frequently triggered by an external event, such as an infection,” says James W. Swan, MD, professor of dermatology at the Loyola University Stritch School of Medicine in Maywood, Illinois.
Certain risk factors, such as a family history or being obese, may increase your odds of developing psoriasis.
According to the National Psoriasis Foundation , at least 10 percent of people inherit genes that could lead to psoriasis, but only 3 percent or less actually develop the disease. For this reason, it is believed that the disease is caused by a combination of genetics and external factors or triggers.
A psoriasis outbreak may be provoked by:
Read Also: Triamcinolone Acetonide Ointment For Psoriasis
Psoriasis As An Autoimmune Disease
The majority of scientists today believe psoriasis is an autoimmune disease. Its long been known that the immune system is involved in psoriasis. But the exact mechanism isnt certain.
In the past two decades, research has established that the genes and gene groups associated with psoriasis are . Research also established that immunosuppressant drugs are effective new treatments for psoriasis. These drugs work by suppressing the immune system thats attacking healthy tissue.
Research is ongoing on the role of the immune systems T cells in psoriasis. T cells are the immune systems soldiers that normally combat infections. When the T cells misfire and instead attack healthy skin, they release special proteins called cytokines. These cause skin cells to multiply and build up on your skin surface, resulting in psoriatic lesions.
A 2017 article reported on new research that has identified the interaction of particular T cells and interleukins already known to be involved in the development of psoriasis. As more specifics are known, it may become possible to develop new targeted drug treatments.
Epidemiology Of Psoriasis And Comorbid Diseases: A Narrative Review
- 1Hospital for Skin Disease , Chinese Academy of Medical Sciences and Peking Union Medical College, Nanjing, China
- 2Sino-French Hoffmann Institute, School of Basic Medicine, The Second Affiliated Hospital, Guangzhou Medical University, Guangzhou, China
- 3The State Key Laboratory of Respiratory Disease, The First Affiliated Hospital, Guangzhou Medical University, Guangzhou, China
You May Like: Ultraviolet Light Machine For Psoriasis
Are There Complications Of Psoriasis
In some people, psoriasis causes more than itchiness and red skin. It can lead to swollen joints and arthritis. If you have psoriasis, you may be at higher risk of:
- Use medicated shampoo for scales on your scalp.
Other steps you should take to stay as healthy as possible:
- Talk to your healthcare provider about lowering your risk for related conditions, such as heart disease, depression and diabetes.
- Lower your stress with meditation, exercise or seeing a mental health professional.
List Of Some Autoimmune Disorders
Primary immune deficiency diseases are those caused by inherited genetic mutations. Secondary or acquired immune deficiencies are caused by something outside the body such as a virus or immune suppressing drugs.
Primary immune diseases are at risk to an increased susceptibility to, and often recurrent ear infections, pneumonia, bronchitis, sinusitis or skin infections. Immunodeficient patients may less frequently develop abscesses of their internal organs, autoimmune or rheumatologic and gastrointestinal problems.
- Primary immune deficiencies
Recommended Reading: Triderma Md Psoriasis Control Cream
How Is Psoriasis Classified
Certain features of psoriasis can be categorised to help determine appropriate investigations and treatment pathways. Overlap may occur.
- Early age of onset < 35 years vs late age of onset > 50 years
- OMIM Online Mendelian Inheritance in Man
- Chularojanamontri L, Griffiths CE, Chalmers RJ. The Simplified Psoriasis Index : a practical tool for assessing psoriasis. J Invest Dermatol. 2013 133:195662. doi: 10.1038/jid.2013.138. PubMed PMID: 23807685.
- Feldman SR, Fleischer AB Jr, Reboussin DM, et al. The self-administered psoriasis area and severity index is valid and reliable. J Invest Dermatol. 1996 106:1836. doi:10.1111/1523-1747.ep12329912PubMed PMID: 8592072.
- Papp K, Gordon K, Thaçi D, et al. Phase 2 trial of selective tyrosine kinase 2 inhibition in psoriasis. N Engl J Med. 2018 379:131321. doi:10.1056/NEJMoa1806382. PubMed
- Fleming P. Tofacitinib: a new oral Janus kinase inhibitor for psoriasis. Br J Dermatol. 2019 180:1314. doi:10.1111/bjd.17323. PubMed
Psoriasis And Behets Disease
Behçets disease is a Th1-dominant disease, and recent studies have furthermore shown that Th17-related cytokines are also involved . However, association of Behçets disease and psoriasis is rare . Musculoskeletal involvement is frequent in Behçets disease, and enthesopathy is also observed in Behçets disease. Recently, BD is proposed to be included in MHC-I-opathy with prevalence of HLA-B 51, in which CD8+ T-cells activate neutrophils and drive inflammation . Apremilast blocks phosphodiesterase-4, which regulates immune and inflammatory processes through modification of the levels of intracellular cyclic adenosine monophosphate, protein kinase A, and various forms of inflammatory cytokine production. Apremilast is used for both psoriasis and Behçets disease.
Don’t Miss: Is Aquaphor Good For Psoriasis
What Is Psoriasis Symptoms Causes Diagnosis Treatment And Prevention
Psoriasis is an autoimmune disease that causes plaques, which are itchy or sore patches of thick, dry, discolored skin.
While any part of your body can be affected, psoriasis plaques most often develop on the elbows, knees, scalp, back, face, palms, and feet.
Like other autoinflammatory diseases, psoriasis occurs when your immune system which normally attacks infectious germs begins to attack healthy cells instead.
Can I Pass Psoriasis On To My Children
While psoriasis is not contagious, it does have a genetic component, which means it can be inherited. About 40% of patients with psoriasis have a family history of the disease. However, just because you have psoriasis does not mean you will always pass it on to your children. If one parent has psoriasis, there is about a 10% chance of passing it on to offspring. If psoriasis affects both parents, there is a 50% chance of passing it on to their children.
Also Check: Medical Treatment For Scalp Psoriasis
What Causes Psoriasis Outbreaks
Psoriasis outbreaks differ from person to person. No one knows exactly what causes flare-ups. Common psoriasis triggers may include:
- Skin injury .
- Streptococcal or other infection that affects the immune system.
- Certain prescription medications .
- Cold weather, when people have less exposure to sunlight and humidity and more to hot, dry indoor air.
Risk Factors And Etiology
Approximately one-third of patients with psoriasis have a first-degree relative with the condition. Research suggests a multifactorial mode of inheritance.2,3 Many stressful physiologic and psychological events and environmental factors are associated with the onset and worsening of the condition. Direct skin trauma can trigger psoriasis . Streptococcal throat infection may also trigger the condition or exacerbate existing psoriasis. Human immunodeficiency virus infection has not been shown to trigger psoriasis, but can exacerbate existing disease. As the infection progresses, psoriasis often worsens.1
Smoking increases the risk of psoriasis and its severity.1,4 Obesity and alcohol use and abuse are also associated with psoriasis.4,5 These associations may not be causative patients with psoriasis may be more susceptible to unhealthy behaviors.4
Recommended Reading: Can You Have Both Eczema And Psoriasis