Diagnosis Of Nail Psoriasis
Diagnosis of nail psoriasis can be made easily in a patient with concomitant skin psoriasis. Close examination with a hand lens can help in appreciating the above mentioned changes in a greater detail. However, in cases of isolated nail psoriasis and in patients presenting with a diagnostic dilemma to a dermatologist the following techniques can be used.
When Do Nail Symptoms Occur
PsA may not present the same way for every person, but it typically always develops in stages.
In its preclinical stage, psoriatic inflammation may only cause fatigue, heel pain, and joint pain. At this time, doctors may not yet be able to identify the condition as PsA.
Once the condition progresses a little, nail changes can begin to occur. These include pitting, discoloration, softness, holes, and dactylitis, or the swelling of the toe or finger. This may still be an early phase of the condition.
As the condition progresses even further, these and other symptoms may get worse and progress to severe damage to the bones.
When To See A Doctor
Nail psoriasis is not contagious, and treatment can reduce or help control the symptoms.
If the nails show symptoms of psoriasis or a fungal infection, see a doctor. This is especially important for people who already have a type of psoriasis.
A person may have to try several treatments before finding one that works.
Symptoms can take time to improve, and they may take up to a year to clear. One reason for this is that the nail plate grows very slowly. The symptoms may also return at a later date.
With new drugs appearing on the market, more effective treatments for nail psoriasis may be on the horizon.
Read Also: Aloe Vera Plant For Psoriasis
Narrowband Ultraviolet B Phototherapy
For adults with generalized plaque psoriasis, the recommended NB-UVB phototherapy starting dose should be based on the minimal erythema dose or it should be determined based on a fixed-dose or skin-phototype protocol.
For adults with generalized plaque psoriasis, a treatment phase of thrice-weekly dosing of NB-UVB phototherapy is recommended.
For adults with psoriasis, treatment with short-term psoralen plus ultraviolet A monotherapy is more effective than NB-UVB.
Owing to its increased safety, higher convenience, and lower cost, NB-UVB is preferred over PUVA monotherapy for psoriasis in adults, even though it is less effective.
In adults with generalized plaque psoriasis, NB-UVB is recommended over broadband ultraviolet B monotherapy.
Treatment with NB-UVB monotherapy is recommended for guttate psoriasis patients, regardless of their age.
For appropriate patients with generalized plaque psoriasis, home-based NB-UVB phototherapy is recommended as an alternative to in-office NB-UVB phototherapy.
Treatment with NB-UVB phototherapy is recommended for pregnant patients who have guttate psoriasis or generalized plaque psoriasis.
As a measure to possibly improve efficacy, NB-UVB phototherapy can be safely augmented with concomitant topical therapy using retinoids, vitamin D analogues, and corticosteroids.
Oral retinoids can be combined with NB-UVB phototherapy in appropriate patients with generalized plaque psoriasis if they have not responded adequately to monotherapy.
Epidemiology Of Nail Psoriasis
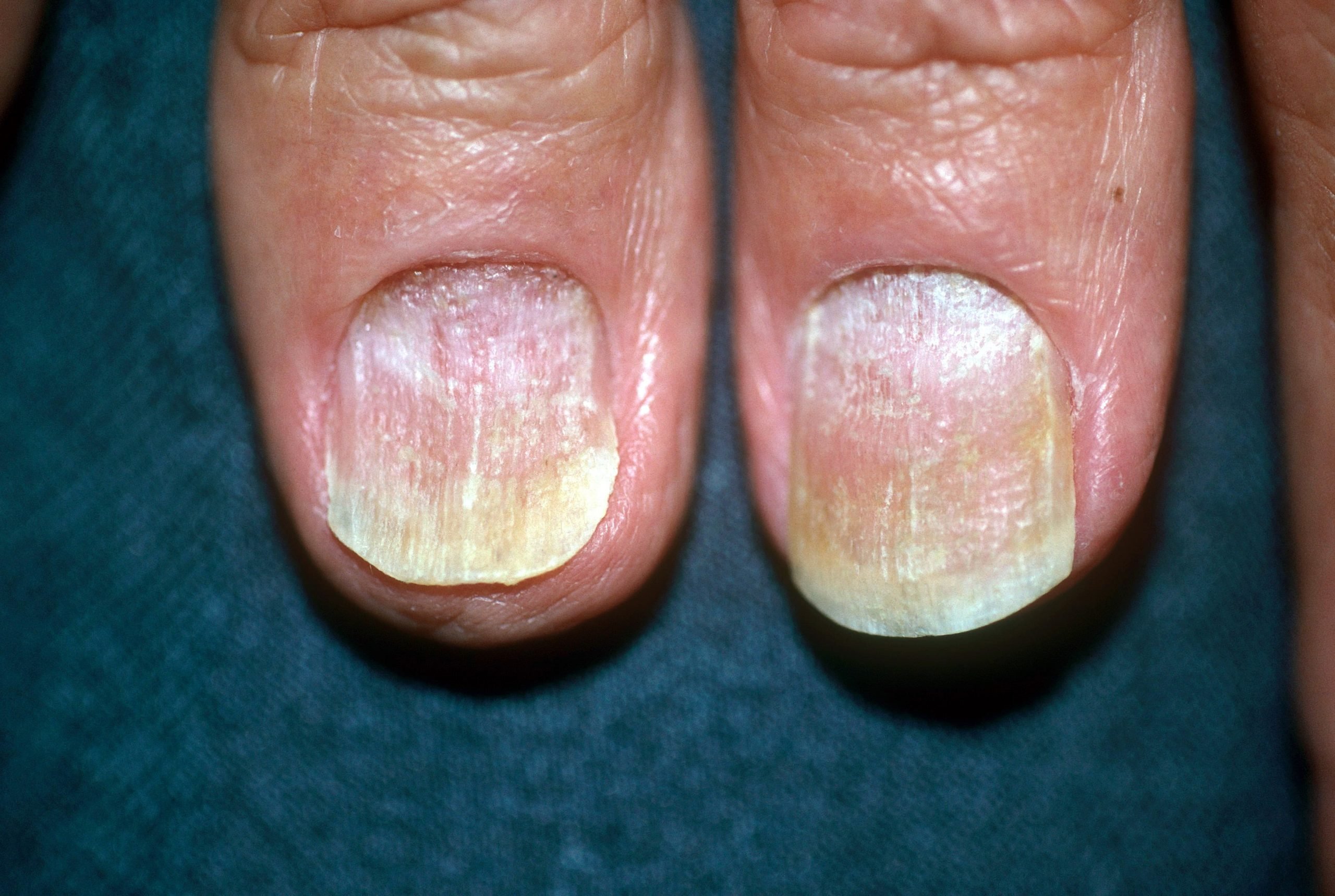
Psoriatic nail disease occurs in 10-55% of all patients with psoriasis, and approximately 7 million people in the United States have psoriasis . Less than 5% of psoriatic nail disease cases occur in patients without other cutaneous findings of psoriasis. About 10-20% of people with psoriasis also have psoriatic arthritis, and nail changes are seen in 53-86% of patients with psoriatic arthritis.
Psoriasis tends to run in families. In Farber’s questionnaire study of 2100 patients, 36% of patients reported the presence of psoriasis in at least 1 relative. Among siblings, 8% are affected if neither parent has psoriasis. This percentage increases to 16-25% if 1 parent or sibling has the disease, and it reaches up to 75% if both parents are affected. If 1 twin has psoriasis, the other twin is at an increased risk of having psoriasis .
In Scandinavia, the prevalence rate of nail psoriasis for adults with psoriasis approaches 5%. The prevalence increases with the age of the population studied.
Psoriatic nail disease is not associated with mortality. In severe cases, patients may have functional and psychosocial impairments.
Males and females are affected equally by nail psoriasis, and the prevalence of nail psoriasis increases with the age of the population studied.
Recommended Reading: Is Hemp Good For Psoriasis
Tlc For Hands And Feet
Avoiding injuries, even small ones , makes good sense for people with psoriasis or PsA affecting the hands and feet.
âThe Koebner phenomenon is the flaring of psoriasis in response to injury. Even minor trauma can cause a flare,â says Duffin. âFor example, if you use your nails to pry open a lid, youâre probably going to make your nail psoriasis worse.â
Similarly, shoving feet into shoes without enough room to wiggle toes or wearing high heels means youâre putting constant pressure on nails and joints, which can increase pain and nail problems.
âI generally recommend flats that have good cushioning and arch support that takes the weight off toe joints â which doesnât mean wearing ballet slippers that have no padding in the bottom,â says Gottlieb.
âYou donât want a triangle profile that squeezes the toes, because that elicits pain.â She also cautions that flip-flops, a summer favorite, expose toes and feet to trauma.
A consultation with a podiatrist, who can advise on the right footwear and design an orthotic for individual foot issues, is often helpful for people with PsA that affects the feet, Gottlieb says.
What Are Nail Psoriasis Causes And Risk Factors
Psoriasis is not contagious. How psoriasis of the nails develops is not completely known. Nail involvement appears to result from a combination of genetic , immunologic, and environmental factors.
Psoriasis tends to run in families. About 40% of people with psoriasis have a first-degree relative who is known to have the condition. If both parents have psoriasis, a person’s risk is up to 75%. Males and females are equally likely to have psoriasis. Psoriasis can occur in people of all races.
Read Also: What Is The Best Medicine For Psoriasis
What Is Psoriatic Nail Disease
Psoriatic nail disease is a type of psoriasis. It is not caused by infection and you cannot pass it on to anyone else.
Psoriasis is a common skin condition that usually causes patches of red, scaly skin but sometimes only affects the nails. There is also a form of arthritis that is linked to psoriasis, called psoriatic arthritis. Psoriatic nail disease is particularly common if you have psoriatic arthritis. You can read more about these conditions in the separate leaflets called Psoriasis and Psoriatic Arthritis.
Overview Of Treatment Of Nail Psoriasis
Many treatment options are available after the diagnosis of nail psoriasis is made. The treatments focus on improvement of the functional and psychosocial aspects of psoriatic nail disease.
The treatment options for nail psoriasis include topical corticosteroids, intralesional corticosteroids, psoralen plus ultraviolet light A , topical fluorouracil, topical calcipotriol, topical anthralin, topical tazarotene, topical cyclosporine, avulsion therapy, and systemic therapy for severe cases. Onychomycosis requires antifungal therapy for improvement. Laser and light therapies have emerged as possible cost-efficient, in-office treatments however, large-scale trials are needed, particularly in consideration for the effects in combination with other current therapies.
For preventive care, keep the nails dry and protect them from trauma to avoid the Koebner effect and possible secondary microbial colonization. In areas of onycholysis, the nail plate should be trimmed to the point of separation for medications to be effective.
At present, no definitive and curative treatment has been agreed upon by medical experts. Discuss all treatment options for psoriatic nail disease with the patient, and choose the best individually tailored regimen.
Also Check: What Is Autoimmune Disease Psoriasis
What Are The Signs And Symptoms Of Psoriasis
Dry, thick, and raised patches on the skin are the most common sign of psoriasis. These patches are often covered with a silvery-white coating called scale, and they tend to itch.
While patches of thickened, dry skin are common, psoriasis can cause many signs and symptoms. What you see and feel tends to vary with the:
-
Type of psoriasis you have
-
Places psoriasis appears on your body
-
Amount of psoriasis you have
You Have Swollen Reddened Skin Around Your Nails
Sometimes people with psoriatic arthritis develop a skin infection around their nails called paronychia, explains Dr. Garshick. This can happen when your nail separates from the bed, when your nails are cracked, or when you have broken skin that allows bacteria, dirt, or other organisms in the cut, according to the Cleveland Clinic. With paronychia, the skin around one or more of your fingernails may suddenly be swollen, reddened, and painful. Paronychia typically requires medical attention treatment depends on the severity of your infection but could include antibiotics, according to the Cleveland Clinic.
Also Check: How Do I Get Rid Of Psoriasis On My Nails
How Common Is Nail Psoriasis
Around half of people with psoriasis have symptoms that affect their nails, and most people with some form of psoriasis will have nail symptoms at some point during their lives. Nail involvement is more common among people with psoriatic arthritis, affecting 80-90% of those patients3,8.
Nail psoriasis usually does not affect people who do not have psoriasis that affects other parts of their bodies. It generally affects people of all ages, genders, and ethnicities at equal rates5.
Treating Nail Psoriasis: Not Just A Cosmetic Issue
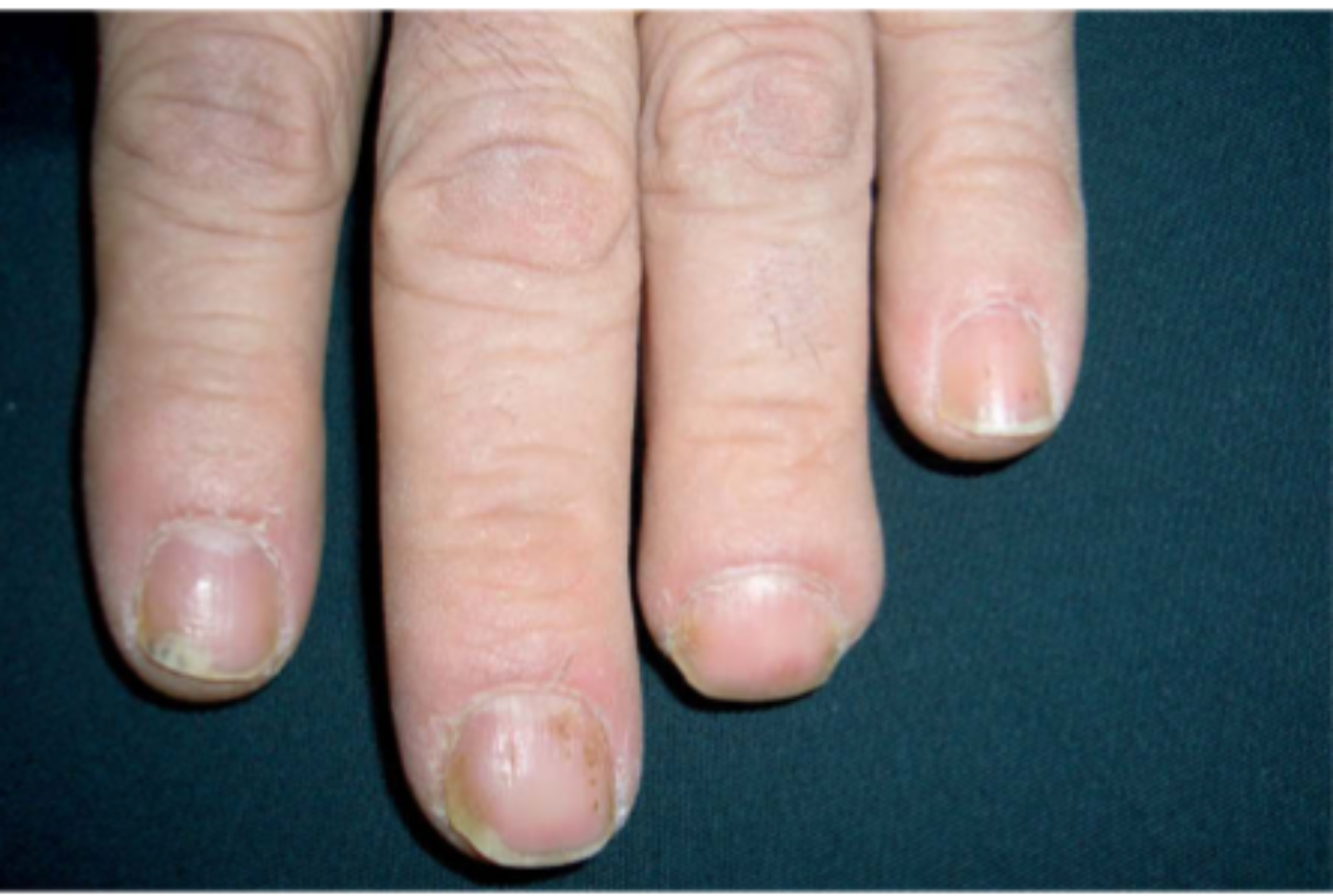
The first level in management of nail psoriasis is patient education.
Crumbling, pitted nails are a common experience for patients with skin psoriasis. A 2007 study in the Journal of the American Academy of Dermatology found that as many as 90 percent of psoriasis patients will experience nail psoriasis at some point. Similarly, between 50 percent and 87 percent of patients with psoriatic arthritis have nail psoriasis as well.
The same 2007 study found that nail psoriasis has major impacts on quality of life, with 90 percent of patients with the condition reporting that they felt distressed by the appearance of their nails. Ninety percent also reported restricting their daily activities because of their nail condition. Understanding the presentation and treatment of nail psoriasis is thus key for rheumatologists, dermatologists and general practitioners who might encounter patients with nail psoriasis. A new article in the journal Clinical and Experimental Rheumatology aims to clarify the latest research.
Clinical features of nail psoriasis
Assessing nail psoriasis]
There are multiple scales used to assess nail psoriasis, but the one used in most clinical trials is NAPSI, the Nail Psoriasis Severity Index. This scale uses a quadrant system to record the location and extent of psoriasis of the nail.
Treatment of Nail Psoriasis
Also Check: How Do You Get Rid Of Psoriasis
How Common Are Psoriatic Arthritis Fingernails And Toenails
Psoriasis and psoriatic arthritis are autoimmune diseases that cause inflammation.
- Psoriasis occurs when the bodys immune system attacks your skin, causing red, scaly, inflamed patches.
- Psoriatic arthritis occurs when the immune system attacks your joints and connective tissues . The disease causes pain and swelling in your joints, as well as fatigue.
Nail symptoms are common in people with psoriasis and even more common in those with psoriatic arthritis. As many as 80% of people with psoriatic arthritis notice changes in their nails. In fact, nail symptoms can be an early warning sign of this type of arthritis.
Complications Of Toenail Psoriasis You Should Be Aware Of
As noted above, toenail psoriasis can lead to a condition known as onycholysis, in which the nail detaches from the nail bed. This can allow bacteria access to the nail bed, leading to infection.
Subungual hyperkeratosis, the accumulation of a chalky substance under the nail, can cause the nail to become raised, which may be painful and can cause difficulty walking normally or wearing shoes.
Read Also: Body Surface Area Assessment Psoriasis
The Advent Of New Treatment Options: Biologic Therapy
Overall, the conventional treatment for nail psoriasis appears to be unsatisfactory, tedious, and inconvenient. Most of the treatment options achieve only a moderate efficacy, complete clearance is infrequent and efficacy of conventional therapy decreases with time. This clinical challenge faced by many dermatologists has recently been addressed with the introduction of the biological response modifiers. These agents have demonstrated efficacy in both the skin and nail components of psoriasis.
Infliximab
The best studied biologic agent is infliximab. The best evidence comes from the EXPRESS trial which was a phase-3 double-blinded, placebo-controlled trial . A total of 378 patients with moderate to severe plaque type psoriasis with nail involvement were randomly assigned in a ratio of 4:1 to receive infliximab 5 mg/kg at weeks 0, 2, 6, and every 8 weeks till week 46. Placebo was given at 0, 2, 6, 14, 22 and crossing over to infliximab occurred at week 24. This study showed that infliximab resulted in significant improvement in nail psoriasis as early as week 10 and at week 50 full clearance was evident in 45% of patients.
Etanercept
Adalimumab
In a study done by van den Bosch et al., 40 mg of adalimumab every other week reduced the mean NAPSI score by 65% after 20 weeks .
Ustekinumab
How Can Nail Psoriasis Be Treated
Psoriasisis a condition that is unique to each person who has it, and so finding atreatment or combination of treatments that work can be a process of trial anderror. Due to how often we use our hands and feet, and the fact that nails growvery slowly, nail psoriasis can be quite difficult to treat.
Nailpsoriasis is mostly treated with topical treatment.Steroid-based treatments are likely to be offered and can be useful, but arenot suitable for long-term use. A moderately potent steroid tape isavailable on prescription and often used for nail psoriasis, as it can be cutto size and wrapped around the nail.
VitaminD-based treatments can also be useful in nail psoriasis. The treatment can beapplied to the affected area, and the fingers then wrapped or covered to helpit to absorb effectively. This should not be done with a steroid treatment. Similarly,topical retinoids applied around and under the nails atnight may be helpful for nail psoriasis. Occasionally, if a fungal infection isalso present, antifungal cream may also be prescribed.
Ultravioletlight therapy, systemic or biologic treatments are not likely to be prescribedfor nail psoriasis alone, but may improve the nails when being used to treatthe rest of a persons psoriasis. However, any nail improvement may lag behindthe rest of the skin for a few months.
Read Also: Best Thing For Psoriasis On Face
Impact On Quality Of Life
Nail psoriasis has a profound negative influence on all aspects of quality of life as well as on daily, sports, and professional activities. Women try to hide their nails and cover them with nail lacquer although common nail varnishes are not harmful, artificial nails, particularly when long, increase the mechanical stress and strain to the nail plate nail bed attachment acting as a Köbner phenomenon and worsening nail psoriasis. Similarly, professional activities with particular use of the fingers may have a deteriorating effect on the disease. Matrix involvement scores higher than pure nail bed affection as it results in more obvious nail plate damage.
Pathophysiology Of Nail Psoriasis
The pathogenesis of the psoriatic nail disorder is not completely known. Nail psoriasis may be due to a combination of genetic, environmental, and immune factors. A well-known fact is that a familial aggregation of psoriasis exists. Studies have linked psoriasis with certain human leukocyte antigen subtypes . A T-cellmediated inflammatory process is being investigated as part of the pathogenesis of psoriasis.
Recommended Reading: Red Light Therapy For Psoriasis
Impact On Function And Quality Of Life
The clinical signs of nail psoriasis are highly visible and have a significant impact on quality of life. In a survey to evaluate the subjective complaints associated with nail involvement, questionnaires were sent to 7000 patients with psoriasis. One thousand seven hundred twenty-eight patients of mean age 47 years and mean disease duration of 12 years provided evaluable responses. Nail psoriasis was present in 1369 , with both fingers and toes affected in 62.6% of patients, just fingers in 26.8% and only toes in 8.6%. There was a positive association between duration of skin lesions and nail psoriasis. Pitting was reported by 75.3% of patients, upward lifting of the nail by 49.3%, onycholysis by 46.2% and discoloration by 29.2%.
Pain caused by nail changes occurred in 51.8% of patients, and more then 90% were concerned about the cosmetic appearance of their nails. Normal daily activities were negatively impacted in 58.9% of patients and a similar number reported that nail psoriasis inhibited their usual housekeeping activities. Importantly, 47.9% of respondents noted that their nail condition restricted their professional activities.
Another study in 69 patients with PsA found that severe nail disease was associated with functional impairment related to arthritis and with higher depression and anxiety scores on the Stanford hospital anxiety and depression scale .
How Does Psoriasis Affect The Elbows And Knees
The elbows and knees are also very common sites for plaque psoriasis symptoms. Half of people with the condition report having symptoms on their elbows, and around one-third of people have symptoms on their knees2. Plaques in these locations can tend to lead to painfulcracks or fissures because the joints move so much during normal activities, which ruptures the plaques. There is a wide range of treatment options available for people with psoriasis symptoms on the elbows and knees.
Read more information on symptoms and treatments for psoriasis on elbows and knees.
Don’t Miss: What Does Psoriasis Look Like On Your Head
What Are Medical Treatments For Nail Psoriasis
A doctor may recommend that a part of the nail be removed, either chemically or surgically. Chemical removal of the nail involves putting an ointment on the nails for seven days. The nail comes off by itself with no bleeding.
Even with effective treatment, an improvement in symptoms may take a long time, since eight to 12 months can be needed to generate a new fingernail.