Does Having Psoriasis Increase The Risk Of Developing Ibd
There are only a few studies that looked into the risk of IBD in people who have been diagnosed with psoriasis. They have shown conflicting results: Some have shown an increased risk of IBD in those that have psoriasis and others have shown the opposite. Additionally, the methods that were used in these studies were not without their drawbacks, which makes the conclusions more difficult to stand by.
One large meta-analysis showed that there is a “significant” association between psoriasis and IBD. Patients with psoriasis had a greater risk of developing Crohn’s disease and ulcerative colitis. The risk of Crohn’s disease was higher than the risk for ulcerative colitis.
At present, it’s not known exactly what the risk is, but there does seem to be a trend towards people with psoriasis having an increased risk of developing Crohn’s disease. The same might not be true for ulcerative colitis: There is less evidence that people with psoriasis might be at an increased risk of developing ulcerative colitis, or the effect might be less than it is for Crohn’s disease.
Before Taking This Medicine
You should not use Humira if you are allergic to adalimumab.
Before you start using this medicine , tell your doctor if you have signs of infection–fever, chills, sweats, muscle aches, tiredness, cough, bloody mucus, skin sores, diarrhea, burning when you urinate, or feeling constantly tired.
Humira should not be given to a child younger than 2 years old . Children using this medicine should be current on all childhood immunizations before starting treatment.
Tell your doctor if you have ever had:
-
a chronic infection
-
any numbness or tingling, or a nerve-muscle disorder such as multiple sclerosis or Guillain-Barre syndrome
-
an allergy to latex rubber
-
if you are scheduled to have major surgery or
-
if you have recently received or are scheduled to receive any vaccine.
Tell your doctor where you live and if you have recently traveled or plan to travel. You may be exposed to infections that are common to certain areas of the world.
Humira may cause a rare type of lymphoma of the liver, spleen, and bone marrow that can be fatal. This has occurred mainly in teenagers and young men with Crohn’s disease or ulcerative colitis. However, anyone with an inflammatory autoimmune disorder may have a higher risk of lymphoma. Talk with your doctor about your own risk.
It is not known whether this medicine will harm an unborn baby. Tell your doctor if you are pregnant. Make sure any doctor caring for your newborn baby knows if you used adalimumab while you were pregnant.
Correlations Between Psoriasis And Inflammatory Bowel Diseases
Nevena Skroza
1Department of Dermatology Daniele Innocenzi, A. Fiorini Hospital, Sapienza University of Rome, Via Firenze, Polo Pontino, 04019 Terracina, Italy
Abstract
For a long time the relationship between inflammatory bowel diseases and psoriasis has been investigated by epidemiological studies. It is only starting from the 1990s that genetic and immunological aspects have been focused on. Psoriasis and IBD are strictly related inflammatory diseases. Skin and bowel represent, at the same time, barrier and connection between the inner and the outer sides of the body. The most important genetic correlations involve the chromosomal loci 6p22, 16q, 1p31, and 5q33 which map several genes involved in innate and adaptive immunity. The genetic background represents the substrate to the common immune processes involved in psoriasis and IBD. In the past, psoriasis and IBD were considered Th1-related disorders. Nowadays the role of new T cells populations has been highlighted. A key role is played by Th17 and T-regs cells as by the balance between these two cells types. New cytokines and T cells populations, as IL-17A, IL-22, and Th22 cells, could play an important pathogenetic role in psoriasis and IBD. The therapeutic overlaps further support the hypothesis of a common pathogenesis.
1. Introduction
2. Epidemiological Correlations
Families affected by Crohns disease or psoriasis are also more likely to be affected by other immune-mediated diseases.
3. Genetic Correlations
Don’t Miss: Can You Have Multiple Types Of Psoriasis
Psoriatic Arthritis Increases The Risk For Uveitis Crohn Disease
Individuals with psoriatic arthritis have a higher risk for uveitis and Crohn disease than the general population and individuals with psoriasis, according to a new review.
To conduct their study, the researchers used data from the UK Clinical Practice Research Datalink between 1998 and 2014. Individuals with psoriatic arthritis who were aged 18 to 89 years were included in the study analysis .
_____________________________________________________________________________
_____________________________________________________________________________
Participants with psoriatic arthritis were matched to individuals with psoriasis and a member of the general population.
Poisson regression was used to determine the adjusted relative risks of uveitis, IBD, Crohn disease, and ulcerative colitis.
Results showed that participants with psoriatic arthritis had a higher risk of uveitis than the general population and psoriasis cohorts. Psoriatic arthritis also significantly increased the risk for Crohn disease but not for ulcerative colitis.
In a primary care-based incidence cohort of patients with , there were substantial risks of developing uveitis and/or Crohns disease, but not ulcerative colitis, when compared with the general population and psoriasis controls, the researchers concluded.
Amanda Balbi
Reference:
What Is Crohns Disease
Crohns disease is a type of inflammatory bowel disease. The cause of Crohns is currently unknown, although genetics, heredity, and environmental factors may all play a role.
People with this condition have chronic inflammation in their digestive tract. This is caused by an exaggerated immune system response to the beneficial bacteria that live in the gut.
Crohns affects people differently. Some symptoms you may experience with Crohns include:
- diarrhea
Read Also: What Causes Scalp Psoriasis To Spread
Don’t Miss: How Do You Treat Psoriasis Of The Skin
Subgroup Analyses Regarding Psoriasis
Further subgroup analyses were performed upon stratification by sex and age . In terms of age, the risk of developing psoriasis was consistently greater in all age groups, including those younger than 30 years. With regard to gender differences, both male and female patients with IBD demonstrated an increased risk of psoriasis. Further analyses conducted on disease severity revealed consistent findings . Subgroup analyses with psoriatic arthritis by age and sex also revealed an increased risk of developing in both female CD and UC patients .
Fig. 2.
Subgroup analysis to assess the risk of psoriasis in patients with IBD by age and sex. CD, Crohns disease CI, confidence interval HR, hazard ratio IBD, inflammatory bowel disease UC, ulcerative colitis.
What Should I Avoid While Using Humira
Do not inject Humira into skin that is bruised, red, tender, or hard.
Avoid being near people who are sick or have infections. Tell your doctor at once if you develop signs of infection.
Do not receive a “live” vaccine while using adalimumab. The vaccine may not work as well during this time, and may not fully protect you from disease. Live vaccines include measles, mumps, rubella , polio, rotavirus, typhoid, yellow fever, varicella , or zoster .
You May Like: How Can I Get Rid Of Psoriasis
How Is Ibd Linked To Plaque Psoriasis
Psoriasis and IBD are both conditions with symptoms that are caused by inflammation that is due to an overreaction of the immune system3. Researchers believe that there is a genetic link between the two conditionsthat certain families carry specific genes that affect the immune systems functioning and make members of those families more likely to develop both conditions5.
People With Psoriasis More Likely To Develop Certain Gut Disorders
25 October 18
People with psoriasis may be at greater risk of developing certain gut disorders, a new study finds.
The research discovered that people with psoriasis, an inflammatory skin condition, were about two times more likely to develop the gut disorders Crohn’s disease and ulcerative colitis compared to people in the general population. Both Crohn’s disease and ulcerative colitis are types of inflammatory bowel disease , a condition in which people experience chronic inflammation in the gastrointestinal tract, according to the Centers for Disease Control and Prevention.
The findings suggest a significant link between these conditions, and “patients with psoriasis should be informed about the increased risk of IBD,” the researchers, from Chang Gung Memorial Hospital in Taiwan, wrote in the Oct. 24 issue of the journal JAMA Dermatology. If patients with psoriasis have bowel symptoms, those individuals may need to consult with gastroenterologists, the authors said.
Recommended Reading: What To Do For Psoriasis On Eyelids
Primary Nonresponse To Drugs
The reason for the higher primary nonresponse rate in IBD compared with other chronic inflammatory diseases is not known but may be driven by greater molecular heterogeneity in IBD. This may be due to the huge array of antigens contained within the gut, which may drive the inflammatory response, or the unique function of the gut as a regulatory and homeostatic organ of the immune system . Alternatively, failure to attain adequate serum drug concentrations may occur more frequently in IBD as discussed below.
Dont Overlook The Elevated Risk Of Inflammatory Bowel Disease In Patients With Psoriasis
According to 2 recent studies, psoriasis seems to be linked to inflammatory bowel disease , possibly through overlapping genetic and immunopathogenic mechanisms.1,2 The pathways mediating inflammation in both psoriasis and IBD may lead to an increased risk of subclinical and undiagnosed IBD among psoriasis patients.1
Take Note
- Genetic and immunopathogenic mechanisms that overlap could explain the connection between psoriasis and IBD.
- A new study found that gastrointestinal signs and symptoms were more prevalent in psoriasis patients than in controls.
- Physicians should keep the psoriasis-IBD comorbidity link in mind when treating their patients with psoriasis.
Evidence suggests, too, that the risk of developing IBD increases with psoriasis severity.1 New research provides consistent evidence that psoriasis patients are at increased risk for experiencing IBD-related gastrointestinal signs and symptoms1 and developing comorbid IBD.2
The relationship between 2 chronic conditions
A modified CalproQuest score was calculated to identify individuals with an increased IBD risk. The CalproQuest is an 8-item questionnaire developed to predict a greater chance of a positive result on a fecal calprotectin test, which reflects intestinal mucosal inflammation indicative of IBD. Psoriasis therapy via injection within the prior 4 months was used as a surrogate for more-severe disease.
Meta-analysis supports a psoriasis-IBD link
Some theories
Its worth asking the question
Read Also: Can Psoriasis Be On Your Face
Skin Rashes Caused By Crohns Disease
- Skin rashes are a common occurrence for people with Crohns disease.
- There are a variety of different causes of rashes, and there are many different treatments for them.
- Keeping Crohns disease under control can be the best way to treat skin rashes.
Skin rashes are one of the most common symptoms associated with Crohns disease. More than 3,200 members of MyCrohnsAndColitisTeam report skin disorders as a symptom. People with Crohns disease are more likely to report skin complications than those with ulcerative colitis. One study of 950 people with inflammatory bowel diseases found 43 percent of those with Crohns disease reported complications outside the intestinal tract, including skin problems, as opposed to 31 percent of those with ulcerative colitis. A possible reason is that ulcerative colitis is confined to the colon and rectum, but Crohns disease can affect any part of the digestive tract from the mouth through the intestines to the anus.
It’s a Crohn’s thing, one MyCrohnsAndColitisTeam member told another who was reporting a rash. About 40 percent of people with Crohns disease develop specific skin manifestations of inflammatory bowel disease known as Crohns skin disease.
Is A New Crohns Disease Treatment On The Horizon
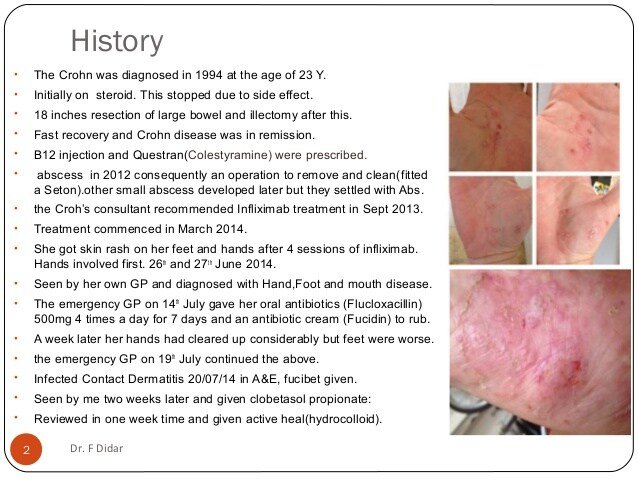
Oct. 17, 2012 A drug used to treat psoriasis may provide a much-needed option for people with bad cases of Crohnâs disease.
In the new study, some people with moderate to severe Crohns given Stelara began to see improvements in their symptoms within six weeks.
Crohns disease is an inflammatory bowel disease marked by inflammation and damage of any part of the digestive tract.
Inflammation plays a central role in both Crohnâs and the skin disease psoriasis. Stelara blocks two proteins that promote inflammation. A commonly used class of drugs for Crohns blocks the activity of another protein that promotes inflammation called tumor necrosis factor . Treatments in this class include Cimzia, Humira, and Remicade.
But not everyone with Crohnâs is helped by TNF drugs, and some who do well at first stop responding to them.
âAbout 60% of people with Crohnâs disease will have an initial response to TNF drugs and of those, half will lose their response over the course of the year,â says researcher William J. Sandborn, MD. He is the chief of the division of gastroenterology at the University of California San Diego School of Medicine. They can still try additional TNF drugs if they havent been helped by one, but surgery is often their last resort, he says.
The new findings are âvery encouraging and bode well that this drug will eventually become a new treatment option for people with Crohnâs,â Sandborn says.
You May Like: Is Neem Oil Good For Psoriasis
You May Like: What Helps Psoriasis On Face
How Common Is Ibd Among People With Psoriasis
Studies suggest that people with psoriasis have a higher risk of developing IBD during their lifetimes3. Statistically, the two conditions occur more often in people who have been studied than they would if the two diseases were not somehow related. For example, one recent study found that 1 in 10 women with psoriasis had developed an IBD4. Research also suggests that people who have both psoriasis and psoriatic arthritis had an even higher risk of inflammatory bowel disease than people who have psoriasis but no psoriatic arthritis diagnosis5.
How Common Is Psoriasis In People With Ibd
IBD is considered an immune-mediated condition. Its not uncommon for people who have one immune-mediated disease to develop another one. IBD and psoriasis are both conditions that have an unknown cause and result in inflammation.
In recent years researchers are uncovering more about the connection between IBD and psoriatic diseases. Psoriasis in the general population only runs at approximately 2% to 3% but for people with IBD, it tends to be higher. Studies show that people with Crohns disease and ulcerative colitis may develop psoriasis at a rate of approximately 13%.
Don’t Miss: How Does Psoriasis Affect Nails
Losing Weight Can Ease Symptoms Of Psoriatic Arthritis And Crohns
If you have both psoriatic arthritis and Crohns, getting the right medications is paramount, but adopting healthy habits is also crucial. That includes a diet low in saturated fat, cholesterol, and, particularly, simple sugars: A review published in April 2020 in the journal Rheumatology and Therapy found that people who have psoriatic arthritis are significantly more likely to have type 2 diabetes than the population at large, possibly because inflammation of the skin and joints may affect glucose metabolism.
Obese patients with gut disorders like Crohns also dont seem to respond to medication as vigorously as nonobese patients, and the drugs may lose their effectiveness more quickly.
Weight can dramatically affect inflammatory disease, Qureshi affirms.
The conundrum is that people with gut disorders and PsA may be more prone to obesity in the first place, whether because they are taking steroids or other factors.
Some studies suggest that up to 45 percent of people with PsA are obese a report published in 2019 in Medicine found that about 28 percent of participants with PsA were obese, as well as suffering from weight-related conditions such as high blood pressure, diabetes, and high cholesterol.
Yet losing just 5 percent of weight can make a difference in managing these conditions. Losing weight, says Qureshi, can have more of an impact than being on a drug.
RELATED: 9 Psoriatic Arthritis Friendly Weight-Loss Tips
How Do Skin Rashes Affect People With Crohns Disease
Rashes and skin problems are a common complaint of MyCrohnsAndColitisTeam members with Crohns disease and affect their lives to varying degrees.
- I get rashes from CD.
- Rash all over my face, so itchy. Not much helps.
- I usually experience a rash during a flare-up.
- Over the last year, I have had countless random rashes show up on my body. I was going crazy until I was recently diagnosed with Crohns disease.
- I developed this rash on my face around my eyes and forehead. Its red, burns, and my eyes feel swollen.
- I know my Crohns causes weird rashes sometimes when it is warmer out, sometimes when I am stressed.
Dont Miss: Productos Naturales Para La Psoriasis
Recommended Reading: What Is The Best Shampoo For Psoriasis
Blank On Student Transcript
If a students name appears on the end of quarter course list for a course, but no grade is reported, the registrar will leave a blank for that course on the students transcript.
A blank which is not replaced by a grade assigned by the instructor, after one quarter on a students record, will then be replaced by an F, NP, or U grade.
Also Check: Cbd Oil For Psoriasis Reviews
The Common Treatments For Gonorrhea
Overview Gonorrhea is a bacterial infection most commonly transmitted through sex. It can affect males and females. Neisseria gonorrhoeae, the causal bacterium, usually targets warm, moist areas of the body. The urethra, rectum, vagina, and throat are the most common sites of infection. It may also affect the cervix
Don’t Miss: Natural Psoriasis Treatment During Pregnancy
Health Conditions Linked To Psoriasis
It is important to visit your primary care provider regularly to screen for these diseases because you may not notice or feel symptoms for some of these health conditions. In addition, if some of these conditions are caught early, they can be easily treated with lifestyle changes or medications.
Evidence shows that people who treat their psoriasis effectively can also lower the risk of other comorbidities.
In 2019, the National Psoriasis Foundation and the American Academy of Dermatology published guidelines on the treatment of psoriasis with attention to comorbidities. The guidelines state the following health conditions as comorbidities of psoriasis.