Psoriatic Arthritis Presentation Classification And Diagnosis
Prevalence of PsA is not known, but it is estimated to be from 0.3% to 1% of the U.S. population. In the psoriasis population, PsA is reported to range from 7% to 42%, although more recently, these numbers have been found to be in the 15% to 25% range . This type of inflammatory arthritis can develop at any age but usually is seen between the ages of 30 and 50 years, with men being affected equally or a little more than are women. Clinical symptoms usually include pain and stiffness of affected joints, > 30 minutes of morning stiffness, and fatigue.
The presentation of joint involvement can vary widely. Five subtypes of arthritis were identified by Moll and Wright in 1973, which included arthritis with predominant distal interphalangeal involvement, arthritis mutilans, symmetric polyarthritis , asymmetric oligoarthritis , and predominant spondylitis . Patients with PsA may also have evidence of spondylitis or sacroiliitis with back pain > 3 months, hip or buttock pain, nighttime pain, or pain that improves with activity but worsens with rest. The cervical spine is more frequently involved than is the lumbar spine in patients with PsA.
Radiograph of the Right Hand and Right Foot
Read Also: Best Bath Soak For Psoriasis
Psoriasis And Psoriatic Arthritis Treatments Can Make It Easier To Live A Full Life With These Conditions
There are no cures for either disease, but an effective treatment plan can minimize symptoms for both psoriasis and psoriatic arthritis. With psoriasis, doctors generally prescribe treatments that prevent your skin cells from growing too quickly, according to the Mayo Clinic. There are many treatment options for this, including creams, light therapy, or oral or injected medications, the Mayo Clinic explains.
As for psoriatic arthritis, treatments generally focus on controlling inflammation to minimize your joint pain and damage. Your doctor might suggest pharmacological options that target your immune system to lower inflammation, along with exercise or other lifestyle modifications, according to the Mayo Clinic. With each condition, the best treatment depends on your particular situation.
Is Psoriasis The Same As Eczema
Psoriasis and eczema are two different skin conditions. They differ in where the disease appears on the body, how much it itches and how it looks. Eczema tends to appear more often behind the knees and inside the elbows. Eczema also causes more intense itching than psoriasis. Many people, especially children, can get both eczema and psoriasis.
Also Check: Head And Shoulders For Scalp Psoriasis
Psoriatic Arthritis And Psoriasis Are Both Autoimmune Conditions
Both conditions happen when your autoimmune system mistakenly attacks healthy cells in your body, causing inflammation. With psoriasis, new skin cells grow too quickly and build up, resulting in thick, scaly rashes that can make it painful to move, according to the Cleveland Clinic. People with psoriatic arthritis also have inflammation, but their symptoms generally result in stiff, painful joints, and swollen skin surrounding the joints, according to the Mayo Clinic.
The exact causes of autoimmune diseases are not clear. Some experts theorize that injuries might trigger psoriatic arthritis and that infections could trigger psoriasis, according to John Hopkins University. Doctors commonly suspect that genetics may determine whether someone is susceptible to autoimmune disorders, but the specifics explaining how or why are up in the air.
Both conditions are lifelong diseases that can alternate between periods of remission where you have very few symptoms and flares in which your symptoms are worse.
Why Is It Important To Recognise Psa
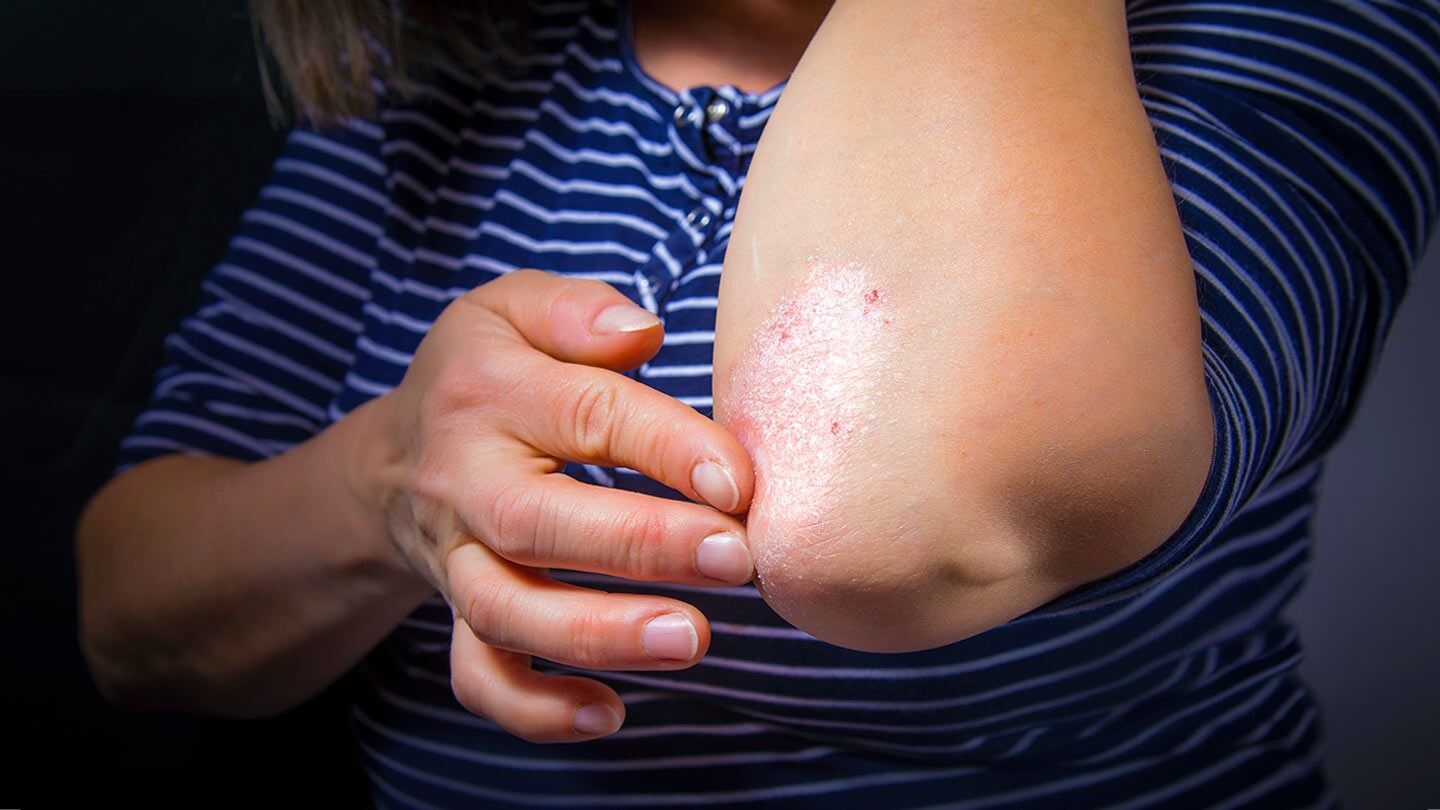
Although PsA was thought initially to be a relatively benign disorder, registry data has shown the destructive and progressive nature of the disease it has a similar impact on quality of life and functional ability as in rheumatoid arthritis. In recent years, the additional burden of increased mortality and significant cardiovascular comorbidity has also been identified. Despite this, identification and treatment are still not optimal. There are significant delays in diagnosis for the majority of patients . Delay in diagnoses of 6 and 12 months have been shown to impact on long-term joint damage and functional disability.
Read Also: Que Es Psoriasis En La Piel Imagenes
How Are Ra And Psa Diagnosed
Because these two conditions share similar symptoms, it’s important to get an accurate diagnosis from a rheumatologist. A rheumatoid factor blood test is one way your doctor can tell which condition you have. RF is a protein found in people with rheumatoid arthritis. People with PsA usually don’t have it. Blood tests looking for other antibodies such as anti-CCP can also help differentiate the two.
Another way to tell is to look at your skin and nails. If you have scaly patches on your skin, pitting and flaking on your nails, or both, you have PsA.
Once you’ve had the disease for a while, X-rays might also be able to distinguish the two conditions.
It is possible to have RA and PsA together, but it’s rare. If you do have both, many of the treatments, including some medications, will work for both conditions.
The Effects Of Psoriasis And Psa
The most common form of psoriasis is plaque psoriasis, also known as psoriasis vulgaris. It affects 80 to 90 percent of all people with psoriasis. Its characterized by plaques. These may come and go, even though psoriasis is a chronic, or long-term, disease.
Like psoriasis, PsA is chronic. PsA is also a progressive condition. It gets worse over time. The inflammatory response that PsA triggers in joints can lead to the gradual destruction of joint cartilage and bone.
If left untreated, this process can result in twisted, painful, or swollen joints that no longer function. Joint pain may be widespread or may only occur on one side of your body.
If you have psoriatic disease, youre also at risk for other conditions. This includes:
Recommended Reading: Vitamins For Eczema And Psoriasis
Summary Plaque Psoriasis Vs Psoriasis
Psoriasis is a chronic multisystem disease with skin and joint manifestations. Plaque psoriasis is the commonest form of psoriasis which is characterized by the appearance of reddish well-demarcated plaques with silver scales usually on the extensor surface of the knees and elbows. Accordingly plaque psoriasis is one manifestation of the broad spectrum of dermatological and systemic manifestations which are identified as psoriasis. This can be identified as the difference between plaque psoriasis and psoriasis.
Recommended Reading: Does Epsom Salt Help Arthritis
Facing The Challenges Of A Dual Diagnosis With Psoriatic Arthritis
Psoriatic arthritis can co-occur with conditions such as fibromyalgia and gout.
About 1.5 million Americans have psoriatic arthritis , a form of inflammatory arthritis. For many of those people, PsA is only part of the story. Thats because patients may have two or more chronic conditions.
Psoriatic arthritis can be difficult to diagnose because it shares symptoms with conditions like rheumatoid arthritis, osteoarthritis, fibromyalgia, and gout.
According to the Psoriatic Arthritis in America 2016 survey, most people who have PsA experience multiple symptoms over a period of years before the condition is properly diagnosed. The survey found that 41 percent of people saw at least four health professionals before a PsA diagnosis was made.
Don’t Miss: Does Hydrocortisone Cream Help Psoriasis
Psoriasis And Psoriatic Arthritis May Increase Gout Risk
Learn how psoriasis, psoriatic arthritis and gout are connected through the presence of uric acid in the body.
Doctors have noticed a connection between psoriasis, psoriatic arthritis and gout for decades. The common denominator is uric acid, a substance that forms when the body breaks down purines, which are found in human cells and many foods. In psoriasis and psoriatic arthritis, uric acid is thought to be a byproduct of rapid skin cell turnover and systemic inflammation. In gout, uric acid builds up in the joints and tissue around the joints often the big toe and forms needle-like crystals, which can cause sudden episodes of intense pain and swelling. If left untreated, gout can become chronic and lead to joint damage.
Psoriasis Arthritis Signs And Symptoms
Psoriatic arthritis, or PsA, is a chronic, autoimmune form of arthritis that causes joint inflammation and occurs with the skin condition psoriasis. It can affect large or small joints, and less commonly, the spine. About a third of people with psoriasis develop PsA.
This condition can also cause painful joints, referred to as psoriatic arthritis.
there is no cure for psoriasis. However, treatment can help manage symptoms, and people with psoriasis can.
What are the signs and symptoms of psoriasis? Dry, thick, and raised patches on the skin are the most common sign of psoriasis. These patches are often covered with a silvery-white coating called scale, and they tend to itch. While patches of thickened, dry skin are common, psoriasis can cause many signs and symptoms.
Diagnosis is typically based on the signs and symptoms. No cure for psoriasis is known, but various treatments can help control the symptoms. These treatments include steroid creams, vitamin D 3 cream, ultraviolet light, and immunosuppressive drugs, such as methotrexate. About 75% of skin involvement improves with creams alone.
The 5 most common symptoms of psoriasis include: Rashes or patches of red, inflamed skin , often covered with loose, silver-colored scales in severe cases, the plaques will grow and merge into.
Psoriasis is a common skin.
If a person also develops psoriatic arthritis, certain joints may stiffen, swell, and become painful, and the symptoms may be worse in the morning.
Read Also: Treatment For Psoriasis On Lips
Psoriatic Arthritis Treatment Options
Psoriatic arthritis symptoms can be treated with systemic drugs that affect your whole body. Depending on your unique case of psoriatic arthritis, your dermatologist may prescribe methotrexate, cyclosporine or certain biologics. In some cases, steroid injections can reduce inflammation quickly in an affected joint. At Dermatology Associates of Plymouth Meeting, we may team with a board-certified rheumatologist to treat joint disease linked to psoriatic arthritis.
In addition to these medications or treatment options, whether you are experiencing psoriasis or psoriatic arthritis, your dermatologist may recommend lifestyle changes to help minimize symptoms and flare ups. We always encourage changes such as quitting smoking, drinking less and minimizing stressors which can help with psoriasis and psoriatic arthritis flare ups. With psoriasis and psoriatic arthritis, it is common for symptoms to come and go, but it is important to continue taking medication and undergoing treatments recommended by your dermatologist.
If you are struggling to manage your plaque psoriasis or psoriatic arthritis, schedule an appointment today. Our team of board-certified dermatologists are experts in treating all types of psoriasis and can develop a personalized treatment plan based on your unique background and needs.
Recent Posts
What Causes Ra And Psa
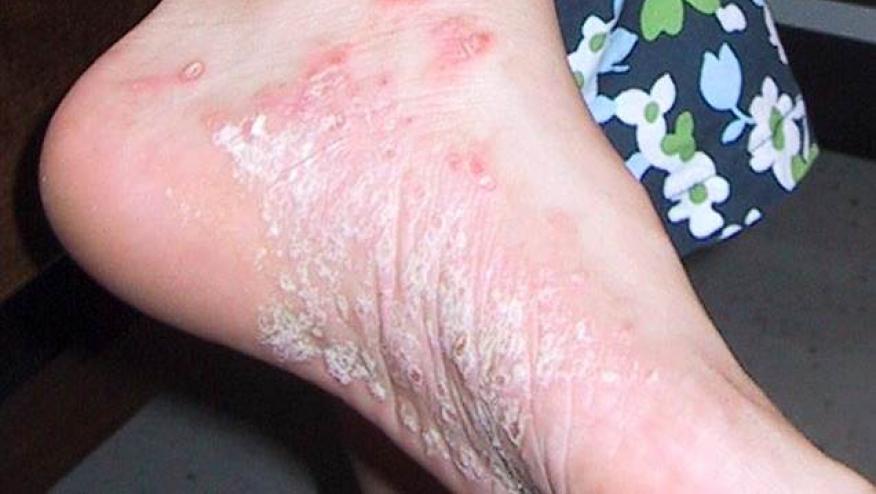
RA runs in families. If you have a close relative with the disease, your chances of having it are higher. Women are more likely than men to get RA. Usually the symptoms start between ages 40 and 60.
PsA also runs in families. Certain genes may be linked to the condition. Compared to RA, PsA often starts between ages 30 and 50.
Researchers don’t know exactly what triggers either type of arthritis. But they think it probably comes from a mix of genes and other factors, including hormones and bacterial or viral infections that may send the immune system into overdrive.
You May Like: Causes Of Psoriasis And Eczema
Treatment Options For Both Psoriasis And Psa
Drugs to suppress immune system activity are among the most effective treatments for psoriasis and PsA.
Systemic, immune-suppressing drugs often provide relief for both conditions. However, your risk of secondary infections and other side effects is greater when using these drugs.
If you have severe psoriasis and are diagnosed with PsA, your doctor may prescribe the anti-inflammatory and immune-suppressant drug methotrexate . This medication aims to slow down the cells in your body that are reproducing too quickly and causing psoriasis flares.
Common side effects of methotrexate include:
- headaches
- dizziness
- upset stomach
A newer class of drugs called biologics, in particular TNF blockers, targets specific parts of the immune system more precisely. Because of this, your doctor may be more likely to recommend them over methotrexate.
Biologics reduce inflammation and psoriasis outbreaks in most people who take them. There are a number of brands of biologics approved for treatment of psoriasis in the United States.
Biologics need to be injected. Some need to be administered more often than others. Common side effects include:
- allergic reaction
Does This Patient Have Psoriatic Arthritis
Psoriatic arthritis is an inflammatory arthritis that is characterized by a diversity of clinical manifestations and a highly variable disease course. This disorder was not recognized as a discrete entity until 1964, and it was Moll & Wrights landmark paper in 1973 that outlined the cardinal clinical features followed by familial studies a year later that documented the contribution of genetic factors in disease etiology.
Innovative translational studies and clinical trials over the last fifteen years have uncovered new disease mechanisms and fostered the development and validation of novel therapies, which have been incredibly effective for the varied clinical features of this disease. Recent attention has focused on the extra-articular manifestations and comorbid conditions associated with PsA because they may lessen function and quality of life and increase mortality.
Diagnosis
In the assessment of a patient for possible PsA, it is important to focus on the history and physical examination of the five key domains of this disease, which include integument manifestations of psoriasis, inflammatory peripheral arthritis, spondylitis, enthesitis, and dactylitis.
Psoriasis
Enthesitis
Dactylitis
Some patients may not have psoriasis but will recall a family history of psoriasis or psoriatic arthritis, which is important to document. Other important elements in the history are symptoms of enthesitis .
Recommended Reading: What Does Beginning Psoriasis Look Like
What Causes Psoriasis Outbreaks
Psoriasis outbreaks differ from person to person. No one knows exactly what causes flare-ups. Common psoriasis triggers may include:
- Skin injury .
- Streptococcal or other infection that affects the immune system.
- Certain prescription medications .
- Cold weather, when people have less exposure to sunlight and humidity and more to hot, dry indoor air.
Recommended Reading: What Helps With Arthritis In Back
Causes Of Psoriatic Arthritis
Almost 1 in 3 people with psoriasis also have psoriatic arthritis.
It tends to develop 5 to 10 years after psoriasis is diagnosed, although some people may have problems with their joints before they notice any skin-related symptoms.
Like psoriasis, psoriatic arthritis is thought to happen as a result of the immune system mistakenly attacking healthy tissue.
But its not clear why some people with psoriasis develop psoriatic arthritis and others do not.
Recommended Reading: How Can Psoriasis Be Treated
Up To 30 Percent Of People With Psoriasis Will Go On To Develop Psa And 85 Percent Of People With Psa Also Have Skin Psoriasis
Psoriasis and psoriatic arthritis are distinct conditions, but they are connected. In fact, data show that up to 30 percent of people with psoriasis will go on to develop PsA and 85 percent of people with PsA also have skin psoriasis.
Although people can be diagnosed with PsA without having any skin involvement, most often they will have a family member with skin psoriasis, says Rebecca Haberman, MD, a rheumatologist at NYU Langone Health in New York City.
Psoriasis is an inflammatory condition of the skin, while psoriatic arthritis also includes inflammation of the joints and entheses , .
Read on to find out the different symptoms of psoriasis vs. PsA, how they are diagnosed and treated, and what you need know about the link between these health conditions.
What Are The Symptoms Of Psoriasis
There are different types of psoriasis. The most common is chronic plaque psoriasis. This causes patches of red, raised skin, with white and silvery flakes.
It can occur anywhere on the skin, but most commonly at the elbows, knees, back, buttocks and scalp.
Psoriasis can cause small round dents in finger and toe nails, this is known as pitting. Nails can also change colour, become thicker and the nail may lift away from your finger.
Read Also: Rheumatoid Arthritis Edema
You May Like: Psoriasis Treatment In Ayurveda Patanjali
Psoriatic Arthritis Versus Rheumatoid Arthritis: Are They The Same
Psoriatic arthritis and rheumatoid arthritis are similar in they both involve your body mistakenly attacking your joints. However, with psoriatic arthritis, your skin is also going to suffer damages. Both have been proven to have genetic factors that are linked to being diagnosed with each disease.
The main difference is that with psoriatic arthritis you will always also be dealing with red, itchy, and painful skin. People living with Rheumatoid arthritis dont always have the accompanied skin condition and may only have to deal with the painful joints.
Read Also: Does Psoriatic Arthritis Itch
What Are The Causes Of Psoriatic Arthritis And Rheumatoid Arthritis
We donât have an understanding of what causes many autoimmune conditions, including RA and PsA, but there are common links among people who develop these diseases.
âWe donât know exactly what causes RA or PSA, but we do know there are genetic components and stress components to both,â Magdalena Perez-Rivera, MD, rheumatology specialist with Conviva Care Centers tells Health.
Here are some of the primary risk factors for RA and PsAyouâll see there is a good amount of overlap.
Read Also: Images Of Psoriasis On Elbows
Key Difference Plaque Psoriasis Vs Psoriasis
Psoriasis is one of the most common dermatological problems that can have adverse effects on both social and mental well-being of the patient. It is an autoimmune condition whose pathogenesis is triggered by different intrinsic and extrinsic factors. Psoriasis can be defined as a chronic multisystem disease with skin and joint manifestations. There are different forms of psoriasis including guttate psoriasis, pustular psoriasis, etc. Out of them, plaque psoriasis is the commonest form of psoriasis which is characterized by the appearance of reddish well-demarcated plaques with silver scales usually on the extensor surface of the knees and elbows. So plaque psoriasis is one element of psoriasis which can have various other clinical manifestations. This is the key difference between Plaque Psoriasis and Psoriasis.
Also Check: Where To Buy Imak Arthritis Gloves