How Does Psoriatic Arthritis Affect Your Feet
Psoriatic arthritis can also cause painful inflammation in the feet. You may feel it in the joints of your toes or ankles. Similar to your fingers, psoriatic arthritis can cause swelling of your entire toe and changes in your toenails.
Enthesitis, which is inflammation where your tendons and ligaments attach to bone, can develop with psoriatic arthritis. This may occur in the bottom of your foot as the result of plantar fasciitis or in your heel due to Achilles tendonitis. Pain is often worst when you first wake up in the morning or after periods of inactivity.
Other symptoms of psoriatic arthritis in your feet include:
How Is Psoriasis Treated
Psoriasis is usually treated by a dermatologist . A rheumatologist may also help with treatment. Treatments can include:
- ultraviolet light from the sun or from home or office treatments. But in some children, sunlight can make psoriasis worse.
- creams, lotions, ointments, and shampoos such as moisturizers, corticosteroids, vitamin D creams, and shampoos made with salicylic acid or coal tar
- medicines taken by mouth or injected medicines
A doctor might try one therapy and then switch to another, or recommend combining treatments. Its not always easy to find a therapy that works, and sometimes what works for a time stops helping after a while.
How Successful Are The Treatments
Anti-inflammatory drugs can help to reduce pain, swelling and stiffness. Unfortunately, however, they can make skin symptoms worse in some people. Steroid injections to joints may give relief. Disease-modifying drugs such as methotrexate can damp down both skin and joint symptoms, as can targeted biologic agents.
In some cases, surgery to remove a thickened synovial membrane , realign a joint or to fuse a joint may stop pain which results from movement.
Sometimes it is possible to remove the painful end of a bone .
Remember: All treatments may have unwanted side effects or require special precautions . Always make sure you have all the information before embarking on any course of therapy this includes reading the patient information leaflets provided with your medicines.
Don’t Miss: Long Term Effects Of Psoriasis
Nail Psoriasis Quick Guide
Learn more about the signs of nail psoriasis, Treatment options and get tips for caring for your nails without making your nail psoriasis worse.
Betteridge, N., Boehncke, W. H., Bundy, C., Gossec, L., Gratacos, J., & Augustin, M. . Promoting patient-centred care in psoriatic arthritis: a multidisciplinary European perspective on improving the patient experience. J Eur Acad Dermatol Venereol, 30, 576-585. doi:10.1111/jdv.13306
Jiaravuthisan, M. M., Sasseville, D., Vender, R. B., Murphy, F., & Muhn, C. Y. . Psoriasis of the nail: anatomy, pathology, clinical presentation, and a review of the literature on therapy. J Am Acad Dermatol, 57, 1-27. doi:10.1016/j.jaad.2005.07.073
Merola, J. F., Li, T., Li, W. Q., Cho, E., & Qureshi, A. A. . Prevalence of psoriasis phenotypes among men and women in the USA. Clin Exp Dermatol, 41, 486-489. doi:10.1111/ced.12805
Who Is At Risk For Palmoplantar Psoriasis
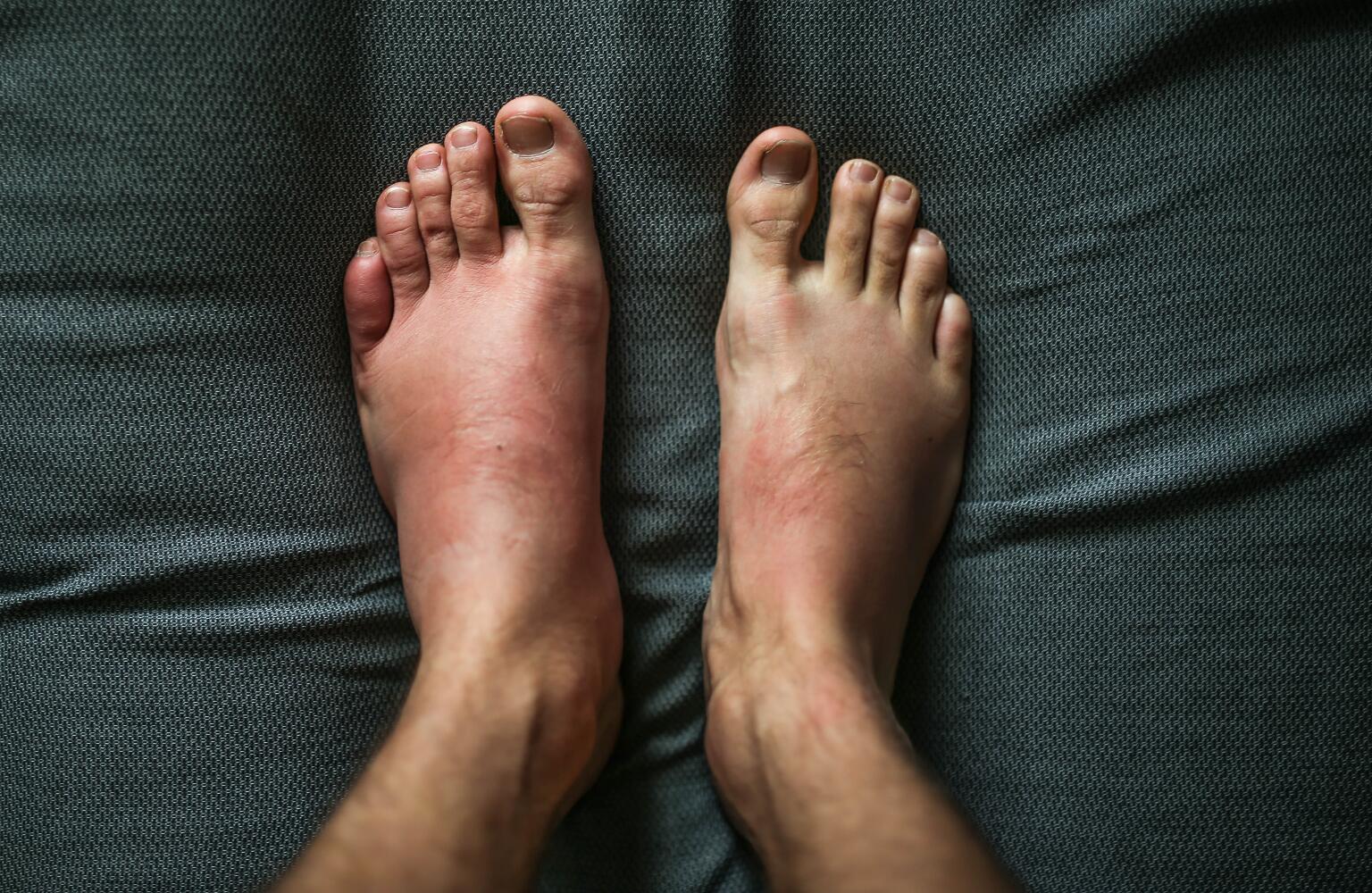
Although it can affect people of any age, there are certain groups of people who may be more susceptible to the skin condition. Theres a connection to genes and family history. Its far more likely that if someone in your family has or has had psoriasis, you will end up with one form or another throughout your life. According to Healthline, there are three genes associated with psoriasis. If you have any number of these, you are more likely to develop psoriasis symptoms throughout your life. The genes are NAT9, RAPTOR and SLC9A3R1.
Theres also a higher chance of someone suffering from palmoplantar psoriasis if they have suffered from certain health conditions. This can include strep throat, type 1 diabetes and even thyroid disease. Smokers also increase their chances of developing palmoplantar psoriasis due to the fact that smoking affects the immune system.
You May Like: Best Natural Treatment For Psoriasis
Also Check: Skin Conditions That Look Like Psoriasis
What Are The Symptoms Of Palmar And Plantar Psoriasis
Palmar and plantar psoriasis usually cause the palms and soles to be partially or entirely covered in thickened, red skin. You may have sharp, noticeable borders where the skin changes from psoriasis patches to unaffected areas. You may also have painful cracks, which are called fissures.
Common symptoms of psoriasis include:
- silvery scales
Researchers are not sure what causes any of the various types of psoriasis, but they do know that the immune system is involved.
However, certain risk factors can make you more likely to develop psoriasis. There are also risk factors that can specifically increase your risk for palmar and plantar psoriasis.
Common Types Of Psoriasis
This is the most common form, accounting for about 80 to 90% of cases.
Its symptoms are dry red skin lesions, known as plaques, covered in silver scales.
They normally appear on your elbows, knees, scalp and lower back, but can appear anywhere on your body.
The plaques can be itchy or sore, or both. In severe cases, the skin around your joints may crack and bleed.
Read Also: What Causes Scalp Psoriasis To Flare Up
For Best Results From Treatment
Treating nail psoriasis can be a challenge. It often takes time to treat. To get results, you need to treat your nails as directed and for as long as directed. Some patients need to try a few treatments to find one that works.
The right nail care can help you get the best results from treatment. Youll find out what dermatologists recommend at: 7 easy-to-follow nail care tips that can reduce nail psoriasis
ImagesImages used with permission of the Journal of the American Academy of Dermatology. J Am Acad Dermatol 2013 69:249.
ReferencesCrowley JJ, Weinberg JM, et al. Treatment of nail psoriasis: Best practice recommendations from the Medical Board of the National Psoriasis Foundation. JAMA Dermatol. 2015 Jan 151:87-94.Dogra A, Arora AK. Nail psoriasis: The journey so far. Indian J Dermatol. 2014 Jul 59:319-33.Lin YK, Chang YC, et al. A Chinese herb, indigo naturalis, extracted in oil used topically to treat psoriatic nails: A randomized clinical trial. JAMA Dermatol. 2015 Jun 151:672-4.Manhart R, Rich P. Nail psoriasis. Clin Exp Rheumatol. 2015 Sep-Oct 33:7-13.van der Velden HMJ, Klaassen KMG, et al. Fingernail psoriasis reconsidered: A case-control study. J Am Acad Dermatol 2013 Aug 69:245-52.
All content solely developed by the American Academy of Dermatology
The American Academy of Dermatology gratefully acknowledges the support from Amgen and .
What Can I Do To Help My Feet
The most important action is to seek advice and help when you notice any changes in your foot, whatever they may be. You can talk to your GP or local pharmacist for advice. Some problems can be resolved simply. For issues that are more persistent you may be referred to a specialist, such as a dermatologist, rheumatologist, physiotherapist, surgeon or chiropodist/podiatrist.
For general foot care, personal hygiene is important, particularly in avoiding fungal and viral infections. Change shoes and socks regularly, avoid shoes which are ill-fitting or cause bad posture. If you are overweight, losing weight could relieve the pressure on your joints and improve your walking gait.
If you are diagnosed with psoriasis, develop a treatment regime that works for you often, applying treatment after a bath or shower, along with the use of an emollient, can make the process easier.
If you have nail involvement, keep nails trimmed and clean. If they are thick, try trimming them after soaking them in a bath or shower, as this makes them softer and easier to cut. Alternatively, seek an appointment with a chiropodist, which is often available via the NHS.
If you have psoriatic arthritis, it is important to rest inflamed joints. Sourcing footwear that supports the foot and helps to reduce the pressure on the inflamed areas can help, as can inner soles and orthotic supports. Once again, a chiropodist is best placed to advise you.
This article is adapted from The psoriatic foot leaflet.
Read Also: Does Collagen Help With Psoriasis
Tablets Capsules And Injections
If your psoriasis is severe or other treatments have not worked, you may be prescribed systemic treatments by a specialist. Systemic treatments work throughout the entire body.
These medications can be very effective in treating psoriasis, but they all have potentially serious side effects. All the systemic treatments for psoriasis have benefits and risks. Before starting treatment, talk to your doctor about your treatment options and any risks associated with them.
If youre planning for a baby, become pregnant or are thinking of breastfeeding, you should also speak to your doctor first before taking any new medicine to check its suitable for use during pregnancy or breastfeeding.
There are 2 main types of systemic treatment, called non-biological and biological .
Take Care Of Your Feet
Start by taking good care of your feet. Wash them regularly with a gentle soap that does not dry the skin or trigger flares. Your doctor can offer medical advice to help you find a soap that will work for you. If you are particularly prone to outbreaks of psoriasis on your feet, an oatmeal foot bath may also soothe your skin.
When your feet are clean and dry, use a gentle moisturizer to keep your feet well hydrated. Some lotions with urea or salicylic acid are specifically designed for people diagnosed with psoriasis.
Recommended Reading: Root Cause Of Scalp Psoriasis
Other Causes For Itching On Hands And Feet
Itchiness on your hands or feet can indicate more than just skin problems. It could also be a result of the medication youâre taking or any health condition youâre dealing with.
1. Medications
People who are taking certain medications to treat some medical conditions also experience itchy hands and feet. This itchiness is usually a side effect of drugs. A person may also be allergic to the medication, and skin rashes or hives may appear.
Identification of the offending medication must be done and consultation with a doctor for advice on these side effects must be considered.
2. Medical Conditions
Persistent itchiness in the hands and feet may be a sign of Crohnâs disease, chronic kidney disease or liver failure. Scarring and inflammation of the liver associated with fatty liver disease can make the body itch, beginning with the palms and soles. Itchy palms may also be associated with thyroid disorders . Other diseases like cancer of the blood and the lymphatic tissues may manifest these symptoms, as well as nutritional deficiencies marked by a lack of vitamins B1, B6 and B12.
Proper diagnosis and treatment of the underlying condition are necessary before symptoms may be alleviated.
3. Stress
Medical Options That May Help Include:
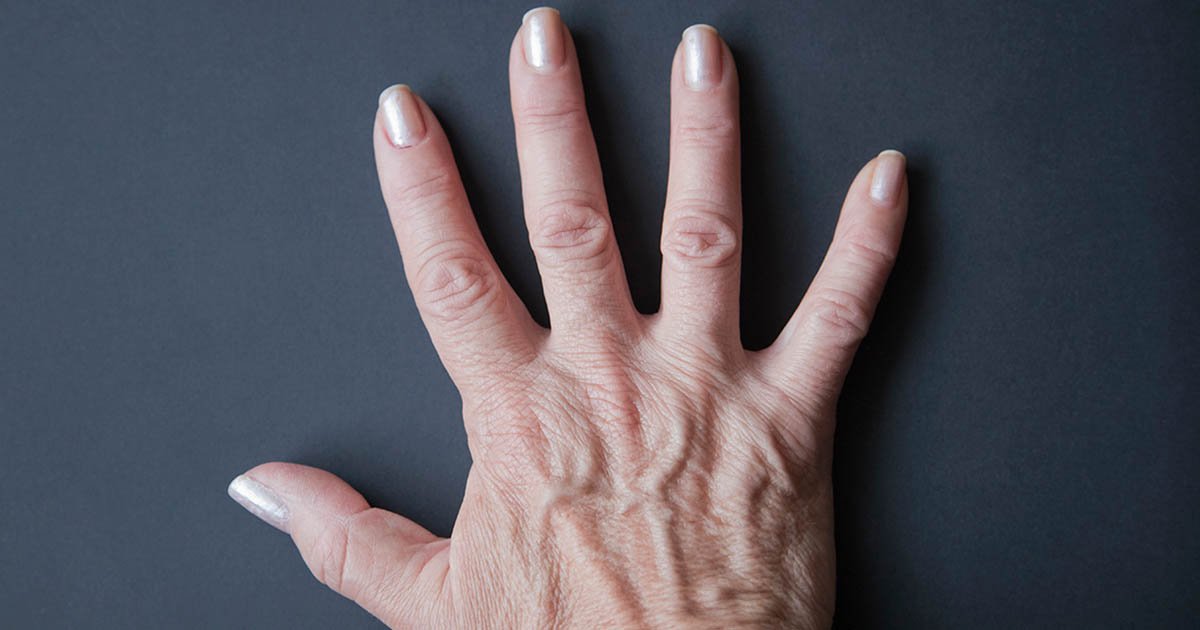
- Topical Steroids These are usually used for up to a month at a time. Steroids need to be strong to work on thick palms and soles, so they will need to be prescribed by your dermatologist.
- Topical Ointments Ointments derived from vitamin A and vitamin D can be used to slow down skin cell growth. These are not the same as the vitamins you take by mouth, Tung says. They are strong medications that need to be monitored by your dermatologist.
- Ultraviolet Light Treatment Light therapy slows down skin cell production in psoriasis and knocks out the immune cells causing the inflammation and is the next step in difficult-to-treat cases. Your doctor can prescribe these light treatments two to three times per week, Tung says. In some cases, ultraviolet light can be combined with a topical medication that increases the effect. Oral medication may also be used with light therapy.
- Oral Medication These included Vitamin A derivatives and Otezla . Otezla works on the inflammation without suppressing the immune system throughout the body, says Tung.
- Biologics. These drugs that block the immune system may be suggested if other treatments arent working. These medications are given by injection and are most likely to be needed for patients with more extensive or resistant psoriasis, says Tung. Since hand and foot psoriasis can be disabling, the more aggressive treatment may be warranted even though limited in extent.
Don’t Miss: Does Psoriasis Make Your Joints Hurt
When To See A Doctor
A doctor can prescribe medication to reduce discomfort during a psoriasis flare.
To diagnose the condition, the doctor will look at the symptoms and ask the person about their medical history.
They may take a small skin sample or biopsy to rule out other skin inflammatory conditions such as eczema, contact dermatitis or a fungal infection.
Often, the doctor can diagnose psoriasis by appearance alone.
There is little information about treatment specifically for palmoplantar psoriasis.
However, options that may relieve symptoms usually involve the following, alone or in combination:
- topical medications
- systemic medication, which affects how the body works
- light therapy
- biologic treatments
A person may have to work with their health provider and try several treatments to find a suitable one.
What Is Generalised Pustular Psoriasis
When pustular psoriasis occurs on areas of the body other than the palms and soles, it is known as Generalised pustular psoriasis or von Zumbusch pustular psoriasis. This is different and unrelated to palmoplantar. Again, the fluid in the pustules is not an infection or bacteria, and the pustules are not contagious.
GPP is quite rare, but it is a serious condition that requires urgent medical attention.
Recommended Reading: Salt Water Good For Psoriasis
Main Symptoms Of Psoriasis
Psoriasis typically causes patches of skin that are dry, red and covered in silver scales. Some people find their psoriasis causes itching or soreness.
There are several different types of psoriasis. Many people have only 1 form at a time, although 2 different types can occur together. One form may change into another or become more severe.
Most cases of psoriasis go through cycles, causing problems for a few weeks or months before easing or stopping.
You should see a GP if you think you may have psoriasis.
Small Area Big Impact
Your hands and feet make up only 4% of your body’s total surface area. But psoriasis here can still have a big effect on your quality of life. You might have pain, or you may just want to cover up the scales. If it affects your work, that could lead to a financial burden as well.
Hands and feet psoriasis can also cause your skin to:
- Crack or split
- Blister or have pimple-like spots
Recommended Reading: Best Over The Counter Psoriasis Medication
Nail Infection Needs Treatment Too
A nail infection can develop if you have nail psoriasis. Because a nail infection can look a lot like nail psoriasis, its important to find out if you have an infection. Testing, which usually consists of scraping the nail, can find an infection. If you have a nail infection, treatment can get rid of it.
Week 16 Results In Patients With Nail Psoriasis
Among patients with nail psoriasis at baseline, a greater percentage of adalimumab-treated patients compared with placebo-treated patients achieved NAPSI 50 at week 16 .3a). Improvement in nail psoriasis at week 16 following treatment with adalimumab is shown in Fig. Fig.4.4. Further evaluation showed that in adalimumab-treated patients, a greater percentage of NAPSI 50 Responders achieved an hfPGA score of clear or almost clear compared with NAPSI 50 Non-Responders .3b). In addition, NAPSI 50 Responders among adalimumab-treated patients demonstrated greater mean percent improvements in ESIF scores and DLQI scores compared with NAPSI 50 Non-Responders .3c). Finally, NAPSI 50 Responders experienced a greater mean reduction in pain VAS score than NAPSI 50 Non-Responders among patients treated with adalimumab .
Nail psoriasis improvement in one patient. Images from a white, 63-year-old male patient, illustrate improvement in the patients nail psoriasis from baseline to week 16 following adalimumab treatment. This patient was previously treated with corticosteroids and infliximab, but did not achieve response with infliximab. Nail Psoriasis Severity Index target fingernail scores range from 0 to 8.
Recommended Reading: Can Psoriasis Cause Weight Gain
Confidence In Social Situations
There is no denying that palmoplantar psoriasis can have an emotional impact, particularly in work or social situations. With hand psoriasis, you may feel self-conscious or embarrassed, say, when shaking hands or when around people who aren’t able to hide their uncertainty about your very visible condition. The same can be said if you have psoriasis on your feet, which may prompt you to avoid footwear like sandals and open-toe shoes.
What steps you take, if any, to hide your palmoplantar psoriasis is up to you. If you feel stress in social situations because of your lesions, it may help to remember that showing confidence and not drawing attention to your skin usually means others with follow suit. For example, try to look people directly in the eye rather than staring at your hands. If you feel comfortable doing so, you might also choose to educate others about your condition. While you may focus on it, most people may not even notice your condition if your skin is properly moisturized.
Remember: You have psoriasis, but it doesn’t define you.
What Are The Causes And Triggers Of Hand Psoriasis
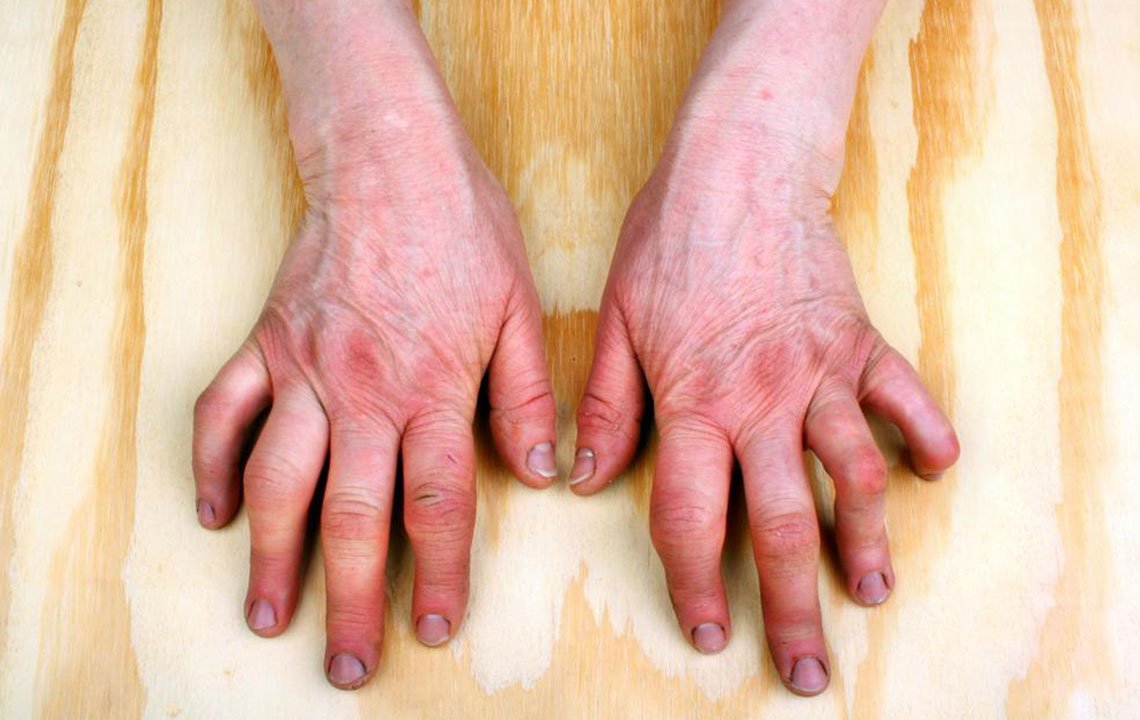
Doctors dont know exactly what causes psoriasis on the hands. Instead of one specific cause, theres likely a combination of genetic and environmental factors that play a role in its development. These include:1
- Genetics, specifically variations on the human leukocyte antigen Cw6, which is a gene partly responsible for immune system activity
- Friction to the palms, such as if you work with hand tools
- History of trauma or injury to the palms
- Irritants, such as exposure to chemicals
- Smoking
Those who work with their hands are most likely to have the condition, such as farmers, manual laborers, massage therapists, and environmental services professionals.
Many of the potential causes for hand psoriasis are also triggers for the condition, but there are a few other things that can cause a flare-up. Pay special attention to seasonal changes, household work, laundry detergent, and stress, as these can all make hand psoriasis worse. Another thing to consider is whether your nightly glass of wine has anything to do with psoriasis flare-ups. According to one 2019 study published in the journal Psoriasis, drinking alcohol has been linked to flare-ups in general, not just on the hands.4
Its tough when your livelihood is causing your hand psoriasis symptoms. Talk to your doctor or workplace if there may be adjustments that could reduce your flare-ups. Examples include protective gloves, padding tools, or reassignment to a different job duty.
You May Like: Over The Counter Medicine For Plaque Psoriasis