Animal Models For Pustular Psoriasis
Psoriasis is a disease unique to humans. However, certain aspects of the disease, such as activation of specific inflammatory pathways or infiltration of specific leukocyte populations such as neutrophils, can be modeled in mice. These models can be transgenic, xenografts, or induced via intradermal cytokine injection or via topical application of the TLR7 agonist imiquimod . We will address some of the mouse models that may have applicability for the study of GPP. No models currently exist to model PPP or ACH.
As discussed above, IL-36 activation is central to pustular psoriasis pathogenesis. Transgenic mice directing overexpression of the Il36a gene to the epidermis with the keratin 14 promoter were found to be small and showed flaky skin. Histology revealed a thickened epidermis, with leukocyte infiltration and increased expression of neutrophil chemokines. Interestingly, this phenotype peaked at postnatal day 5 and resolved by postnatal day 21. However, when these mice were backcrossed to Il36rn/ mice, they developed a dramatically more severe skin phenotype characterized histologically by intracorneal and intraepithelial pustules, parakeratosis and dilated superficial dermal blood vessels. Intradermal injection of Il-36 into mouse skin, has been used to induce an inflammatory phenotype, but this phenotype is less robust than the transgenic Il36rn/ model.
Supporting Acts: Indispensable Players In The Ensemble Of Psoriasis Immunology
Autoantigen presentation alone does not suffice to induce the psoriatic cascade in genetically predisposed individuals. Rather, costimulatory effects of various gene products orchestrate the activation of the actual autoimmune response. Such risk gene variants modulate inflammatory signaling pathways , peptide epitope processing and/or Th/c17 differentiation .
Table 1. Genetic factors implicated in psoriasis.
These genetic variations create costimulatory signals which modulate innate and adaptive immune mechanisms and shape the proinflammatory environment. In sum and in conjunction with the appropriate HLA molecules and autoantigens, they may eventually exceed the thresholds for activation and maintenance of pathogenic autoimmune and autoinflammatory responses in psoriasis . Likewise, regulatory mechanisms involving programmed death -1 signals have emerged recently as modulators of chronic inflammation in psoriasis . However, the complex interactions of various players are by no means fully understood. Therefore, they are listed here only as a whole.
The autoantigens described so far cannot fully explain the genesis of psoriasis. To give just one example of the latter notion: Psoriatic lesions can also occur in vitiligo foci that do not contain melanocytes . Alterations of resident cell types such as vascular endothelial cells or the cutaneous nervous system are also involved in the disease process . Further research is certainly needed here.
Autoimmune Diseases Comorbid With Psoriasis
Consistent with the autoimmune nature of psoriasis, numerous other autoimmune diseases, including autoimmune bullous diseases,125 vitiligo,126 alopecia127 and thyroiditis,128 are comorbid with psoriasis. Among them, autoimmune bullous diseases, such as bullous pemphigoid and antilaminin 1 pemphigoid, are consistently documented.37, 125, 129, 130 In a nationwide populationbased study of 3485 patients with bullous pemphigoid and 17425 matched controls, psoriasis is significantly associated with bullous pemphigoid .130 In a casecontrol study of 287 patients with bullous pemphigoid and 1373 matched controls, the prevalence rate of psoriasis is greater in patients with bullous pemphigoid compared with control subjects .125 This association is also significant among both sexes.125 In a case series of coexisting psoriasis and autoimmune bullous diseases, bullous pemphigoid is the most prevalent followed by antilaminin 1 pemphigoid .129
Psoriasis is also associated with autoimmune hair loss, namely alopecia areata , in a national database in Taiwan.132 In a cohort study including 25 341 patients with psoriasis, a significant association of alopecia areata and psoriasis was also noted .127
Recommended Reading: Can You Have Psoriasis On Your Hands
The Plot Thickens: Actual Auto
Pathogenic T cells in psoriatic skin lesions facilitate hyperproliferation of keratinocytes, influx of neutrophilic granulocytes, as well as production of other inflammatory cytokines, chemokines and antimicrobial peptides. They feature a Th17 signature, i.e., they express IL-17A, IL-22, and IFN- . Dendritic cells maintain activation and differentiation of lesional Th17 cells primarily through secretion of IL-23 .
Figure 2. Initiation of psoriasis by antigen-dependent and antigen-independent immune mechanisms. Complexes of self-DNA with fragments of the antimicrobial peptide, cathelicidin, can stimulate plasmacytoid dendritic cells through TLR9. They can also be presented by HLA-C*06:02 molecules and specifically activate T cells through their TCR. Likewise, the melanocyte-derived ADAMTSL5 can activate pathogenic CD8+ T cells after presentation by HLA-C*06:02.
In general, both HLA restriction and peptide specificity of a given T cell are determined by its T cell receptor repertoire . Activation and clonal expansion of T cells occur upon antigenic stimulation. In the absence of foreign antigens, clonal T cell expansion is highly suggestive for autoimmunity in inflammatory diseases . Indeed, oligoclonal T cell expansion has been identified in psoriatic lesions in early well-designed studies as well as in more recent investigations . It has been interpreted as an indicator for antigen-specific immune responses.
Treatments For Pustular Psoriasis
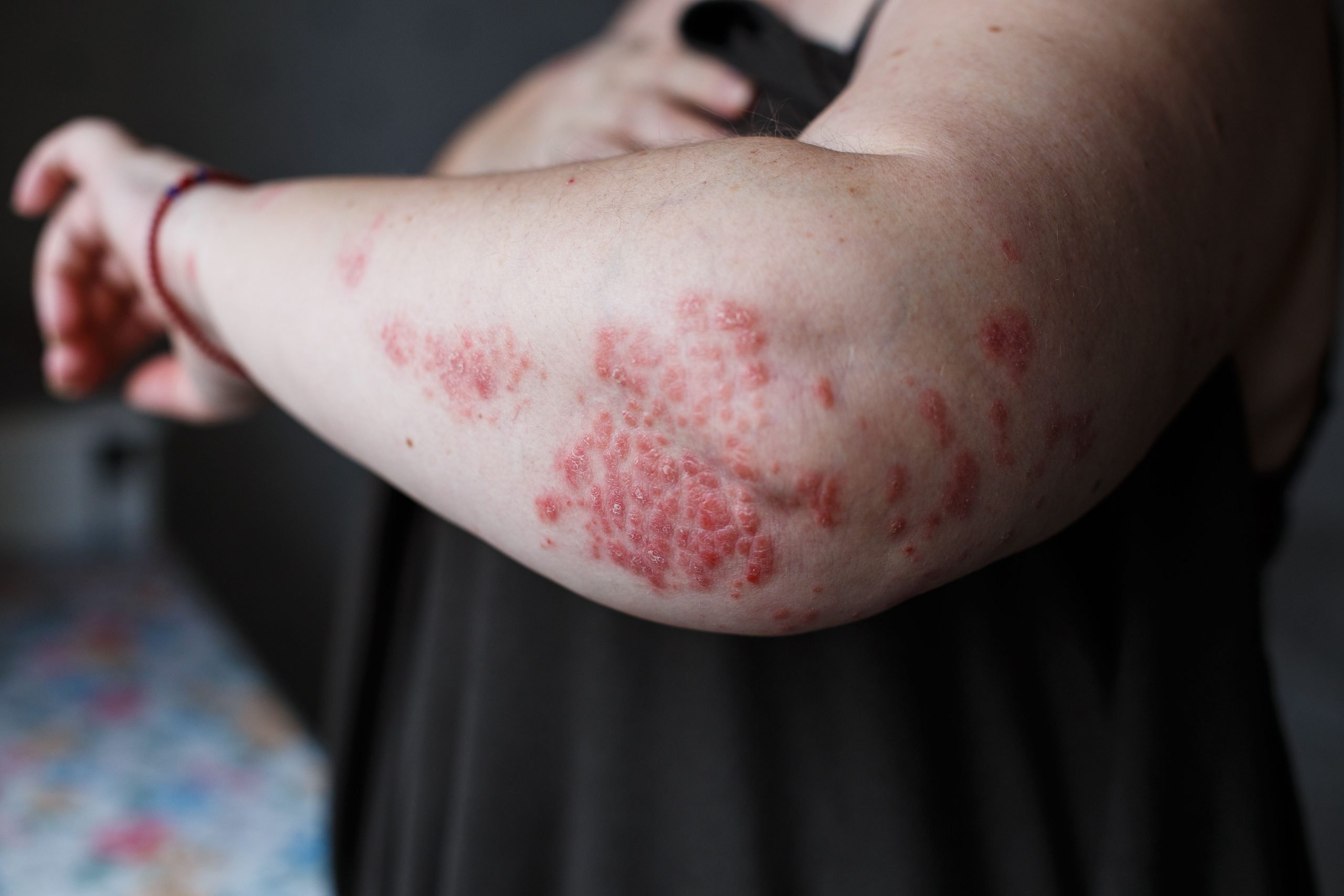
As a world leader in the treatment of psoriasis, our Department of Dermatology understands the importance of research in pustular psoriasis and is committed to developing safe and effective therapies for this condition.
Mount Sinai specialists are skilled in customizing the right treatment plan based on the type of pustular psoriasis you have, as well as factors such as the severity of your symptoms, age, and other medical conditions. Treatment options include:
- Topicals including corticosteroids and non-steroidal drugs
- Biologics that block the activity of certain cells and proteins in the immune system that play a key role in causing psoriasis
- Oral treatments such as acitretin and cyclosporine
Also Check: Dr Blaine’s Revitaderm Psoriasis Treatment Reviews
Acrodermatitis Continua Of Hallopeau
This type of pustular psoriasis is rare. It causes pus-filled bumps on the fingertips, toes, or both. The disease can also develop underneath the nails.
Often beginning on one finger or toe, new pus-filled bumps may continue to appear. When this happens, new pustules can develop on more than the fingers and toes. In rare cases, the pus-filled bumps can slowly spread up the arms or legs.
Anyone who has pus-filled bumps over much of the skin needs immediate medical care. When widespread, pustular psoriasis can be life-threatening.
The first choice for treating this type of pustular psoriasis often includes the following.
-
Synthetic vitamin D combined with a strong corticosteroid: This combination is applied to the skin.
-
PUVA: This is a type of light treatment that involves taking a medication called psoralen before getting UVA light treatments on the affected skin.
While the above describes what treatment may be used for each type of pustular psoriasis, your treatment plan may include different medications. Your age, other medical conditions , and general health also play key role in determining which treatment is best for you.
ImageGetty Images
ReferencesFitzpatrick JE. Pustular eruptions. In: Fitzpatrick JE and Aeling JL. Dermatology Secrets. Hanley & Belfus, Inc., Philadelphia, 1996:66-7.
Jeon C, Nakamura M, et al. Generalized pustular psoriasis treated with apremilast in a patient with multiple medical comorbidities. JAAD Case Rep. 2017 3: 495-7.
Diet And Pustular Psoriasis
Eating a diet rich in anti-inflammatory foods may help prevent flare-ups and could reduce your possibility of developing related health conditions like psoriatic arthritis or heart disease.
Although theres little research on diets that may specifically affect pustular psoriasis, the following foods and supplements are recommended for helping to prevent psoriasis flare-ups in general:
- vegetables like broccoli, cauliflower, and leafy greens like kale and spinach
- berries, cherries, grapes, and other dark fruits
- fatty fish, including salmon, sardines, and trout
- fish oil supplements (an older
The appearance of your skin may cause feelings of anxiety, but the outlook for pustular psoriasis is good if you receive treatment.
Treatment can improve and eventually clear the skin. Your outlook will depend on:
- the type of pustular psoriasis you have
- the frequency of your flare-ups
- your reaction to treatment
- your overall health
Children who dont develop secondary infection have a good outlook. In older adults, especially those with von Zumbusch pustular psoriasis, aggressive treatment is necessary to prevent serious complications. Treatment will also help reduce your risk of a flare-up.
Its important to take steps to avoid triggers. These steps include:
- avoiding environmental factors
Don’t Miss: How To Reduce Redness In Psoriasis
Conditions Associated With Palmoplantar Pustulosis
Certain conditions have been reported to occur in patients with palmopustular pustulosis more often than in unaffected patients.
- Chronic plaquepsoriasis
- Autoimmune diseases particularly gluten sensitive enteropathy , thyroid disease and type 1 diabetes.
- Streptococcal tonsillitis.
- Rarely, synovitisacnepustulosishyperostosisosteomyelitis syndrome.
Palmoplantar pustulosis may rarely be provoked by the tumournecrosis factor -alpha inhibitors .
Symptoms Of Pustular Psoriasis
There are various forms of pustular psoriasis, based on the location of symptoms. The different types are:
- General pustular psoriasis , which covers large areas and can involve chills, fever, heart rate changes, and fatigue. GPP can occur in episodes and be life-threatening without treatment.
- Localized pustular psoriasis, which commonly affects the feet and/or hands
- Acropustulosis, which affects only the tips of toes and/or fingers
Don’t Miss: Salicylic Acid Products For Psoriasis
Doctor’s Notes On Pustular Psoriasis
Pustular psoriasis is a rare form of psoriasis that appears as clearly defined, raised bumps filled with pus . The skin under and around the bumps is red. Pustular psoriasis is classified into one of several types, depending on symptoms. Symptoms may be sudden and severe , long term , or in between . Widespread pustular psoriasis affects large areas of skin and can cause fever.
In the generalized form of pustular psoriasis, symptoms include
- fiery red and tender skin,
- a feeling of general discomfort or uneasiness,
- nausea, along with clusters of pustules.
Pustules tend to appear on the anal and genital areas and the skin folds in the skin. In a day, the pustules coalesce to form “lakes” of pus that dry and peel off in sheets. The skin underneath is a smooth reddish surface, on which new pustules can appear. These episodes may recur for days to weeks causing discomfort and exhaustion. Once the pustules improve, most other symptoms usually disappear.
What Is the Treatment for Pustular Psoriasis?
Treatment for generalized pustular psoriasis in adults includes:
- Oral retinoids
- Infliximab: a biologic, which can decrease inflammation quickly
- Because patients often respond rapidly, some experts believe this may be the first choice when GPP is severe
How Is Psoriasis Diagnosed And Treated
Psoriasis often has a typical appearance that a primary care doctor can recognize, but it can be confused with other skin diseases , so a dermatologist is often the best doctor to diagnose it. The treatment of psoriasis usually depends on how much skin is affected, how bad the disease is , or the location . Treatments range from creams and ointments applied to the affected areas to ultraviolet light therapy to drugs . Many people who have psoriasis also have serious health conditions such as diabetes, heart disease, and depression. Some people with psoriasis also have an inflammatory condition which affects their joints, called psoriatic arthritis.
Psoriatic arthritis has many of the same symptoms as other types of arthritis, so a rheumatologist is often the best doctor to diagnose it. The treatment of psoriatic arthritis usually involves the use of drugs .
Psoriatic disease may be treated with drugs or a combination of drugs and creams or ointments.
Also Check: Psoriasis Treatment Center Of Central New Jersey
How To Get The Right Arthritis Diagnosis
There is no single test for psoriatic arthritis, says Azar. Along with a physical exam, youll likely need a series of both imaging procedures and blood tests for a diagnosis, and to rule out other forms of arthritis, such as rheumatoid arthritis or gout.
Theres no one test to diagnose rheumatoid arthritis either, but, as with PsA, blood tests are part of the workup. The presence of autoantibodies in the bloodstream, either rheumatoid factor or cyclic citrullinated peptide antibodies, will suggest an RA diagnosis. These antibodies tend to be less typical in people with psoriatic arthritis, according to an article published in Rheumatic and Musculoskeletal Diseases in August 2018.
As part of the physical exam, the doctor will closely evaluate the affected joints. RA involves the joints in a symmetrical fashion, and often, when rheumatoid factor is very high, there may be nodules under the skin, Azar says. According to the National Rheumatoid Arthritis Society, 20 percent of patients with RA develop these firm lumps.
Psoriatic arthritis, on the other hand, can reveal itself in a variety of ways, affecting a large joint or a single small finger joint of the hand, says Azar.
Another notable difference between the two diseases is bone involvement. RA is characterized by bone loss or erosion near the joint, while PsA is marked by both bone erosion and new bone formation, Azar says. An X-ray or other imaging method can help reveal whats going on.
What Are The Symptoms Of Psoriasis
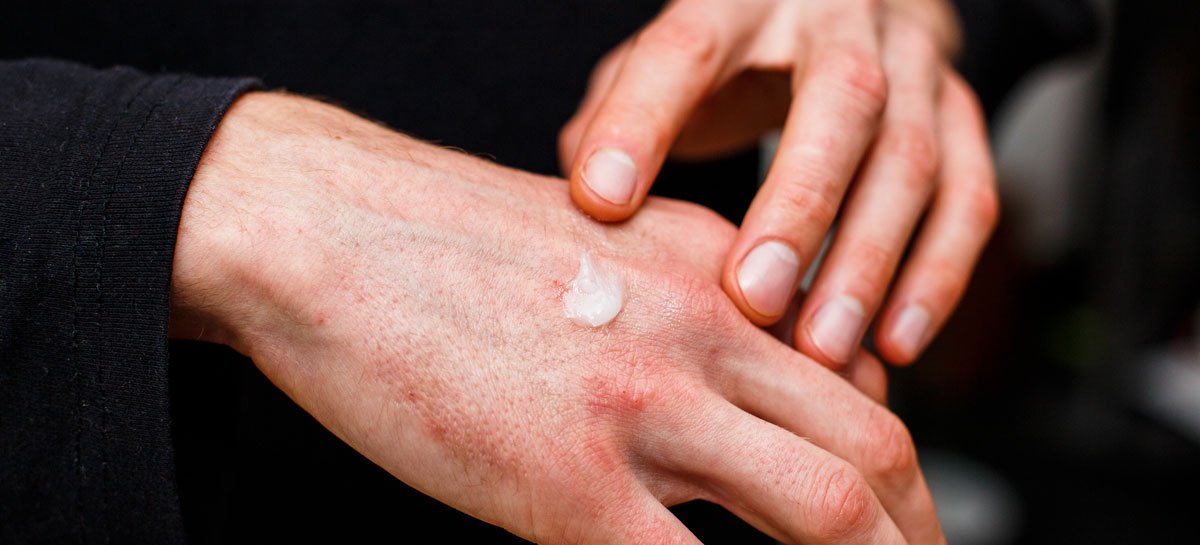
The following are the most common symptoms of psoriasis. Psoriasis comes in several forms and severities. Symptoms may include:
-
Plaque psoriasis. This type of psoriasis is the most common. Symptoms may include patches of red, raised skin on the trunk, arms, legs, knees, elbows, genitals, and scalp. Nails may also thicken, become pitted, and separate from the nail beds.
-
Guttate psoriasis. This type of psoriasis affects mostly children. Symptoms may include many small spots of red, raised skin. A sore throat usually proceeds the onset of this type of psoriasis.
-
Pustular psoriasis. Symptoms may include small pustules all over the body or just on the palms, soles, and other small areas.
The symptoms of psoriasis may look like other skin conditions. Always talk with your healthcare provider for a diagnosis.
Read Also: What Does Psoriasis Look Like On A Black Person
Systemic Implications And Complications
There are several comorbidities and associated systemic disorders that have been demonstrated to be associated with psoriasis. In addition, erythrodermic and pustular psoriasis also carry morbidity when acute and severe in presentation.
Erythrodermic and pustular psoriasis
High-output congestive heart failure may occur with erythrodermic psoriasis in the setting of acute onset and systemic manifestations such as fever, chills, and malaise. These patients also are at increased risk of superinfection and subsequent sepsis, especially from Staphylococcus aureus. Fluid and electrolye imbalance and peripheral edema from negative nitrogen balance through protein loss because of skin exfoliation also can occur and should be treated. Patients with pustular disease also should be evaluated for hypocalcemia, as this may occur. Other potential complications include deep venous thrombosis andpulmonary embolism caused by inmobility.
For psoriasis in general:
Psoriatic arthritis
Obesity/metabolic syndrome
Cardiovascular disease
All patients should be counseled that they are increased risk for cardiovascular disease and they should be advised to promote heart healthy behaviors. In fact, some academic centers have established multidisciplinary centers where patients can be evaluated and more extensively counseled for behavior modification and close monitoring for the development of cardiovascular disease.
Autoimmune diseases:
Psychiatric Illness
Personal behaviors
There Are Several Types Of Pustular Psoriasis And They Are All Treatable
Pustular psoriasis is a type of psoriasis there are several types of pustular psoriasis including Von Zumbusch, palmoplantar, and acropustulosis.
Psoriasis is called an autoimmune disease because it occurs when T-cells that usually fight viruses and bacteria in the body attack healthy cells instead. The T-cells also join with neutrophils to accelerate the build-up of the warm, red skin lesions that make up psoriasis. This disease is caused by both genetics and environmental factors.
Pustular psoriasis, usually affects adults, and appears as tiny blisters enclosing pus surrounded by red skin. The pus is not an infection, it is simply a collection of white blood cells. Sometimes pustular psoriasis is limited to the hands and feet, but it sometimes covers the whole body. The developmental pattern of pustular psoriasis starts with red skin, then the pustules, and then scaling.
A combination approach is often used by dermatologists to help manage pustular psoriasis. For generalized pustular psoriasis, some dermatologists prefer using acitretin and methotrexate, either combined or separately, as they can cause pustular psoriasis to go into remission. Phototherapy is also used.
Palmoplantar pustulosis is a psoriasis that occurs on the palms of the hand and soles of the feet. The pustules appear on red plaques of skin that soon turn brown and crust over. Treatment includes topical creams, phototherapy, or acitretin, methotrexate, or cyclosporine.
You Might Also Enjoy…
- 4.94/5
You May Like: How To Cure Psoriasis At Home
Pustular Psoriasis Of Pregnancy
Pustular psoriasis of pregnancy, also called impetigo herpetiformis, is a very rare variant. It can be life threatening for the mother and fetus if its not treated.
Pustular psoriasis of pregnancy most often appears early in the third trimester. It can reappear in future pregnancies, usually at an earlier stage.
Symptoms may include:
- pus-filled bumps on the inner thighs and groin that join together and spread
- pustules in the mouth and under the nails
Although the exact cause is unknown, some possible risk factors may be a family history of psoriasis or a gene mutation triggered by increasing levels of progesterone.
Your treatment will depend on the type of pustular psoriasis you have and how serious it is. Sometimes it takes several tries or a combination of treatments to find the most effective approach.
Your doctor will probably prescribe ointments first because they can soothe your skin and reduce inflammation.
UV light, both natural and artificial, is used to treat psoriasis. PUVA therapy is a combination of UV light and psoralen, an oral medication that makes your skin more sensitive to it. PUVA stands for psoralen plus ultraviolet A.
Your doctor may also prescribe medications like:
- acitretin , an oral retinoid
- cyclosporine
- tumor necrosis factor-alpha blockers like infliximab , adalimumab , and etanercept
- interleukin-12/23 inhibitors like ustekinumab
TNF-alpha blockers and interleukin-12/23 inhibitors belong to a group of powerful drugs known as biologics.
Who Is At Risk For Developing This Disease
Psoriasis has been diagnosed in approximately 2.6% of individuals in the United States, which amounts to approximately 5 million adults with psoriasis. Peak onset of the disease is roughly bimodal, most often at ages 16 to 22 and then ages 57 to 60 however, the disease can occur at any age.
Erythrodermic psoriasis is an uncommon form of psoriasis, affecting 1% to 2.25% of patients with psoriasis and may occur at any age, although it is less common in the pediatric population. Pustular psoriasis is equally rare and has an average age of onset at 50 years however, children ages 6 weeks to 10 years also can rarely be affected.
Risk factors ultimately resulting in the initial presentation of psoriasis or worsening of psoriasis are poorly understood. Koebnerization , preceding streptococcal infection, HIV infection, certain medications , cigarette smoking, alcohol consumption, and emotional stress have been cited to increase risk for developing or exacerbating disease.
Family history also may increase the risk for development of disease. Some families appear to have an autosomal dominant pattern of inheritance with varying penetrance, and studies of twin siblings have demonstrated concordant disease in approximately 65-70% of monozygotic twins and only 20-25% in dizygotic twins. However, the development of psoriasis is multifactorial, resulting from genetic and environmental factors and still poorly understood.
You May Like: Laser Treatment For Scalp Psoriasis