Who Is At Risk For Psoriatic Arthritis
Psoriasis affects 2-3 percent of the population or approximately 7 million people in the U.S. and up to 30% of these people can develop psoriatic arthritis. Psoriatic arthritis occurs most commonly in adults between the ages of 35 and 55 however, it can develop at any age. Psoriatic arthritis affects men and women equally.
It is possible to develop psoriatic arthritis with only a family history of psoriasis and while less common, psoriatic arthritis can occur before psoriasis appears. Children of parents with psoriasis are three times more likely to have psoriasis and are at greater risk for developing psoriatic arthritis. The most typical age of juvenile onset is 9-11 years of age.
What About Vaccines For Shingles
There are two vaccines available to help prevent shingles: Zostavax, a live vaccine, and the newer Shingrix, a nonliving vaccine that was approved by the FDA in 2017.
Shingrix is now preferred over Zostavax. It is recommended for people age 50 and older, including those who have rheumatoid arthritis . Its given in two doses, with two to six months between doses.
According to the CDC, Shingrix may be used for adults who are taking low-dose immunosuppressive therapy, are anticipating immunosuppression, or have recovered from an immunocompromising illness.
Though Shingrix has been shown to be more effective at preventing shingles than Zostavax, some experts question whether its safe for people with inflammatory arthritis. The Shingrix vaccine was studied in HIV patients, cancer patients, and transplantation patients, who all did fine, Elizabeth Kirchner, MSN, CNP, from the Cleveland Clinic told MedPage Today.
But patients with immune-mediated inflammatory diseases such as rheumatoid arthritis, psoriatic arthritis, ankylosing spondylitis, and lupus were all excluded from those trials. The concern: kicking up the immune system in autoimmune patients who already have an overactive immune system, she told MedPage.
Getting the shingles vaccine does not guarantee you wont get the disease its only used as a prevention strategy. You should ask your doctor if Shingrix is safe for you.
Causes Of Psoriatic Arthritis
Almost 1 in 3 people with psoriasis also have psoriatic arthritis.
It tends to develop 5 to 10 years after psoriasis is diagnosed, although some people may have problems with their joints before they notice any skin-related symptoms.
Like psoriasis, psoriatic arthritis is thought to happen as a result of the immune system mistakenly attacking healthy tissue.
But it’s not clear why some people with psoriasis develop psoriatic arthritis and others do not.
You May Like: Best Treatment For Psoriasis Scars
What Can I Do To Help My Feet
The most important action is to seek advice and help when you notice any changes in your foot, whatever they may be. You can talk to your GP or local pharmacist for advice. Some problems can be resolved simply. For issues that are more persistent you may be referred to a specialist, such as a dermatologist, rheumatologist, physiotherapist, surgeon or chiropodist/podiatrist.
For general foot care, personal hygiene is important, particularly in avoiding fungal and viral infections. Change shoes and socks regularly, avoid shoes which are ill-fitting or cause bad posture. If you are overweight, losing weight could relieve the pressure on your joints and improve your walking gait.
If you are diagnosed with psoriasis, develop a treatment regime that works for you often, applying treatment after a bath or shower, along with the use of an emollient, can make the process easier.
If you have nail involvement, keep nails trimmed and clean. If they are thick, try trimming them after soaking them in a bath or shower, as this makes them softer and easier to cut. Alternatively, seek an appointment with a chiropodist, which is often available via the NHS.
If you have psoriatic arthritis, it is important to rest inflamed joints. Sourcing footwear that supports the foot and helps to reduce the pressure on the inflamed areas can help, as can inner soles and orthotic supports. Once again, a chiropodist is best placed to advise you.
This article is adapted from The psoriatic foot leaflet.
Methotrexate Related Adverse Events
The first papers on methotrexate use detailed the acute toxicity associated with high dose therapy for cancer, and later long-term sequelae. Later studies in non-malignant disease showed similar problems with high dose therapy but not so with lower doses, weekly regimens and concomitant use of folic acid. The adverse events associated with methotrexate use can be divided into two broad subsets those symptomatic but rarely life-threatening adverse events experienced by patients, and those rarely symptomatic but potentially life-threatening adverse events which require careful monitoring by physicians.
Methotrexate-induced lung disease is a good example, an entity widely believed to be common, serious and potentially fatal. Incorrectly apportioning blame on methotrexate can result in two potential risks to the patient: denying them an effective drug and delaying the appropriate investigation and treatment of the real cause of their symptoms. Recent studies show this is in fact a rare occurrence and may not exist at all. Furthermore, it appeared that any increased risk was likely due to a small increase in respiratory infections with methotrexate use, rather than interstitial lung disease. This knowledge has the potential to significantly change clinical practice as cessation of methotrexate frequently occurs as a knee jerk reaction to any cough or dyspnoea.
You May Like: Is Humira Good For Arthritis
Recommended Reading: Does Smoking Make Psoriasis Worse
Psoriatic Arthritis And Rheumatoid Arthritis Are Both Chronic Inflammatory Conditions
With both diseases, an overzealous immune system mistakenly attacks healthy cells in your body. That can result in joint pain, stiffness, and swelling, along with perpetual fatigue and other symptoms more specific to either disease.
The causes of psoriatic arthritis and rheumatoid arthritis are still up in the air, but doctors suspect the diseases have an underlying genetic component that may make a person more susceptible to certain environmental triggers.
In any case, psoriatic arthritis and rheumatoid arthritis are both lifelong diseases that can occur in flares . And while theres no cure for either disease, treatments for both psoriatic arthritis and rheumatoid arthritis have come a long way toward keeping symptoms at bay, sometimes even putting the disease into remission. Plus, the right medication can help protect your body from the permanent damage these conditions can cause if left untreated, so its important to work with your doctor to manage your disease.
How Psoriatic Arthritis And Rheumatoid Arthritis Differ
Psoriatic arthritis and rheumatoid arthritis are both autoimmune diseases that affect the joints. Both are inflammatory and progressivecausing joint stiffness, pain, and swelling, as well as persistent fatigue. In addition, both occur in flares and can be treated with medications that suppress the immune system.
However, PsA and RA are different diseasesand the differences are important when it comes to their prognosis and the best approach for managing each condition.
With PsA, the joint symptoms are tightly linked to inflammation of the skin from psoriasis . With RA, the immune system primarily targets joint tissue.
The different underlying disease processes mean that the conditions are diagnosed with different methods and they also require different therapeutic approaches.
You May Like: Can You Get Rid Of Psoriasis Forever
Light Therapy And Other Psa Medications
Light therapy uses medication, followed by exposure to bright light, to treat psoriasis skin rashes.
A few other medications also treat PsA symptoms. These include secukinumab and ustekinumab . These drugs are injected under your skin. Stelara comes with a warning that it can increase your risk for infections and cancer.
There are things you can do at home to help improve your symptoms:
Surgery And The Psoriatic Foot
Orthopaedic surgery to correct deformed joints is only justified in the presence of long-standing deformity where pain is preventing adequate mobility and all alternative medical treatments have failed. The advancement of newer techniques in recent years has seen better results in small joint replacement, but such procedures still need careful consideration and discussion with advice from an appropriate surgeon.
Recommended Reading: Best Over The Counter Scalp Psoriasis Treatment
Symptoms Of Ra And Psa
Both RA and PsA cause joint swelling, stiffness, and pain. Although both conditions affect joints in the fingers and toes, they do it in slightly different ways. And each one can cause other symptoms, too.
Rheumatoid arthritis:
- Often starts in the smaller joints, like the ones in your fingers and toes over time, it may affect other joints, too, like your wrists, knees, hips, and ankles.
- Usually shows up on the same joints on both sides of your body that means it’s symmetric.
- Often makes joints feel stiffer in the morning
- Can lead to fatigue, low-grade fever, and weight loss
Psoriatic arthritis:
- Can affect joints in the back and pelvis in addition to the ones in fingers and toes
- Often affects only one side of your body that means it’s asymmetric.
- Sometimes causes foot pain, especially on the sole of your foot or the back of your heel
- May make your fingers swell up like sausages
- May make your nails pit and flake
- Tends to affect entheses, areas where tendons or ligaments attach to bones
With both conditions, you’ll probably have times when your symptoms get worse. These are called flares. In between these flares are times without symptoms called remissions.
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Don’t Miss: How To Use Olive Oil For Psoriasis
What Is Psoriatic Arthritis
Psoriatic arthritis is a chronic inflammatory disease that attacks both your skin and your joints. About the same number of men and women are diagnosed with psoriatic arthritis. Usually, the first signs of psoriatic arthritis appear between ages 30 and 50, although the disease can strike at any age.
- About 1 in 3 people with psoriasis may develop psoriatic arthritis.
- Joint pain may appear within 10 years after skin symptoms first appear.
- About 85% of people with psoriatic arthritis develop skin symptoms like red, flaky patches known as plaques before they develop joint symptoms.
How PsA differs from other forms of arthritis
Despite sharing multiple characteristics and symptoms, psoriatic arthritis, rheumatoid arthritis, and osteoarthritis arent the same. Its important to not only understand the many types of arthritis, but also how they differ from each other. Talk to a doctor to learn more about the conditions listed below or if you are experiencing symptoms.
|
Psoriatic Arthritis |
||
|
A chronic inflammatory condition attacking the skin and joints |
A chronic inflammatory condition attacking the bodys joints |
Caused over time by wear and tear |
|
Can affect many different joints in the body skin plaques may be present due to psoriasis |
Often targets many joints at one time on both sides of the body |
Usually affects isolated joints |
|
Joints ache and are tender and swollen |
Joints ache and are tender and swollen |
Joints ache and may be tender but have little or no swelling |
How Do Ra And Psa Affect You
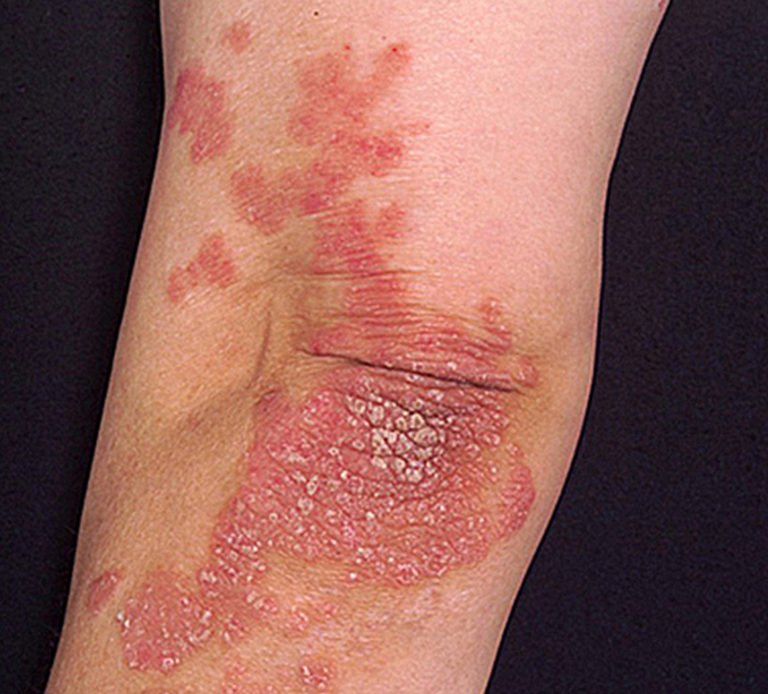
When you have RA, your immune system attacks the lining of the tissues around your joints. They swell up and become painful. Over time, they can become damaged and deformed.
With PsA, your immune system attacks and damages not just your joints, but your skin, as well. It causes your body to make too many skin cells, which leads to psoriasis, a skin condition that often affects people with PsA.
Recommended Reading: Does Guttate Psoriasis Leave Scars
Radiographic Features Of Ra And Psa
Use of imaging can provide important information to help practitioners identify and differentiate between types of inflammatory arthritis. Conventional radiography can be used to identify juxta-articular bony proliferations, which can be used to help discern PsA from other types of inflammatory arthritis, and to visualise osteodestructive lesions characteristic of RA. Other characteristic radiographic changes observed in patients with severe PsA are bone resorption, pencil-in-cup deformities and ankylosis. However, conventional radiographs are not as sensitive as ultrasound or MRI for detection of bone erosions and may not help clinicians detect soft-tissue changes well. Additionally, in our experience, radiologists will often report changes consistent with osteoarthritis in patients with PsA, and it is necessary for rheumatologists to interpret these findings in the proper clinical context.
Ultrasound imaging can be used to identify characteristic features of inflammatory arthritis, including enthesitis, cortical bone erosions, cartilage lesions, synovitis and tenosynovitis. Bone erosions are an important diagnostic criterion of RA that can be identified based on intra-articular discontinuity of the bone surface. Ultrasound evaluations of bone erosions are more reliable for joints that are easily accessible than for carpal or tarsal bones, which cannot be viewed circumferentially.
Does The Severity Of Skin Or Nail Psoriasis Matter
- Nail changes are found in 2 out of 5 individuals with psoriatic arthritis, compared with around half in those with psoriasis alone.
- Nail changes include pitting and discolouration of the nail due to abnormalities in the growth of tissue in the nailbed.
- The risk of developing psoriatic arthritis is greater in individuals with severe psoriasis, yet severe psoriatic arthritis may occur with minimal skin disease.
Also Check: How Are Eczema And Psoriasis Difference
What Causes Psoriatic Arthritis
The cause of psoriatic arthritis is unknown. Researchers suspect that it develops from a combination of genetic and environmental factors. They also think that immune system problems, infection, obesity, and physical trauma play a role in determining who will develop the disease. Psoriasis itself is neither infectious nor contagious.
Recent research has shown that people with psoriatic arthritis have an increased level of tumor necrosis factor in their joints and affected skin areas. These increased levels can overwhelm the immune system, making it unable to control the inflammation associated with psoriatic arthritis.
What’s The Difference Between Psoriatic Arthritis And Rheumatoid Arthritis
RA and PsA are both inflammatory conditions that affect people in the same age group and are often symmetrical, which means symptoms affect the joints on both sides of the body, rheumatologist Vinicius Domingues, MD, medical advisor to CreakyJoints, tells Health. Both conditions are also the result of an overactive immune systemone where your body attacks the joints and causes pain, stiffness, and swelling.
Many symptoms are the same between the two diseasesand treatments often overlap as wellbut the main difference is where those symptoms are located. People with PsA, for example, often have symptoms in the distal joints of their fingers and toes, whereas people with RA suffer in their middle joints. PsA also affects more than just your joints, often attacking your eyes, skin, nails, and tendons.
Recommended Reading: Plaque Psoriasis And Rheumatoid Arthritis
Why Does Having Arthritis Affects Your Shingles Risk
The research is pretty clear: People with rheumatoid arthritis are about twice as likely to develop shingles as otherwise-healthy adults, according to a study published in Arthritis Care & Research. Understanding why, however, is less clear: Experts think its likely due to dysfunction in the immune system when you have inflammatory arthritis, as well as effects from the immune-suppressing medications people take to manage their disease.
Corticosteroids, such as prednisone, are prescribed to relieve acute symptoms of RA and are known to increase the risk of shingles: In one 2015 observational study that analyzed data that from more than 28,800 people with RA, researchers showed corticosteroid use and aging were linked to an increased risk of shingles. Conventional DMARDs like methotrexate were not associated with a higher risk of shingles.
Other research suggests a higher risk of shingles among people who use certain biologic therapies, such as tumor necrosis factor inhibitors, as well the drug tofacitinib, which is part of a new class of drugs for RA called janus kinase inhibitors, or JAK inhibitors.
Add Exercise To Your Daily Routine If You Can
Keeping your joints moving can ease stiffness. Being active for at least 30 minutes per day will also help you lose excess weight and give you more energy. Ask your doctor what type of exercise is safest for your joints.
Biking, walking, swimming, and other water exercises are gentler on the joints than high-impact exercises like running or playing tennis.
Also Check: Hemp Oil For Scalp Psoriasis
What Is Hashimoto’s Thyroiditis
Hashimoto’s thyroiditis is an autoimmune condition where the immune system attacks cells in the thyroid gland. Over time, this can cause chronic inflammation and eventual thyroid failure. Therefore, people with Hashimoto’s often develop hypothyroidism because their thyroid gland cannot produce thyroid hormone, which helps control metabolism.
Often, Hashimoto’s goes undetected until a person develops an underactive thyroid. Therefore, people with this condition develop symptoms of hypothyroidism.
Common symptoms of hypothyroidism include:
- Weight gain
Suppose you or your doctor suspect you have Hashimoto’s. In that case, you should order a complete thyroid panel to check your thyroid hormone levels and TPO antibodies, which help indicate if there is an autoimmune process at play.