How Does Psoriatic Arthritis Affect Your Hands
Psoriatic arthritis is an autoimmune disease, meaning your immune system wrongfully attacks its own healthy tissues. This results in inflammation within your joints, tendons, and ligaments. Its usually asymmetrical, not affecting the same joints on both sides of your body. Psoriatic arthritis symptoms can range in severity, but they typically flare up at times and get better during others.
You may notice the joints in your fingers hurt and are hard to move. They may even be warm to the touch. Simple tasks like turning a doorknob or buttoning a shirt can feel difficult.
Psoriatic arthritis can alter the appearance of your hands. Changes in your nails, such as pitting, discoloration, or crumbling, may be an early sign of psoriatic arthritis. The entire length of your fingers can also become swollen, taking on a sausage-like appearance. This condition, called dactylitis, may be an indication that the disease is progressing.
In rare cases, a complication known as arthritis mutilans can develop. This leads to permanent deformity and an inability to move certain joints, making it hard to use your hands.
Feet Dont Fail Us Nowcheck Out Our Heel
by Health Writer
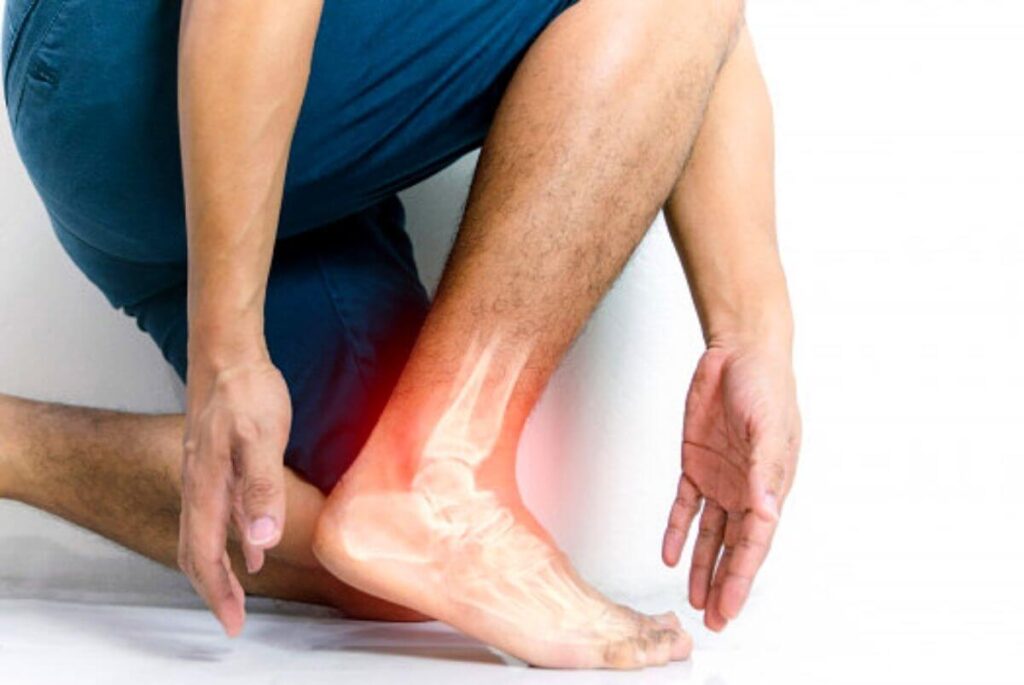
We dont tend to think much about our feet until they start acting upand with a whopping 118 bones and joints between the two of them, there are a lot of ways they can do just that. For those living with psoriatic arthritis , that can spell increased pain, swelling and tenderness. No one really knows why psoriatic arthritis affects the feet so often, but we do know that the disease tends to attack the smaller joints, which makes the feet particularly susceptible, and it also can affect the area where tendons and ligaments attach to the bone, says Doug Tumen, D.P.M., a podiatrist in Woodstock, NY, and author of Ask the Foot Doctor. Podiatrists, in fact, can sometimes even be the first to have a clue that someone might have the disease.
We asked experts how psoriatic arthritis affects your feet, plus their go-to pain-relieving strategies designed to put you back in actionstat.
Causes Of Hand & Foot Psoriasis
Psoriasis is generally believed to be a genetic disease that is triggered by environmental factors where the immune system of the body reacts with the skin cells. The symptoms of hand and foot psoriasis generally worsen in winter, with psychological stress, infections and with certain medications like beta blockers NSAIDs. Dermal injury can also act as a potential trigger for psoriatic skin changes at that very spot. This is known as the Koebner phenomenon. It is characterized by skin cells which multiply up to 10 times quicker than normal. As the underlying cells reach the dermal surface and die, their volume causes elevated red plaques covered with white scales.
Don’t Miss: Treating Scalp Psoriasis And Seborrheic Dermatitis
It Was A Very Humbling Experience
It got to the point that Frances couldnt walk anywhere without terrible pain. She requested a handicap placard because merely walking from her car to the drugstore to pick up a prescription was unbearable. I was just getting by, Frances says of her life back then. She spent most days just trying to get to and from her job at the Federal Communications Commission and get her work done.
She painfully recalls one two-week period where her foot pain was so bad she couldnt get out of bed. I got a Home Depot paint bucket, filled it with ice and water, and was icing my feet in ice water on and off all day for two weeks, Frances says. I had to walk on my tippy toes just to get to the bathroom and the kitchen. That was at its worst.
When she eventually got to another podiatrists office, it was the last straw. Im not a crier, but I broke down and started crying. I said, I cant take this pain anymore, Frances says. The podiatrist acknowledged that she should not be having this much pain with only plantar fasciitis and sent her to a pain management specialist for more testing.
Managing Psoriasis Symptoms Of The Feet

About 10 percent of people are born with genes that could cause psoriasis, but only about 2 percent of people actually get it, Tung says. Some things that could trigger psoriasis include stress and injury. People who have psoriasis of the feet or hands can easily trigger psoriasis symptoms with injury, since these are areas that are constantly used and exposed. Its also important for people with this kind of psoriasis to baby their feet and hands, since cracking of the skin can lead to infection.
Hands and feet psoriasis symptoms include dry, cracked, irritated skin and in the case of palmoplantar pustulosis pus-filled blisters. These psoriasis symptoms are more common in women than men, usually affect only adults, and can interfere with both work and leisure activities.
Recommended Reading: Best Body Soap For Psoriasis
Diagnosing Toenail Psoriasis What To Expect
Toenail psoriasis is often misdiagnosed as a fungal infection under the toenail the symptoms of these conditions are often the same and can be difficult to distinguish, particularly if your doctor does not have a background in dermatology.
Differential diagnosis of toenail psoriasis from toenail fungus is further complicated by the fact that toenail psoriasis can often cause onychomycosis.
One test that is frequently employed to distinguish fungal infections from other skin disorders is the KOH wet mount. This involves taking a specimen from under the nail and examining it under a microscope.
Potassium hydroxide is applied to the sample, which dissolves hair, skin cells, and other debris, leaving behind any fungus that may be present. If the KOH test is inconclusive, your doctor may take a sample of your nail for biopsy.
What Does Psoriasis On The Feet Look And Feel Like
In many cases, psoriasis on the feet presents like psoriasis does elsewhere on the body. The most common type is plaque psoriasis . Psoriasis on the feet may appear with:
- Clearly defined red, purple, or brown patches or lesions on the skin, often covered with thick, silvery scales
- Patches of thick, dry skin that may crack or bleed easily and that may cover the entire sole
- Soreness, burning, or itching, either on a red patch of skin or over much of the foot
- Small patches of skin that are scaly but not necessarily red
- Signs of inflammation, such as heat and redness
- Small pustules on the bottom of the feet
Pain and discomfort from psoriasis on the feet may be worse than pain from psoriasis elsewhere on the body because of the pressure caused by walking. Feet are highly sensitive, which can make basic movements uncomfortable if they are affected by psoriasis. When your feet hurt, even getting out of bed or wearing socks can be painful. Many MyPsoriasisTeam members with psoriasis on their feet report that their feet feel like they are on fire. One member even said, My feet feel like Im walking on knives. Another member shared, My feet are inflamed, red, and painful.
Occasionally, different types of psoriasis will appear on the feet.
Recommended Reading: Is Psoriasis Considered A Disability
Impacts Of Psoriatic Arthritis In The Knees
PsA tends to be asymmetric, meaning different joints on either side of the body are affected . Symptoms in the knees can be mild and develop slowly or arise suddenly and severely. Arthritis usually follows the appearance of psoriasis on the skin. In addition to pain, swelling, and stiffness in the knee joints, PsA can lead to enthesitis and peripheral arthritis.
How Does Psoriasis Impact The Feet
There are a few different ways psoriasis can disrupt your daily life by attacking your feet. If you have psoriasis theres already so much going on with your body, that you may not realize its affecting your feet too. You may think the pain in your feet is from standing too long or normal everyday fatigue.
It could be more severe than you think. Since Ive had these feet for almost 60 years Im thinking Im just getting old and my feet are old too. They hurt more than usual, but Im so used to pain that I just ignore it now.
Recommended Reading: Is Psoriatic Arthritis Related To Psoriasis
Past Research And Achievements In This Area
In 2015, research led by our centre for genetics and genomics at the University of Manchester identified genetic variants associated with psoriatic arthritis, but not with psoriasis or rheumatoid arthritis. This helped to establish psoriatic arthritis as a condition in its own right. The findings could lead to the development of drugs specifically for psoriatic arthritis.
Later in the same year, our TICOPA trial looked at the benefits of early aggressive drug treatment for people with psoriatic arthritis followed by an increase in drug dosage if initial treatment isnt working. The trial found that patients treated this way, required fewer hospital- and community-based services than patients receiving the standard care.
Symptoms Of Psoriasis On The Feet
The most common type of psoriasis is plaque psoriasis with red, dry patches of skin. The patches can appear anywhere on the body, including the feet. Usually, they are covered in silvery scales and can be sore and itchy.
A less common type of psoriasis is palmoplantar pustulosis, affecting the soles of the feet and the palms of the hand. Here you will find tiny, pus-filled blisters.
Its easy to confuse psoriasis with athletes foot, a common foot fungal infection that is very contagious. Athletes foot most often appears between the toes or under the nails, while psoriasis is found on the soles. While athletes foot is itchy, psoriasis on the foot can be painful and sore.
Also Check: Is Neem Good For Psoriasis
Heavy Drinking Can Lead To Seriously Dry Scaly Feet
One side effect of heavy drinking is the development of psoriasis, which is a skin condition that leads to red, scaly patches of skin all over your body. When psoriasis affects a persons feet, simple things like walking can become extremely uncomfortable. Psoriasis can also cause unsightly pits in the toenails. Meanwhile, drinking dehydrates your entire body which can lead to heel fissures as well as flaky, cracked foot skin.
Treatment For Psoriasis On The Feet

If you think that you might have psoriasis on your feet, make an appointment with a podiatrist or a dermatologist. These experts can help determine whether psoriasis or another condition may be causing your dry, flaky, itchy feet. Clinical examination of your skin and possibly a skin biopsy will help confirm the diagnosis.
If psoriasis is determined to be the cause of your symptoms, there are several ways you and your doctor can help alleviate your discomfort. Keep in mind that it may take a while to find the right treatment.
Don’t Miss: Causes Of Psoriasis And Eczema
Getting Started On The Right Foot
Get proper counseling and support to ensure you have success with your treatments. Dont be afraid to reach out to your health officials for assistance with treatments or questions. They can also intercede as advocates for you at your workplace, educating employers about this disease.
This is especially important if your psoriasis on your feet affects your work. Your feet work hard they are always in constant use, which puts a lot of wear and tears on them.
Remember to wear comfortable shoes and soak your feet in warm water each day and moisturize, moisturize, moisturize!!
Distal Interphalangeal Predominant Psa
Distal interphalangeal predominant PsA primarily affects the small joints of the fingers and toes that are closest to the finger and toenails. It affects about 10% of people with PsA.
DIP PsA causes stiffness and pain in the toes, especially in the morning. Stiff and painful toes make to harder to walk and stand for long periods. DIP PsA may also cause nail changes, including detachment, discoloration, crumbling, and pitting .
Read Also: Best Treatment For Psoriasis On Elbows
Bone Erosion In Psoriatic Arthritis And Psoriasis
In one part of the study, the researchers looked at how age affects the level of bone erosion in psoriatic arthritis and psoriasis.
They found that the youngest PsA patients had a similar number of erosions in their dominant hand as did a control group of healthy people without PsA. But psoriatic arthritis patients older than 60 had an average erosion of 2, almost double that of the younger group.
This suggests that age is a key determinant of erosive damage in the joints, according to the study authors.
People with PsA had more erosions than did those with psoriasis . In fact, there werent significant differences in the amount of erosive bone damage in people with psoriasis and healthy controls.
Bone erosions occur as a result of both inflammatory and mechanical damage to bone and joints. People without inflammatory joint disease such as healthy people and those with only psoriasis most likely experience this kind of bone damage from mechanical wear and tear, but in patients with PsA, the additional inflammatory trigger appears to speed up erosions, the researchers told MedPage Today.
In other words, bone erosion appears to be more of an issue for psoriatic arthritis patients than for those with only psoriasis. People with psoriasis dont appear to be at greater risk for bone erosion than the general population.
Home Remedies For Psoriatic Arthritis On Feet
A number of lifestyle changes and home remedies can help lessen pain and other psoriatic arthritis symptoms. These include:
- Wearing supportive shoes when you talk to manage psoriatic arthritis foot pain. Gottlieb recommends talking to your physician for tips about buying shoes that can help with your particular concerns.
- Making time for gentle movement when you are able to. Low-impact exercise can improve flexibility and mobility of the joints while strengthening the muscles. Although walking is the most accessible low-impact activity, biking and swimming may be more doable if you have psoriatic arthritis on your feet.
- Avoiding rigorous high-impact exercise and sports that can exacerbate enthesitis pain.
- Using ice packs on your foot joints can reduce swelling and provide temporary relief.
- Participating in activities you find relaxing may help you reduce stress, which can trigger a psoriatic arthritis flare. Of course, alleviating stress is easier said than done. You may find it helpful to schedule a calendar reminder to practice yoga, meditation, or deep-breathing exercises for just a few minutes each day.
- Elevating your feet to bring down swelling.
- Taking a bath or soaking your feet in warm water and Epsom salts, which can help relax your muscles.
Read Also: Does Heat Make Psoriasis Worse
Pain On The Sole Of Your Foot
The plantar fascia is a thick tissue that runs along the bottom of your foot. It connects the toes to the heel bone, and often becomes inflamed when you have psoriatic arthritis. Its common for people to assume they have only plantar fasciitis, or inflammation of the plantar fascia, when they actually have psoriatic arthritis.
Bright Future For Psoriasis Of The Feet:
- There Is No Cure, But There Are Amazing Treatments.
- They are getting better every year, in fact over the past 10 years research is showing drugs that display a decreased toxicity while achieving better results.
- Combine these systemic medication innovations with topical creams and UV therapy The future is very bright!
You May Like: Psoriasis Treatment Creams Over The Counter
What You Can Do
Before your appointment, you may want to write a list of answers to the following questions:
- What types of symptoms are you having? When did they begin?
- Do you or any of your close family members have psoriasis?
- Has anyone in your immediate family ever had psoriatic arthritis?
- What medications and supplements do you take?
You may want to bring a friend or a family member with you to your appointment. It’s hard to remember everything about a complicated condition, and another person may remember information that you miss.
Medical Options That May Help Include:
- Topical Steroids These are usually used for up to a month at a time. Steroids need to be strong to work on thick palms and soles, so they will need to be prescribed by your dermatologist.
- Topical Ointments Ointments derived from vitamin A and vitamin D can be used to slow down skin cell growth. These are not the same as the vitamins you take by mouth, Tung says. They are strong medications that need to be monitored by your dermatologist.
- Ultraviolet Light Treatment Light therapy slows down skin cell production in psoriasis and knocks out the immune cells causing the inflammation and is the next step in difficult-to-treat cases. Your doctor can prescribe these light treatments two to three times per week, Tung says. In some cases, ultraviolet light can be combined with a topical medication that increases the effect. Oral medication may also be used with light therapy.
- Oral Medication These included Vitamin A derivatives and Otezla . Otezla works on the inflammation without suppressing the immune system throughout the body, says Tung.
- Biologics. These drugs that block the immune system may be suggested if other treatments arent working. These medications are given by injection and are most likely to be needed for patients with more extensive or resistant psoriasis, says Tung. Since hand and foot psoriasis can be disabling, the more aggressive treatment may be warranted even though limited in extent.
Also Check: What To Do For Psoriasis On Elbows
Psoriatic Arthritis Treatment For Feet
There is no cure for psoriatic arthritis but there are medications that help control inflammation and pain. Each of these psoriatic arthritis treatments work differently, and your doctor will make a recommendation based on your particular situation.
Some of the most commonly prescribed medications include:
- Nonsteroidal anti-inflammatory drugs are available over the counter and by prescription to help ease pain and inflammation. These do not prevent psoriatic arthritis from progressing.
- Disease-modifying antirheumatic drugs are available only by prescription. These drugs can prevent psoriatic arthritis from worsening and preserve joint tissue.
- Immunosuppressants target your immune system to prevent it from attacking healthy tissue.
- Biologics are a new form of DMARDs that target the specific part of the immune system triggering inflammation. Sometimes biologics are used in conjunction with another DMARD.
Doctors may also administer corticosteroid injections into the affected foot joints to help with pain, according to Gottlieb.