Metabolic Comorbidities Of Psoriatic Arthritis
Learn more about the connections and risks of metabolic disorders in people with PsA.
More than half of people with psoriatic arthritis have at least one other medical condition . Forty percent of people with PsA have three or more comorbid conditions. Understanding and managing these conditions can help you better control your PsA, help your medications be more effective and improve your overall health.
Common Comorbidities of PsA
The most common comorbidity of PsA is cardiovascular disease . People with PsA also develop metabolic comorbidities, specifically obesity, diabetes, metabolic syndrome and non-alcoholic fatty liver disease. In addition to raising the risk of CVD, these comorbidities can lead to reduced quality of life, high healthcare costs, more complex PsA treatment and early death.
Metabolic Comorbidities
Comorbidity Triggers
Managing Weight and Inflammation
If you are overweight, losing weight will decrease your risk for developing diseases like diabetes, fatty liver disease and cardiovascular disease. It may also make your psoriatic arthritis treatments work better. Because inflammation increases your comorbidity risks, you should work with your rheumatologist and dermatologist to minimize disease activity.
Quick Links
What Are The Symptoms Of Psoriatic Arthritis
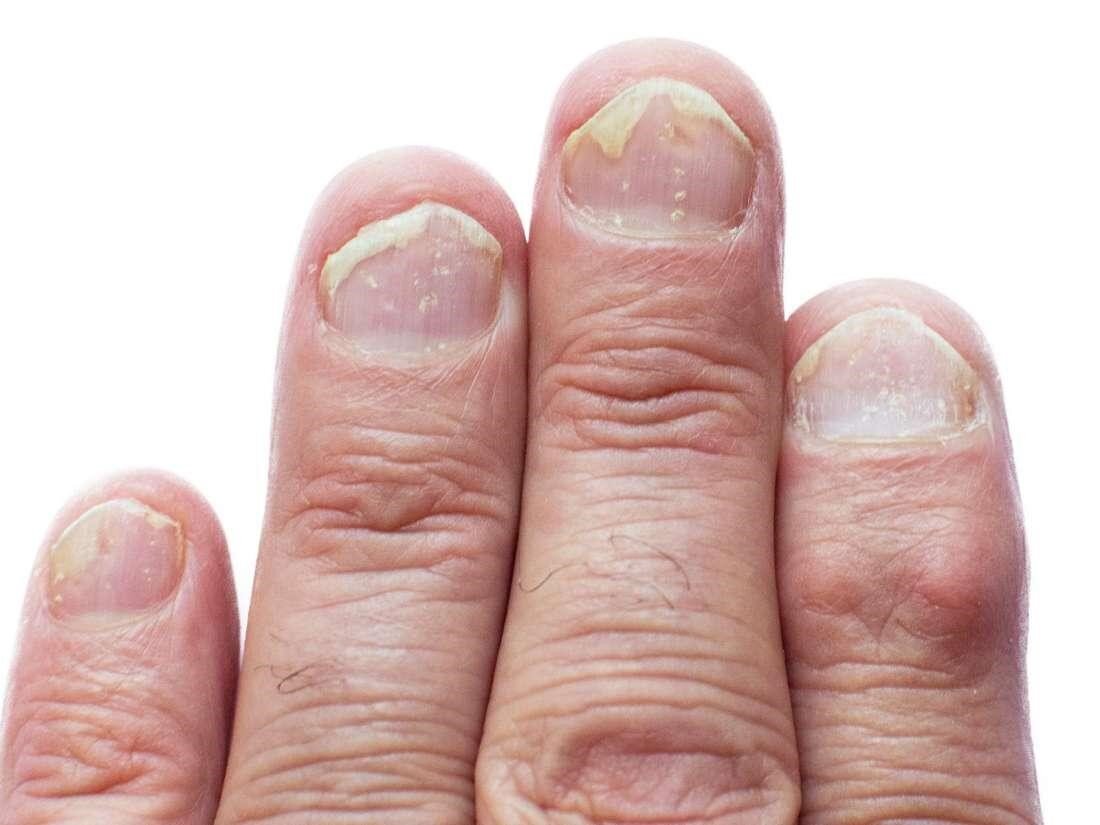
Thepsoriasis symptoms may start before or after the arthritis. Psoriasis causes red, scalyrashes and thick, pitted fingernails. About 3 in 20 to 3 in 10 people with psoriasismay develop psoriatic arthritis. Symptoms of psoriatic arthritis may include:
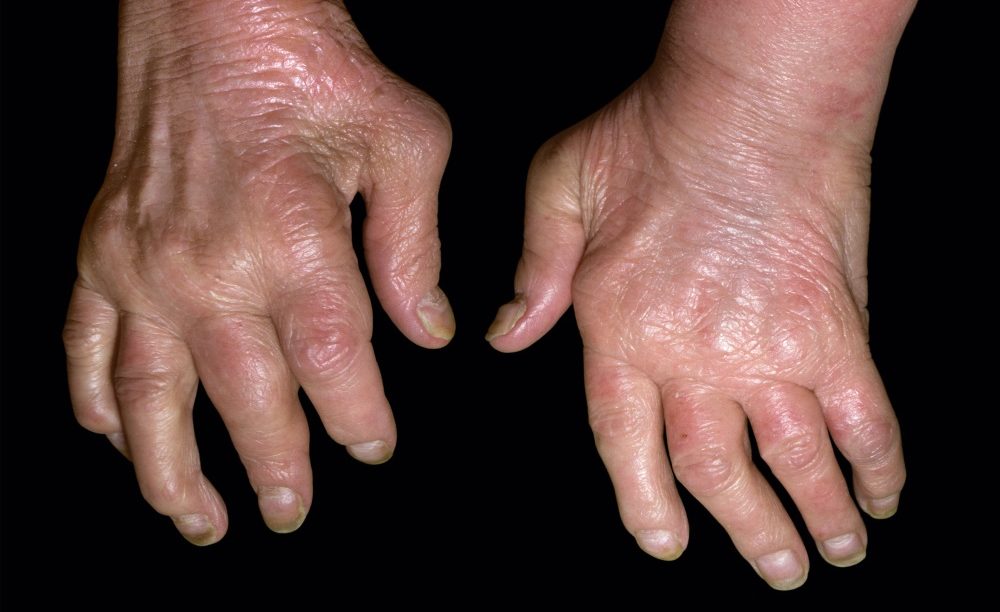
- Inflamed, swollen, and painful joints, often in the fingers and toes
- Deformed joints from chronic inflammation
The symptoms of psoriatic arthritis can look like other health conditions. Make sure to see your healthcare provider for a diagnosis.
Connect With Others Who Understand
MyPsoriasisTeam is the social network for people living with psoriasis and psoriatic arthritis. Here, 87,000 members regularly discuss their experiences with managing their symptoms, finding the right treatments, and living with psoriasis or PsA.
Do you experience PsA symptoms in your elbows? How do you relieve your pain? Join MyPsoriasisTeam today and share your stories with others by leaving a comment below or starting a conversation on your Activities page.
Also Check: Psoriasis On Face And Neck
Studies Selected And Characteristics
The full selection process is shown in Fig. . Overall, 26 articles were finally included, 16 cohort 1) and ten casecontrol studies .
Main characteristics of the 16 cohort studies selected for systematic literature review
| Study, year | |
|---|---|
| Nail dystrophy, type and site of psoriasis | 7 |
| Nail pitting, obesity, smoking, and alcohol habits, family history of PsA | 8 |
| Inflammation and structural damage detected by imaging | 7 |
| Depression, obesity, smoking, and alcohol habits | 8 |
| Inflammation and structural damage detected by imaging | 6 |
| Inflammation and structural damage detected by imaging, musculoskeletal complaints, family history of PsA | 7 |
| Obesity, smoking, and alcohol habits | 8 |
| Nail involvement, inflammation, and structural damage detected by imaging, musculoskeletal complaints | 8 |
CRPD Clinical Practice Research Datalink, DB database, DNPR Danish National Patient Register, NA not available, THIN The Health Improvement Network
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
You May Like: Psoriasis En La Cabeza Tratamiento
Psoriasis And Psoriatic Arthritis: Pathophysiology Therapeutic Intervention And Complementary Medicine
ISBN |
What are VitalSource eBooks?
Routledge & CRC Press eBooks are available through VitalSource. The free VitalSource Bookshelf® application allows you to access to your eBooks whenever and wherever you choose.
- Mobile/eReaders Download the Bookshelf mobile app at VitalSource.com or from the iTunes or Android store to access your eBooks from your mobile device or eReader.
- Offline Computer Download Bookshelf software to your desktop so you can view your eBooks with or without Internet access.
- System requirements for Bookshelf for PC, Mac, IOS and Android etc.»
Most VitalSource eBooks are available in a reflowable EPUB format which allows you to resize text to suit you and enables other accessibility features. Where the content of the eBook requires a specific layout, or contains maths or other special characters, the eBook will be available in PDF format, which cannot be reflowed. For both formats the functionality available will depend on how you access the ebook .
Treatment Of Psoriatic Arthritis
-
Arthritis treated with disease-modifying antirheumatic drugs and biologic agents
Ustekinumab is an interleukin -12 and IL-23 antagonist. The dosage is 45 mg subcutaneously at weeks 0 and 4 followed by 45 mg every 12 weeks thereafter. The dosage is 90 mg subcutaneously if the patient weighs > 100 kg. Adverse effects are similar to those of the other biologic agents Biologic agents Rheumatoid arthritis is a chronic systemic autoimmune disease that primarily involves the joints. RA causes damage mediated by cytokines, chemokines, and metalloproteases. Characteristically… read more .
Secukinumab is an IL-17 inhibitor. Secukinumab can be given at a dosage of 150 mg subcutaneously at weeks 0, 1, 2, 3, and 4 and every 4 weeks thereafter. Without the loading dosage, secukinumab is given at 150 mg subcutaneously every 4 weeks. If patients continue to have active psoriatic arthritis, a dose of 300 mg should be considered. Secukinumab may be given with or without methotrexate. Adverse effects include urticaria, upper respiratory infections, fungal infections due to Candida, diarrhea, herpes zoster, and inflammatory bowel disease.
Read Also: Home Remedies To Cure Psoriasis
Psoriasis Psa And Thyroid Disease
While researchers have studied connections between psoriasis/PsA and other autoimmune diseases, a late 2018 study published in the Journal of the American Academy of Dermatology found that having psoriasis and PsA increases the risk of developing autoimmune Graves disease and Hashimotos thyroiditis. The risk was even greater for patients with PsA.
As with many autoimmune disease issues, researchers havent yet determined the explanation. But they theorize that genetic and immune system irregularities common to both diseases may link psoriasis/PsA and autoimmune thyroid disease.
Based on their findings, the study authors recommended increased physician awareness of the risks. They also advised thyroid screening for patients with psoriasis and PsA, and for those psoriasis/PsA patients who have thyroid symptoms.
Role Of Tnf In Psoriasis And Psoriatic Arthritis
TNF is a key proinflammatory cytokine capable of driving inflammation in a number of different clinical settings. That TNF plays an important role in psoriasis and PsA has been demonstrated in a number of ways. Firstly, the TNF protein and message in skin and synovial tissue has been well documented. Secondly, TNF gene polymorphism analysis also suggests a role for TNF if not in disease initiation quite likely in disease severity. Thirdly, evidence from clinical trials strongly supports a role for TNF inhibition, as a high degree of clinical benefit in both skin and joint disease has been demonstrated.
Also Check: Home Remedies For Itchy Scalp Psoriasis
Physical And Occupational Therapy For Psa In The Elbow
The following types of therapy can help reduce elbow problems caused by PsA.
Physical Therapy
Working with a physical therapist can help you remain active and independent while dealing with your elbow pain. They will assess your movements, address your needs, and even help manage your pain.
Occupational Therapy
An occupational therapist can help you by providing alternative ways of performing various daily activities. Devices such as brushes with a longer handle and zipper aids can make tasks easier when dealing with PsA-related pain.
How To Prevent Psoriasis And Psa Flare
The symptoms of psoriatic disease cant be completely stopped, but they can usually be controlled with treatment.
Identifying what triggers your psoriasis and PsA flares is key to treating the condition. Because PsA is a result of psoriasis, both conditions may be triggered by the same environmental factors.
For some people, stress can be a major trigger for a psoriasis flare. Learning breathing exercises, practicing yoga, and using other coping mechanisms for stress may help stop stressful situations from making your psoriasis symptoms worse.
The biggest lifestyle change that might ease the symptoms of psoriatic disease is diet. Looking at your diet to identify things that trigger your psoriasis symptoms could mean removing some foods as a form of treatment.
Obesity is known to contribute to psoriasis symptoms. Maintaining a healthy diet is essential to being in a healthy weight range. If you can avoid carrying extra pounds, studies indicate that your symptoms will be less severe.
Drinking alcohol and smoking can also trigger flares, so limiting or eliminating these factors entirely can be beneficial.
Don’t Miss: What Does Scalp Psoriasis Look Like
Treatment Options For Both Psoriasis And Psa
Drugs to suppress immune system activity are among the most effective treatments for psoriasis and PsA.
Systemic, immune-suppressing drugs often provide relief for both conditions. However, your risk of secondary infections and other side effects is greater when using these drugs.
If you have severe psoriasis and are diagnosed with PsA, your doctor may prescribe the anti-inflammatory and immune-suppressant drug methotrexate . This medication aims to slow down the cells in your body that are reproducing too quickly and causing psoriasis flares.
Common side effects of methotrexate include:
- headaches
- dizziness
- upset stomach
A newer class of drugs called biologics, in particular TNF blockers, targets specific parts of the immune system more precisely. Because of this, your doctor may be more likely to recommend them over methotrexate.
Biologics reduce inflammation and psoriasis outbreaks in most people who take them. There are a number of brands of biologics approved for treatment of psoriasis in the United States.
Biologics need to be injected. Some need to be administered more often than others. Common side effects include:
- allergic reaction
Data Extraction And Assessment Of The Risk Of Bias
Study characteristics and data were extracted on a standardized form. Information from primary studies was captured through summary of findings tables. The risk of bias and methodological quality of the included studies were assessed with different tools, depending on study design: the NewcastleOttawa scale for observational studies and the ROBIS tool for SLR .
Also Check: Nail Psoriasis Treatment In Ayurveda
Treatment For Psoriatic Arthritis
Treatment for psoriatic arthritis aims to:
- relieve symptoms
- slow the condition’s progression
- improve quality of life
This usually involves trying a number of different medicines, some of which can also treat the psoriasis. If possible, you should take 1 medicine to treat both your psoriasis and psoriatic arthritis.
The main medicines used to treat psoriatic arthritis are:
- non-steroidal anti-inflammatory drugs
- biological therapies
There Are Various Forms Of Psoriasis And Psoriatic Arthritis
There are five types of psoriatic arthritis, and the disease can trigger symptoms in different areas of your body depending on the type you have, according to NYU Langone Health. They are:
- Asymmetric oligoarthritis can cause pain and stiffness in up to five joints on either side of your body.
- Symmetric arthritis is characterized by painful, swollen joints on just one side of your body.
- Spondylitic arthritis When you experience arthritis symptoms in your spine, or you might have neck pain and difficulty moving your head.
- Distal interphalangeal predominant psoriatic arthritis involves inflammation in your fingernails and toenails.
- Arthritis mutilans is a rare but severe form of psoriatic arthritis that causes damage in the bones of your toes and fingers, according to NYU Langone.
The Mayo Clinic explains there are six types of psoriasis, and your symptoms may vary depending on the type you have.
Psoriasis and psoriatic arthritis do share one common symptom: fatigue, which is likely due to high levels of inflammation, according to NYU Langone Health.
Don’t Miss: Selsun Blue Shampoo For Psoriasis
Biological Rationale For Psa Prevention And Interception
It is increasingly clear that there is a close connection between the immunopathogenesis of skin and joint disease in PsO and PsA with both the normal skin and enthesis sharing IL-23/IL-17 axis immunogenetics and innate as well as adaptive IL-23/17 lineage immune cells in healthy tissue. The emergent IL23/IL-17 axis blockers are associated with skin clearance in up to 50% of cases, however, responses in signs and symptoms of PsA are modest, which has been interpreted as a relative lack in depth of response in PsA. However, the clearance of dactylitis, the pathognomonic lesion of PsA, is reported up to 80%90% of cases at 6 and 12 months.This illustrates a closer therapeutic connection between skin and joint than hitherto appreciated as does the similar responses of PsA to IL-17A, IL23 and TNF inhibitor class drugs.
How Is Psoriatic Arthritis Diagnosed
Psoriatic arthritis is easier to confirm if you already have psoriasis. If you donthave the skin symptoms, diagnosis is more difficult. The process starts with a healthhistory and a physical exam. Your healthcare provider will ask about your symptoms. Youmay have blood tests to check the following:
- Erythrocyte sedimentation rate . This test looks at how quickly red blood cells fall to the bottom of a test tube. When swelling and inflammation are present, the bloods proteins clump together and become heavier than normal. They fall and settle faster at the bottom of the test tube. The faster the blood cells fall, the more severe the inflammation.
- Uric acid. High blood uric acid levels can be seen in psoriatic arthritis but are not used for diagnosis or monitoring.
- Imaging. X-rays, CT scans, ultrasound, MRI, and skin biopsies may all be used to help diagnosis.
Recommended Reading: Is Psoriasis Caused By Inflammation
Key Points About Psoriatic Arthritis
- Psoriatic arthritis is a form of arthritis with a skin rash.
- Psoriasis is a chronic skin and nail disease. It causes red, scaly rashes and thick, pitted fingernails. The rash may come before or after the arthritis symptoms.
- Psoriatic arthritis causes inflamed, swollen, and painful joints. It happens most often in the fingers and toes. It can lead to deformed joints.
- Treatment may include medicines, heat and cold, splints, exercise, physical therapy, and surgery.
Psoriatic Arthritis Signs And Symptoms
Early symptoms with psoriatic arthritis are important. People will complain of pain and swelling in their joints hands, feet, wrists, etc. They may have a small patch of psoriasis or have psoriasis covering many areas of the body. There may be complaints of stiffness and fatigue. For example, studies in Toronto showed the year before they were diagnosed, people had reported joint pain, fatigue, and stiffness. Early in the disease, people will often have episodes of worsening of the psoriatic arthritis and then episodes of improvement.
Recommended Reading: Does Vitamin E Oil Help Scalp Psoriasis
Cytokines Metalloproteinases And Cartilage Degradation
In a recent study, we examined the relations between local and systemic markers of inflammation, the levels of cytokines and matrix metalloproteinases in synovial fluid, and markers of cartilage metabolism in early arthritis. We demonstrated high levels of tumour necrosis factor , interleukin -10, and MMPs in the joint fluid of patients with early PsA, confirming a previous study which found increased production of these cytokines in cell cultures from PsA joints. In addition, Fraser et al demonstrated a direct correlation between the levels of TNF, MMP-1, and markers of collagen degradationfurther evidence that collagenase cleavage of cartilage collagen begins early in the disease and probably results from cytokine driven production of proteases.
What Causes Psoriasis And Psoriatic Arthritis
The symptoms of both psoriasis and psoriatic arthritis arise when the bodys immune system malfunctions, leading to inflammation.
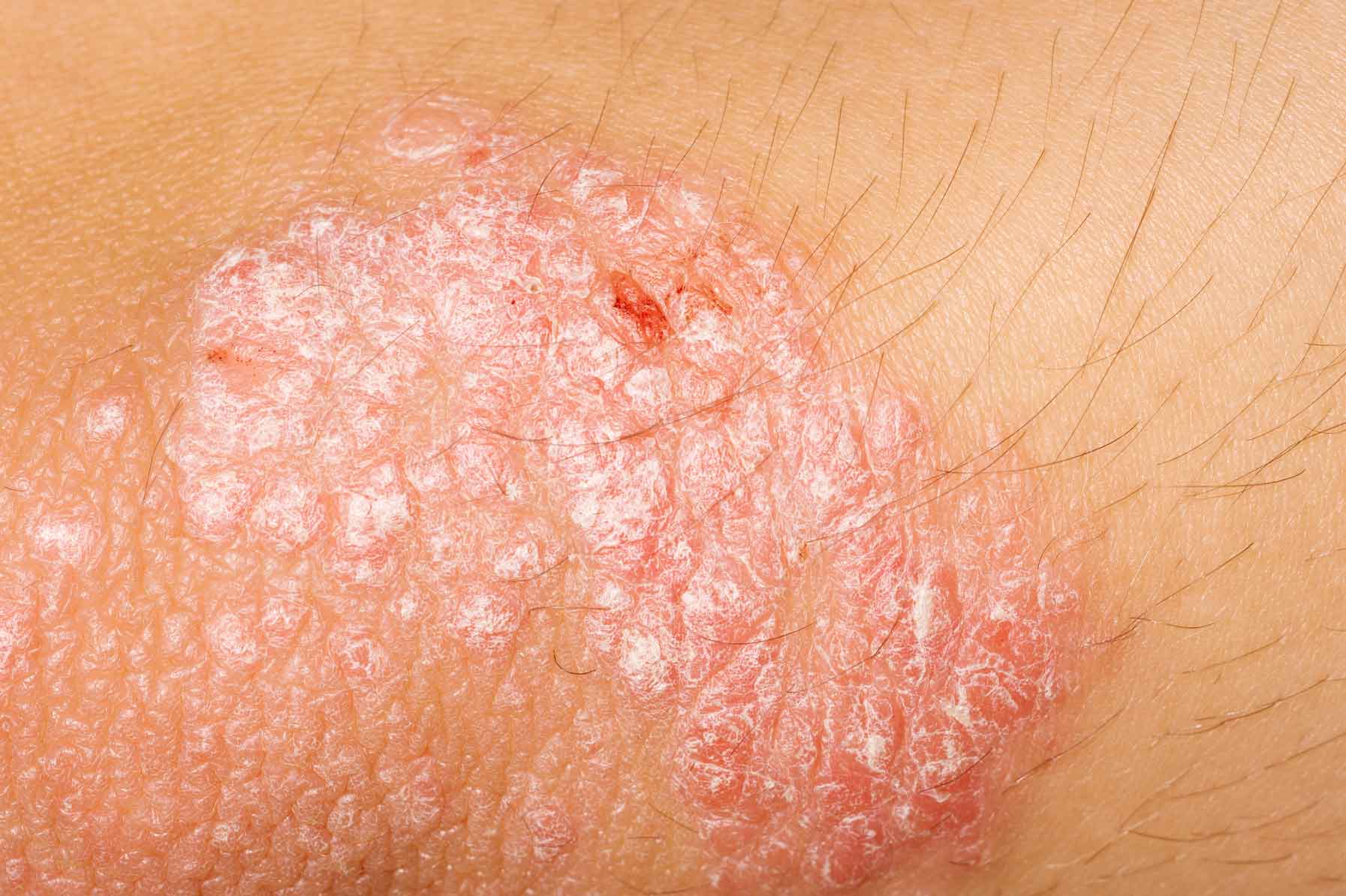
In psoriasis, the faulty reaction causes skin cells to grow too fast, promoting a buildup of skin cells on the surface. These cells appear as a scaly rash.
In psoriatic arthritis, the inflammation affects the joints. Permanent damage can result if the person does not seek treatment.
Doctors do not yet know the exact causes of psoriasis and psoriatic arthritis. However, they do know that genetics contribute to both conditions.
An estimated 1 out of 3 people with psoriasis say that they have a family member with psoriasis. Also, around 40 percent of people with psoriatic arthritis have a family member with psoriatic disease.
Still, many people have genes for psoriatic disease and never develop it. To develop psoriatic disease, a person must have the specific genes for it, as well as a trigger that activates it.
Possible triggers for psoriatic disease include:
- an infection, such as strep throat or a cold
- use of tobacco or smoking
- heavy alcohol use
These triggers may bring on psoriasis, and they can also cause flares. Flares are cycles during which symptoms become worse. Triggers vary from person to person and may change over time.
Psoriasis and psoriatic arthritis symptoms often come and go in cycles. They may get worse during a flare and then improve. Symptoms may also move around, affecting different areas of the body at different times.
Recommended Reading: Home Remedies To Remove Psoriasis Scars