How Is Psoriatic Arthritis Treated
Treatment will depend on your symptoms, age, and general health. It will also depend on the severity of your condition.
Boththe skin condition and the joint inflammation are treated. Early diagnosis andtreatment helps prevent joint damage. Some medicines used to treat psoriatic arthritisinclude:
- Nonsteroidal anti-inflammatory medicines to ease symptoms
- Corticosteroids for inflammation
- Immunosuppressive medicines such as methotrexate to reduce inflammation if NSAIDs donât work
- Biologic medicines to ease inflammation
- Vitamins and minerals such as calcium and vitamin D to slow bone deformation
Other treatment may include:
Psoriatic Arthritis Often Affects People Who Have Psoriasis
Having psoriasis, a disease that often causes inflamed, scaly patches of skin on areas like your knees, elbows, and scalp, puts you at greater risk of getting psoriatic arthritis down the road. The Cleveland Clinic estimates that up to 30% of people with psoriasis get diagnosed with psoriatic arthritis. However, its possible to get psoriatic arthritis even if you dont have psoriasis, and vice versa. Psoriatic arthritis affects people of all genders at relatively equal rates and typically shows up in people between the ages of 30 and 50, says the Cleveland Clinic.
NYU Langone Health explains there are five types of psoriatic arthritis, and depending on which one you have, the disease can show up in very different ways in your body. Around three-quarters of people with the condition have a type called asymmetric oligoarthritis, which impacts up to five joints, though not necessarily the same ones on each side of the body. When the same joints are affected on each side, it may be due to symmetric arthritis, a type of psoriatic arthritis thats similar to rheumatoid arthritis. Theres also spondylitic arthritis, which affects the spine, and distal interphalangeal predominant psoriatic arthritis, which mainly involves the joints near your fingernails and toenails. The rarest form of psoriatic arthritis is arthritis mutilans. Its a severe form of the disease that can destroy the bones in your hands, per the Mayo Clinic.
Treatment Recommendations And Guidelines For Management Of Psa
Table 1 Pro-inflammatory cytokines associated with disease pathogenesis of PsA, RA, and OAFull size table
For patients with an inadequate response to TNFis and other bDMARDs, tsDMARDs are increasingly recommended for patients with PsA and RA . The efficacy of JAK inhibition in PsA has been established for patients with inadequate response or intolerance to csDMARDs and has been reported to significantly improve physical function, psoriasis, enthesitis, and dactylitis related to PsA . Similarly, inhibiting PDE4 has been reported to significantly improve signs and symptoms of PsA and patient-reported outcome measures with sustained response up to 5 years regardless of prior bDMARD experience however, inhibition of radiographic progression is not established with PDE4 inhibition . tsDMARDs effectively improve clinical manifestations, disease activity, and patient-related outcome measures of RA compared with csDMARDs, although greater improvements are achieved when administered in combination with csDMARDs . While efficacy of tsDMARDs has been recognized for both diseases, it is still important to differentiate PsA from RA for the consideration of tsDMARD treatment since some agents have not been thoroughly studied in PsA and may not be as effective as in RA. Although PsA, RA, and OA have various overlapping clinical manifestations, variations in underlying pathogenesis and response to therapy translate into significantly varying clinical outcomes.
Recommended Reading: Psoriasis Vs Eczema On Feet
Does This Patient Have Psoriatic Arthritis
Psoriatic arthritis is an inflammatory arthritis that is characterized by a diversity of clinical manifestations and a highly variable disease course. This disorder was not recognized as a discrete entity until 1964, and it was Moll & Wrights landmark paper in 1973 that outlined the cardinal clinical features followed by familial studies a year later that documented the contribution of genetic factors in disease etiology.
Innovative translational studies and clinical trials over the last fifteen years have uncovered new disease mechanisms and fostered the development and validation of novel therapies, which have been incredibly effective for the varied clinical features of this disease. Recent attention has focused on the extra-articular manifestations and comorbid conditions associated with PsA because they may lessen function and quality of life and increase mortality.
Diagnosis
In the assessment of a patient for possible PsA, it is important to focus on the history and physical examination of the five key domains of this disease, which include integument manifestations of psoriasis, inflammatory peripheral arthritis, spondylitis, enthesitis, and dactylitis.
Psoriasis
Enthesitis
Dactylitis
Some patients may not have psoriasis but will recall a family history of psoriasis or psoriatic arthritis, which is important to document. Other important elements in the history are symptoms of enthesitis .
Recommended Reading: What Does Beginning Psoriasis Look Like
What Causes Psoriasis And Psoriatic Arthritis

While no one knows the exact cause of psoriasis or PsA, experts believe that a faulty immune system is partly to blame. Specifically, the immune system attacks healthy skin cells and joints, causing the inflammation, swelling, and pain characteristic of psoriatic disease.
Genetics plays a part, too: Often will have other family members with psoriatic disease, says Dr. Haberman. In fact, roughly 40 percent of people with PsA have at least one close family member with psoriasis or psoriatic arthritis. Research is still ongoing, however, and its not clear whether having a family history of psoriasis alone increases PsA risk.
Obesity is also a common risk factor for people with psoriasis and PsA. According to a 2019 study in the journal Medicine, roughly 40 percent of people with psoriasis are obese. While it is unknown why obesity is so strongly linked to psoriatic diseases, we do know that obesity is associated with the production of inflammatory chemicals in the body, says Dr. Haberman. It may be that this underlying inflammatory environment helps predispose the body to the development of psoriasis and PsA, she says.
Other risk factors for psoriasis include:
- Family history
- Viral and bacterial infections
- Stress
- Obesity
- Smoking
- Alcohol consumption
Read more here about psoriatic arthritis risk factors.
Read Also: Psoriasis In Ear Natural Treatment
Psoriasis Arthritis Signs And Symptoms
Psoriatic arthritis, or PsA, is a chronic, autoimmune form of arthritis that causes joint inflammation and occurs with the skin condition psoriasis. It can affect large or small joints, and less commonly, the spine. About a third of people with psoriasis develop PsA.
This condition can also cause painful joints, referred to as psoriatic arthritis.
there is no cure for psoriasis. However, treatment can help manage symptoms, and people with psoriasis can.
What are the signs and symptoms of psoriasis? Dry, thick, and raised patches on the skin are the most common sign of psoriasis. These patches are often covered with a silvery-white coating called scale, and they tend to itch. While patches of thickened, dry skin are common, psoriasis can cause many signs and symptoms.
Diagnosis is typically based on the signs and symptoms. No cure for psoriasis is known, but various treatments can help control the symptoms. These treatments include steroid creams, vitamin D 3 cream, ultraviolet light, and immunosuppressive drugs, such as methotrexate. About 75% of skin involvement improves with creams alone.
The 5 most common symptoms of psoriasis include: Rashes or patches of red, inflamed skin , often covered with loose, silver-colored scales in severe cases, the plaques will grow and merge into.
Psoriasis is a common skin.
If a person also develops psoriatic arthritis, certain joints may stiffen, swell, and become painful, and the symptoms may be worse in the morning.
Fingers Toes And Skin
Another telling clue is the presentation of the disease on the fingers and toes. With PsA, the distal joints will be the focus of pain, swelling, and stiffness. By contrast, RA primarily involves the proximal joints .
With severe PsA, the fingers can also take on a sausage-like appearance , making it difficult to ball your fist. While this can occur with RA, it is not the hallmark that it is with PsA.
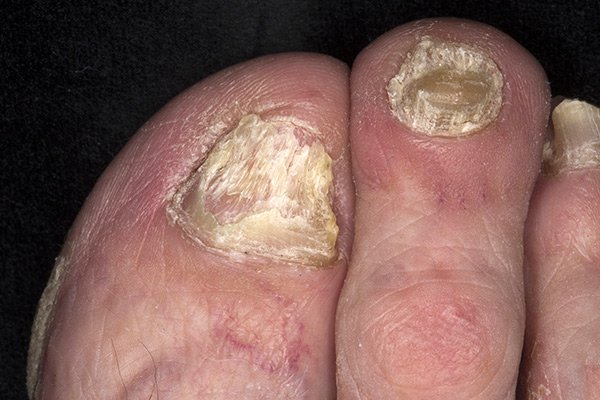
Around 85% of people of PsA with also have the most typical form of psoriasis, characterized by dry, flaky skin plaques. Moreover, half will have nail psoriasis at the time of their diagnosis. Neither of these occurs with RA.
Recommended Reading: What Can I Do For Arthritis In My Hands
Read Also: Red Light Therapy For Psoriasis
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Dont Miss: How To Use Olive Oil For Psoriasis
Psoriasis Treatment Over The Years
One of the earliest treatments for psoriasis was coal tar. Medical professionals may still recommend using coal tar as a first-line treatment in cases of mild plaque psoriasis. And they may recommend it in combination with other medications for cases of moderate or severe plaque psoriasis.
In the 1920s, William Goeckerman developed Goeckerman therapy, which combined UVB light with coal tar to treat psoriasis. Doctors still today for moderate or severe psoriasis.
Throughout the 1900s, experts created several new treatments, such as:
- Corticosteroids: This treatment involves using inflammation-reducing drugs, such as amcinonide.
- Psoralen with ultraviolet A : This therapy consists of taking a light-sensitizing drug, such as methoxsalen , and then exposing the skin to long-wave ultraviolet light.
- Methotrexate and Cyclosporine : These drugs help suppress overactive immune systems.
- Vitamin D3: There is an between low vitamin D levels and psoriasis. D3 is the ingredient in the topical medication calcipotriene .
- Narrowband UVB phototherapy: This therapy is the most common type of for skin conditions.
Biologic drugs are the most recent development in the treatment of psoriasis. These drugs
Read Also: How Do Biologics Work For Psoriasis
Do You Need To Modify Rheumatoid Arthritis Medications Before Or After Getting The Vaccine
Temporarily stopping certain immunosuppressant medications after receiving the vaccine, or timing when you get the vaccine in the course of your treatment, might help increase the effectiveness of the COVID-19 vaccine if you have RA.
But whether this is right for you depends on a number of factors, including which medications you take and your overall health. For example, if your RA is not well-controlled and skipping medications is likely to cause you to flare, your doctor may suggest that you keep taking them. You and your doctor should decide together about making any medication changes. You should not stop taking any of your rheumatoid arthritis medications on your own.
Most disease-modifying antirheumatic drugs, including biologics, should not be stopped for those with rheumatoid arthritis. Here are the RA drugs for which the ACR guidance suggests changes may be recommended:
- Methotrexate: Skip for 1 week after each vaccine dose
- JAK inhibitors : Skip for 1 week after each vaccine dose
- Abatacept , injectable form: Skip one week before and after the first vaccine dose only
- Abatacept , IV form: Get COVID-19 vaccine 4 weeks after your last infusion, then skip a week and get next infusion
- Rituximab : Get COVID-19 vaccine approximately 4 weeks before next infusion, then delay next infusion by 2-4 weeks after second vaccine dose if possible
- Cyclophosphamide infusion: Time administration so its one week after each COVID-19 vaccine dose
Health Conditions Linked To Psoriasis
It is important to visit your primary care provider regularly to screen for these diseases because you may not notice or feel symptoms for some of these health conditions. In addition, if some of these conditions are caught early, they can be easily treated with lifestyle changes or medications.
Evidence shows that people who treat their psoriasis effectively can also lower the risk of other comorbidities.
In 2019, the National Psoriasis Foundation and the American Academy of Dermatology published guidelines on the treatment of psoriasis with attention to comorbidities. The guidelines state the following health conditions as comorbidities of psoriasis.
Recommended Reading: Is Coal Tar Good For Psoriasis
Key Points About Psoriatic Arthritis
- Psoriatic arthritis is a form of arthritis with a skin rash.
- Psoriasis is a chronic skin and nail disease. It causes red, scaly rashes and thick, pitted fingernails. The rash may come before or after the arthritis symptoms.
- Psoriatic arthritis causes inflamed, swollen, and painful joints. It happens most often in the fingers and toes. It can lead to deformed joints.
- Treatment may include medicines, heat and cold, splints, exercise, physical therapy, and surgery.
Psoriasis And Psoriatic Arthritis Treatments Can Make It Easier To Live A Full Life With These Conditions
There are no cures for either disease, but an effective treatment plan can minimize symptoms for both psoriasis and psoriatic arthritis. With psoriasis, doctors generally prescribe treatments that prevent your skin cells from growing too quickly, according to the Mayo Clinic. There are many treatment options for this, including creams, light therapy, or oral or injected medications, the Mayo Clinic explains.
As for psoriatic arthritis, treatments generally focus on controlling inflammation to minimize your joint pain and damage. Your doctor might suggest pharmacological options that target your immune system to lower inflammation, along with exercise or other lifestyle modifications, according to the Mayo Clinic. With each condition, the best treatment depends on your particular situation.
Recommended Reading: What Causes Plaque Psoriasis To Flare Up
Psoriatic Arthritis Treatment Options
Psoriatic arthritis symptoms can be treated with systemic drugs that affect your whole body. Depending on your unique case of psoriatic arthritis, your dermatologist may prescribe methotrexate, cyclosporine or certain biologics. In some cases, steroid injections can reduce inflammation quickly in an affected joint. At Dermatology Associates of Plymouth Meeting, we may team with a board-certified rheumatologist to treat joint disease linked to psoriatic arthritis.
In addition to these medications or treatment options, whether you are experiencing psoriasis or psoriatic arthritis, your dermatologist may recommend lifestyle changes to help minimize symptoms and flare ups. We always encourage changes such as quitting smoking, drinking less and minimizing stressors which can help with psoriasis and psoriatic arthritis flare ups. With psoriasis and psoriatic arthritis, it is common for symptoms to come and go, but it is important to continue taking medication and undergoing treatments recommended by your dermatologist.
If you are struggling to manage your plaque psoriasis or psoriatic arthritis, schedule an appointment today. Our team of board-certified dermatologists are experts in treating all types of psoriasis and can develop a personalized treatment plan based on your unique background and needs.
Recent Posts
Rheumatoid Arthritis Doesnt Have That Psoriasis Link
The Cleveland Clinic reports that women are diagnosed with rheumatoid arthritis at 2.5 times the rate of men. A common misconception about rheumatoid arthritis is that its an elderly persons disease, but the truth is that its often diagnosed between the ages of 20 and 50.While rheumatoid arthritis can affect people in different ways, its signature characteristics include tenderness, pain, and swelling in more than one joint, per the CDC. And although psoriatic arthritis may impact different joints on each side of the body, rheumatoid arthritis usually causes more symmetrical symptoms, says David Wanalista, D.O., rheumatologist at Atlantic General Rheumatology. Its a progressive disease, so it usually worsens with time, starting with the joints between your fingers and toes and in your hands and feet. The inflammation from rheumatoid arthritis can wear down your cartilage, and without that tissue acting as a shock absorber, your bones can eventually erode, which can lead to fusion of the joint.
Also Check: How Long Does It Take For Psoriasis To Clear Up
What You Should Know About Psoriatic Arthritis
Psoriaticarthritis is an autoimmune disease, meaning it occurs when the bodys immune system mistakenly attacks healthy tissue, in this case the joints and skin. The faulty immune response causes inflammation that triggers joint pain, stiffness and swelling. The inflammation can affect the entire body and may lead to permanent joint and
Bottom Line: If Youre Having Joint Pain Or Other Symptoms Of Arthritis Talk To Your Doctor
Its impossible to pinpoint psoriatic arthritis, rheumatoid arthritis, or any of the other dozens of types of arthritis based on symptoms and an online search alone. But some of these diseases can cause serious long-term damage, so talk to your doctor about a diagnosis and treatment options so you can find relief sooner rather than later.Related:
Recommended Reading: What Foods To Avoid If You Have Psoriasis
Psoriatic Arthritis And Psoriasis Are Both Autoimmune Conditions
Both conditions happen when your autoimmune system mistakenly attacks healthy cells in your body, causing inflammation. With psoriasis, new skin cells grow too quickly and build up, resulting in thick, scaly rashes that can make it painful to move, according to the Cleveland Clinic. People with psoriatic arthritis also have inflammation, but their symptoms generally result in stiff, painful joints, and swollen skin surrounding the joints, according to the Mayo Clinic.
The exact causes of autoimmune diseases are not clear. Some experts theorize that injuries might trigger psoriatic arthritis and that infections could trigger psoriasis, according to John Hopkins University. Doctors commonly suspect that genetics may determine whether someone is susceptible to autoimmune disorders, but the specifics explaining how or why are up in the air.
Both conditions are lifelong diseases that can alternate between periods of remission where you have very few symptoms and flares in which your symptoms are worse.