Psoriasis Relief And Treatments
When you need relief from your psoriasis symptoms, topical treatments are typically the most helpful. After a comprehensive exam, Dr. Eckman will provide you with an accurate diagnosis, setting the foundation for your psoriasis treatment plan and helping to determine which medication would work best for you. Topical treatment options may include corticosteroids, tazarotene, or vitamin D. You may also benefit from oral methotrexate, ultraviolet B and psoralen UVA phototherapy, or biologics for patients with moderate to severe psoriasis.
Supplements And Alternative Treatments
The National Psoriasis Foundation suggest some herbs and natural remedies that may help with psoriasis in general.
- Tea tree oil: Always dilute with a carrier, such as almond oil, before applying. Do not take by mouth. Some people may have an allergic reaction.
- Epsom or Dead Sea salts: Add these to lukewarm water to soak the hands or feet.
- Oats: You can add these to a soak or a bath.
- Apple cider vinegar: Apply directly to the skin or dilute in equal parts with water. You can also add it to salads to take it by mouth.
- Capsaicin: Some people find that applying a cream containing the spicy ingredient in chili peppers to the skin may help reduce itching and burning.
- Mahonia Aquifolium: Also known as Oregon grape, applying a 10-percent topical cream may help reduce mild to moderate symptoms of psoriasis.
- Turmeric: Adding this spice to food or taking supplements may help with some types of psoriasis.
Ask a health professional before using any of these, to make sure they are safe and suitable for you to use.
Apply a small amount to a small area of skin to check your reaction, in case you have an allergy or the treatment makes symptoms worse.
Don’t Forget Your Pharmacist
They can be an important part of your team. Your pharmacist can help you create a plan to make sure you can follow your doctor’s instructions safely and easily, no matter how many times your plan changes. They might also be able to suggest over-the counter products that may help your treatment plan work even better.
Lindsey Bordone, MD, assistant professor of dermatology, Columbia University Medical Center.
Latanya Benjamin, MD, associate professor of pediatric dermatology, Florida Atlantic University.
American Academy of Dermatology: “Psoriasis Treatment Can Change During Each Stage of Life,” “Psoriasis: Diagnosis and Treatment,” “What Is A Dermatologist?”
National Psoriasis Foundation: “Addressing the Under-Treatment of Patients with Psoriasis: Results from patient surveys,” “Dermatologist,” “Your health care team,” “Rheumatologist,” “Physical therapy can help you manage PsA pain,” “Shopping for a doc?” “Topical Treatments,” “Your Care Team,” “Life With Psoriasis.”
American College of Physicians: “Psoriasis symptoms can be tough to address.”
Dermatology: “Are Your Patients Satisfied: A Systematic Review of Treatment Satisfaction Measures in Psoriasis.”
American Physical Therapy Association: “Who Are Physical Therapists?”
DermNetNZ: “Psychological effects of psoriasis”
You May Like: Psoriasis Around Eyes Natural Treatment
Youre Planning To Go On A Vacation
The current TSA flying standards prohibit liquids, gels, and aerosols larger than 3.4 ounces in your carry-on luggage. Any liquid must also fit in one quart-sized zip-top bag.
While this restriction isnt disastrous for most people, it can be for those with psoriasis. Topical creams often come in larger sizes, and youll likely want to reapply medicated lotion during the flight because of the aircrafts dry air.
Before traveling, get a letter from your doctor or print out a copy of your prescription to show to any TSA officer. Your creams may still be subjected to further screenings, but you can fly easier by knowing you have everything youll need with you during the flight.
How To Prepare And What To Expect
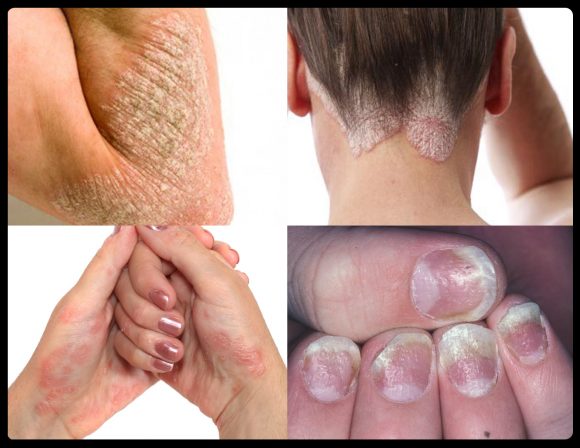 Dr. Health Clinic” alt=”PSORIASIS > Dr. Health Clinic”>
Dr. Health Clinic” alt=”PSORIASIS > Dr. Health Clinic”> A key part of the preparation for a visit with a dermatologist is to track and record all symptoms. Doing this allows for a thorough discussion, which will help the dermatologist create an effective treatment plan.
Symptom tracking is particularly important for psoriasis, which can alternate between flare-ups of varying duration and periods of remission that can last for 112 months.
The person should note:
- Intensity: People can use a scale of 110 to rate the intensity of each symptom.
- Location: The dermatologist will want to know what part of the body each symptom affects.
- Duration: It is important to note how long each symptom lasts.
- Variation: People should record how any symptoms change over time.
Other preparations may include:
- writing the names and dosages of all prescription and over-the-counter medications and dietary supplements
- checking the medical history of family members
- gathering lab results from tests that another doctor has ordered to bring along
- avoiding wearing makeup, moisturizer, and nail polish
A person may also find it helpful to bring a pen and notebook to the consultation to write down instructions or any unfamiliar terms.
The ideal frequency of appointments will vary among individuals. It will depend on several factors, including:
- the severity of the psoriasis
- the frequency of flare-ups
- the development of any other health conditions
Also Check: Steroid Cream For Psoriasis Over The Counter
What Is A Dermatologist
A dermatologist is a doctor who primarily treats conditions related to the skin. This also includes conditions that affect the nails and hair. According to the American Academy of Dermatology , dermatologists work with more than 3,000 related diseases, including psoriasis.
Dermatologists are often the first points of contact for those with PsA. This is especially the case for those who have psoriasis, but havent yet received a diagnosis for the arthritis component. A dermatologist treating a someone with psoriasis might ask about joint pain or stiffness, as these are common indicators of possible PsA.
In treating PsA, a dermatologist may prescribe topical ointments to minimize itchiness and pain as well as prescription medication. Light therapy might also be used in the dermatologists office.
How Often Should You See Your Doctor
It depends on your condition and how long youâve been on your current treatment. At first, your doctor may want to see you every few months. If they put you on a biologic drug, theyâll want to see you more often. You may need to check in every 6-12 weeks. Once your psoriasis is under control, you may only need to go in every 6 months.
You May Like: How Do Doctors Diagnose Psoriasis
Expert Treatment For Patients With Psoriasis
ColumbiaDoctors dermatologists have extensive expertise in the management of all types of psoriasis. Our physicians offer a full range of the many medications and therapies available today. Your dermatologist will work closely with you to develop a comprehensive plan that includes realistic lifestyle changes, diet, therapies, and medications.
The goal of treatment is to slow down the multiplication of skin cells. Your dermatologist may try several approaches before finding the one that works for you, and a treatment that works at one time may stop working later.
What If Those Psoriasis Treatments Dont Work
If psoriasis doesnt improve, your healthcare provider may recommend these treatments:
- Light therapy: UV light at specific wavelengths can decrease skin inflammation and help slow skin cell production.
- PUVA: This treatment combines a medication called psoralen with exposure to a special form of UV light.
- Methotrexate: Providers sometimes recommend this medication for severe cases. It may cause liver disease. If you take it, your provider will monitor you with blood tests. You may need periodic liver biopsies to check your liver health.
- Retinoids: These vitamin A-related drugs can cause side effects, including birth defects.
- Cyclosporine: This medicine can help severe psoriasis. But it may cause high blood pressure and kidney damage.
- Immune therapies: Newer immune therapy medications work by blocking the bodys immune system so it cant jumpstart an autoimmune disease such as psoriasis.
Recommended Reading: Manuka Honey For Plaque Psoriasis
What Are Your Nail Psoriasis Treatment Options
Many people who have psoriasis also experience changes in their fingernails or toenails. But there are treatments that can help.
Nail psoriasis is the term for changes in your fingernails and toenails that occur as a result of having the autoimmune disease psoriasis. According to the National Psoriasis Foundation, up to 55 percent of people with skin psoriasis also have nail psoriasis.
While its not a life-threatening condition, nail psoriasis can affect your quality of life, since it may cause you discomfort and affect your self-esteem. It may also be a clue that youre at greater risk of developing psoriatic arthritis. Although it cannot be cured, nail psoriasis can be helped with treatment.
Psoriasis Comes And Goes And Is Different For Everyone
Psoriasis is a life-long condition that can come and go at any time. Most people with psoriasis will have times when their condition is more severe followed by times when their symptoms are mild or they have none at all .
How severe psoriasis is also varies greatly from one person to another. In Australia and New Zealand, doctors divide psoriasis into two main groups:
This grading is based on a combination of the appearance of the plaques, the area they cover and how psoriasis affects quality of life. Classifying psoriasis like this helps doctors to work out a treatment plan and also to monitor your treatment progress.
Recommended Reading: Can A Dog Get Psoriasis
Oral Or Injected Medications For Psoriasis
When your psoriasis is severe or doesn’t respond to other treatments, your dermatologist may prescribe an oral or injected medication. Some of these medications have serious possible side effects, so your physician will monitor you closely. Biologic medications, which work by altering or suppressing your immune system, have been found to be helpful with psoriasis. These are usually administered by injection.
Home Treatment For Psoriasis
There are some home remedies that may help minimize outbreaks or reduce symptoms of psoriasis:
- Exposure to sunlight.
- Apply moisturizers after bathing to keep skin soft.
- Avoid irritating cosmetics or soaps.
- Do not scratch to the point you cause bleeding or excessive irritation.
- Over-the-counter cortisone creams can reduce itching of mild psoriasis.
A dermatologist may prescribe an ultraviolet B unit and instruct the patient on home use.
You May Like: Is Neem Oil Good For Psoriasis
Recommended Reading: Can A Dermatologist Help With Psoriasis
There Are Several Other Types Of Psoriasis:
Guttate psoriasis causes many small teardrop shaped plaques to appear over the body. It often affects children and young adults and is usually triggered by a virus or strep throat infection. Guttate psoriasis is the second most common type of psoriasis and about 10 per cent of people who have it go on to develop plaque psoriasis.
Inverse psoriasis is where patches of very red skin appear in body folds and where skin rubs together: behind the knees, under the arms and breasts, in the groin, belly button and ears, and between bottom cheeks. The patches are usually smooth and shiny without scales. People with inverse psoriasis often have another type of psoriasis on a different part of their body at the same time.
Palmoplantar psoriasis affects the palms of the hands or the soles of the feet with scaling, redness and sometimes with small pus-containing blisters.
Other rare and serious forms of psoriasis include pustular and erythrodermic psoriasis.
How Is Psoriasis Treated
While there is currently no cure for psoriasis, there are treatments that keep symptoms under control so that you can perform daily activities and sleep better. Your treatment may include:
- Medications you put on your skinsuch as creams, ointments, lotions, foams, or solutionsor others that are injected or taken by mouth.
- where your doctor shines an ultraviolet light on your skin in their office.
Read Also: How Can You Cure Psoriasis
How Do Dermatologists Treat Psoriasis
If you have psoriasis, a dermatologist can create a treatment plan to meet your individual needs. To create this plan, your dermatologist will consider the:
-
Type of psoriasis you have
-
Places psoriasis appears on your body
-
Severity of the psoriasis
-
Impact psoriasis has on your life
-
Other medical conditions you have
Your treatment plan may include medication you apply to your skin, advice to help you care for your skin, and tips to help prevent flare-ups. To control psoriasis, some people also need light treatments or medication that works throughout the body.
You can find out about the different treatments for psoriasis at: Medications and light treatments for psoriasis
Your dermatologist will want to see you for follow-up appointments. These appointments can be very helpful because your dermatologist can:
-
Find out how well the treatment plan is working for you
-
Modify your treatment plan if necessary
-
Watch for signs of psoriatic arthritis, a disease that you want to catch early
-
Assess your risk of developing other diseases that are more common in people with psoriasis
-
Help you set realistic expectations for managing your psoriasis
A dermatologist can also answer questions you have about treating psoriasis. Common questions that patients ask include:
ReferencesBergstrom KG and Kimball AB. 100 questions and answers about psoriasis. Sudbury, MA: Jones and Bartlett Publishers 2005.
All content solely developed by the American Academy of Dermatology
Is Psoriasis The Same As Eczema
Psoriasis and eczema are two different skin conditions. They differ in where the disease appears on the body, how much it itches and how it looks. Eczema tends to appear more often behind the knees and inside the elbows. Eczema also causes more intense itching than psoriasis. Many people, especially children, can get both eczema and psoriasis.
Also Check: Essential Oil Treatment For Psoriasis
What Is A Rheumatologist
A rheumatologist is a doctor who treats conditions related to the bones, joints, and muscles. These often include autoimmune diseases such as gout, lupus, and various forms of arthritis.
Though the precise underlying causes of autoimmune diseases arent fully understood, they are thought to be related to the body attacking its own healthy tissues. Over time, untreated autoimmune diseases can also damage your organs, eyes, and nervous system. The goal of a rheumatologist is to come up with a treatment plan to reduce the damaging inflammation caused by related autoimmune diseases.
Its important to note that while autoimmune diseases, like arthritis, can cause symptoms of the skin, rheumatologists work to treat the underlying inflammation that causes them. This differs from a dermatologist, who can treat the skin problems at the surface level. Rheumatologists use drugs that target inflammation so the body stops attacking healthy tissues. These come in the form of biologics, corticosteroids, and nonsteroidal anti-inflammatory drugs .
What Causes Psoriasis Outbreaks
Psoriasis outbreaks differ from person to person. No one knows exactly what causes flare-ups. Common psoriasis triggers may include:
- Skin injury .
- Streptococcal or other infection that affects the immune system.
- Certain prescription medications .
- Cold weather, when people have less exposure to sunlight and humidity and more to hot, dry indoor air.
Read Also: What Is Biological Treatment For Psoriasis
How Do You Get Rid Of Psoriasis On The Scalp Naturally
Thick scales on your forehead, hairline, behind your ears, or on the back of your neck can be softened with coconut, olive, or peanut oil. Massage a small amount into your scalp, then put on a shower cap overnight, and shampoo in the morning. Repeat for two or three nights. The dead skin should soften and wash away.
What Are Other Types Of Psoriasis
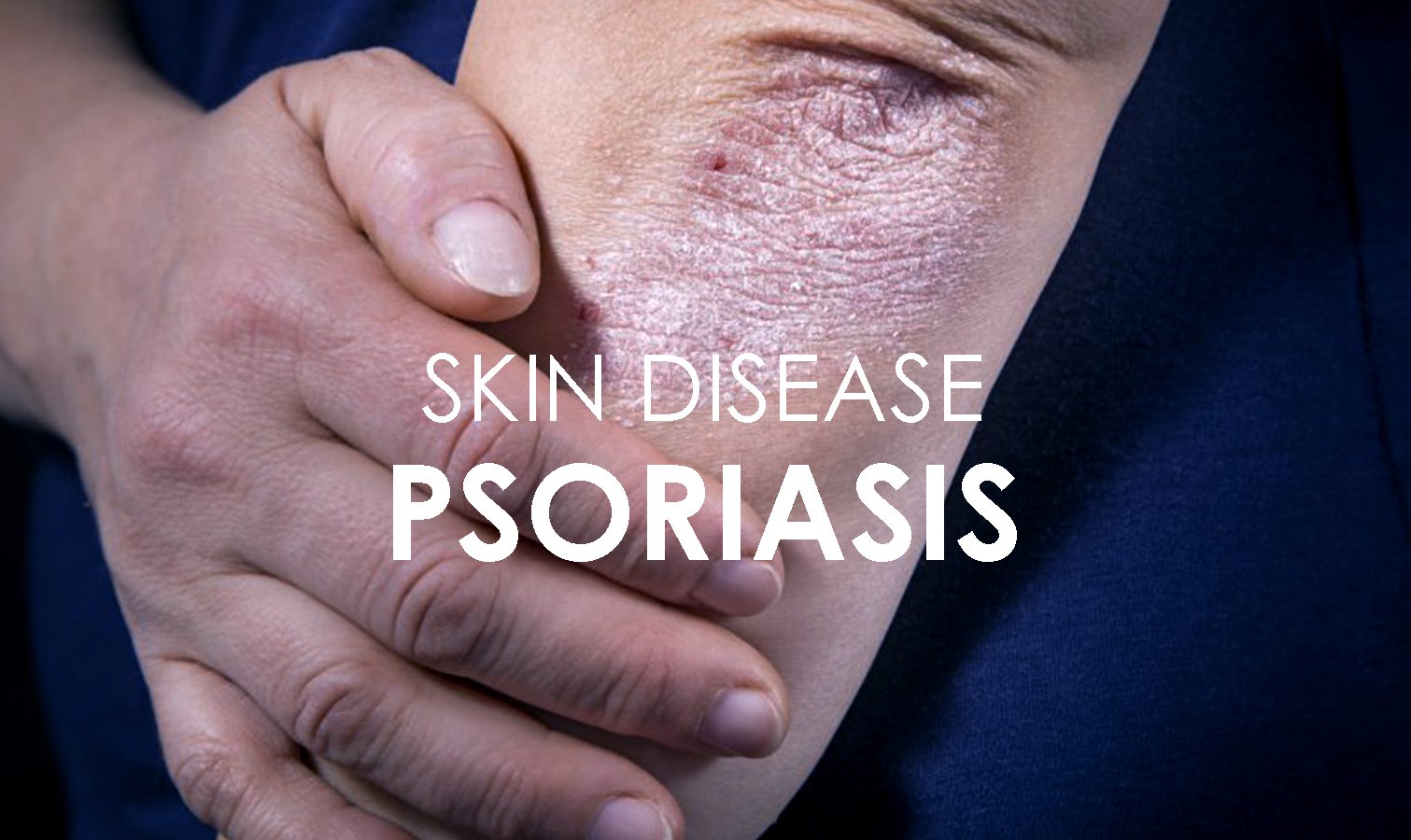
Plaque psoriasis is the most common type. About 80% to 90% of people with psoriasis have plaque psoriasis.
Other, less common types of psoriasis include:
- Inverse psoriasis appears in skin folds. It may look like thin pink plaques without scale.
- Guttate psoriasis may appear after a sore throat caused by a streptococcal infection. It looks like small, red, drop-shaped scaly spots in children and young adults.
- Pustular psoriasis has small, pus-filled bumps on top of the red patches or plaques.
- Sebopsoriasis typically appears on the face and scalp as red bumps and plaques with greasy yellow scale. This type is a cross between psoriasis and seborrheic dermatitis.
You May Like: Best Natural Shampoo For Psoriasis
How Do You Get Rid Of Scalp Psoriasis At Home
When it comes to your scalp, apple cider vinegar can help relieve the itch associated with psoriasis. Try it by saturating your scalp with a mixture of 1 to 2 parts water and 1 part vinegar several times a week for 10 minutes but dont try this at-home treatment if you have cracked or bleeding skin.
Which Specialists Will I Need
That will depend on your situation. For example, if your psoriasis is mild and doesn’t affect your life very much, you may need only your primary doctor. If you have a flare or your symptoms are getting worse, you may want to bring in a dermatologist.
If you start to feel stiffness, pain, or tenderness in your joints, it might be time to add a rheumatologist or a physical therapist to the mix. If your psoriasis starts to take a toll on your mental health, a psychologist or psychiatrist should join the roster.
Your psoriasis doctor can help build your team as you need to expand it. Make sure everyone you see for your psoriasis knows about everyone else, so they can work together to give you the treatment you need.
Don’t Miss: Should I Bandage My Psoriasis
How Do I Decide On A Treatment With My Dermatologist
Your dermatologist will recommend treatments based on:
- The severity of your disease
- Your health history and overall health
- Your experience with previous treatments
Your dermatologist may be guided by the psoriasis treatment targets published by the NPF Medical Board. These targets make achieving clear or almost clear skin the new standard of care for psoriasis.
Your dermatologist may also turn to the six psoriasis treatment guidelines published by NPF and the American Academy of Dermatology in 2019-20. These guidelines give health care providers an up-to-date reference â and give you the information needed to make informed decisions about your care.
Remember, finding the right treatment may take time. Continue to work closely with your dermatologist to ensure you are meeting your treatment goals.
The NPF Patient Navigation Center can help you connect with dermatologists in your area who understand psoriasis and how to treat it.