Medications For Psa In The Shoulder
One of the main goals of treating PsA with medication is to control inflammation. Medication helps to reduce joint pain and prevent joint damage, and it might repair some of the previous damage to the joint.
There are several medications used to treat PsA and manage PsA pain.
Nonsteroidal Anti-Inflammatory Drugs
Nonsteroidal anti-inflammatory drugs can help relieve pain and reduce inflammation caused by PsA. These drugs include over-the-counter medications, like Ibuprofen, as well as other options only available by prescription.
These drugs may not be strong enough to work alone, however. As one MyPsoriasisTeam member wrote, Aleve and Ibuprofen aren’t helping my PsA shoulder pain. Your rheumatologist will work with you to determine whether NSAIDs are right for you and, if they are, which ones will be the most helpful.
Steroid Injections or Oral Steroid Treatments
Steroid injections are sometimes injected directly into the shoulder. They can quickly reduce inflammation and help ease painful joints caused by PsA. They can even keep pain and inflammation away for months at a time.
However, repeated injections into the same joint can cause damage, and the inflammation may be worse after the injection wears off. One MyPsoriasisTeam member explained, Im on day eight of the 10-day Prednisone taper. Yup, my stiff neck and shoulder pain are returning with a vengeance.
Disease-Modifying Antirheumatic Drugs
Who Gets Psoriatic Arthritis
This joint pain affects about 30% of people with psoriasis. It’s common among men and women and can start at any age. But there are a few things that make you more likely to have it.
- If you already have psoriasis, especially lesions on your nails
- If someone in your family has psoriatic arthritis
- If you are between the ages of 30 and 50
Itâs possible to have psoriatic arthritis without the skin condition. Sometimes a viral or bacterial infection can trigger it if your body is already prone to get it.
For those with both conditions, joint pain usually starts about 5 to 12 years after psoriasis symptoms begin.
What Are The Symptoms Of Psoriasis
There are different types of psoriasis. The most common is chronic plaque psoriasis. This causes patches of red, raised skin, with white and silvery flakes.
It can occur anywhere on the skin, but most commonly at the elbows, knees, back, buttocks and scalp.
Psoriasis can cause small round dents in finger and toe nails, this is known as pitting. Nails can also change colour, become thicker and the nail may lift away from your finger.
Don’t Miss: Psoriasis Area Severity Index Pasi
Psa Can Cause Chronic Joint Pain
PsA is a chronic disease characterized by arthritic inflammation of the joints, including dactylitis and enthesis. Enthesitis is inflammation where tendons and ligaments connect to the bone, while dactylitis is inflammation of the small joints of the hands and feet. This inflammation in the hands can make fingers look like sausages, such as Klockow experienced. In addition, PsA can affect the spine, similar to ankylosing spondylitis.
About 30 percent of people with psoriasis will develop PsA. According to the Joint American Academy of Dermatology/National Psoriasis Foundation Guidelines of Care for the Management and Treatment of Psoriasis with Awareness and Attention to Comorbidities: In the vast majority of adult patients, skin manifestation of psoriasis precedes PsA, often by years. Some people develop PsA and never notice or develop psoriasis. Technically, Klockow says, she was never told she has psoriasis.
As a chronic inflammatory disease, PsA is associated with joint pain, says rheumatologist Dafna Gladman, M.D., professor of medicine at University of Toronto and senior scientist at Toronto Western Research Institute in Ontario, Canada. The joint pain from PsA is likely to be chronic unless the inflammation is controlled, Dr. Gladman says.
Classification Of Psoriatic Arthritis
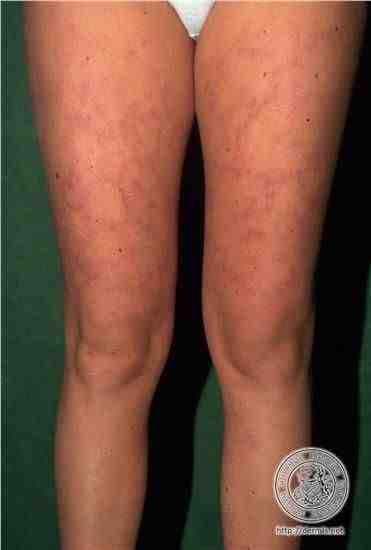
Psoriatic arthritis is a form of spondyloarthritis. Spondyloarthritis is an umbrella term used to describe a family of disorders, including ankylosing spondylitis, non-radiographic axial spondyloarthritis, psoriatic arthritis, reactive arthritis, enteropathic arthritis and undifferentiated spondyloarthritis. These different forms of spondyloarthritis share several clinical features:
- Axial joint inflammation
- Asymmetric oligoarthritis
- Dactylitis: ‘sausage digits’
- Enthesitis: pain and swelling at the insertion of tendons and ligaments, commonly at the heel, tibial tuberosity and humerus this affects up to 53% of patients with psoriatic arthritis
- Negative Rheumatoid Factor
- HLA-B27 positivity: HLA-B27 is a specific protein involved with immune regulation. 57% of psoriatic arthritis patients with axial involvement are positive for HLA-B27
- Geneticsusceptibility to the condition/family history
- Distinctive radiological features.
Also Check: Best Conditioner For Scalp Psoriasis
Take Your Time And Do What Works For You
One MyPsoriasisTeam member shared the importance of taking their time and using treatments that work for them when experiencing pain: I have arthritis in my shoulders, and some days, the pain upon waking and then doing my hair is horrible. I give myself extra time for the Ibuprofen to start working before I get ready for the day.
Hang in there, the member added, and know you are not alone. This site is great that way because most of us understand what you are going through.
Treating Inflammation In Psoriatic Disease
Because the joint damage that psoriatic arthritis causes can be irreversible, identifying and treating it quickly is important. Early treatment can help slow the progression of the disease and prevent permanent joint damage. Today, both dermatologists and rheumatologists are better at identifying psoriatic arthritis, or a persons potential for it, so it can be treated at the earliest opportunity.
The inflammation of psoriatic arthritis can be treated with corticosteroids, methotrexate, and biologic drugs. Nonsteroidal anti-inflammatory drugs , ice packs, cold compresses, and heating pads may also soothe the inflammation of affected joints on a temporary basis.
In a perfect world, a single therapy would help both skin inflammation and arthritic conditions. Its far more likely that your health care providers will use a number of treatment options over time to relieve symptoms and manage psoriatic arthritis. Its important, if you do have both a dermatologist and a rheumatologist, to make sure they are aware of each others prescriptions for you.
Patience is important. Psoriatic arthritis usually doesnt progress rapidly, and most medications that help the symptoms take a few months to fully take effect. Your health care providers will work with you to find the best combination of therapies to treat your condition.
Read Also: What Happens If You Pick Psoriasis
An Itching Or Burning Feeling On The Skin
Although psoriasis patches arent usually irritating, some people do report itchiness. People who have psoriasis of the scalp can report its very itchy or dry, says Anthony Rossi, MD, FAAD, a board-certified dermatologic surgeon at Memorial Sloan Kettering Cancer Center and assistant professor of dermatology at Weill Cornell Medical College.
The itching and pain can interfere with basic daily activities including self-care, sleep, and even walking.
Common Symptoms Of Psoriatic Arthritis May Include:
Sausage-like swelling along the entire length of fingers and toesalso called dactylitisis often a telltale sign of psoriatic arthritis, as opposed to rheumatoid arthritis, in which the swelling is usually confined to a joint. In PsA, it is possible to have swelling in your hands and feet before developing joint symptoms.
Psoriatic arthritis typically affects the ankles, knees, fingers, toes, and lower backand can cause joint damage if not treated appropriately. People with PsA may experience joint pain, swelling, and tenderness in one or more joints, as well as stiffnessparticularly in the morning or after a period of rest.
The skin symptoms of psoriatic arthritis include a rash, thick, red skin, or flaky, silver-white scaly patches, as in plaque psoriasis. The skin may itch and be painful. Up to 85% of people with PsA experience skin problems associated with psoriasis before having psoriatic arthritis symptoms.
Difficulty moving joints and limbs as freely as before is a sign of PsA.
In PsA, joints tend to be stiff and inflexible either first thing in the morning or after a period of rest.
Some people may develop back pain as a result of psoriatic arthritis, including a condition called spondylitis. Spondylitis causes inflammation of the joints between the vertebrae of your spine and in the joints between your spine and pelvis .
Many patients with PsA experience fatigue . Managing the level of inflammation can help lessen fatigue.
Don’t Miss: I Have Psoriasis In My Ears
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
The Effects Of Psoriasis And Psa
The most common form of psoriasis is plaque psoriasis, also known as psoriasis vulgaris. It affects 80 to 90 percent of all people with psoriasis. Its characterized by plaques. These may come and go, even though psoriasis is a chronic, or long-term, disease.
Like psoriasis, PsA is chronic. PsA is also a progressive condition. It gets worse over time. The inflammatory response that PsA triggers in joints can lead to the gradual destruction of joint cartilage and bone.
If left untreated, this process can result in twisted, painful, or swollen joints that no longer function. Joint pain may be widespread or may only occur on one side of your body.
If you have psoriatic disease, youre also at risk for other conditions. This includes:
Recommended Reading: Is Eating Oatmeal Good For Psoriasis
Occurrence In The United States
According to the National Psoriasis Foundation, psoriatic arthritis affects about 1 million people in the United States, or about 30% of all persons with psoriasis. However, prevalence rates vary widely among studies. In one population-based study, less than 10% of patients with psoriasis developed clinically recognized psoriatic arthritis during a 30-year period. A random telephone survey of 27,220 US residents found a 0.25% prevalence rate for psoriatic arthritis in the general population and an 11% prevalence rate in patients with psoriasis. However, the exact frequency of the disorder in patients with psoriasis remains uncertain, with the estimated rate ranging from 5-30%.
Moreover, since the late 20th century, the incidence of psoriatic arthritis appears to have been rising in both men and women. Reasons for the increase are unknown it may be related to a true change in incidence or to a greater overall awareness of the diagnosis by physicians.
Understanding And Managing Skin Pain With Psoriasis
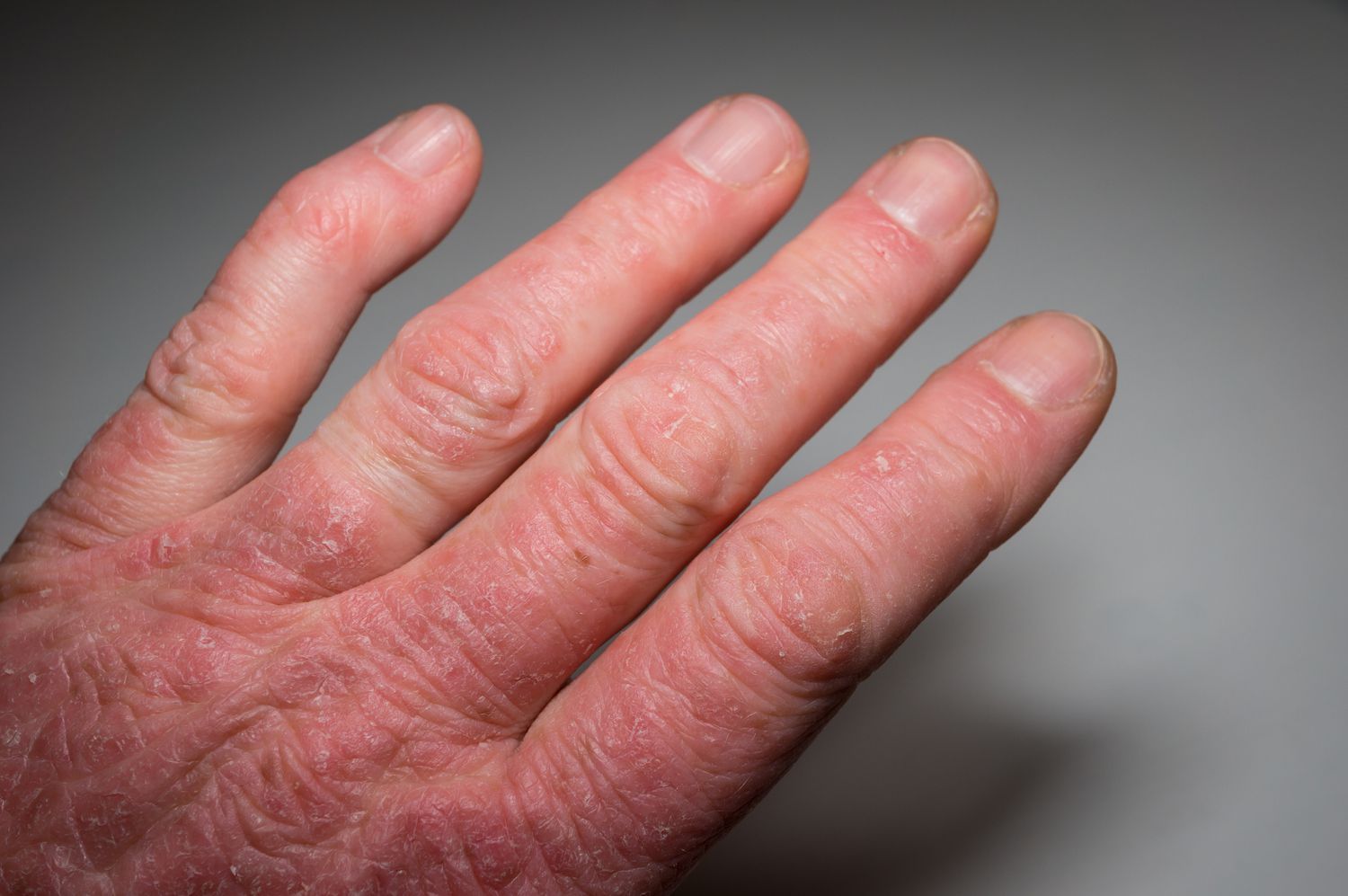
People who have psoriasis pain use words such as, aching, burning, stabbing, throbbing, cramping, stinging, and more to describe skin pain. And when psoriasis flares become painful, you will want relief fast.
Having some remedies on hand can help you to soothe skin when you need relief. Heres what you need to know about skin pain and how to best manage its effects.
Also Check: Are Tanning Beds Good For Psoriasis
Loss Of Significant Joint Mobility
For example, you were able to flex your wrist 60 degrees, and two years later, you lost 50 percent of that range of motion. Its possible to feel okay and still experience loss of range of motion, says Dr. Domingues. But the idea is to prevent joint damage and to make you have less pain. If you have less pain and are still progressing, that means your treatment could be working better.
The Link Between Psoriasis And Psoriatic Arthritis
If you have plaque psoriasis , you might be at greater risk for developing psoriatic arthritis . Psoriasis and psoriatic arthritis are both chronic autoimmune diseases. While plaque psoriasis affects the skin, psoriatic arthritis can cause joint pain and stiffness. Psoriatic arthritis affects up to 25% of patients with plaque psoriasis, but some medical professionals think this number could be closer to 40% in patients with more severe skin lesions.1 In fact, having plaque psoriasis puts you at greater risk for developing psoriatic arthritis later in life.
In most cases, people affected by PsA develop psoriasis of the skin before experiencing any symptoms of PsA. Studies indicate that on average, skin lesions were present for about 12 years before joint issues occurred.2 However, there are some people who experience joint pain and discomfort before or without showing any PsO symptoms.3
You May Like: Psoriasis On Face African American
Psoriasis And Joint Pain
As a chronic autoimmune disorder, psoriasis can impact skin, joints and nails, and symptoms can vary from intermittent to chronic and from mild to debilitating. Symptoms develop as the immune system attacks the body, rather than protecting it from foreign intruders, which leads to inflammation. On the skin, this can manifest as sensitive, red patches and flaky skin.
Although both psoriasis and psoriatic arthritis can cause joint pain, stiffness and swelling, the signs of psoriatic arthritis often resemble those of rheumatoid arthritis. Common psoriatic arthritis symptoms include:
- Swollen fingers and toes which is often a precursor to significant joint symptoms
- Foot pain, particularly at the back of your heel or in the sole of your foot
- Lower back pain called spondylitis which causes inflammation of the joints between your spinal vertebrae and in the joints between your pelvis and spine.
There are several different types of psoriatic arthritis that are identified based on how symptoms are affecting your body. For example, symmetric psoriatic arthritis affects both sides of the body whereas asymmetric psoriatic arthritis only affects one side of the body. There are other types of psoriatic arthritis that are diagnosed based on the location of your inflammation.
How Psoriatic Arthritis Treatment Prevents Disease Progression
The primary way to slow the progression of PsA is through medications that modify the immune system. It may take trial and error to find the treatment that works best for a given patient, notes Dr. Haberman. While we have a lot of medication options for PsA, we dont know which ones a patient will respond to, so sometimes we need to try more than one medication to find the one thats right for that patient, she says.
In addition, medications that have been effective for you can stop working over time. If this happens, your doctor may recommend a medication that works differently say, targets a different part of the immune system to control disease activity.
There are many drugs used to treat PsA. The ones that you will use will depend on the type and severity of symptoms as well as the most problematic areas .
Medications use to treat PsA include:
Recommended Reading: How Do I Get Rid Of Psoriasis On My Nails
Treatment Options For Psoriatic Arthritis
While there is no cure for psoriatic arthritis, there are several treatments available that can help you manage inflammation and joint pain.5 Remember to speak with your healthcare provider before taking any medications, including over-the-counter medicines.
- Nonsteroidal anti-inflammatory drugs can relieve pain and reduce inflammation. These types of medications are usually available over the counter, but stronger NSAIDs are available with a prescription.
- Disease-modifying antirheumatic drugs can slow the progression of psoriatic arthritis and prevent damage to the joints and other tissues affected by psoriatic arthritis.
- Immunosuppressants can help tame your overactive immune system.
- Biologic agents target certain parts of the immune system that trigger inflammation and lead to joint damage.
Crohns Disease And Other Digestive Problems
Symptoms such as abdominal pain and cramping, blood in your stool, and diarrhea could be signs of inflammatory bowel disease. People who have both psoriasis and psoriatic arthritis are at risk for developing Crohns disease in particular, according to the NPF. This is likely because the mutations in the genes of people who have psoriatic arthritis and Crohns disease are similar, or it may be related to side effects from treatment.
If you struggle with digestive issues, be sure to visit your doctor for an evaluation.
Also Check: Best Treatment For Pustular Psoriasis
Can Psoriatic Arthritis Affect Other Parts Of The Body
Having psoriatic arthritis can put you at risk of developing other conditions and complications around the body.
The chances of getting one of these are rare. But its worth knowing about them and talking to your doctor if you have any concerns.
Eyes
Seek urgent medical attention if one or both of your eyes are red and painful, particularly if you have a change in your vision. You could go to your GP, an eye hospital, or your local A& E department.
These symptoms could be caused by a condition called uveitis, which is also known as iritis. It involves inflammation at the front of the eye.
This can permanently damage your eyesight if left untreated.
Other symptoms are:
- blurred or cloudy vision
- sensitivity to light
- not being able to see things at the side of your field of vision known as a loss of peripheral vision
- small shapes moving across your field of vision.
These symptoms can come on suddenly, or gradually over a few days. It can affect one or both eyes. It can be treated effectively with steroids.
Heart
Psoriatic arthritis can put you at a slightly higher risk of having a heart condition. You can reduce your risk by:
- not smoking
- staying at a healthy weight
- exercising regularly
- eating a healthy diet, thats low in fat, sugar and salt
- not drinking too much alcohol.
These positive lifestyle choices can help to improve your arthritis and skin symptoms.
Talk to your doctor if you have any concerns about your heart health.
Crohns disease
Non-alcoholic fatty liver disease