How Will Psoriatic Arthritis Affect Me
Starting the right treatment as soon as possible will give you the best chance of keeping your arthritis under control and minimise damage to your body.
Psoriatic arthritis can vary a great deal between different people. This makes it difficult to offer advice on what you should expect.
It will usually have some effect on your ability to get around and your quality of life, but treatment will reduce the effect it has.
Psoriatic arthritis can cause long-term damage to joints, bones and other tissues in the body, especially if it isnt treated.
Common Psoriatic Arthritis Symptoms Include:
Swollen fingers and toes
Tender, painful, or swollen joints
Reduced range of motion of joints
Morning stiffness
Lower back, upper back, or neck pain
General fatigue
or separationfrom nail bed
If you are experiencing any symptoms of psoriatic arthritis listed above, it’s important to tell your dermatologist or rheumatologist.
Effects On The Immune System
PsA is an autoimmune condition, which means that it influences the way that the immune system works. The immune system fights pathogens, such as bacteria and viruses. In someone with an autoimmune condition, it mistakenly attacks healthy cells.
In a person with PsA, the immune system attacks the joints, tendons, and the insertion points of tendons and ligaments. If a person also has psoriasis, it also affects the skin.
Researchers do not fully understand why this happens. They think that some bacterial infections, including strep throat, may trigger PsA. In addition, if a person has a genetic susceptibility, they may develop PsA as a result of severe stress, a physical injury, or an event that causes the immune system to react strongly.
720% of people with psoriasis develop uveitis, and it is more common in people who have PsA than in those who have psoriasis alone.
Uveitis is a group of diseases related to eye inflammation. Without treatment, it can lead to vision loss. People with PsA should have regular eye exams for this reason.
Don’t Miss: Will A Tanning Bed Help Psoriasis
Treatments For Your Skin
If your psoriasis is affecting your quality of life, or your treatment is not working, you may be referred to a dermatologist.
There are a number of treatment options for psoriasis.
Ointments, creams, and gels that can be applied to the skin include:
- ointments made from a medicine called dithranol
- steroid-based creams and lotions
- vitamin D-like ointments such ascalcipotriol and tacalcitol
- vitamin A-like gels such astazarotene
- salicylic acid
- tar-based ointments.
For more information about the benefits and disadvantages of any of these talk to your GP, dermatologist, or pharmacist.
If the creams and ointments dont help, your doctor may suggest light therapy, also known as phototherapy. This involves being exposed to short spells of strong ultraviolet light in hospital.
Once this treatment has started, youll need to have it regularly and stick to the appointments youve been given, for it to be successful. This treatment is not suitable for people at high risk of skin cancer or for children. For some people, this treatment can make their psoriasis worse.
Retinoid tablets, such as acitretin, are made from substances related to vitamin A. These can be useful if your psoriasis isnt responding to other treatments. However, they can cause dry skin and you may not be able to take them if you have diabetes.
Some DMARDs used for psoriatic arthritis will also help with psoriasis.
Psoriasis Can Affect Internal Organs As Well As The Skin
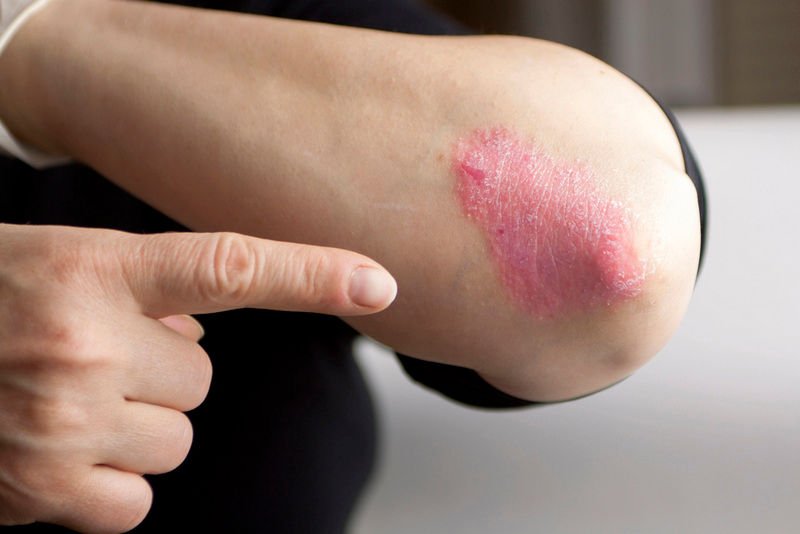
Not only can psoriasis affect the skin, but it can have devastating effects that can affect your internal organs.
The systemic inflammation inside the body that accompanies the disease is often overlooked.
Patients may think that they are having success with their treatments if they cannot see the thick psoriasis plaques on their skin.
However, patients can have serious consequences on their joints, arteries and other organs if not properly treated early to decrease the inflammation.
It is important to know that psoriasis is an autoimmune disease. It is not contagious and is caused when the immune system attacks the skin.
As a result, scaly red patches or plaques occur on the skin.
In addition to skin problems, some patients can develop psoriatic arthritis. Signs and symptoms of this are painful, stiff and swollen joints that can come and go.
Psoriatic arthritis can affect any joint in the body, including the back or neck.
An early and accurate diagnosis of psoriatic arthritis is essential because persistent inflammation can cause damage to the joints.
Nobody knows exactly what causes psoriatic arthritis, but it can affect anyone.
Psoriatic arthritis typically occurs in people with skin psoriasis, but it can occur in people without skin psoriasis, particularly in those who have relatives with psoriasis.
Sometimes certain heart medications like B-blockers can cause a psoriasis flare on the skin or it may be triggered by a streptococcal throat infection.
Read Also: Does Otezla Work For Psoriasis
Points To Remember About Psoriatic Arthritis
- Psoriatic arthritis causes swelling and pain in joints and the places where tendons and ligaments attach to bones.
- Most people who get psoriatic arthritis already have the skin disease psoriasis.
- Although there is no cure for psoriatic arthritis, treatments can slow its progress, lower pain, and protect the joints.
- You can do things at home to help you live with the condition, such as maintain a healthy weight, do low-impact exercise, and avoid smoking.
Work With A Physical Therapist
If youre not sure how to start exercising, or if psoriatic arthritis symptoms have prevented you from exercising, you may want to work with a physical therapist. These specialists are trained to help you strengthen and lengthen your muscles in ways that should help minimize pain and maximize effectiveness. If you have specific areas of your body that often hurt, the therapist may be able to recommend exercises to address that pain.
Many MyPsoriasisTeam members have shared their experiences with physical therapy. One wrote, I’m still going to physical therapy, and it helps me some.
Another said, Physical therapy got me moving, and my stiffness is better.
Recommended Reading: Is Cerave Moisturizing Cream Good For Psoriasis
You Might Avoid Wearing Short Sleeves On A Hot Day If You Have Psoriasis Too
As if psoriatic arthritis wasnt enough, many people who have the condition also have psoriasis, which produces patches of thick, red skin and silvery scales. Even when the temperature is 80 degrees and climbing, sleeveless shirts arent an option for many. My psoriasis is mainly on my elbows, so I would never dream of wearing a sleeveless dress, Dishner says. Three-quarter sleeves are my best friends.
Youre A Serious Germaphobe
You wash your hands religiously, carry sanitizing wipes everywhere, and avoid germ hubs, such as bowling alleys and movie theaters. And with good reason: Anything that can affect your immune system may worsen your symptoms.
Many psoriatic arthritis medications suppress the immune system, leaving you more susceptible to germs, and flare-ups can occur when you get an infection. While vitamins and general attention to hygiene can help ward off sickness, having to skip bowling night with your family to avoid getting sick can still sting even if it does help you avoid a monthlong cold.
You May Like: What To Put On Psoriasis To Stop Itching
Swollen Joints Fingers And Toes
Often you’ll notice swelling in your knees, ankles, feet, and hands. Usually, a few joints are inflamed at a time. They get painful and puffy, and sometimes hot and red. When your fingers or toes are affected, they might take on a sausage shape. Psoriatic arthritis might affect pairs of joints on both sides of your body, like both of your knees, ankles, hips, and elbows.
Never Underestimate A Good Nights Sleep
In Mandelinâs practice, his PsA patients often report chronic pain and fatigue. He finds that while pain and fatigue can present together, they can be separate issues. So he begins at the most basic level. âWhatâs going on metabolically?â he asks. âLetâs get a blood count. Maybe they have anemia. Letâs do an iron study. Maybe they have an iron deficiency.â
Mandelin then moves on to sleep quality. âFrankly, as our population gets heavier and heavier, weâre running across more cases of undiagnosed sleep apnea. Fatigue can amplify your pain,â he says. Sleep apnea, he explains, is one of the components of chronic pain thatâs not involved with PsA. âSuccessfully addressing sleep apnea wonât fix the whole world, but it can at least fix your fatigue. It wonât fix your chronic pain but it helps.â
He is an advocate of sleep studies and the use of CPAP devices he cites the strides in sleep technology over the past few years. âMany face masks donât even look like masks,â he says, though he acknowledges that adapting to these devices may not be easy. âYou have to commit to it, grit your teeth and get through that first month. If you can start getting enough sleep, many things about your health and your overall life will improve.â
Get more advice for better sleep with our Healthy Sleep Guide.
You May Like: Light Therapy For Psoriasis Cost
Psoriatic Arthritis And Back Pain
Learn more about axial arthritis or spondylitis, which causes back pain and may affect your treatment for PsA.
When you think of psoriatic arthritis , you may imagine skin symptoms or the commonly affected joints, like the fingers, knees, ankles or elbows . However, for many people with the disease, back pain can become a symptom as well. When the spine is affected, its known as axial arthritis or spondylitis. Spondylitis affects the spine and sacroiliac joints, which are located at the bottom of the back.
Who Does Spondylitis Affect?
Many people with PsA have axial arthritis and most of them will have a mix of peripheral and axial arthritis. A much smaller number of people with PsA can have inflammation primarily in the axial area without peripheral symptoms.Axial involvement is usually a late-onset feature of PsA, but not always. Studies show that most PsA patients with spondylitis can have back symptoms for up to 10 years before diagnosis is made.Other symptoms of PsA that people with axial disease may have include inflammation where ligaments and tendons insert into bones inflammation of an entire finger or toe skin disease pitting and lifting of nails from the nailbed eye inflammation and inflammatory bowel disease .Since the treatment for PsA with axial involvement may be different than for PsA with only peripheral symptoms, it is important to know the signs and talk to your doctor about your back pain.
Mechanical Pain vs. Inflammatory Back Pain in PsA
What This Means For You
Clauw believes that roughly half of all people who have PsA experience some degree of centralized pain â and for these folks, treating the joints involved with anti-inflammatories, biologics or other therapies might not ease the pain. This is because centralized pain extends beyond the joints.
He speaks candidly in a YouTube video. âOne of the problems we have in pain treatment is that all of our drugs sort of suck,â Clauw says. âTheyâre only modestly effective.â
You can use drugs to manage hypertension, Clauw notes, but not chronic pain. Nonsteroidal anti-inflammatory drugs, for instance, work well for pain from actual injuries, such as a broken leg. They most likely wonât help with pain from the brain.
Clauw doesnât rule out the use of medications for pain. However, he also favors non-drug therapies to help control symptoms, such as exercise, yoga, tai chi, acupuncture, mindfulness, good sleep habits, cognitive behavior therapy and stress reduction.
Don’t Miss: How To Cure Psoriasis Arthritis Naturally
What To Look Forand What To Do About It
by Health Writer
Psoriatic arthritis doesnt always lookor feelthe same. Sometimes, symptoms are gradual and mild others might occur quickly and severely. Worsening joint pain and swelling, or new or worsening psoriatic lesions, are the most common red flags that someone is having a PsA flare, says Yamen Homsi, M.D., the section chief of rheumatology at NYU Langone Hospital in Brooklyn, NY. But there may be other signs that a flare is on the way. Knowing what to look out for is important so you can let your doctor know whats going on and stay one step ahead of a flare.
Treatments For The Arthritis
Non-steroidal anti-inflammatory drugs
NSAIDs, or non-steroidal anti-inflammatory drugs, can reduce pain, but they might not be enough to treat symptoms of psoriatic arthritis for everyone.
Some people find that NSAIDs work well at first but become less effective after afew weeks. If this happens, itmight help to try a different NSAID.
There are about 20 different NSAIDs available, including ibuprofen, etoricoxib, etodolac and naproxen.
Like all drugs, NSAIDs can have side effects. Your doctor will reduce the risk ofthese, by prescribing the lowest effective dose for the shortest possible period of time.
NSAIDs can sometimes cause digestive problems, such as stomach upsets, indigestion or damage to the lining of the stomach. You may also be prescribed a drug called a proton pump inhibitor , such as omeprazole or lansoprazole, to help protect the stomach.
For some people, NSAIDs can increase the risk of heart attacks or strokes. Although this increased risk is small, your doctor will be cautious about prescribing NSAIDs ifthere are other factors that may increase your overall risk, for example, smoking, circulation problems, high blood pressure, high cholesterol, or diabetes.
Some people have found that taking NSAIDs made their psoriasis worse. Tell your doctor if this happens to you.
Steroid treatment
Steroid injections into a joint can reduce pain and swelling, but the effects do wear off after a few months.
Disease-modifying anti-rheumatic drugs
Recommended Reading: What Does Psoriasis And Eczema Look Like
Types Symptoms And Treatment
Like psoriasis and PsA elsewhere on the body, psoriatic disease in the hands and feet can cause itchy, scaling, reddened skin plaques and painful, swollen joints. Specific types and symptoms of hand and foot psoriasis and PsA, however, can also cause less-familiar skin and joint issues.
Palmoplantar psoriasis, plaque psoriasis on the feet or hands, affects about 40 percent of people with plaque psoriasis, who often donât have much skin disease elsewhere. As noted, its substantial effects on function and quality of life mean dermatologists typically use advanced medications to control symptoms. Treating certain types of palmoplantar psoriasis is still challenging, despite the rapidly expanding list of medications for psoriasis and PsA. Often, palmoplantar psoriasis doesnât respond as well to treatment as does psoriasis on other parts of the body.
Most biologics, which work by targeting specific proteins that turn up inflammation in psoriatic disease, such as tumor necrosis factor or interleukin-17 , have some effect on certain people with palmoplantar psoriasis.
No one treatment works for everyone, and people with palmoplantar psoriasis may have to try several medications or combinations of treatments to relieve symptoms. Gary Bixby, for example, didnât get better with either a TNF or an IL-17 inhibitor. The third biologic he tried blocks another interleukin protein, IL-23, and, three months after his first injection, heâs getting better results.
Diagnosing And Treating Psoriatic Arthritis
Having a physical exam is the first step to diagnosing and treating PsA. Your physician will talk with you about ongoing symptoms. Let your physician know if you have a family history of PsA, psoriasis or other autoimmune diseases. Your health care provider will also check for tenderness, swelling, limited movement, and skin or nail changes.
Read More: Aging With Arthritis
There is no cure for PsA. But that doesn’t mean you cant manage the disease and have a healthy, active life. You can work with your health care team to find the best treatment for you.
Treatment varies based on how the disease affects your life, Dr. Jones says. If you have mild symptoms, you may only need treatment during flare-ups. People with severe psoriatic arthritis may need a more aggressive treatment plan to reduce inflammation and improve quality of life.
Don’t Miss: Dr Blaine’s Revitaderm Psoriasis Treatment Ingredients
Swollen Fingers And Toes
They can get so puffy, they look like sausages. Your doctor may call it dactylitis, or sausage digits. This painful swelling happens to more than a third of people with the disease. It results from joint inflammation and usually affects a few fingers and toes. You might mistake it for gout if it shows up only in your toes. Be sure you get the right diagnosis, because gout and PsA have different treatments.
How Does This Condition Affect The Tendons & Ligaments
Enthesitis occurs in up to 50% of people with PsA.4 Symptoms of PsA in the tendons and ligaments include pain and inflammation. When enthesitis affects the heel of the foot, it is known as Achilles tendonitis.
At the bottom of the foot, enthesitis can cause plantar fasciitis. Enthesitis can also occur in the fingers, toes, pelvis, knees or upper body.5,6
PsA can be asymmetrical, occurring on only one side of the body. For example, all the joints in one finger on the left hand may be affected while the same finger on the right hand is unaffected. PsA can also be symmetrical, with the same joints affected on both sides of the body.2
PsA and enthesitis are chronic and can have periods of remission and flares.6
Read Also: Rheumatoid Arthritis Itching Skin
You May Like: How To Control Psoriasis Itching
Heel Pain And Foot Pain
In addition to attacking the joints, psoriatic arthritis also causes pain and tenderness where ligaments and tendons attach to the bones, which are called entheses. The two most commonly affected spots are the Achilles tendon and the plantar fascia, which causes pain at the back of the heel and the sole of the foot.
If You Have Psoriatic Arthritis Youre Well Aware Of The Way The Inflammatory Disease Can Affect Your Skin And Your Joints Stiffness Swelling And Pain In Any Of The Bodys Joints Knees Shoulders Neck
If you have psoriatic arthritis , youre well aware of the way the inflammatory disease can affect your skin and your joints , but you might not know as much about how psoriatic arthritis can damage your bones.
PsA is an autoimmune disease where the bodys immune system attacks both the joints and skin . About 30 percent of people with the skin disease psoriasis also develop psoriatic arthritis.
A new German study published in the journal Arthritis Research & Therapy sought to examine how different kinds of bone damage occur in people with both psoriatic arthritis and psoriasis, to better understand what kind of underlying mechanisms these disease share when it comes to causes of bone damage.
Researchers used a new form of imaging called high-resolution peripheral quantitative computed tomography , which can look at bones in 3D. It allows doctors to see bone density and fragility more accurately than traditional bone scans.
Don’t Miss: Psoriasis In Female Genital Area