How Is Psoriasis Considered An Autoimmune Disease
For much of history, psoriasis has been seen as a disease of the skin. It is now clear that psoriasis is an autoimmune disease that impacts many systems of the body, involving multiple inflammatory pathways, with a primary presentation affecting the skin4. This inflammation can also affect the joints, vascular system, and eyes of people with psoriasis.
Psoriasis is the most common known human autoimmune disease, found in approximately 2-3% of the general population.
Several dozen gene locations have been identified that are believed to be involved in the development of psoriasis3. These genes are known to affect innate immunity, cell signaling processes, and skin barrier function.
These studies also provide more evidence that people with psoriasis may be genetically predisposed to other autoimmune diseases5.
With psoriasis, the body’s immune system goes haywire, sending out faulty signals that speed up the growth of skin. The way psoriasis affects the skin is primarily driven by a type of white blood cell called a T cell, as well as myeloid dendritic cells2. Normally, T cells help protect the body against foreign invaders.
Inflammatory myeloid dendritic cells release specific proteins to activate T cells. These T cells are then put into action by mistake and become so active that they trigger other immune responses, which lead to chronic inflammation and to the rapid turnover of skin cells5.
What Happens During Psoriasis Autoimmune Attacks
In people with psoriasis, the immune system attacks autoantigens on tissues in the skin. These autoantigens include protein products made by the skin cells. Studies have identified the presence of these autoantigens in psoriatic lesions.
Autoantigens are believed to activate T cells and other cells of the immune system. T cells can destroy tissue and produce inflammatory chemicals such as interleukin-17A that promote the abnormal growth of skin cells.
Other immune cells, known as B cells, can also contribute to autoimmunity in psoriasis. B cells produce proteins known as antibodies that can help destroy antigens. In people with psoriasis and psoriatic arthritis , B cells make antibodies against the autoantigens associated with the skin. Antibodies made against autoantigens are referred to as autoantibodies.
Ultimately, the dysfunction and autoimmune activity of the immune system in psoriasis leads to the severe inflammation that contributes to overactive skin cell growth and psoriatic lesions or joint damage. High levels of inflammation from the overactive immune system may also be behind a higher risk for heart disease in people with psoriasis.
Lifestyle Changes Can Help Too
Eating a healthy diet that includes limiting alcohol consumption, quitting smoking, getting regular exercise, maintaining or reaching a normal weight, and managing stress with yoga, meditation or other mindbody practices may also help reduce inflammation and your risk of psoriatic disease comorbidities.
âMany of these comorbid conditions can be reversed by treating psoriasis and making the right lifestyle changes,â says Dr. Mehta, who emphasizes that taking small steps each day can lead to better heath.
âI tell my patients, âEach day, please do one thing for your psoriasis, one thing for your mind and one thing for your body,ââ he says.
References:
1. Elmets CA, Leonardi CL, Davis DMR, Wu JJ, Hariharan V, Menter A, et al. Joint AAD-NPF Guidelines of Care for the Management and Treatment of Psoriasis with Awareness and Attention to Comorbidities. Published February 13, 2019. J Am Acad Dermatol. Doi.org/10.1016/j.jaad.2018.11.058
2. Takeshita J, Grewal S, Langan SM, Mehta NN, Ogdie A, Van Voorhees A, Gelfand JM. Psoriasis and Comorbid Disease Part I. Epidemiology. March 2017. J Am Acad Dermatol. Doi.org/10.1016/j.jaad.2016.07.064
3. Mathew AJ, Chandran V. Depression in Psoriatic Arthritis: Dimensional Aspects and Link with Systemic Inflammation. Published April 22, 2020. Rheumatology and Therapy. Doi.org/10.1007/s40744-020-00207-6
Don’t Miss: Is Mg217 Good For Psoriasis
Why Do People Get Psoriasis
Both genetic and environmental factors are believed to be responsible for whether or not a person will get psoriasis. The theory is that those who develop the disease are born with a particular genetic makeup that causes vulnerability to psoriasis, and those who actually develop the disease are exposed to something in the environment that triggers the disorder.
Encountering certain environmental triggers seems to jump-start the machinery of the body’s immune system in vulnerable individuals. Some of the environmental factors that seem to be able to trigger psoriasis or to cause a flare-up of the condition in someone who already has the disorder include:
- Infections. Psoriasis often starts or worsens after you’ve had some kind of infection, especially one caused by streptococcus bacteria .
- Medications. Lithium, anti-malaria drugs, high blood pressure medicines and the anti-inflammatory drug Indocin are some of the drugs that seem to be possible triggers.
- Skin injury. Overly dry skin, sunburn, cuts, and scratches sometimes lead to psoriasis.
- Stress. Some studies suggest that stress can serve as a trigger for psoriasis.
How Does It Affect Psoriasis Treatment Options
The primary goals of treatment are to:
- Reduce symptoms
- Control the autoimmune process
- Maintain the body’s ability to fight disease
For people with moderate to severe plaque psoriasis, an immunosuppressive drug may be needed to reduce their immune system’s abnormal responses. Your healthcare provider may prescribe medication that is designed to affect processes of inflammation throughout your entire body, like a corticosteroid.
In other cases, your healthcare provider may choose a therapeutic biologic medication that is designed to target a specific inflammatory pathway.
Combining biologics with traditional psoriasis therapies may provide an important treatment option for people who do not adequately respond to monotherapy. These approaches are called combination therapy.
Combination therapy may also help in the prevention or treatment of co-occurring diseases in certain patients.
One concern of patients considering biologics for treatment of psoriasis is it may increase their risk of infection. However, it is important to note that much of the available data regarding susceptibility to infection with biologic therapy derives from studies in inflammatory diseases other than psoriasis, such as rheumatoid arthritis and Crohns disease.
Also Check: How To Treat Plaque Psoriasis On Scalp
What Is Cdc Doing About Psoriasis
In 2010, CDC worked with experts in psoriasis, psoriatic arthritis, and public health to develop a public health perspective that considers how these conditions affect the entire population. The resulting report is Developing and Addressing the Public Health Agenda for Psoriasis and Psoriatic Arthritis pdf icon. You can read a short article about the agendaexternal icon in The American Journal of Preventive Medicine.
CDCs National Health and Nutrition Examination Survey , an intermittent source of national psoriasis data, has included questions about psoriasis as late as the 2013-2014 cycle. A recent analysis of NHANES data estimates that 7.4 million adults had psoriasis in 2013external icon.
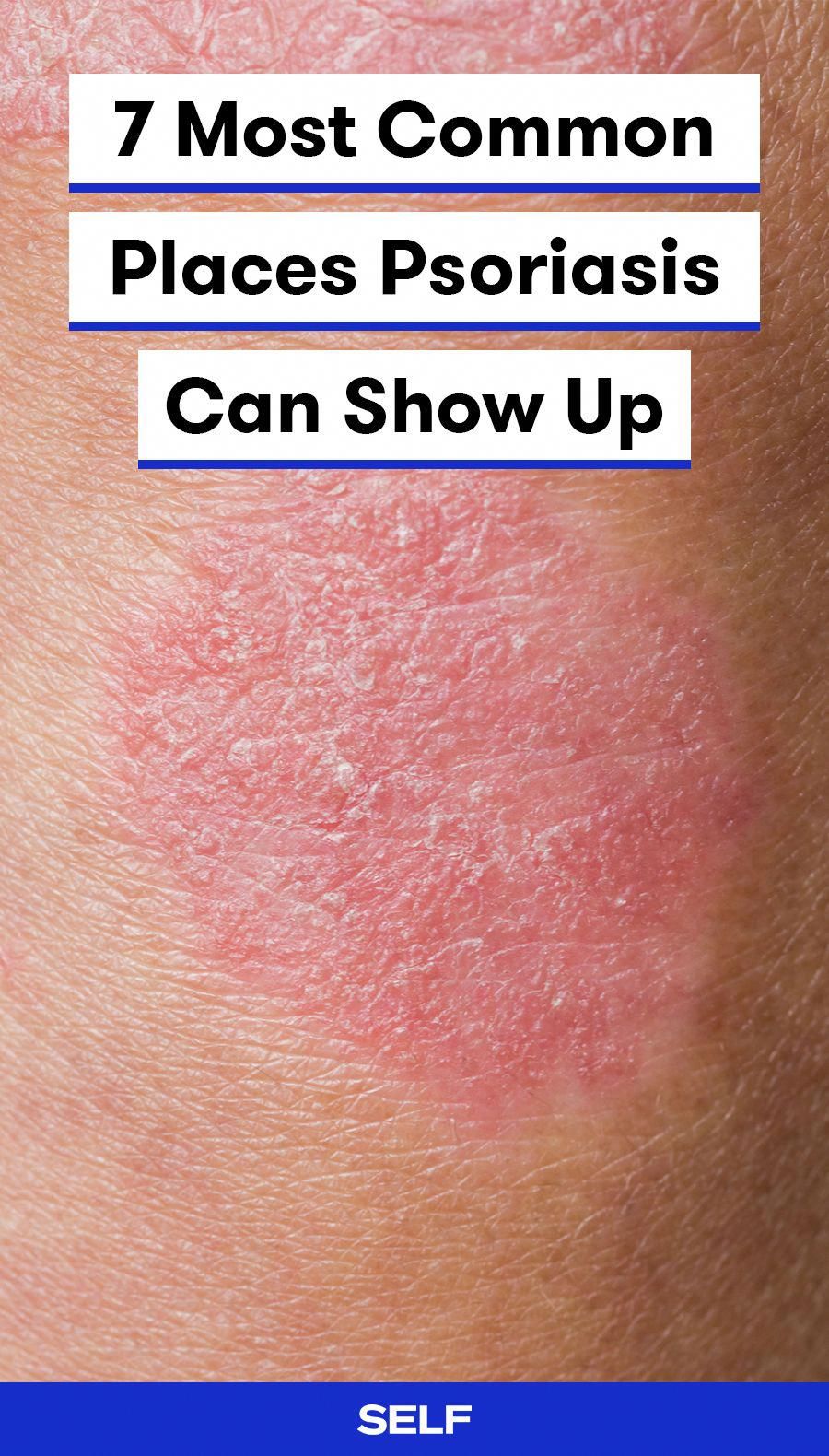
- Psoriasis causes patches of thick red skin and silvery scales. Patches are typically found on the elbows, knees, scalp, lower back, face, palms, and soles of feet, but can affect other places . The most common type of psoriasis is called plaque psoriasis.
- Psoriatic arthritis is an inflammatory type of arthritis that eventually occurs in 10% to 20% of people with psoriasis. It is different from more common types of arthritis and is thought to be related to the underlying problem of psoriasis.
- Psoriasis and psoriatic arthritis are sometimes considered together as psoriatic disease.
Who is at risk for psoriasis?
Anyone can get psoriasis. It occurs mostly in adults, but children can also get it. Men and women seem to have equal risk.
Can I get psoriasis from someone who has it?
What About Different Types Of Psoriasis
Does the type of psoriasis you have affect your lymphoma risk? In 2021, a new analysis of 25 different studies found that people with moderate to severe plaque psoriasis have a higher risk of all types of blood and lymph node cancers, including Hodgkinâs and non-Hodgkinâs lymphoma, multiple myeloma, and leukemia, and a much higher risk of CTCL.
Psoriatic arthritis, an autoimmune disease that causes both psoriasis skin patches and swollen, painful arthritis in your joints, doesnât seem to increase risk of lymphoma or other cancers.
Pustular psoriasis is a rare type that causes pustules, or raised skin bumps. Pustular psoriasis may occur along with plaque psoriasis or appear on its own. Itâs possible that pustular psoriasis may increase your risk of lymphoma.
In some rare cases, CTCL causes skin bumps on the palms or soles of the feet that are mistaken for pustular psoriasis. Doctors could miss this cancer unless they do a biopsy, or tissue sample test.
Read Also: How To Make Psoriasis Go Away
How Are Autoimmune Diseases Diagnosed
Diagnosing an autoimmune disease usually takes healthcare providers longer than it does to diagnose other diseases. This is because many autoimmune diseases have similar symptoms with each other and with other diseases. You can help your healthcare provider with the diagnosing process by bringing the following to your appointment:
- A detailed list of any symptoms and how long youve had them.
- A record of your familys health history. Note if anyone in your family has an autoimmune disease.
In addition to interviewing you about your symptoms, your healthcare provider may do some blood tests to check for autoimmune diseases, including:
- Antinuclear antibody test .
Specific symptoms combined with specific blood markers may prove that you have an autoimmune disease.
What Is An Autoimmune Disease
In an autoimmune disease, the body loses the ability to tell the difference between some of the bodys tissues and harmful microbes that can cause sickness, leading the body to attack healthy tissue.
The immune system is made up of cells and proteins that attack anything foreign to the body, such as invading bacteria, viruses, and other potential causes of infection and sickness. The immune system is designed to attack and neutralize invaders by recognizing molecules on them known as antigens. It is important that the immune system knows the difference between the bodys own tissues and a foreign invader.
However, when immune cells begin responding abnormally, they misidentify aspects of our own body as harmful invaders and attack. This abnormal response is described as being autoreactive or autoimmune auto is a Greek prefix meaning self. The self-antigens targeted in autoimmune diseases are known as autoantigens.
Autoimmune diseases are classified by the type of tissue that is being attacked. For example, in rheumatoid arthritis, the tissue lining the inside of the joints is attacked. In type 1 diabetes, the immune system attacks and destroys insulin-producing cells in the pancreas. In celiac disease, the immune system attacks the small intestine when gluten is consumed. And in people with psoriasis, the immune system produces inflammatory reactions against molecules related to the skin.
Also Check: How Does Psoriasis Affect The Body
Saponins Enterohepatic Circulation And Fat
Bile salts , which are produced by the liver, stored in the gallbladder, and then secreted into the small intestine after eating, are necessary to digest fats. They are created from cholesterol, which is converted into one of two types of fatty acid and then conjugated with the amino acids glycine or taurine to create a detergentlike structure . The majority of bile salts are reabsorbed by the small intestine and recycled back to the liver for reuse . Bile salts act as an emulsifier , by breaking apart large fat globules so that lipases can more effectively do their job. Bile acids also facilitate absorption of fats and fat-soluble vitamins by creating structures called micellesaggregates of fatty acids, lipids, cholesterol, and fat-soluble vitaminswhich are water soluble and easily absorbed by the enterocytes.
Psoriasis = An Autoimmune Disease
Its taken years, but most researchers now classify psoriasis as an autoimmune disease. At the very least, they recognize a link between the two.
Its not hard to understand why. Folks with psoriasis have overactive T cells your immune systems personal fighter jets just like folks with other autoimmune diseases.
During a psoriasis flare-up, your T cells attack healthy skin cells with a special protein called cytokines. The cytokines make your skin cells multiply super fast so much so that they start building up on top of each other. This forms those dry, scaly patches.
In 2017, researchers confirmed that cytokines are involved in triggering psoriasis, which was a major milestone in the development of treatments.
Since then, research continues to indicate that immunosuppressants help with psoriasis.
Read Also: What Is Arthropathic Psoriasis Unspecified
What Is The Difference Between Scalp Eczema And Scalp Psoriasis
Scalp eczema and scalp psoriasis can look very similar. Theyre both inflammatory skin conditions. Scalp psoriasis typically has well-defined plaques, while scalp eczema is much itchier, even before you see the rash.
Your healthcare provider can tell the difference between scalp eczema and scalp psoriasis during an examination.
A note from Cleveland Clinic
Scalp psoriasis is an autoimmune condition that causes thick patches of skin to develop on your scalp or the skin around your scalp. You may feel self-conscious, and it can be unpleasant if its itchy or painful. However, it isnt contagious, and treatments can help your symptoms improve. Its important to pay attention to your skin, including your scalp. Contact your healthcare provider as soon as you notice any plaques developing on your scalp.
Who Will Be Responsible For My Healthcare
Youre likely to see a team of healthcare professionals.
Your doctor, usually a rheumatologist, will be responsible for your overall care. And a specialist nurse may help monitor your condition and treatments. A skin specialist called a dermatologist may be responsible for the treatment of your psoriasis.
You may also see:
- a physiotherapist, who can advise on exercises to help maintain your mobility
- an occupational therapist, who can help you protect your joints, for example, by using splints for the wrist or knee braces. You may be advised to change the way you do some tasks to reduce the strain on your joints.
- a podiatrist, who can assess your footcare needs and offer advice on special insoles and good supportive footwear.
You May Like: How To Get Rid Of Psoriasis On Neck
Psoriatic Disease Affects More Than Skin And Joints
The systemic inflammation that drives symptoms of psoriatic disease can raise your risk for other health problems.
If you have psoriasis or psoriatic arthritis , you may know that these diseases raise your risk for some other conditions as well. When one disease is triggered by or linked to another, the related condition is called a âcomorbidity.â PsA, for example, is a common comorbidity of psoriasis, affecting up to 33 percent of people with psoriasis.
According to the recent Joint AAD-NPF Guidelines of Care for the Management and Treatment of Psoriasis with Awareness and Attention to Comorbidities, other comorbidities for which psoriatic disease raises risk include:
- Cardiovascular disease
- Mental health impacts, including depression and anxiety
- Inflammatory bowel disease
- Uveitis
- Nonalcoholic fatty liver disease
Just how this elevated risk happens for each comorbidity isnât fully understood. One underlying factor that likely plays an important role in triggering or contributing to development of many comorbidities, however, is systemic inflammation, explains dermatologist Paul S. Yamauchi, M.D., Ph.D.
The weapons the immune system uses for this attack are inflammatory immune cells that normally defend the body from injury and infection.
Problems With The Immune System
Your immune system is your body’s defence against disease and it helps fight infection. One of the main types of cell used by the immune system is called a T-cell.
T-cells normally travel through the body to detect and fight invading germs, such as bacteria. But in people with psoriasis, they start to attack healthy skin cells by mistake.
This causes the deepest layer of skin to produce new skin cells more quickly than usual, triggering the immune system to produce more T-cells.
It’s not known what exactly causes this problem with the immune system, although certain genes and environmental triggers may play a role.
Don’t Miss: First Line Treatment For Psoriasis
What Exactly Is An Autoimmune Disease
When you have an autoimmune disease, your body mistakes normal, healthy tissues for foreign invaders. Basically, it goes to war with itself, causing damage and inflammation.
Not so fun fact: There are 100+ autoimmune diseases. Some of them, like psoriasis, only affects one body part . Others are system-wide, leaving your body exhausted and achy almost 24/7.
Regardless of your autoimmune diagnosis, your body is doing its war-waging thing because of some mysterious perfect storm of genetics and environmental factors.
Environmental Triggers Of Psoriasis
Several environmental factors including physical trauma, drug reactivity, infection as well as modifiable variables such as psychological stress, obesity, smoking, and alcohol have been associated with a predisposition toward psoriasis development and exacerbation of the disease.
Physical trauma
Heinrich Koebner first described physical trauma as a trigger and exacerbating factor for psoriasis in 1872. He observed the development of psoriatic lesions after a direct cutaneous injury, such as excoriation, tattoos, burns, and animal or insect bites, in previously normal-appearing skin . The new psoriatic lesion was characterized morphologically as identical to the injury site, known as an isomorphic response. The Koebner response has been observed with other dermal diseases such as vitiligo and lichen planus, but the frequency for its manifestation is higher among psoriasis patients. The prevalence of Koebner response in psoriasis patients ranges from 24%51%.
Psoriasis onset following an injury may take anywhere from 3 days to 2 years to develop, and may be dependent on seasonal variation as well as disease severity .,
Drug-induced psoriasis
Other reported medications that exacerbate psoriasis include ACE inhibitors, calcium channel blockers, and IL-2 among others.
Infections
Stress
Alcohol and smoking
Obesity
You May Like: How To Stop Psoriasis Hair Loss