Rheumatoid Arthritis And Psoriatic Arthritis: The Similarities And Differences
All forms of arthritis involve tenderness and swelling of the joints. And, at first glance, psoriatic arthritis can be very hard to differentiate from other common types of arthritis, including rheumatoid arthritis and osteoarthritis.
Because psoriatic arthritis symptoms can overlap with those of rheumatoid arthritis and osteoarthritis not just swollen, achy joints but also stiffness and chronic fatigue diagnosing this autoimmune disease can be tricky.
Unlike rheumatoid arthritis, there is no blood test that can determine if a person has psoriatic arthritis, says M. Elaine Husni, MD, MPH, a rheumatologist at the Cleveland Clinic in Ohio.
Psoriatic arthritis can also affect the body in different ways depending on the person and how advanced the disease is, says Dr. Husni. As a result, a rheumatologist may need to examine a patient several times and run a number of tests before having enough information to make a definitive diagnosis.
One unique symptom of psoriatic arthritis that doctors look for is the presence of psoriasis, a condition that causes thick, discolored, scaly skin patches known as plaques, as well as pitted nails or nails that separate from the nail bed, according to the American Academy of Dermatology.
Like psoriatic arthritis, psoriasis stems from a faulty immune response, in which the immune system mistakenly attacks healthy cells and tissues.
Treatment Options For Fibromyalgia And Psoriatic Arthritis
Treating fibromyalgia can be difficult as its exact cause is unknown. Therefore, the goal of fibromyalgia treatment is symptom management. A doctor may prescribe analgesics, or painkillers, to address fibromyalgia. However, there is a risk of developing an addiction to these drugs, so doctors may recommend this option with caution. Nonsteroidal anti-inflammatory drugs can also be taken for pain management, but once again long-term use of these drugs can yield unwanted side effects. In some cases, antidepressants may be prescribed as well.
Some alternative and complementary therapies and treatments for fibromyalgia include massages, acupuncture, cognitive behavioral therapy, movement therapies, and chiropractic.
There is currently no cure for psoriatic arthritis, but treatment options are available. Medical treatments involve the use of anti-inflammatory medications, disease-modifying anti-rheumatic drugs , immunosuppressants , steroid injections , and joint replacement surgery.
Home remedies for psoriatic arthritis include exercising, protecting your joints, maintaining a healthy weight extra weight adds stress to already painful joints, and using cold and hot packs to reduce inflammation. Diet, too, can play a role in treating psoriatic arthritis.
Psoriasis Isnt Caused By Poor Hygiene
Psoriasis is an autoimmune disease and has nothing to do with poor hygiene. It is neither caused or worsened by poor hygiene. Much like other illnesses of the immune system, people who have the condition have a genetic tendency to develop it.
If someone in your family has psoriasis, you may have the genes to develop the condition. But even with the right genes, there still needs to be something that triggers the disease. This could be anything from a physical illness to a skin injury or even extreme stress, or a certain medication. Once something triggers psoriasis, it is either short-lived or life-long. If it is life-long, there are often treatments to control it.
Also Check: Is Eating Tomatoes Bad For Arthritis
Don’t Miss: What Is Eczema And Psoriasis
Which Doctor Is Best At Diagnosing Psoriatic Arthritis
Normally, a dermatologist would be the first stop for diagnosis and treatment of psoriasis which is the skin condition that often triggers psoriatic arthritis. But arthritis falls within the area of expertise of the rheumatologist. He would be more competent in assessing the extent of damage suffered by joints, and he will customize a treatment plan tailored to individual patients.
Why Some People With Psoriasis Develop Psa
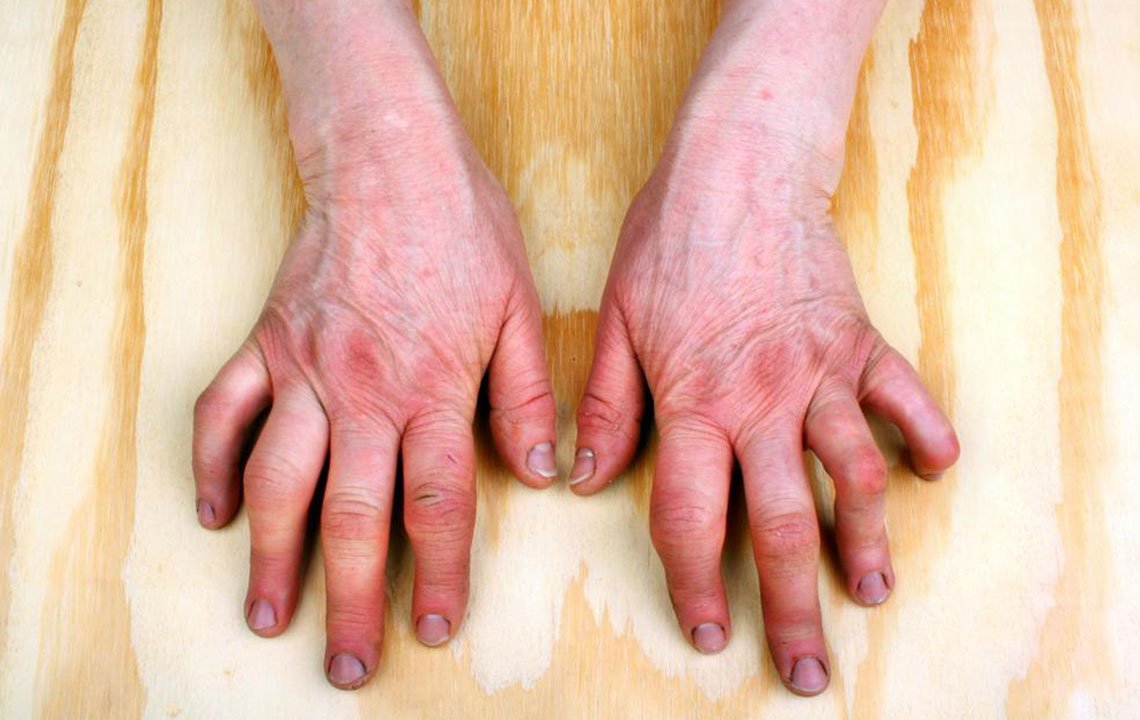
Although psoriasis and PsA may appear unrelated, both conditions reflect underlying immune system problems.
In psoriasis, your overactive immune system causes your bodys skin cells to develop too rapidly. This can be triggered by many environmental factors, such as stress or smoking.
One thing these triggers have in common is that they stimulate your bodys inflammation response. This same inflammation response can happen in your joints. Inflamed joints are what cause PsA.
In PsA, white blood cells target your bodys tissues instead of protecting your body against foreign substances. Though PsA is connected to psoriasis, it has very distinctive symptoms of its own. For this reason, some researchers have referred to PsA as a disease within a disease.
The Centers for Disease Control and Prevention calculates that 10 to 20 percent of people with psoriasis will go on to develop PsA. This is slightly lower than the figures provided by the National Psoriasis Foundation, which put the risk at about 1 in 3, or 30 percent.
Psoriasis is typically diagnosed by the onset of plaques. These are scaly patches of raised, silver-white or reddish skin. PsA affects your joints, typically those in your fingers, toes, and lower back.
PsA can come in many forms. It can trigger other side effects such as fatigue and decreased range of motion. Because psoriasis is more visibly apparent, its often easier to diagnosis than PsA.
Don’t Miss: Psoriasis En Los Pies Fotos
How Are Ra And Psa Diagnosed
Because these two conditions share similar symptoms, it’s important to get an accurate diagnosis from a rheumatologist. A rheumatoid factor blood test is one way your doctor can tell which condition you have. RF is a protein found in people with rheumatoid arthritis. People with PsA usually don’t have it. Blood tests looking for other antibodies such as anti-CCP can also help differentiate the two.
Another way to tell is to look at your skin and nails. If you have scaly patches on your skin, pitting and flaking on your nails, or both, you have PsA.
Once you’ve had the disease for a while, X-rays might also be able to distinguish the two conditions.
It is possible to have RA and PsA together, but it’s rare. If you do have both, many of the treatments, including some medications, will work for both conditions.
How Do Lupus And Psoriatic Arthritis Differ From Each Other
The similarities in symptoms often complicate initial diagnosis of lupus and psoriatic arthritis. The antibodies produced in both cases cause inflammation and damage to the tissue and both represent the auto-immune disease category. Both are identified to cause damage to vital organs like heart, brain, lungs, and kidneys. Both lupus and psoriatic arthritis do not have a definitive test. Normally when your body senses entry of any foreign particles or microorganisms, the immune cells get activated and release certain antibodies into the bloodstream in an attempt to get rid of the foreign bodies.
But when you have any auto-immune condition, the immune system fails to differentiate the bodys own healthy tissues from foreign bodies, and thus release antibodies that attack the healthy tissues.
Psoriasis shows silver scaly patches which are usually flat whereas, lupus rashes are red, raised, and usually in areas that are exposed to sunlight . These patches may vary from person to person. Some people find them itchy, some find them painful. The symptom depends on the location and sensitivity of your skin.
Lupus is characterized by immune-mediated damages to the skin, joints, blood, kidneys, heart, and lungs while psoriatic arthritis has symptoms such as inflamed skin and joints.
However, these conditions are not the same. Learn more about the differences here:
Also Check: Psoriasis On Palms Of Hands Treatment
I Feel At A Loss Sometimes Depressed Is This Normal
Yes, this is a very normal process, a form of mourning and coming to terms with the fact that you have arthritis, and some things may have to change in your lifestyle to compensate, making things easier for you. Dont panic, try to work through your feelings, talking with a partner or someone close to you, If the feelings don’t pass, see your doctor who may be able to refer you to some form of short-term counselling.
How Is Psoriatic Arthritis Diagnosed
There is no test which clearly diagnoses early psoriatic arthritis. When you first develop symptoms of arthritis it can be difficult for a doctor definitely to confirm that you have psoriatic arthritis. This is because there are many other causes of arthritis. However, if you have developed psoriasis within the previous few years and then an arthritis develops, there is a good chance that the diagnosis is psoriatic arthritis.
In time, the pattern and course of the disease tend to become typical and a doctor may then be able to give a firm diagnosis.
Some tests may be done, such as blood tests and X-rays. These can help to rule out other types of arthritis. For example, most people with rheumatoid arthritis have an antibody in their blood called rheumatoid factor. This does not usually occur in psoriatic arthritis. Also, the X-ray appearance of joints affected by psoriatic arthritis tends to be different to that seen in rheumatoid arthritis and osteoarthritis.
Recommended Reading: Scalp Psoriasis Vs Seborrheic Dermatitis
What Are The Symptoms Of Psoriasis
There are different types of psoriasis. The most common is chronic plaque psoriasis. This causes patches of red, raised skin, with white and silvery flakes.
It can occur anywhere on the skin, but most commonly at the elbows, knees, back, buttocks and scalp.
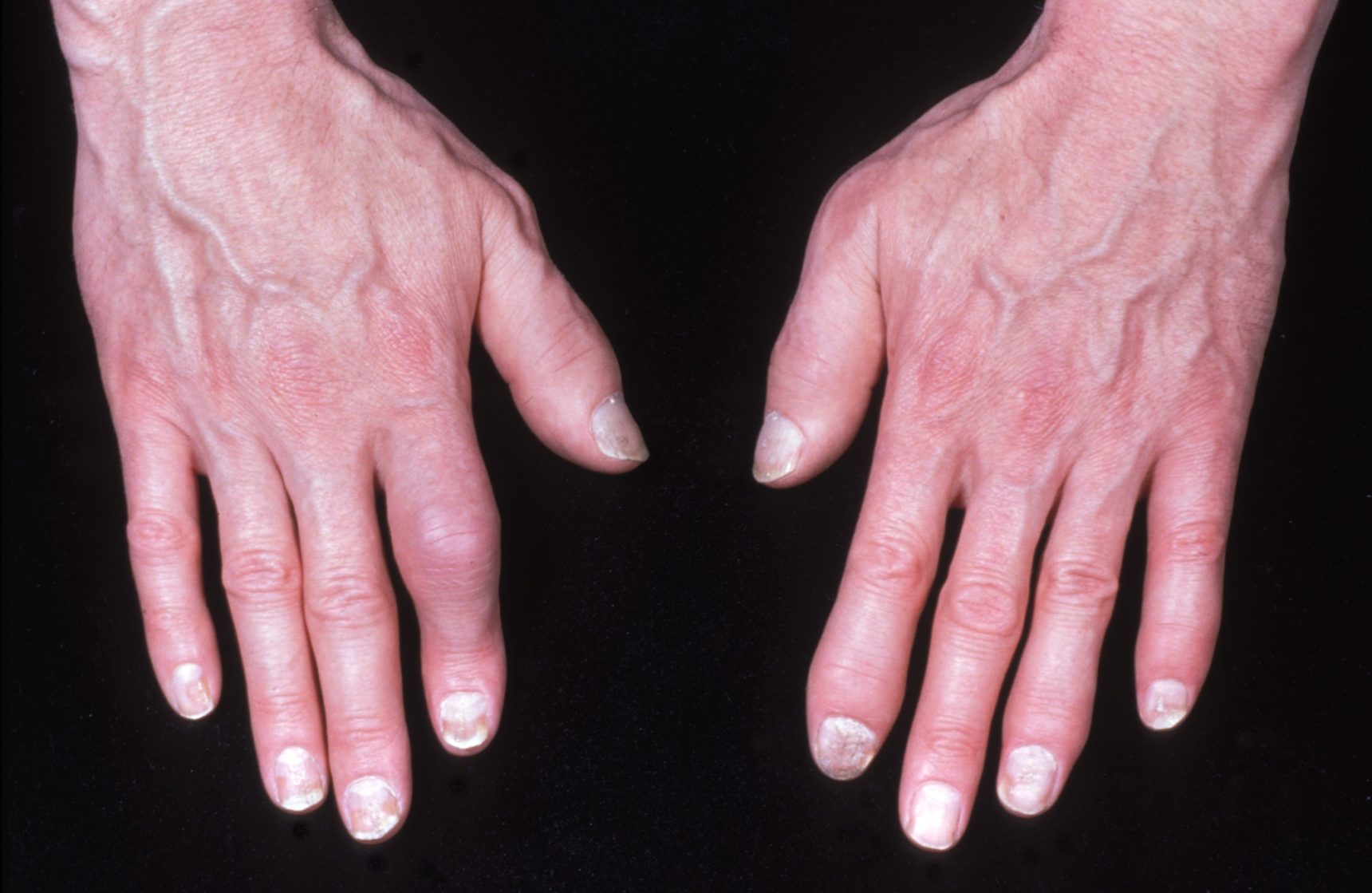
Psoriasis can cause small round dents in finger and toe nails, this is known as pitting. Nails can also change colour, become thicker and the nail may lift away from your finger.
What Are The Symptoms Of Psa
Beyond the classic symptoms of arthritis, including painful and swollen joints, PsA presents itself with a number of symptoms. If you are living with PsA, you may have one or several of these symptoms during flare-ups. Additionally, the presence of psoriasis is also a classic symptom of PsA. Though, in a small percentage of individuals who live with PsA, no symptoms of psoriasis appear at all. In the overwhelming majority of cases, even if no psoriasis is present, there is a family history of it.
Some of the more common symptoms of PsA include:
- Joint pain and inflammation
Recommended Reading: Can You Get Psoriasis At Any Age
What Are The Side Effects Of Taking A Biologic
Each PsA biologic is different. Each has its own potential side effects.
However, there are also similarities in this class of drugs. The most common side effect for all biologics is an increased risk of unusual, or opportunistic, infections.
In addition, TNF-alpha inhibitors may cause new or worsening heart failure.
If you and your doctor decide to try this course of treatment with a biologic, you may experience flu-like symptoms or respiratory infections.
Since biologics are given by injection or via an intravenous solution, you may also experience discomfort where the needle pokes your skin.
Biologics may lead to more serious side effects, such as blood disorders or cancer.
For these reasons, its a good idea to maintain a strong relationship with your doctor that focuses on open communication.
Together, you can talk about and decide on whether a biologic is the right treatment for your psoriatic arthritis.
Biologics are recommended for those living with moderate to severe PsA. But some people arent candidates for biologics.
Thats because the drugs side effects may do more harm than good.
People with compromised immune systems or active infections shouldnt take biologics for their PsA. These drugs suppress the immune system and can be unsafe if yours is already compromised in some way.
The cost and out-of-pocket expenses for biologics can also be a barrier for some people.
Can Psoriatic Arthritis Affect Children Too
As many as 12,000 children in the UK are affected by arthritis. It is known as juvenile chronic arthritis , of which there are three main types, stills disease, polyarticular juvenile chronic arthritis and polyarticular onset juvenile chronic arthritis. Psoriatic arthritis is a minor subset of JCA and is uncommon.
Recommended Reading: Witch Hazel For Scalp Psoriasis
What Is Psoriatic Arthritis Video
Psoriatic arthritis can cause pain, swelling and stiffness in and around your joints.
It usually affects people who already have the skin condition psoriasis . This causes patches of red, raised skin, with white and silvery flakes.
Sometimes people have arthritis symptoms before the psoriasis. In rare cases, people have psoriatic arthritis and never have any noticeable patches of psoriasis.
Psoriatic arthritis and psoriasis are autoimmune conditions. Our immune system protects us against illness and infection. In autoimmune conditions, the immune system becomes confused and attacks healthy parts of the body.
Both conditions can affect people of any age.
Its estimated that around one in five people with psoriasis will develop psoriatic arthritis.
People with psoriasis are as likely as anyone else to get other types of arthritis, such as osteoarthritis or rheumatoid arthritis. These conditions are not linked to psoriasis.
Psoriatic arthritis is a type of spondyloarthritis. These are a group of conditions with some similar symptoms.
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Read Also: Does Quitting Smoking Help Psoriasis
Summary Plaque Psoriasis Vs Psoriasis
Psoriasis is a chronic multisystem disease with skin and joint manifestations. Plaque psoriasis is the commonest form of psoriasis which is characterized by the appearance of reddish well-demarcated plaques with silver scales usually on the extensor surface of the knees and elbows. Accordingly plaque psoriasis is one manifestation of the broad spectrum of dermatological and systemic manifestations which are identified as psoriasis. This can be identified as the difference between plaque psoriasis and psoriasis.
Dont Miss: Why Is Psoriasis Medicine So Expensive
Treatment Options For Psoriasis Only
The most common treatments for mild psoriasis are topical skin creams and ointments. These include vitamin D, salicylic acid, and a class of drugs called corticosteroids.
Vitamin D has been deemed an effective treatment for autoimmune problems in the body, including psoriasis.
Corticosteroids have been found to be at least as effective as vitamin D. The drawback of corticosteroids is that over time, using them on your skin might make your skin weaker. Other side effects of corticosteroids include:
- broken blood vessels
- irritation
- skin that bruises
Corticosteroids range from mild to extremely potent. The more potent the drugs, the higher the potential for side effects. Because psoriasis is a chronic disease, the best treatments are those that can be used long term without risk of injury to your body.
Certain home remedies may also help you relieve psoriasis symptoms. Daily baths using Epsom salts can soothe scaly patches on your skin. Topical aloe vera and Oregon grape have been found to help reduce irritation and inflammation.
Recommended Reading: Does Hydrocortisone Cream Help Psoriasis
What Can Prevent Someone From Getting A Second Type Of Psoriasis
Most types of psoriasis cannot be prevented.
That said, if you already have plaque psoriasis, it may be possible to reduce your risk of developing another type of psoriasis on your skin. Dermatologists recommend taking the following precautions:
-
Protect your skin to prevent sunburn
-
Take medication as directed and speak with your dermatologist before stopping a medication
-
Treat your psoriasis so that its well-controlled
-
Watch your weight so that you stay at a weight thats recommended for your age and height
Watching your weight may help prevent inverse psoriasis. This type of psoriasis is more common in people who are 20 or more pounds overweight.
What Are Treatments For Scalp Psoriasis
According to the NPF, scalp psoriasis can be difficult to treat because of the hair covering the plaques. Doctors usually start with basics in treating it, says Dr. Gohara, often with prescription topical inflammatory medications, a form of steroid.
If a person has a mild case of scalp psoriasis, there are OTC psoriasis products that can be tried first, says the NPF look for products that contain salicylic acid or coal tar. Shampoos targeted to help psoriasis can help: Salicylic acid shampoos cut thru the over-proliferation of the skins top layer on the scalp, says Dr. Gohara. There are other shampoos containing coal tar that can be tried as well.
, which uses UV light to slow cell growth, is also used to treat psoriasis. As dermatologists, were always telling people to avoid UV light, but its a very effective anti-inflammatory, says Dr. Gohara. For scalp psoriasis, a doctor can use a hand-held phototherapy device with a comb to specifically target that area, according to the NPF.
Dont Miss: Shampoo And Conditioner For Psoriasis
Recommended Reading: Vitamin A Derivative For Psoriasis
How Do Ra And Psa Affect You
When you have RA, your immune system attacks the lining of the tissues around your joints. They swell up and become painful. Over time, they can become damaged and deformed.
With PsA, your immune system attacks and damages not just your joints, but your skin, as well. It causes your body to make too many skin cells, which leads to psoriasis, a skin condition that often affects people with PsA.