Inflammation May Link Psoriasis And Depression
If you experience psoriasis along with anxiety or depression, youre not alone. Its thought that 43 percent of people with psoriasis also have anxiety. An estimated 20 to 30 percent of people with psoriasis are thought to be affected by depression .
There are a number of reasons why this correlation exists. One academic paper noted that there may be a close connection between depression and inflammation. Depression and negative experiences can trigger a stress response in the body, which increases inflammation. The inflammation can then exacerbate symptoms of depression.
The paper further noted that people with depression have higher levels of pro-inflammatory cytokines by 30 percent in comparison to those who dont experience depression.
Effects Of Inflammation On Psoriasis
Inflammation is the bodys natural response to defend and repair. When a healthy person becomes sick, their immune system triggers inflammation. White blood cells rush in to protect against invaders and repair the damage. When the illness stops , the inflammation stops.
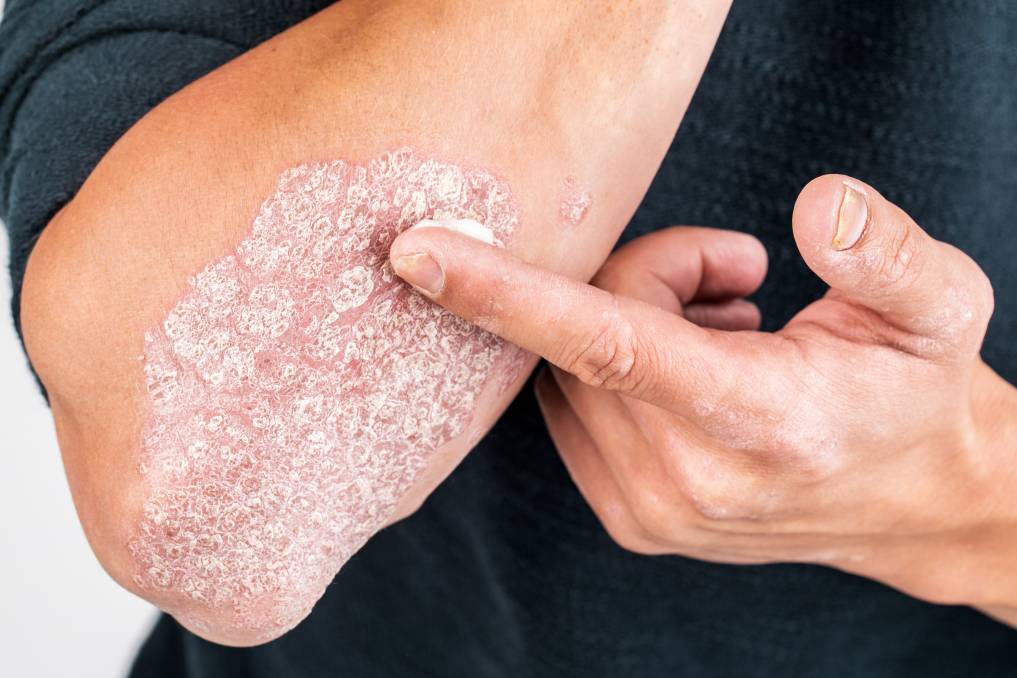
But for people with inflammatory conditions, that inflammation continues. In people with psoriasis, that widespread inflammatory response pushes new skin cell growth before old skin cells have had an opportunity to shed.
New skin cells then push up old cells to the surface leading to plaques and scales. These become visible on the skins outermost layer.
The effects of psoriasis dont always stop at the skin. Up to 30% of people with psoriasis will go on to develop a type of arthritis called psoriatic arthritis . PsA is a chronic, inflammatory kind of arthritis. The ongoing inflammation wreaks havoc on the joints and areas where the tendons and ligaments connect to bone .
Studies have found people with psoriasis are at a higher risk for many different health conditions, including heart attacks, strokes, diabetes, inflammatory bowel disease, and depression. The same inflammatory processes that promote psoriasis also play a role in the development of many of these other very serious conditions.
Bibliography For Psoriasis In Skin Of Colour
- Amico S, Barnetche T, Dequidt L, et al. Characteristics of postinflammatory hyper- and hypopigmentation in patients with psoriasis: a survey study. J Am Acad Dermatol. 2020 83:1188-91. doi:10.1016/j.jaad.2020.02.025. PubMed
- Geng A, McDonald C. Psoriasis. In: Taylor SC, Kelly AP, Lim HW, Serrano AMA . Taylor and Kelly’s Dermatology for Skin of Color, 2nd edn. McGraw Hill, 2016: Chapter 24.
- Kaufman BP, Alexis AF. Psoriasis in skin of color: insights into the epidemiology, clinical presentation, genetics, quality-of-life impact, and treatment of psoriasis in non-white racial/ethnic groups [published correction appears in Am J Clin Dermatol. 2018 19:405-23. doi:10.1007/s40257-017-0332-7. PubMed
- Yan D, Afifi L, Jeon C, Cordoro KM, Liao W. A cross-sectional study of the distribution of psoriasis subtypes in different ethno-racial groups. Dermatol Online J. 2018 24:13030/qt5z21q4k2. PubMed
Recommended Reading: Does Head And Shoulders Help Psoriasis
Shades Of Gray: Crosstalk Between Adaptive And Innate Immunity In Psoriasis
In addition to the antigen-specific facilitation of inflammation in psoriasis, there are several strong connections to components of the innate immune system. The crosstalk between the innate and adaptive branches of the immune system in psoriasis is complex and can only be highlighted by a few selected examples. Its fine-tuning arguably determines the actual clinical correlate within the spectrum of the disease. Indeed, there is accumulating circumstantial evidence that in patients with stable and mild disease, mechanisms of adaptive immunity are more likely to be in the foreground, while innate mechanisms seem to be more important in patients with active severe disease, systemic involvement and comorbid conditions . The impact on systemic comorbid diseases has been interpreted, at least in part, as a systemic spillover of innate inflammatory processes in severe psoriasis . Of course, such factors are not specific for psoriasis, but appear to account for a general inflammatory state in patients with severe psoriasis.
Patients with severe psoriasis have increased levels of inflammatory cytokines, CRP, fibrinogen, 2 macroglobulin or PAI-1 in the blood , they show transcriptomic, proteomic and metabolomic abnormalities and there are connections with chronic stress and biophysical properties of the skin .
Treatment For Psoriatic Arthritis
Treatment for psoriatic arthritis aims to:
- relieve symptoms
- slow the condition’s progression
- improve quality of life
This usually involves trying a number of different medicines, some of which can also treat the psoriasis. If possible, you should take 1 medicine to treat both your psoriasis and psoriatic arthritis.
The main medicines used to treat psoriatic arthritis are:
- non-steroidal anti-inflammatory drugs
- biological therapies
Read Also: Is Milk Bad For Psoriasis
Dealing With More Than Just Psoriasis
Managing any disease can be a challenge. When you have psoriasis, you may need to keep track of multiple medications, such as: prescription skin creams, ultraviolet light therapy, and powerful medicines. Thatâs in addition to things you might do at home to look and feel better, from daily oatmeal baths to avoiding alcohol.
Managing other diseases in addition to psoriasis only adds to your burden. You could be facing:
- Emotional distress
- Increased risk for drug interactions
- Limited activity
Itâs a lot to handle, but your doctor can help in ways you might not have thought about. The key is to be an active partner in controlling your diseases, not just a passive listener. You can start by bringing your doctor a list of your concerns — emotional, financial, and medical. Here are some examples to get you started:
- Why are you prescribing a certain medication? Does it have risks that I should know about, especially considering other drugs I take?
- I donât take certain medications regularly because of the cost. Do I have other options?
- I have a health goal to take fewer medications / lose 15 pounds / feel less depressed, but I need help. Can you help me create a plan?
If you donât like what you hear, or donât feel youâre getting the help you need, remember it never hurts to get a second opinion.
Show Sources
Screening Patients With Psoriasis For Associated Comorbidities
In the field of dermatology, guidance is lacking regarding how and when to screen patients with psoriasis for common cardiometabolic comorbidities. In the authors opinions, dermatologists, nurse practitioners, and physician assistants can play an important role in ensuring that such screenings are performed, along with well-established screenings . Comorbidity screenings for patients with psoriasis should include taking a complete medical history, thorough physical examination, blood pressure measurement, and a comprehensive metabolic panel, including liver and kidney function, and measurements of glucose, triglyceride, and cholesterol levels . Patients meeting three or more of the criteria from Table 3 have metabolic syndrome.
Dermatology care providers knowledgeable about psoriasis and associated comorbidities can provide proper referral to a primary care physician or specialist. Interdisciplinary collaboration between dermatologists, primary care, and other specialists is important to ensure that care is coordinated and patients receive appropriate follow-up for optimal management of comorbidities
Also Check: How Do I Know If I Have Scalp Psoriasis
What Are The Symptoms Of Psoriasis
Psoriasis causes different symptoms in different people. Symptoms normally develop before age 45.
The most common symptoms are dry, raised, red patches of skin covered with silvery scales. The patches usually appear on the knees, elbow, lower back and scalp, but they can appear anywhere on the body.
Psoriasis can also cause dents and discolouration of the nails.
Some people get small, drop-shaped sores on the chest, arms, legs or scalp. Some people get swollen, painful joints.
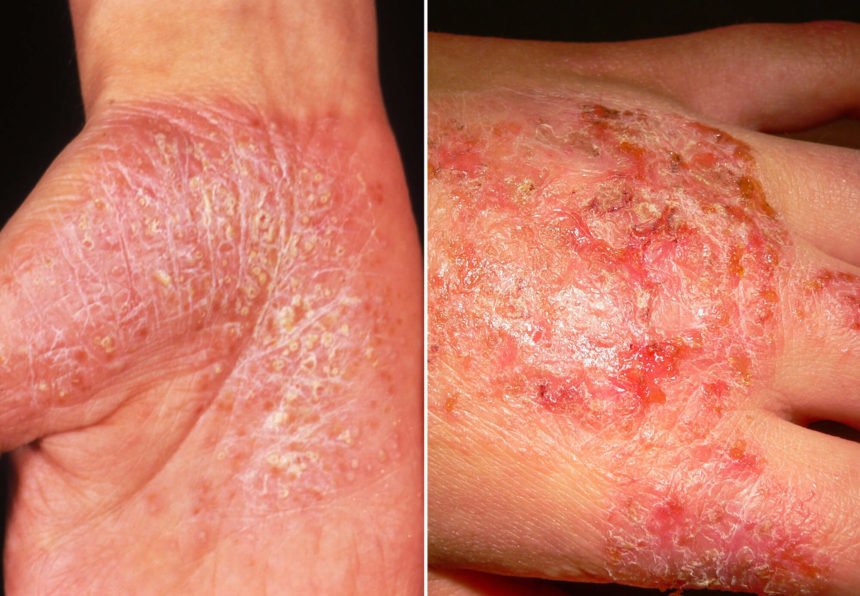
The symptoms of some rare types of psoriasis include pus-filled blisters or a red, peeling rash that itches or burns intensely.
Cross section illustration of psoriasis
Close-up of psoriasis on skin
Getting The Right Diagnosis
If you think you have psoriasis, see your doctor right away. It shouldnât take long to get an answer once youâre there. Usually, all it takes to diagnose psoriasis is a discussion about your medical history and an exam of your skin, scalp, and nails. Some doctors may also take a small sample of skin to examine under a microscope. This test is called a biopsy.
While youâre at the doctor, be sure to speak up if you have any other symptoms besides skin and/or nail problems — especially if you have joint issues, including:
- Heel pain
- Morning stiffness that improves during the day
- Swelling just above your heel
- Swollen or tender joints
Because psoriasis often goes along with PsA, youâll want to know as soon as possible if you have both. Early diagnosis and treatment of PsA can help prevent permanent damage to your joints.
You May Like: New Treatment For Plaque Psoriasis
Psoriasis Psoriatic Arthritis And Crohns Disease: Whats The Connection
Crohns disease and ulcerative colitis can be associated with psoriasis and psoriatic arthritis , which are comorbidities of CD and colitis. A comorbidity is when two or more disorders occur in the same person and cause adverse interactions.
CD and UC are the two main types of inflammatory bowel disease . CD is characterized by chronic inflammation in the lining and deeper layers of the digestive tract. UC causes sores and inflammation in the lining of the colon and rectum.
Psoriasis causes a proliferation of skin cells that become dry, itchy, and scaly with discolored patches of thickened skin . Skin can become infected during flares. Approximately 30 percent of people with psoriasis develop PsA, a type of inflammatory arthritis. Symptoms include joint pain, swollen and stiff joints, tendon pain, fatigue, and eye redness and pain .
For people with Crohns or colitis, the increased risk for psoriasis is approximately three times that of the general population.
MyCrohnsAndColitisTeam members have discussed their challenges with IBD, psoriasis, and PsA. Today, I meet with a dermatologist to discuss Stelara to treat both Crohn’s and psoriasis, one member wrote. The GI doctor gave me a prescription for prednisone to help, but I have severe osteoporosis, so before starting, I am trying to connect all medical providers to be on one page.
Common Pathways Of Psoriatic And Atherosclerotic Plaque Formation
To this end, epidemiological evidence in favor of psoriasis being associated with cardiovascular comorbidity and potentially functioning as an independent cardiovascular risk factor has been summarized. As genetic overlap cannot satisfyingly explain the excess cardiovascular risk of patients with severe psoriasis, mechanistic studies are needed to further clarify the link.
Atherosclerosis as a key process in cardiovascular diseases has long been recognized as an inflammation-driven phenomenon . This is also true for psoriasis . The cardiologist Späh was among the first who discussed a potentially common inflammatory pathway and the idea of an integrated treatment approach . He stressed altered endothelial function and subsequent recruitment of leukocytes, primarily T-lymphocytes, to developing lesions as a shared early step in the process of plaque formation in atherosclerosis and psoriasis. Lymphocyte extravasation has indeed been studied in detail with the intention to develop targeted therapies for psoriasis, but to date, none of the potential candidates was found to be sufficiently effective to validate development into a marketed drug . Meanwhile, many more shared mechanisms of atherosclerosis and psoriasis have been studied in detail.
Don’t Miss: How Does Salicylic Acid Help Psoriasis
Risk Factors For Developing Psoriasis
Both psoriasis and CD have genetic risk factors and are linked to an increased prevalence of each of these conditions among first-degree family members parents, children, and siblings. Some other risk factors for developing psoriasis, with or without IBD, include:
- Obesity
- Some viral and bacterial infections
Wendy Cantrell Crnp Dnp
Wendy Cantrell earned her Bachelor of Science and Master of Science degrees in Nursing from the University of Alabama at Birmingham in 1996 and 2000, and in 2011 she earned the title Doctor of Nursing Practice. Currently, she is an Assistant Professor of Dermatology in Birmingham, AL, and she is the Manager of the Clinical Research Division for the department. A prolific scholar, Dr. Cantrell has published many peer-reviewed articles on a number of dermatological issues during her 15 years of practice. With a family history of psoriasis, Dr. Cantrell has expressed her enthusiasm and dedication in pursuing new research, new drugs, and alternative therapies in order to enhance the quality of life for those afflicted with psoriatic disease.
Read Also: Is Exfoliating Good For Psoriasis
Supporting Acts: Indispensable Players In The Ensemble Of Psoriasis Immunology
Autoantigen presentation alone does not suffice to induce the psoriatic cascade in genetically predisposed individuals. Rather, costimulatory effects of various gene products orchestrate the activation of the actual autoimmune response. Such risk gene variants modulate inflammatory signaling pathways , peptide epitope processing and/or Th/c17 differentiation .
Table 1. Genetic factors implicated in psoriasis.
These genetic variations create costimulatory signals which modulate innate and adaptive immune mechanisms and shape the proinflammatory environment. In sum and in conjunction with the appropriate HLA molecules and autoantigens, they may eventually exceed the thresholds for activation and maintenance of pathogenic autoimmune and autoinflammatory responses in psoriasis . Likewise, regulatory mechanisms involving programmed death -1 signals have emerged recently as modulators of chronic inflammation in psoriasis . However, the complex interactions of various players are by no means fully understood. Therefore, they are listed here only as a whole.
The autoantigens described so far cannot fully explain the genesis of psoriasis. To give just one example of the latter notion: Psoriatic lesions can also occur in vitiligo foci that do not contain melanocytes . Alterations of resident cell types such as vascular endothelial cells or the cutaneous nervous system are also involved in the disease process . Further research is certainly needed here.
Symptoms Of Psoriatic Arthritis
The severity of the condition can vary considerably from person to person. Some people may have severe problems affecting many joints, whereas others may only notice mild symptoms in 1 or 2 joints.
There may be times when your symptoms improve and periods when they get worse .
Relapses can be very difficult to predict, but can often be managed with medicine when they do occur.
Don’t Miss: Is Apple Cider Vinegar Good For Psoriasis
Treatment Of Psoriasis As A Systemic Disease
Choice of psoriasis treatment is generally based on severity of skin disease and impact on quality of life, although clinicians should also consider the effects of different treatments on systemic inflammation and associated comorbidities. Of particular concern for patients with moderate-to-severe psoriasis is the observation that comorbid cardiovascular disease shortens the average lifespan by five to six years compared with patients with mild psoriasis.25,28 However, it is not yet known if reducing psoriasis severity can lengthen patient lifespan. Table 4 summarizes a population-based study evaluating differences in risks for associated comorbidities by psoriasis severity.29 Risk for many inflammatory comorbidities increases significantly with increasing psoriasis severity.
Because topical therapies and ultraviolet B phototherapy are applied locally to psoriatic lesions, these treatments may primarily have local effects. In contrast, some conventional oral systemic therapies, especially methotrexate, are associated with reductions in cardiovascular risk in patients with psoriasis and inflammatory arthritis.30,31 Possible effects of methotrexate on inflammation are being tested in an ongoing study , evaluating the effects of low-dose methotrexate on major adverse cardiac events incidence in approximately 7,000 patients with type 2 diabetes or metabolic syndrome with history of coronary artery disease.32
How Is Psoriasis Classified
Certain features of psoriasis can be categorised to help determine appropriate investigations and treatment pathways. Overlap may occur.
- Early age of onset < 35 years vs late age of onset > 50 years
- OMIM Online Mendelian Inheritance in Man
- Chularojanamontri L, Griffiths CE, Chalmers RJ. The Simplified Psoriasis Index : a practical tool for assessing psoriasis. J Invest Dermatol. 2013 133:195662. doi: 10.1038/jid.2013.138. PubMed PMID: 23807685.
- Feldman SR, Fleischer AB Jr, Reboussin DM, et al. The self-administered psoriasis area and severity index is valid and reliable. J Invest Dermatol. 1996 106:1836. doi:10.1111/1523-1747.ep12329912PubMed PMID: 8592072.
- Papp K, Gordon K, Thaçi D, et al. Phase 2 trial of selective tyrosine kinase 2 inhibition in psoriasis. N Engl J Med. 2018 379:131321. doi:10.1056/NEJMoa1806382. PubMed
- Fleming P. Tofacitinib: a new oral Janus kinase inhibitor for psoriasis. Br J Dermatol. 2019 180:1314. doi:10.1111/bjd.17323. PubMed
Also Check: Sulfur 8 Shampoo For Psoriasis
Psoriasis = An Autoimmune Disease
Its taken years, but most researchers now classify psoriasis as an autoimmune disease. At the very least, they recognize a link between the two.
Its not hard to understand why. Folks with psoriasis have overactive T cells your immune systems personal fighter jets just like folks with other autoimmune diseases.
During a psoriasis flare-up, your T cells attack healthy skin cells with a special protein called cytokines. The cytokines make your skin cells multiply super fast so much so that they start building up on top of each other. This forms those dry, scaly patches.
In 2017, researchers confirmed that cytokines are involved in triggering psoriasis, which was a major milestone in the development of treatments.
Since then, research continues to indicate that immunosuppressants help with psoriasis.
Things To Know About Psoriatic Arthritis
Learn more about what it means to have psoriatic arthritis.
1. PsA Is an Autoimmune Disease
2. It Has Ups and Downs, Called Flares
3. It Can Be a Master of Disguise
4. It Has Distinguishing Features
5. It Affects Up to a Third of People with Psoriasis
6. Its Gender Neutral
7. It May be Hereditary
8. Its Not Contagious
9. It Isnt Just About Your Joints
10. You May Not Look Sick
11. Effective Treatment is Available
Hello,
Also Check: What Type Of Doctor Treats Plaque Psoriasis
Therapies For Pso And Ad Have Limitations Related To Safety Tolerability Convenience And Price
> 50% of PsO and > 90% of AD sufferers are dissatisfied with current treatment options1,2
Topicals
1 Alcusky, M., et al. Dermatol Ther 7, 463483 . 2 Okubo, Yukari, et al. Journal of Dermatological Treatment 31.8 : 821-830.
Simply put, there remains a significant need for oral medicines that are effective, safe, well-tolerated and affordable for the millions of people suffering from psoriasis and atopic dermatitis around the globe, especially for people with mild and moderate disease.