What A Dermatologist Evaluates
- Risk for developing other medical conditions
- Response to past treatments for psoriasis
- Concerns about how psoriasis affects your life
- Other medications
Your dermatologist can see the signs of psoriasis during a physical examination of your skin, scalp, and nails, and can take your medical history and symptom history to make an accurate diagnosis.
They will ask you about:
- Symptoms, such as red bumps or itchy skin
- Joint problems, such as pain and swelling or stiffness when you wake up
- Blood relatives who have psoriasis
- Recent changes in your life, such as an illness or increased stress
Before Stopping Psoriasis Treatment Talk With Your Dermatologist
Because psoriasis is a lifelong disease, its understandable that you may want to stop treatment at some point. Alwaystalk with your dermatologist before you stop treatment.
Some treatments can be stopped immediately. Others need to be discontinued slowly to prevent psoriasis from worsening .
When psoriasis rebounds, it may become a more serious type of psoriasis. A person who had plaque psoriasis may suddenly have pustular psoriasis or erythrodermic psoriasis.
The best way to prevent a rebound is to talk with your dermatologist. Your dermatologist can tell you whether you can stop the treatment abruptly or slowly. Sometimes, the best approach is to gradually switch to another treatment.
Emotional Impact Of Psoriasis
Because of the effect that psoriasis can have on physical appearance, low self-esteem and anxiety are common among people with the condition. This can lead to depression, especially if the psoriasis gets worse.
Your GP or dermatologist will understand the psychological and emotional impact of psoriasis, so talk to them about your concerns or anxieties.
Read Also: What Does Beginning Psoriasis Look Like
Can Psoriasis Go Away
Psoriasis is a skin disease that develops due to changes in genetic makeup, and most often, it is passed from your parents . It may also occur due to changes in the immune system, autoimmune response, in which your own antibodies start attacking the cells of your body.
Psoriasis is a chronic inflammatory condition that has no definite cure and only the symptoms can be managed. At times, treatment can make psoriasis symptoms disappear and give you clear skin for a while.
This symptom-free period is referred to as remission. A remission is followed by the reappearance of the symptoms and this period is known as relapse.A remission can last for months or years ranging from one to 12 months.
The course of psoriasis is unpredictable, varying considerably among patients, so it’s impossible to know if you will have a remission and how long it will last.
Are Cosmetic Procedures Safe To Get
Noninvasive cosmetic procedures are more popular now than ever. Injectables like Botox can improve the appearance of wrinkles, while fillers restore lost volume. Lasers can be used to even skin tone and texture, and even eliminate unwanted blood vessels or hair. These procedures are safe for people with psoriasis.
If youre interested in a cosmetic procedure, speak to your doctor about whether its right for you. In some cases, your doctor may want to hold or adjust your medications. Its important that theyre aware of your full medical history and current medications.
Don’t Miss: Does Psoriasis Come Back In The Same Spots
Treating A Child Requires Special Considerations
Before treating a child, a dermatologist carefully considers:
-
Whether treatment is necessary
-
The risks and benefits of potential treatments
Having a visible skin disease can be very stressful. Psoriasis on the scalp can be especially troubling for a child or teenager, especially if it causes hair loss. A child can feel embarrassed and start to withdraw from others. Constant itch and pain can make it difficult to concentrate during school and to sleep at night.Some children, however, are not bothered by their psoriasis, especially if it is covered by clothing and causes little itch or pain. In that case, treatment may be unnecessary. Before treating a child, a dermatologist also looks at the short- and long-term effects of treating psoriasis. When treating a child, its important to anticipate what treatment may be required in the future. If treatment is needed now, a dermatologist can develop a treatment plan that minimizes side effects and maximizes the beneficial effects of treatment.
Related AAD resources
Adjusting Your Psoriasis Treatment Plan With Age
Many medications to treat psoriasis are considered safe as you get older, including corticosteroids, vitamin D analogues, tazarotene, acitretin, , methotrexate, and some biologics. Your doctor may be more cautious with topical steroids though, because both aging and topical steroids cause skin to thin. Let your doctor know if your skin appears more transparent or if it bruises easier, has purple spots, or has visible blood vessels.
Most important, make sure your dermatologist knows about every medication youre taking and any other diagnoses youve received. Some psoriasis medications arent safe for people with liver disease, kidney disease, or heart failure, all of which are more common in people over 65. Other medications, including biologics, may not be appropriate if you have certain infections, including hepatitis B, which is more common in older adults who were born before a hepatitis B vaccination existed.
Cancer is also more common with age. Its important to let your doctor know if youve been diagnosed with any kind of cancer. Your dermatologist needs to know, because it will affect treatments for psoriasis, says Unwala.
Read Also: Is Eating Honey Good For Psoriasis
Does Aging Skin Affect Psoriasis
As the skin ages, collagen and elastic fibers weaken and the skin gets thinner. This makes it sensitive to trauma, leading to easier bruising and even open sores in severe cases.
This is a challenge for anyone, but it can be even more challenging if you have psoriasis. Psoriasis plaques that occur on weakened skin can lead to pain and bleeding.
If you have psoriasis, its important to protect yourself from the sun because UV exposure is known to cause skin damage. You also must be careful when using topical steroid creams to treat psoriasis. Overuse of steroids is associated with skin thinning and development of stretch marks, especially with long-term use over years.
What Is Psoriasis Symptoms Causes Diagnosis Treatment And Prevention
Psoriasis is an autoimmune disease that causes plaques, which are itchy or sore patches of thick, dry, discolored skin.
While any part of your body can be affected, psoriasis plaques most often develop on the elbows, knees, scalp, back, face, palms, and feet.
Like other autoinflammatory diseases, psoriasis occurs when your immune system which normally attacks infectious germs begins to attack healthy cells instead.
Also Check: Does Shea Butter Help With Psoriasis
Generalised Pustular Psoriasis Or Von Zumbusch Psoriasis
This causes pustules on a wide area of skin, which develop very quickly. The pus consists of white blood cells and is not a sign of infection. The pustules may reappear every few days or weeks in cycles. During the start of these cycles, von Zumbusch psoriasis can cause fever, chills, weight loss and fatigue.
What Are The Clinical Features Of Psoriasis
Psoriasis usually presents with symmetrically distributed, red, scaly plaques with well-defined edges. The scale is typically silvery white, except in skin folds where the plaques often appear shiny with a moist peeling surface. The most common sites are scalp, elbows, and knees, but any part of the skin can be involved. The plaques are usually very persistent without treatment.
Itch is mostly mild but may be severe in some patients, leading to scratching and lichenification characterised by thickened leathery skin and increased skin markings. Painful skin cracks or fissures may occur.
When psoriatic plaques clear up, they may leave brown or pale marks that can be expected to fade over several months.
Read Also: Guttate Psoriasis How Long Does It Last
What Is Psoriasis Epidemiology
Who gets psoriasis more often: women or men? And do your chances of developing this long-term skin condition go up based on your race, ethnicity, or age?
The field of epidemiology can help us answer these questions. Itâs a branch of science that looks at how often diseases affect different groups of people and why. Medical experts can then use the information to plan and assess ways to prevent or manage diseases.
Psoriasis affects an estimated 7.5 million to 8 million people in the United States and about 125 million worldwide. Your immune system and your genes both play a role in causing it. Hereâs a closer look at who tends to get this condition.
Are There Popular Skincare Products Or Ingredients To Avoid Ones To Use

Its important to take special care of your skin if you have psoriasis. I generally tell my patients to steer clear of products with drying alcohols, fragrances, and sulfates. All of these can cause skin irritation and dryness.
Trauma to the skin can lead to a psoriasis breakout, known as the Koebner phenomenon. So its important to avoid activities or products that can cause irritation.
I tell my patients to use gentle, hydrating, non-soap cleansers that wont disrupt the skin barrier. Shower with lukewarm water for 10 minutes or less, and moisturize the skin after patting dry.
If you have thick scales on your scalp or other parts of your body, skincare products that contain salicylic acid may be helpful. Salicylic acid is a beta hydroxy acid that exfoliates the skin to help remove the scale on psoriasis plaques.
You May Like: Neostrata Psorent Psoriasis Topical Solution
Take A Whole Health Approach
When you think about psoriasis and your health, you might focus only on your skin. But you need to take a broader look at your health as you age. Psoriasis can make you more likely to get some kinds of cancer, such as lymphoma and non-melanoma skin cancer. It also can raise your risk of low bone density conditions like osteopenia and osteoporosis. And the same is true for type 2 diabetes and metabolic syndrome .
About 30% of people who have psoriasis also get psoriatic arthritis. Thatâs a condition that causes stiff and swollen joints and other issues like fatigue. Psoriatic arthritis often gets worse over time, especially if itâs not treated.
âIf you have psoriasis, itâs especially important to work closely with all your doctors,â says Shari Lipner, MD, PhD, a dermatologist at Weill Cornell Medicine and New York-Presbyterian Hospital in New York.
If a dermatologist or rheumatologist treats your psoriasis, make sure your primary care physician or family doctor knows what kinds of psoriasis treatments youâre getting and have gotten in the past. Some psoriasis medications may make you more likely to have health problems like infections or cancer. So your doctor may want to keep a closer watch on you. And some medications used to treat arthritis, heart disease, and other conditions may make psoriasis worse.
What Every Senior Should Know About Psoriasis
Aug 2, 2018 | Health & Wellness, Senior Safety |
Psoriasis, a condition that causes the body to make new skin cells in days rather than weeks, causes thick, scaly patches that often appear on the knees, elbows, lower back, scalp, nails, and joints.
Symptoms tend to worsen with age, and psoriasis can be linked to other conditions that affect seniors, including type 2 diabetes, inflammatory bowel disease, and heart disease. Though not contagious, senior psoriasis is one of the more serious of skin diseases. It often progresses into a chronic condition, and theres no known cure.
You May Like: Home Remedies For Psoriasis On Your Head
Patient Disposition And Characteristics
Of the 12,090 patients enrolled in the registry, 7511 were eligible for inclusion in this analysis. The median duration of follow-up as of the data cut-off date for this analysis was 4.17 years . Patients with EOP accounted for 72.9% of the total sample size . Most patients in the study population were enrolled at sites located in North America . Mean age was 44.8 years in the EOP group and 60.2 years in the LOP group. More than half of the patients in each group were male , and most patients were White . Most patients had a diagnosis of plaque psoriasis other diagnoses, which were not mutually exclusive, included guttate, erythrodermic, pustular, and/or inverse psoriasis. Baseline disease severity for the overall population was moderate in most patients, as measured by PGA and %BSA more than one-third of patients had a self-reported history of psoriatic arthritis.
Table 1 Demographic and patient characteristics at enrollment by age of onset
Psoriasis Signs In Seniors
There are eight different types of senior psoriasis that may develop, each with their own symptoms.
Plaque psoriasisThe most-common form accounts for about 80 to 90 percent of people with senior psoriasis. Symptoms include:
- Patches of thick, raised skin called plaques
- Scale over some plaque
- Plaques of different sizes
- Smaller plaques joined together to form larger ones
Guttate psoriasisThis tends to appear after infection. Patches on the skin appear:
- Small and scaly
- Salmon to pink in color
- Temporary, often clearing in a few weeks or months without treatment
Inverse psoriasisThis often develops in areas where skin touches skin Symptoms include:
- Smooth, red patches of skin that look raw
- Little, silvery-white coating
- Sore or painful
Pustular psoriasisThis type causes pus-filled bumps that usually appear on the feet and hands. Symptoms include:
- Red, swollen skin dotted with pus-filled bumps
- Extremely sore or painful
- Brown dots after the pus-filled bumps dry
Pustular psoriasis This type is serious and life-threatening, causing pus-filled bumps to develop. Call your doctor immediately if these symptoms appear:
- Dry, red, and tender skin
- Pus-filled bumps covering most of the skin, often developing within hours
- Smooth, glazed surface when dried skin peels off
- A new crop of bumps may appear in a few days or weeks
Erythrodermic psoriasisSerious and life-threatening, this type of senior psoriasis needs immediate medical care. Symptoms include:
Also Check: Uv Light Box For Psoriasis
Metabolic Syndrome And Heart Disease
According to a review published in JanuaryFebruary 2018 in Clinical Dermatology, numerous studies have strongly linked psoriasis to metabolic syndrome, a collection of conditions that includes abdominal obesity, high blood pressure, high cholesterol, type 2 diabetes, insulin resistance, and nonalcoholic fatty liver disease. The risk of being diagnosed with metabolic syndrome increases with age, and having it ups the risk of heart disease, according to a study published in May 2018 in the journal Translational Research.
We can consider as a risk factor for heart disease, just as we think of family history, smoking, and gender as risk factors, says Unwala. Metabolic syndrome, she explains, involves inflammation in the bloodstream, and psoriasis is an inflammatory disease. Certain drugs used to treat metabolic syndrome, including blood pressure medications, may also trigger psoriasis flares.
The good news is that treating psoriasis can help reduce your risk of heart disease. Treatment of skin results in overall improvement of health, which is especially important for an older population at higher risk of heart disease, says Unwala. Making lifestyle changes, such as eating a healthy diet and exercising regularly, can also help keep your heart healthy and lower your risk of metabolic syndrome.
How Is Psoriasis Diagnosed
Doctors usually diagnose psoriasis by examining the skin, scalp, and nails. They’ll also ask whether someone else in your family has psoriasis and if you recently had an illness or started taking a new medicine.
Rarely, doctors might take a skin sample to check more closely. A can tell the doctor whether it’s psoriasis or another condition with similar symptoms.
Also Check: Crohn’s Disease And Psoriasis Treatment
We’re On This Journey With You
Although psoriasis can start at any age, most people experience their first flare between the ages of 15 and 35.
Approximately one-third of those who get psoriasis are under 20 years old when the disease first surfaces. Every year, roughly 20,000 children under 10 are diagnosed with psoriasis. It may take time to get a correct diagnosis, as psoriasis is sometimes confused with other skin diseases like eczema and diaper rash.
Quality Of Life And Psychological Aspects Of Psoriasis

Although psoriasis generally does not affect survival, it certainly has a number of major negative effects on patients, demonstrable by a significant detriment to quality of life. Despite this, most clinical trials of new treatments for psoriasis focus on objective physical measures for the primary endpoint of efficacy. This is incongruous as it is the improvement in quality of life that patients and physicians rely upon when selecting treatment. Impairment of quality of life has been highlighted particularly by the work of Finlay. Patients with psoriasis have a reduction in their quality of life similar to or worse than patients with other chronic diseases, such as ischaemic heart disease and diabetes. That patients with psoriasis feel stigmatised by the condition is well established. This of itself contributes to everyday disability leading to depression and suicidal ideation in more than 5% of patients.
Furthermore, quality of life measures take into account the effect of the treatment on the patient. Quality of life data fulfils the role of measuring the intangible changes in a patients life that determine treatment success. For a clinically meaningful change to exist for psoriasis and other chronic, non-life threatening diseases, a treatment must provide an improvement in the patients quality of life. In an attempt to provide an holistic assessment of overall disease severity, a specific tool has been developedthe Salford Psoriasis Index :
Recommended Reading: Best Shampoo For Plaque Psoriasis
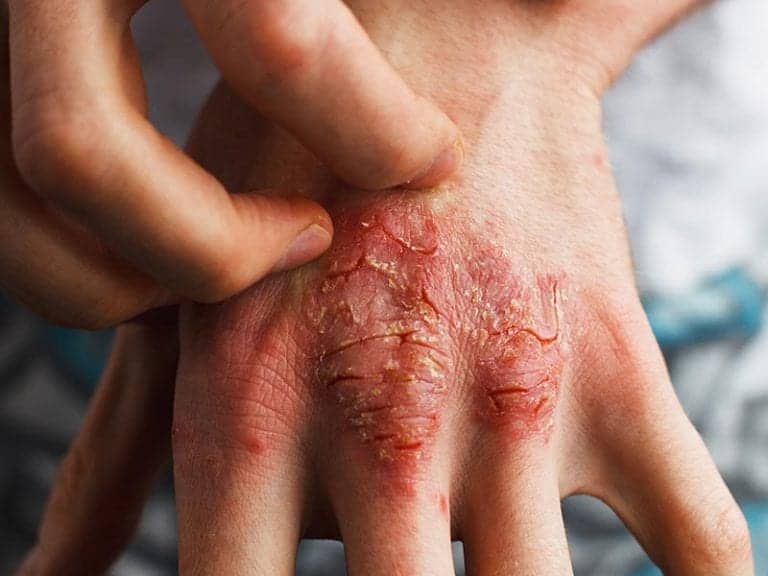
Is It Psoriasis Or Eczema
Like psoriasis, eczema is a very itchy skin condition. In fact, eczema usually results in a more intense itch than psoriasis. Scratching causes inflammation of the skin, leading to a worsening of the eczema. Scratching can also cause a secondary bacterial infection.
Eczema is not a specific disease, but rather a term referring to a group of rash-like conditions. The most common type of eczema is caused by a reaction to irritants, like detergents, soaps, or household cleansers.
Eczema often shows up on the back of the knees or the inside of the elbows.
Eczema can affect anyone and affects children more than psoriasis does.