Inflammatory Bowel Diseases And Psoriasis
There are several pathophysiological links between psoriasis and IBD. Elevated concentrations of cytokines in serum and tissues are present both in psoriasis and IBD, and agents that inhibit their action often improve both conditions. Approximately 15% of patients with IBS are diagnosed with cutaneous EIM of IBD .
Psoriasis affects approximately 10% of general population and may be characterised by the involvement of several organs, leading to arthritis, cardiovascular diseases, chronic kidney disease, diabetes and metabolic syndrome, the so-called psoriatic march.
The incidence of IBD is higher in populations with psoriasis, psoriatic arthritis and ankylosing spondylitis . The risk of UC in psoriatic patients is 1.6-times higher than in the general population . There are several hypothetic explanations for this phenomena including genetic predisposition or environmental factors with growing evidence for the deleterious role of T helper 17 cells in IBD and psoriasis . Psoriasis is more frequent in patients with CD in a study by Lee et al., psoriasis was present in 9.6% patients with CD compared to 2% controls, and patients with CD were more likely to have a first-degree relative with psoriasis . Systemic inflammation is responsible for the severity and chronicity of psoriasis, as well as for the development of concomitant diseases, e.g. cardiovascular diseases or metabolic syndrome.
Whats The Connection Between Leaky Gut And Psoriasis
Theres little scientific evidence to link leaky gut syndrome to any health condition, including psoriasis. However, this doesnt mean the syndrome or the link doesnt exist.
When proteins leak from the gut, the body recognizes them as foreign. The body then attacks them by triggering an autoimmune, inflammatory response in the form of psoriasis. Psoriasis is an autoimmune disease that causes an inflammatory skin response. Because of this, its within the realm of possibility that the two conditions are related.
How Is Ibd Linked To Plaque Psoriasis
Psoriasis and IBD are both conditions with symptoms that are caused by inflammation that is due to an overreaction of the immune system3. Researchers believe that there is a genetic link between the two conditionsthat certain families carry specific genes that affect the immune systems functioning and make members of those families more likely to develop both conditions5.
Read Also: Psoriasis Spots All Over Body
Study Population: Ibd Patients
The IBD group included patients with a diagnosis of CD or UC, defined according to current guidelines. For each patient, clinical characteristics, including demographic data, gender, age, risk factors for IBD and characteristics of IBD were reported in a common database. Available data regarding family history of psoriasis were also reported.
Patients were enrolled according to the following inclusion criteria: 1] diagnosis of IBD made according to current clinical, histological or radiological criteria, 2] regular follow up at our referral IBD centre 3] compliance with dermatological assessment 4] indication for dermatological assessment, given by the IBD-dedicated gastroenterologist in relation to the presence of any type of skin lesion, including psoriasis, deserving further evaluation 5] available demographic and clinical characteristics reported in clinical records.
Psoriasis Increases The Risk Of Concurrent Inflammatory Bowel Disease: A Population
Correspondence Address
| How to cite this article: Lee JY, Kang S, Bae JM, Jo SJ, Koh SJ, Park HS. Psoriasis increases the risk of concurrent inflammatory bowel disease: A population-based nationwide study in Korea. Indian J Dermatol Venereol Leprol 2019 85:145-152 |
Abstract
Background:Aim:Methods:Results:Limitations:Keywords:
Introduction
Methods
This study was exempt from approval by the Institutional Review Board.
Data source
We used the database of the Health Insurance Review and Assessment Service, an independent Government agency responsible for conducting reviews of health claims data and evaluating the appropriateness of medical benefits submitted by healthcare organizations. Health Insurance Review and Assessment Service’s claims data include all medical utilization covered by insurance program of entire Korean population. National Health Insurance program covers the majority of the population and Medical Aid manages the remaining 3% .
Study population and operational definitions of psoriasis and inflammatory bowel disease
Study outcomes
The primary endpoint was annual prevalence of inflammatory bowel disease in patients with psoriasis and the general population, respectively. The secondary outcome was risk of inflammatory bowel disease in psoriasis subgroups according to age, sex, insurance type and psoriasis severity.
Statistical analysis
Results
Characteristics of patients with psoriasis and the general population
| Figure 1: |
Discussion
Recommended Reading: Natural Remedies For Plaque Psoriasis
The Psoriatic Liver And Bile
I mentioned that my bowel bypass patients had horrendous liver disease, including frank cirrhosis, which did not show up on routine liver function tests. I postulated that the syndrome did not occur until the liver had been hammered by high concentrations of PGs in the portal and lymphatic circulation from the gut.22 I think that a similar mechanism is at work in psoriasis. Nonalcoholic fatty liver disease is present in 48% to 59% of psoriatics.71 A study has shown that the severity of
Topical And Light Therapy Treatments For Psoriasis
There are several treatments for psoriasis, including light therapy, topical treatments, and medications. In many cases, more than one treatment might be used at the same time to combat the symptoms of psoriasis. Generally, topical therapies might be tried first, before moving on to light therapy or systemic medications.
- Topical treatments. There are various types of creams and ointments that may be used for psoriasis, both over the counter and prescription. Some of the active ingredients include corticosteroids, vitamin D, retinoids, anthralin, calcineurin inhibitors , salicylic acid, and coal tar. In some cases, moisturizers might also be used to combat dryness.
- Light therapy. Light that contains ultraviolet A and ultraviolet B may also be used to treat psoriasis. This is usually used along with other treatments. Sunlight from outside might be used, for short periods of time. Ultraviolet rays can also be administered via phototherapy with a light panel, box, or booth. In severe cases, a medication that makes the skin more sensitive to ultraviolet light might also be used at the same time as light therapy in order to make it more effective. A type of laser is also sometimes used because it can target specific areas on the body with a stronger dose of ultraviolet B light.
Read Also: How To Diagnose Scalp Psoriasis
Psoriasis And Celiac Disease
When you have celiac disease, you can’t digest gluten, a protein in wheat, rye, and barley. Celiac disease can damage your small intestine and prevent it from absorbing key nutrients.
The chance of getting celiac disease is nearly 3 times higher among people with psoriasis. About 4 of every 100 have it. Research shows that the higher the levels of specific antibodies related to celiac disease, the worse psoriasis tends to be.
Medical Treatment For Uc
Table 3. Evidence from clinical trials for class of therapeutic options for ulcerative colitis.
Due to the ineffectiveness of IL-17i for CD, there have not been trials for their use in UC. As for IL-23i, there is an ongoing phase II/III trial of RZB for UC .
In contrast to CD, the JAKi, TOF, was approved for use in moderate-to-severe UC based on three pivotal phase III OCTAVE studies, showing a significantly greater percentage of clinical remission at week 8 for induction, and remission at week 52 for maintenance in TOF compared to placebo group . UPA met the clinical remission, endoscopic improvement and histological improvement endpoints in a phase III induction trial for moderate-to-severe UC .
Don’t Miss: Remedios Para La Psoriasis Cuero Cabelludo
Causal Association Between Inflammatory Bowel Disease And Psoriasis: A Two
- 1Department of Dermatology, Xiangya Hospital, Central South University, Changsha, China
- 2National Clinical Research Center for Geriatric Disorders, Xiangya Hospital, Central South University, Changsha, China
- 3Department of Spine Surgery and Orthopaedics, Xiangya Hospital, Central South University, Changsha, China
Background: Previous observational studies have found an association between inflammatory bowel disease and psoriasis. Using the mendelian randomization approach, we aim to determine whether there was a causal association between IBD and psoriasis.
Methods: We performed a two-sample MR with the genetic instruments identified for IBD and its main subtypes, Crohns disease and ulcerative colitis , from a genome-wide association study involving 25,042 cases with an IBD diagnosis and 34,915 controls. Summarized data for psoriasis were obtained from different GWAS studies which included 4510 cases and 212,242 controls without psoriasis. Causal estimates are presented as odds ratios with 95% confidence intervals .
There appears to be a causal relationship between IBD and psoriasis, especially for PsA, but for psoriasis and IBD, only total psoriasis and PsA were associated with CD. Understanding that specific types of psoriasis and IBD constitute mutual risk factors facilitates the clinical management of two diseases.
Healing The Gut To Treat Psoriasis
All disease starts in the gut. This saying may sound like a new fad, but in fact, this is quoted from Hippocrates himself who proposed this not ten years ago, a hundred years ago, but thousands of years ago! Praised as one of the most influential figures in medicine and healing, Hippocrates upheld the theory of autointoxication, which claimed that by-products of incomplete digestion may poison the body and, therefore, cause disease. Intrigued? Read on.
Lets talk about psoriasis the prototype chronic inflammatory disease in dermatology. If Hippocrates theory is true, how does this apply to psoriasis? As dermatologists, we rarely discuss gut issues with psoriasis patients. We are trained to target the end-result inflammation with topicals after topicals, followed by systemic immune-suppressants and biologics. But what if we turned our focus to the cause of the inflammation? The lessons that Dr. Haines Ely shared in his talk Is Psoriasis A Bowel Disease? presented at the 2020 Integrative Dermatology Symposium were truly enlightening.
A new way of treating psoriasis
Okay, raise your hand if you like spending hours on biologics prior authorizations and handling patient complaints about medication cost. No one! Wouldnt it be amazing to recommend systemic treatments that work by reducing the overall inflammation, without the hassle of involving insurance companies and chronic lab monitoring? If your answer is yes, youre gonna love this!
Endotoxemia, the culprit
Read Also: Is Psoriasis Warm To The Touch
How Common Is Ibd Among People With Psoriasis
Studies suggest that people with psoriasis have a higher risk of developing IBD during their lifetimes3. Statistically, the two conditions occur more often in people who have been studied than they would if the two diseases were not somehow related. For example, one recent study found that 1 in 10 women with psoriasis had developed an IBD4. Research also suggests that people who have both psoriasis and psoriatic arthritis had an even higher risk of inflammatory bowel disease than people who have psoriasis but no psoriatic arthritis diagnosis5.
How Is Inflammatory Bowel Disease Linked To Psoriasis
- print page
- Bookmark for later
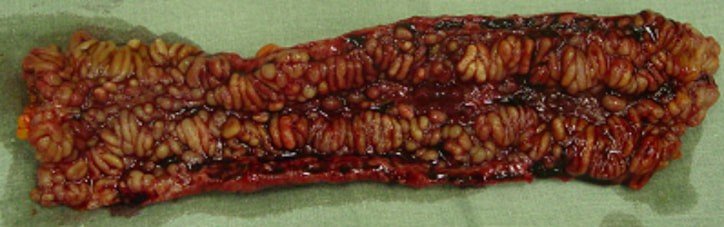
Inflammatory bowel disease is the name for a set of conditions in which chronic inflammation inside of the digestive tract can cause many different symptoms, including abdominal pain, diarrhea, and cramping1. The most common forms of IBD are called ulcerative colitis and Crohns disease.
Like psoriasis, IBD is a chronic inflammatory condition. Symptoms may get better or even disappear for longer periods of time, but the condition is not curable and symptoms return or flare-up over time.
Recommended Reading: Best Dead Sea Products For Psoriasis
A Common Inflammatory Pathway
As researchers discover more about the inflammatory pathways of IBD and psoriasis, some overlap between the two diseases is being uncovered . Crohn’s disease and psoriasis are both considered Th1 mediated conditions. Th1 is a helper cell that mounts an inflammatory response when the body is invaded by a foreign substance such as a parasite, bacteria, or virus. Ulcerative colitis is considered a Th2-like mediated condition. Th2 cells are activated when there is a bacteria, allergic response, or toxin present. As the role of these T cells is better understood in regards to the development of IBD and psoriasis, it could lead to the creation of more effective treatments for these diseases.
Management Of Psa With Consideration Of Extra
Given the heterogeneity in manifestations, enhanced collaboration between disciplines are required to deliver optimal care for PsD . While collaborations between rheumatologists and dermatologists are increasing , collaborations with gastroenterologists and ophthalmologists have traditionally been weaker. Apart from setting up combined clinics, collaborations between disciplines can take other forms as determined by needs and circumstances of different institutions. Minimally, identifying key stakeholders specializing in the care of PsA patients and keeping them in close communication over the management plan is essential. These collaborations serve both clinical and educational needs. Close collaboration between the various disciplines will help in early diagnosis of the various manifestations, providing expert advice on choice of therapeutics to create a patient-centric, individualized care plan for the heterogeneous manifestations. Often, the therapeutics will need to cover multiple domains, but the predominant domain should drive the therapeutic option of choice in the shared decision-making process.
All in all, detailed considerations of all domains and extra-articular manifestations are necessary to formulate the best therapeutic option. Multi-disciplinary collaborative care models are advocated for optimal care for patients with PsA, and especially so for those who present with co-morbidities.
You May Like: What Is The Best Shampoo For Psoriasis Of The Scalp
Correlations Between Psoriasis And Inflammatory Bowel Diseases
Nevena Skroza
1Department of Dermatology Daniele Innocenzi, A. Fiorini Hospital, Sapienza University of Rome, Via Firenze, Polo Pontino, 04019 Terracina, Italy
Abstract
For a long time the relationship between inflammatory bowel diseases and psoriasis has been investigated by epidemiological studies. It is only starting from the 1990s that genetic and immunological aspects have been focused on. Psoriasis and IBD are strictly related inflammatory diseases. Skin and bowel represent, at the same time, barrier and connection between the inner and the outer sides of the body. The most important genetic correlations involve the chromosomal loci 6p22, 16q, 1p31, and 5q33 which map several genes involved in innate and adaptive immunity. The genetic background represents the substrate to the common immune processes involved in psoriasis and IBD. In the past, psoriasis and IBD were considered Th1-related disorders. Nowadays the role of new T cells populations has been highlighted. A key role is played by Th17 and T-regs cells as by the balance between these two cells types. New cytokines and T cells populations, as IL-17A, IL-22, and Th22 cells, could play an important pathogenetic role in psoriasis and IBD. The therapeutic overlaps further support the hypothesis of a common pathogenesis.
1. Introduction
2. Epidemiological Correlations
Families affected by Crohns disease or psoriasis are also more likely to be affected by other immune-mediated diseases.
3. Genetic Correlations
Alter The Bowel Flora Toward Normal
Treatment of psoriasis begins with altering the bowel flora toward normal. American gastroenterologists dont believe in testing for Blastocystis hominis, but they do believe in H pylori. If either of these organisms are present, the patients psoriatic plaques will itch. If itching is present I will test for and treat H pylori. B hominis can be occult. It is known to produce intestinal inflammation, arthritic clinical manifestations, fatigue, flatulence, and abnormal bowel habits.47 It can be
Recommended Reading: How To Cure Psoriasis Arthritis Naturally
Psoriasis And Inflammatory Bowel Disease As One Unit
Having psoriasis gives a patient a 1.75-fold increased odds of developing ulcerative colitis and a 1.70-fold increased odds of developing Crohn’s disease.
Psoriasis and IBD share pathophysiologic commonalities. They both share genetic susceptibility loci on chromosome 6p21. Interleukin 23 and IL-12 play important roles in the pathogenesis of both psoriasis and IBD. IL-23 causes the downstream differentiation and activation of helper TH17 helper lymphocytes. These helper t cells produce IL17 that plays an important role in both IBD and psoriasis. In psoriasis, IL-17 induces hyperproliferation of keratinocytes, maturation of myeloid dendritic cells, and recruitment of neutrophils and macrophages in psoriatic lesions. In IBD there is also increased expression of IL-17 in both the serum and the gut suggesting its importance in the disease pathogenesis.
Another commonality between the skin and gut is that they both have an abundant blood supply and are exposed to microbiota that can stimulate the immune system. Bacteria can affect the physiology and immune response of the epithelium of the skin and gut by regulating biological metabolites. This can lead to immune dysregulation with elevated cytokine levels and the activation and differentiation of T cells.
REFERENCEFu Y, Lee CH, Chi CC. Association of Psoriasis With Inflammatory Bowel Disease: A Systematic Review and Meta-analysis. JAMA dermatology. 2018 Dec 1 154:1417-23.
What Are The Causes And Symptoms Of Ibd
The exact causes of IBD are still unknown. However, researchers think that they are probably caused by a combination of genetics, the environment, and microorganisms in the gut . The current theory is that these diseases develop when a persons immune system has the genetic tendency to overreact to harmless microorganisms in the gut1. This reaction causes chronic inflammation anywhere along the digestive tract. The differences between Crohns disease and ulcerative colitis have to do with the location and severity of the symptoms2.
Read Also: Psoriasis Medications Covered By Medicare
Psoriasis And Inflammatory Bowel Disease: Links And Risks
Accepted for publication 7 April 2016
20 July 2016Volume 2016:6 Pages 7392
Introduction
Psoriasis and the group of inflammatory bowel diseases are chronic, inflammatory, organotropic conditions. The former affects the skin of 2%3% of the population, with hyperproliferation of keratinocytes, impaired epidermal barrier function at the sites of skin lesions, and skin infiltration by activated inflammatory cells.1 Ulcerative colitis and Crohns disease are the two most prevalent representatives of the IBD group. UC usually affects the rectum and may extend to the colon, with restriction of the inflammatory process to the mucosa and submucosa layers, while CD can affect any site of the digestive tract, with segmentary distribution of the lesions and inflammatory infiltration of all intestinal wall layers.2
Immune dysregulation, determined by genetic predisposition and environmental assaults, underlies all three conditions. A coincidence of psoriasis and IBD has been observed in various clinical settings: they can appear as concomitant disease events in the same patient or as paradoxical treatment-related adverse events.3,4
Diseases coincidence
Psoriasis and IBD cluster at all genetic levels of human populations, ie, they share the same geographic/ethnic, kindred, and patient niches. These diseases are more frequent in Northern Europe and North America compared to most regions of Africa, Asia, and the Middle East .57
Genetic collation
Microbiota
Comorbidities
Discussion