How Are Treatment For Psoriatic Arthritis And Rheumatoid Arthritis Different
Treatments for PsA and treatments for RA are more alike than they are different. Both involve immunosuppressants, which turn off pieces of the immune system that are too active.
According to 2021 RA guidelines, the first-choice treatment for RA is methotrexate. If methotrexate isnt enough to control inflammation, then providers add a biologic medication, like a TNF-alpha inhibitor.
Generally speaking, the same holds true for PsA. But the 2018 PsA guidelines mention that going straight to a biologic instead of trying methotrexate first might be a better choice for some.
After methotrexate and TNF-inhibitors, treatment options for PsA and RA can go down different paths. Thats because different parts of the immune system are overactive in each condition. For example, a biologic like Cosentyx might work great for PsA, but it wont be helpful for RA. On the other hand, a biologic like Actemra might work great for RA, but its no good for PsA.
If all of this sounds confusing, thats because it is. But try not to worry. Your rheumatologist specializes in these medications, and theyll work with you to find the treatment thats best for your specific case.
Psoriasis Vs Psoriatic Arthritis: What Sets Them Apart
Distinguishing between two separate but related conditions
The medical world can be confusing from a patients perspective. Diseases that sound related might not be and diseases that sound totally different might be. In the case of psoriasis vs psoriatic arthritis, its not really any simpler. Based on the names of the conditions, you might assume theyre somehow related, and thats true. However, there are also considerable differences to set them apart.
If you or a loved one have been diagnosed with either condition, youre likely wondering about the connection between these two conditions. In todays blog well break down exactly how they are related, and how they arent, to help you move forward with a practical understanding of the two conditions.
Psoriatic Arthritis Or Rheumatoid Arthritis
Dr. Cassandra Calabrese explains the similarities and differences between PsA and RA.
Prominent morning stiffness, swelling, redness, and warmth of the joints â these are all indicators that you may have inflammatory arthritis. The question is, what kind?
While rheumatoid arthritis might come to mind first, psoriatic arthritis is more common than you might think. Among those living with psoriasis, about 1 in 3 will develop PsA, and it can happen at any age.
Both RA and PsA result in inflammation inside the lining of the joints, and both involve the immune system. A number of key differences, however, can help health care providers distinguish one from the other. Cleveland Clinic rheumatologist Cassandra Calabrese, D.O., discussed the two diseases and how they differ.
Diagnosis and Differentiators
There is currently no blood test for PsA, but in general, the joint pain and swelling for PsA would be asymmetric, involving potentially fewer joints, and typically would involve different joints than RA, says Dr. Calabrese.
âNot every patient with psoriasis and joint pain has psoriatic arthritis, but if there’s new joint pain, worsening joint pain, or joint pain that’s interfering with daily activities, then that patient should see a rheumatologist,â she recommends.
Diagnosis for RA is often more straightforward. âThe majority of cases have positive autoantibodies, so blood markers called rheumatoid factor and anti-CCP antibody that test positive,â says Dr. Calabrese.
Read Also: How To Get Rid Of Psoriasis Overnight
Are Treatment Plans All That Different
Despite presenting very differently, there are many of the same treatment options for PsO and PsA, including nonsteroidal anti-inflammatory drugs and biologic drugs like Enbrel , Cosentyx , and Humira . There are, however, a few variances. For instance, as Dr. Friedman explains, unlike psoriasis, psoriatic arthritis typically doesnt respond to topical creams, as it primarily affects the joints, and creams are unable to effectively penetrate the dermis and reach the nerves underneath.
PsA needs to be treated with systemic therapies, such as biologics, for which we have many, Dr. Friedman says. But there are a good number of treatments approved for both plaque psoriasis and psoriatic arthritis. Biologic drugs, for example, work for both PsA and PsO by blocking certain cells or proteins in our immune systemsuch as the T-cell or the tumor necrosis factor-alpha proteinthat largely contribute to the development of psoriasis and psoriatic arthritis.
Dr. Finney adds that because joint changes associated with PsA can be permanent, prompt systemic treatment is highly warranted if someone does notice joint symptoms. Below, find a few systemic treatments for PsA and how they work.
Can Psoriatic Arthritis Affect Children Too
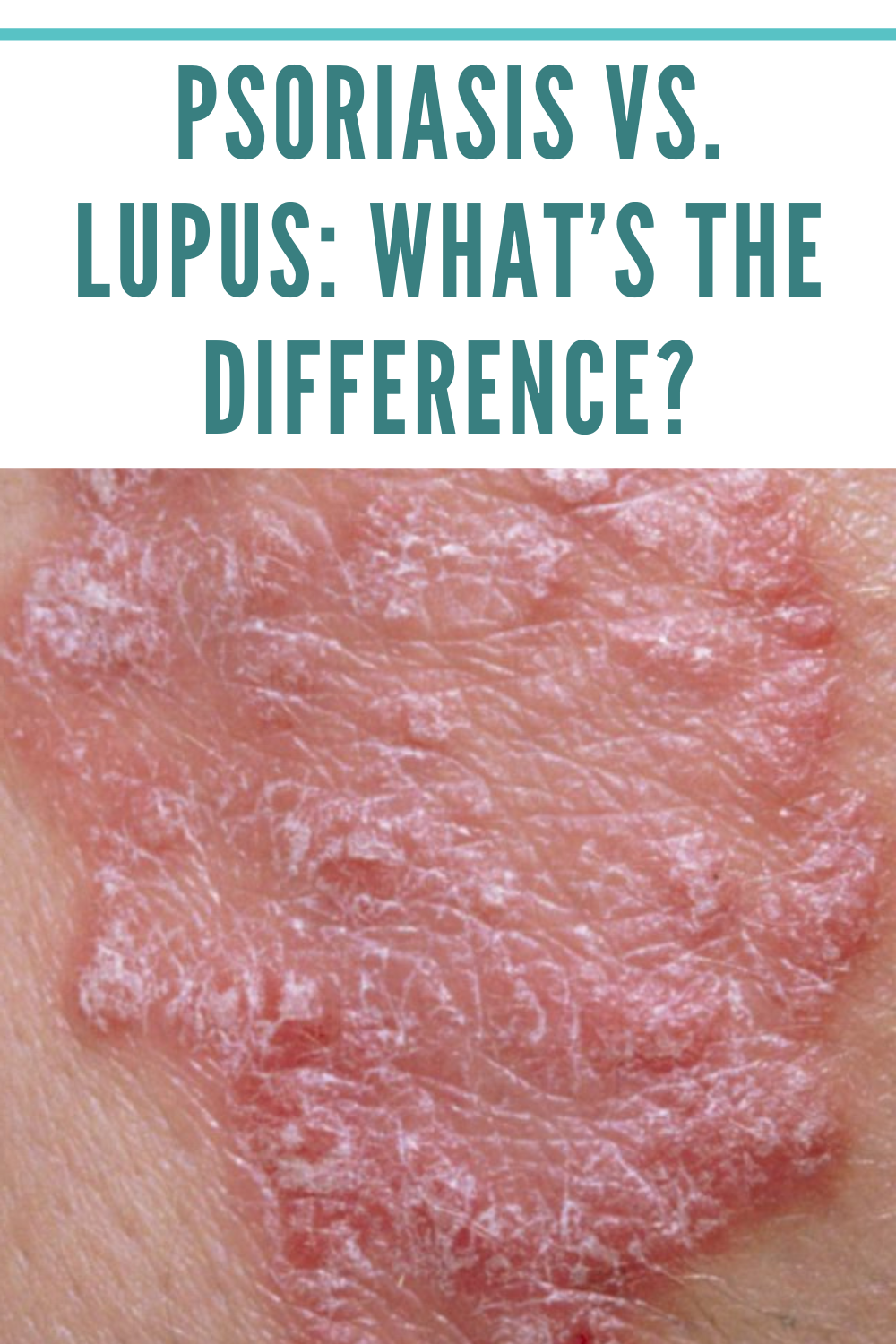
As many as 12,000 children in the UK are affected by arthritis. It is known as juvenile chronic arthritis , of which there are three main types, stills disease, polyarticular juvenile chronic arthritis and polyarticular onset juvenile chronic arthritis. Psoriatic arthritis is a minor subset of JCA and is uncommon.
Don’t Miss: How To Treat Psoriasis In Kids
Do Psa And Pso Have Overlapping Symptoms
As we briefly mentioned above, psoriatic arthritis causes joint pain, swelling, and stiffness , while psoriasis largely affects the skin by way of painful, scaly red or silver patches called plaques. Psoriatic arthritis often begins with stiffness at rest, meaning joints when you first wake up, says Adam Friedman, M.D., a board-certified dermatologist based in Washington, D.C. Lower back pain and heel pain can also be early signs.
As for psoriasis, the plaques can appear just about anywhere on the body, including the face, scalp, and genitalia, all of which can be especially debilitating. Other initial symptoms of psoriasis include small scaly spots of skin, itching, and red patches however, you should always go see your doctor instead of trying to diagnose yourself, as the aforementioned symptoms could be another skin condition, as well. Its also worth noting that psoriasis ranges in severity, with some people only having minor flare-ups every now and then, and others having acute cases that cover up to 50% or more of their body.
Speaking of severity, PsA symptoms can also range from mild to severe, with some folks only experiencing mild tension in their fingertips and/or spine, and others struggling with immense joint pain, swelling, and discomfort. Other symptoms that are often associated with psoriatic arthritis include inflammation in areas where tendons and ligaments attach to the bone, and eye inflammation.
Treatment For Gout Vs Psoriatic Arthritis
If you have both PsA and gout, you will need to treat both conditions. There are separate medications to treat PsA and gout. In general, PsA is treated with medication that suppresses your immune system while gout requires treatment with medications that lower uric acid in the blood and controls gout flares, says Dr. Singh.
For gout patients: The goal of gout treatment is to first reduce the inflammation causing flare-ups by using such medications as nonsteroidal anti-inflammatory drugs , corticosteroids , and oral colchicine. Once an acute gout flare is under control, your doctor may prescribe medication to control your uric acid levels, including xanthine oxidase inhibitors , uricosuric agents, and enzymes that break down uric acid.
If there is suspicion that a patient has both gout and PsA, sometimes treating the more acute symptoms of gout first allows for more clear assessment of other arthritis involvement, and the need for additional treatment for psoriatic arthritis, says Dr. Kohler.
For psoriatic arthritis patients: There are many drugs available to treat PsA. The ones your health care provider recommends will depend on your most troublesome PsA symptoms. Treatments and medications for psoriatic arthritis include:
Because both gout and PsA have risk factors related to your lifestyle and diet, patients with PsA and gout can benefit from adopting healthy habits, including:
Read Also: Does Stress Cause Psoriasis Flare Ups
What Causes Psoriasis Outbreaks
Psoriasis outbreaks differ from person to person. No one knows exactly what causes flare-ups. Common psoriasis triggers may include:
- Skin injury .
- Streptococcal or other infection that affects the immune system.
- Certain prescription medications .
- Cold weather, when people have less exposure to sunlight and humidity and more to hot, dry indoor air.
Recommended Reading: What Helps With Arthritis In Back
Overlap Of Some Symptoms
Although muscle weakness is main symptom of autoimmune myositis, approximately 30% of people with myositis experience joint aches and inflammation.6 In contrast to PsA, joint pain and swelling in myositis is typically mild. PsA and dermatomyositis both can affect the nails, although the effects are different. Nail psoriasis may appear as pitting, crumbling, red dots, or oil drops. Dermatomyositis causes changes to the nail beds and thickened cuticles.1
You May Like: Is Psoriasis A Symptom Of Something Else
Surgery And The Psoriatic Foot
Orthopaedic surgery to correct deformed joints is only justified in the presence of long-standing deformity where pain is preventing adequate mobility and all alternative medical treatments have failed. The advancement of newer techniques in recent years has seen better results in small joint replacement, but such procedures still need careful consideration and discussion with advice from an appropriate surgeon.
You May Like: Get Rid Of Psoriasis For Good
Treatment Options For Ankylosing Spondylitis Vs Psoriatic Arthritis
There is no cure for either AS or PsA. However, in the case of either condition, medication is critical to treat symptoms, protect joints, slow disease progression, and improve quality of life. Your rheumatologist will best determine the best treatment plan for your specific symptoms and health needs, says Dr. Norton.
Some of the treatments for AS and PsA overlap, though certain medications are better for certain symptoms.
For AS patients: Non-steroidal anti-inflammatory drugs like ibuprofen and naproxen are considered a first-line treatment for ankylosing spondylitis. If these medications dont adequately relieve symptoms, doctors frequently turn to biologics, which are targeted therapies that act on the immune system to stop inflammation. They are either infused with an IV or injected with a syringe or auto-injector pen.
Different biologics act on different parts of the immune system. In AS, commonly used biologics include those that block the protein tumor necrosis factor as well as those that block a protein called interleukin-17 .
FDA-approved anti-TNF biologics for AS include adalimumab , certolizumab pegol , etanercept , golimumab , and infliximab . FDA-approved IL-17 inhibitors for AS include secukinumab and ixekizumab .
PsA patients may also benefit from phototherapy or topical creams to treat skin plaques.
Read Also: Psoriasis In Children’s Hair
Which Came First: Psa Or Pso
Can you have psoriatic arthritis without having psoriasis? Lets get this one out of the way first, shall we? The short answer is yes, yes you can have psoriatic arthritis and not psoriasishowever, if you have PsA, you will likely have a history of psoriasis and/or psoriatic arthritis somewhere in your family line. It is very rare for a patient to develop PsA prior to having psoriasis noticeable on the skin, but it has been reported, says Robert Finney, M.D., a board-certified dermatologist in New York City. Psoriatic arthritis occurs in less than 30 percent of patients with psoriasis and is more common in patients with extensive skin disease, who are diagnosed at a younger age. Additionally, Dr. Finney says psoriatic arthritis more frequently occurs in those who experience nail changes related to psoriasis, such as pitting, lifting, or orange splotches.
Serological Features Of Ra And Psa
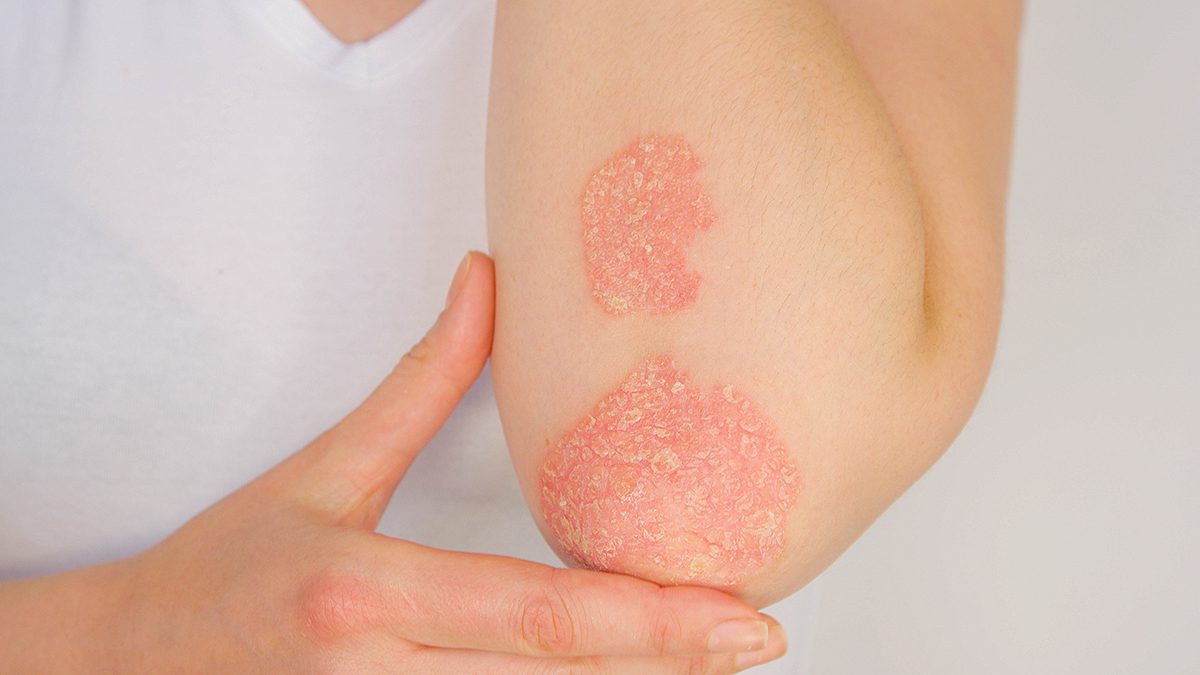
RA is a seropositive arthropathy, with approximately 80% of patients having a positive test result for RF or CCP antibodies. CCP antibodies are a more specific marker for RA than RF, but both biomarkers are considered to be distinct and complementary predictors of disability and joint erosion.
In contrast, PsA is a seronegative inflammatory arthropathy. RF and CCP are absent in most patients with PsA, and if patients do have positive test findings for RF or CCP, the titres are usually low. In a study comparing patients with RA or PsA and controls, the mean RF and anti-CCP titre values were substantially higher in patients with RA compared with PsA . Titres in patients with PsA were similar to values in controls. Although the presence of serum RF or CCP antibodies is generally not used to exclude diagnosis of non-rheumatic diseases , data suggest that at anti-CCP titre values 11.6 U/mL, it is highly probable that patients have RA rather than PsA. In both patients with RA and PsA, the presence of anti-CCP antibodies is associated with bone destruction, suggesting that the osteocatabolic effect of anti-CCP antibodies is not found only in RA as previously thought.
Increased ESR and CRP levels are markers of inflammation, but not necessarily just in RA. Other rheumatological diseases associated with elevated ESR and CRP levels include polymyalgia rheumatica, Sjögrens syndrome and ankylosing spondylitis.
Recommended Reading: Betamethasone Dipropionate Cream For Psoriasis
Tips For Identifying Oa
OA isnt a disease that cycles, like PsA. Instead, it can gradually get worse.
OA pain may be mild at first. You might notice a slight twinge in your knee when you bend it, or your joints might ache after a workout.
The pain, swelling, and stiffness will get worse as the joint damage increases. Along with the pain, your joints will feel stiff especially when you first wake up in the morning.
OA will most likely affect the joints of your body that move the most.
This includes the joints in your:
- hands
Both Interfere With Activities Of Daily Living
Both conditions can result in a loss of normal function in affected areas, making it difficult to perform everyday tasks. Although the impact on daily living are similar, the causes are different. In PsA, painful, swollen, and stiff joints can limit movement and mobility. In myositis, limitations result from weakness of the large muscles close to the center of the body .
You May Like: How To Heal Psoriasis Scars
What Is Erythrodermic Psoriasis
Erythrodermic psoriasis is a rare form of psoriasis associated with extreme inflammation, itching and pain that affects most of the body. Other symptoms include large sheets of shedding skin , an increase in heart rate, swelling due to fluid retention and significant changes in your body temperature. Its important to seek immediate medical attention if youâre experiencing a flare-up of erythrodermic psoriasis as it can lead to pneumonia or heart failure if left untreated.6
Managing Symptoms Of Autoimmune Arthritis
Several medications work for both psoriatic arthritis and rheumatoid arthritis:
- Nonsteroidal anti-inflammatory medications reduce pain and swelling.
- Disease-modifying antirheumatic drugs protect joints and slow the disease, and less of the joint is destroyed, meaning theres less swelling, pain and less loss of joint function.
- Biologics target the specific parts of the immune system that drive inflammation.
As researchers learn more about the causes of inflammatory arthritis, theyre developing new medications to manage these diseases. Some of these new drugs are designed to specifically target one disease or the other.
Both psoriatic arthritis and rheumatoid arthritis are chronic diseases. They cant be cured, but they can be managed, Dr. Rosian says. By working with your doctor to get the correct diagnosis, you can manage symptoms to feel your best.
Don’t Miss: Does Shaving Your Head Help Scalp Psoriasis
How Do Ra And Psa Affect You
When you have RA, your immune system attacks the lining of the tissues around your joints. They swell up and become painful. Over time, they can become damaged and deformed.
With PsA, your immune system attacks and damages not just your joints, but your skin, as well. It causes your body to make too many skin cells, which leads to psoriasis, a skin condition that often affects people with PsA.
The Different Forms Of Myositis
Both forms of myositis cause muscle weakness. The weakness begins in the shoulders and hips. It usually worsens over weeks or months, although it may happen more quickly in rare cases.1 Due to weakness, patients have a difficult time with everyday tasks such as getting out of a chair, climbing stairs, and lifting objects.1 In advanced disease, patients may have trouble swallowing and breathing.
People with dermatomyositis have skin changes in addition to muscle weakness. Skin changes usually occur first.1 A blue-purple rash may appear on the eyelids. A red rash may spread on the face, neck, and chest or on the back and shoulders. It may get worse after time in the sun and can be itchy. Gottrons rash is a typical sign of dermatomyositis. Gottrons rash looks like red to purple flat papules on the knuckles.
Autoimmune myositis is uncommon and can be difficult to diagnose properly.1,2 Multiple other conditions are considered in the differential diagnosis.
Don’t Miss: Are Eggs Good For Psoriasis
How Do Psoriasis And Psa Overlap
For every 10 patients who walk in the door with psoriasis, about three or four of them will eventually get PsA, says Elaine Husni, MD, MPH, vice chair of the department of rheumatic & immunologic diseases at the Cleveland Clinic in Ohio. Most cases almost always start with the skin condition and then within seven to 10 years later, joint pain symptoms start to develop.
However, skin and joint symptoms can develop at the same time and, more rarely, joint symptoms can appear before skin involvement, says Dr. Haberman. While estimates vary, one study showed that up to 3 percent of patients developed joint disease before skin disease, she notes.
In some cases, there may have been skin involvement that went unnoticed or undiagnosed. For example, psoriasis can be sneaky and show up in hidden or private areas like the scalp, intergluteal cleft , belly button, and inside the ear, explains Dr. Husni. Since people dont really examine their scalp or buttocks very often, small psoriasis patches can get missed and delay diagnosis, she says.
Adds Dr. Haberman: You might have a small fleck in your scalp that you just think of as dandruff that is actually psoriasis.
Whats more, people with psoriasis in some of these hidden areas may actually be more prone to PsA. Studies have shown that you may be at higher risk of developing PsA if you have scalp, nail, or inverse psoriasis, says Dr. Haberman.
Recommended Reading: Can Rheumatoid Arthritis Affect Your Lungs