How Is Psoriatic Arthritis Diagnosed In A Child
Psoriatic arthritis is easier to confirm if your child already has psoriasis. If the skin symptoms have not yet occurred, diagnosis is more difficult. Your childs healthcare provider will take your childs medical history and do a physical exam. The provider will ask about your child’s symptoms. Your child may have blood tests such as:
-
Erythrocyte sedimentation rate . This test looks at how quickly red blood cells fall to the bottom of a test tube. When swelling and inflammation are present, the blood’s proteins clump together and become heavier than normal. They fall and settle faster at the bottom of the test tube. The faster the blood cells fall, the more severe the inflammation.
-
Uric acid. High blood uric acid levels are linked to psoriatic arthritis.
-
Complete blood count . This test checks for low counts of red blood cells , white blood cells, and platelets.
-
Antibody blood tests. These tests are done to look for certain kinds of proteins, called antibodies, in your blood. These tests can be positive for many kinds of rheumatic diseases. Younger children are more likely to have a positive antinuclear antibody test.
Other tests may include:
-
X-rays. This test uses a small amount of radiation to create images of organs, bones, and other tissues.
-
Eye exam. This is done by a pediatric eye doctor . The exam looks for uveitis, a swelling of the middle layer of the eye.
Treatment For Psoriatic Arthritis And Rheumatoid Arthritis Is Similar But Figuring Out Which Disease You Have Can Be Tricky
No single test can diagnose rheumatoid arthritis or psoriatic arthritis, reports the Mayo Clinic. Rather, your doctor will check your medical history and closely examine your symptoms to see if you have signs of either disease. Symptoms like ongoing morning stiffness, swelling of three or more joints on the same sides of the body for at least six weeks, and rheumatoid nodules may make your doctor suspect rheumatoid arthritis, the Cleveland Clinic says. To diagnose psoriatic arthritis, your doctor will likely examine your joints to search for swelling and stiffness, your fingernails for any issues like pitting, and your feet for soreness, according to the Mayo Clinic.
is very much an art, and the skills and experience of a rheumatologist are necessary, John M. Davis III, M.D., M.S., a clinical rheumatologist, vice chair and practice chair of the division of rheumatology, and associate professor of medicine at the Mayo Clinic College of Medicine and Science, tells SELF. There is a great need for more sensitive and specific diagnostic tests.
Your doctor may also order imaging tests, like X-rays and MRIs, to help determine if you have psoriatic arthritis. Keep in mind, though, that certain symptoms and test results dont show up in everyone with these diseases, and they may also overlap with other conditions, making it a challenge to get a firm diagnosis.
Dealing With These Conditions Can Be Difficult Enough Without The Added Stress Of Losing Your Hair Luckily Any Loss Is Usually Temporary Heres How To Safeguard Your Strands
If youre one of the roughly 2 percent of Americans who have psoriasis, a chronic condition that typically causes raised, red patches of skin topped with silvery scales, theres a good chance that it has impacted your scalp. This also holds true for the more than 40 percent of people with psoriasis who also have psoriatic arthritis , a form of arthritis that can appear in combination with psoriasis.
Psoriasis causes skin cells to divide about 10 times faster than normal. The excess cells pile up on the surface of the skin, causing scaly patches of itchy, dry skin. Known as plaques, these lesions often itch, burn, and sting.
Recommended Reading: Does Psoriasis Get Worse With Heat
Joint Symptoms In People With Psa And Ra
Both psoriatic arthritis and rheumatoid arthritis cause similar joint symptoms. Joints affected by PsA or RA can feel painful, stiff, swollen, and hot. The symptoms of PsA and RA tend to show up in different joints.
The two diseases, for instance, affect different parts of the spine. PsA sometimes leads to a condition called spondylitis that causes lower back pain. Spondylitis involves inflammation in the joints of the spine and between the spine and pelvis. Up to half of people with PsA will experience spondylitis pain. RA, on the other hand, often causes problems in the cervical spine, in the neck. Up to 80 percent of people with RA experience neck pain.
RA is also more likely than PsA to affect the hands, such as the joints in the wrists and fingers, whereas PsA is more likely to affect the feet. Additionally, PsA and RA affect different small joints within the fingers and toes. RA affects the first two joints, and PsA attacks the joint closest to the nail bed.
People with PsA can experience dactylitis, a condition in which the fingers or toes swell up and resemble sausages. Dactylitis is often the first symptom of PsA, and it may be the only joint symptom a person experiences for several years. PsA also affects the nails. People with PsA often have pitted, ridged nails, which appear similar to nails with a fungal infection.
Will Drug Treatments For Psoriatic Arthritis Make My Psoriasis Worse
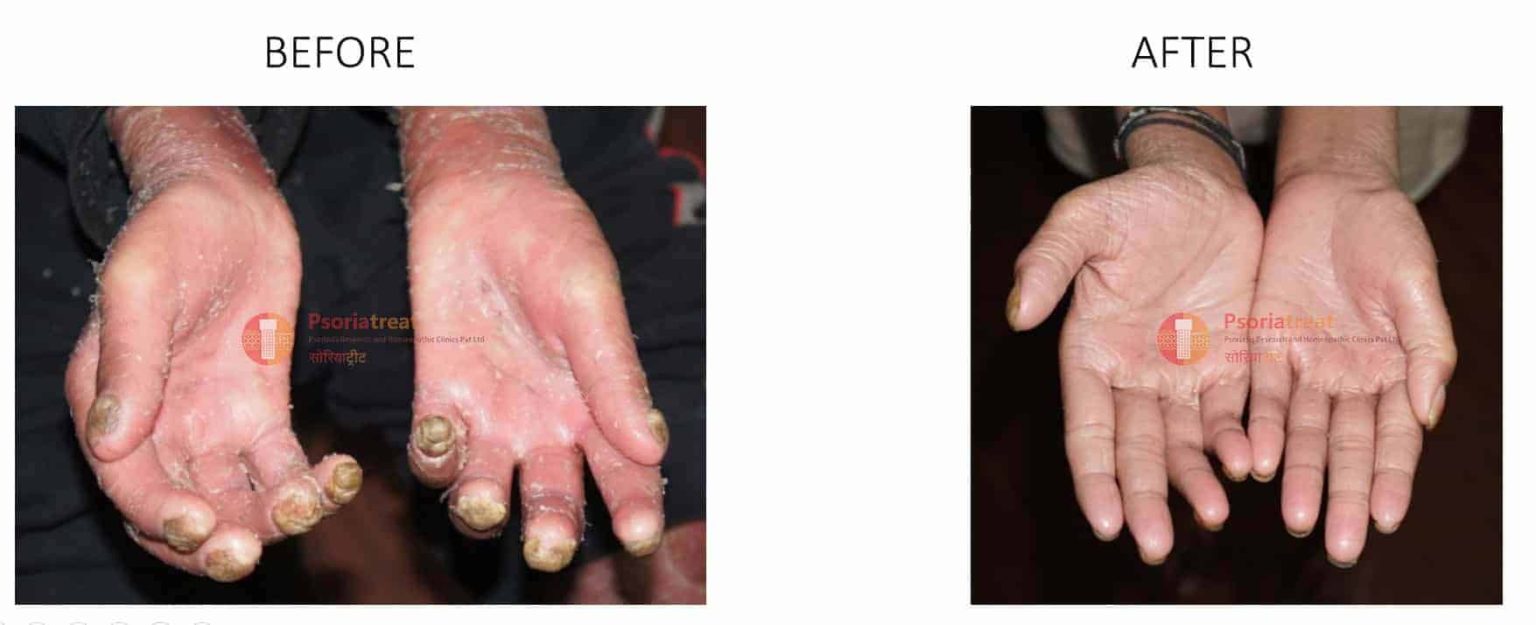
Some drug treatments may make psoriasis worse, but then again, some can also make it better too. Before you start any treatments offered, discuss this both with your dermatologist and rheumatologist. DONT FORGET to politely request that both consultants let each other know of your treatment regimes, this helps both of them evaluate your treatment and any side effects that you may be likely to experience. Some people find that when their psoriasis is bad their arthritis is also bad and as one improves, so does the other. This most often occurs when the skin and joint disease start simultaneously. Some of the arthritis treatments also help the skin and this is can help the doctors decide which is the best drug to use.
Recommended Reading: Best Shampoo Bar For Psoriasis
How Is Psoriatic Arthritis Mutilans Diagnosed
ishonestNo.364 Acne Scars
In some cases, people diagnosed with psoriatic arthritis didnt know they had psoriasis. In 85 percent of psoriatic arthritis cases, symptoms of psoriasis are obvious before arthritis is apparent.
To diagnose psoriatic arthritis mutilans, your doctor will first confirm you have arthritis. After checking your joints for signs of swelling or tenderness, youll receive diagnostic testing.
Your doctor may order lab tests to check for inflammation or the presence of certain antibodies. Both can point to arthritis. You doctor will also likely recommend an X-ray or other imaging test to assess joint damage.
Once your doctor has diagnosed you with arthritis, theyll test a blood sample to find out what kind of arthritis you have. For example, if the rheumatoid factor and cyclic citrullinated peptide antibodies are in your blood, you may have rheumatoid arthritis .
At this time, there isnt a lab biomarker for psoriatic arthritis or the psoriatic arthritis mutilans subset. Psoriatic arthritis mutilans is diagnosed by checking the severity of the bone destruction. There are very few conditions associated with such severe bone loss.
Treatment Options For Both Psoriasis And Psa
Drugs to suppress immune system activity are among the most effective treatments for psoriasis and PsA.
Systemic, immune-suppressing drugs often provide relief for both conditions. However, your risk of secondary infections and other side effects is greater when using these drugs.
If you have severe psoriasis and are diagnosed with PsA, your doctor may prescribe the anti-inflammatory and immune-suppressant drug methotrexate . This medication aims to slow down the cells in your body that are reproducing too quickly and causing psoriasis flares.
Common side effects of methotrexate include:
- headaches
- dizziness
- upset stomach
A newer class of drugs called biologics, in particular TNF blockers, targets specific parts of the immune system more precisely. Because of this, your doctor may be more likely to recommend them over methotrexate.
Biologics reduce inflammation and psoriasis outbreaks in most people who take them. There are a number of brands of biologics approved for treatment of psoriasis in the United States.
Biologics need to be injected. Some need to be administered more often than others. Common side effects include:
- allergic reaction
Don’t Miss: Psoriasis On Face And Scalp Treatment
Work And Psoriatic Arthritis
Having psoriatic arthritis may make some aspects of working life more challenging. But, if youre on the right treatment, its certainly possible to continue working.
Help and support is available, and you have rights and options.
The Government scheme Access to Work is a grant that can pay for equipment to help you with activities such as answering the phone, going to meetings, and getting to and from work.
The 2010 Equality Act, and the Disability Discrimination Act in Northern Ireland makes it unlawful for employers to treat anyone with a disability less favourably than anyone else. Psoriatic arthritis can be classed as a disability if its making every-day tasks difficult.
Your employer may need to make adjustments to your working environment, so you can do your job comfortably and safely.
You might be able to change some aspects of your job or working arrangements, or train for a different role.
In order to get the support youre entitled to, youll need to tell your employer about your condition. Your manager or HR department might be a good place to start.
Other available support might include:
- your workplace occupational health department, if there is one
- an occupational therapist. You could be referred to one by your GP or you could see one privately
- disability employment advisors, or other staff, at your local JobCentre Plus
- a Citizens Advice bureau particularly if you feel youre not getting the support youre entitled to.
Fingers Toes And Skin
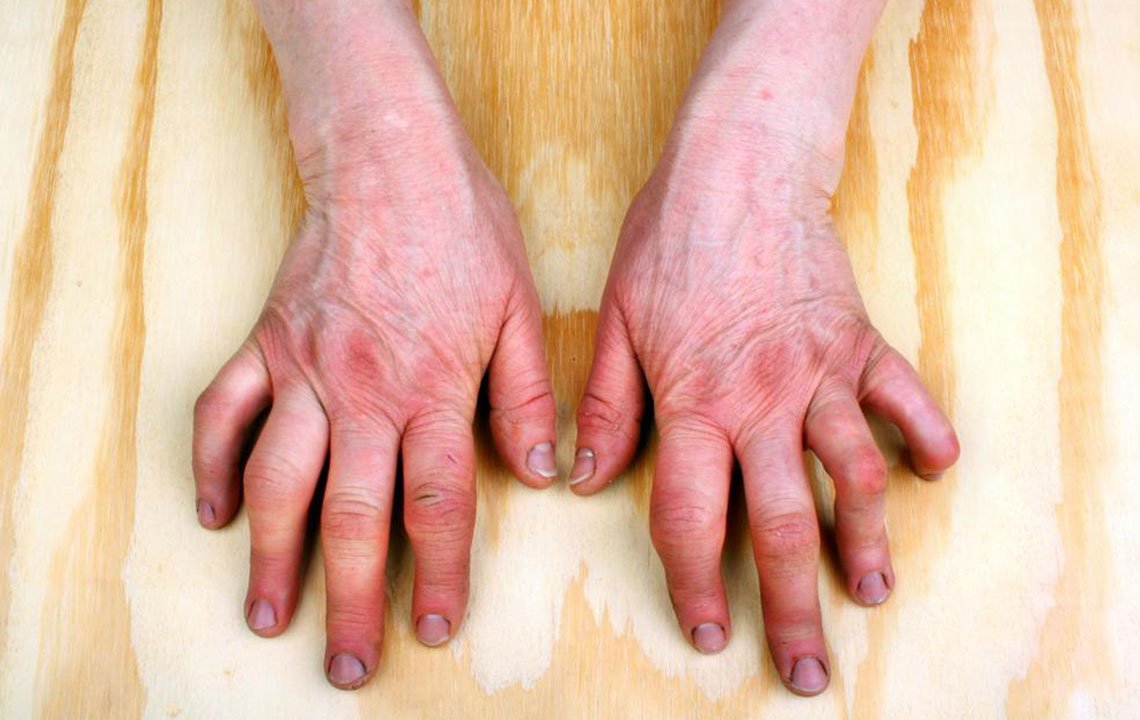
Another telling clue is the presentation of the disease on the fingers and toes. With PsA, the distal joints will be the focus of pain, swelling, and stiffness. By contrast, RA primarily involves the proximal joints .
With severe PsA, the fingers can also take on a sausage-like appearance , making it difficult to ball your fist. While this can occur with RA, it is not the hallmark that it is with PsA.
Around 85% of people of PsA with also have the most typical form of psoriasis, characterized by dry, flaky skin plaques. Moreover, half will have nail psoriasis at the time of their diagnosis. Neither of these occurs with RA.
Recommended Reading: What Can I Do For Arthritis In My Hands
Recommended Reading: Does Psoriasis Affect The Face
What Causes Rheumatoid Arthritis Rashes
People with RA are prone to episodes known as flares. A flare indicates that there is increased disease activity in a persons body. A person may have more symptoms associated with the condition, including fever, joint swelling, and fatigue. During a flare-up, a rheumatoid arthritis rash is more likely to occur.
When vasculitis causes a rash, this is most likely due to inflammation of small arteries and veins. This is due to high levels of rheumatoid factor in the blood.
RA can cause complications beyond a rash. Vasculitis can affect blood flow in arteries and veins. The results of severe episodes of vasculitis can be:
- numbness and tingling in the nerves, including loss of sensation in the hands and feet
- affected blood flow to the extremities that can cause gangrene in the fingers or toes
- systemic vasculitis that affects blood flow to the brain or heart that can result in heart attack or stroke
The occurrence of RV is rare, and the complications above are even rarer. However, its possible that a rash could be a precursor to something more severe. See your doctor if you experience any signs or symptoms of RV.
Treatment For Psoriatic Arthritis
Treatment for psoriatic arthritis aims to:
- relieve symptoms
- slow the condition’s progression
- improve quality of life
This usually involves trying a number of different medicines, some of which can also treat the psoriasis. If possible, you should take 1 medicine to treat both your psoriasis and psoriatic arthritis.
The main medicines used to treat psoriatic arthritis are:
- non-steroidal anti-inflammatory drugs
- biological therapies
Don’t Miss: Best Oral Medication For Psoriasis
Signs And Symptoms Of Psoriatic Arthritis
For most people, psoriatic arthritis develops years after psoriasis. Contact your dermatologist if you have psoriasis and any of these signs or symptoms:
- A very noticeable swollen finger or toe
- Swollen and tender joints
- Stiffness when you wake up or sit for hours that fades as you move
- Nails that are pitted
- Nail separating from nail bed
- Lower back pain
How Psoriasis And Psoriatic Arthritis Affect The Scalp
For many patients, the scalp is the only part of the body where psoriasis occurs or its the first location where the autoimmune disease develops.
Research shows that at least a quarter of people with plaque psoriasis, the most common type of psoriasis, initially present with lesions on the scalp.
Its very common for psoriasis to affect the scalp statistics show a range of 40 percent to 80 percent of people with psoriasis have scalp involvement, says Mount Kisco, New York, dermatologist David Bank, MD, who is also an assistant clinical professor of dermatology at Columbia Presbyterian Medical Center in New York City. It may occur in isolation or with psoriasis in other areas.
Scalp psoriasis can run the gamut from mild to severe .
Sometimes, in addition to the scalp, plaques also cover nearby areas such as the forehead, back of the neck, and the skin around the ears.
Recommended Reading: Plaque Psoriasis On African American Skin
Add Exercise To Your Daily Routine If You Can
Keeping your joints moving can ease stiffness. Being active for at least 30 minutes per day will also help you lose excess weight and give you more energy. Ask your doctor what type of exercise is safest for your joints.
Biking, walking, swimming, and other water exercises are gentler on the joints than high-impact exercises like running or playing tennis.
Psoriatic Arthritis Presentation Classification And Diagnosis
Prevalence of PsA is not known, but it is estimated to be from 0.3% to 1% of the U.S. population. In the psoriasis population, PsA is reported to range from 7% to 42%, although more recently, these numbers have been found to be in the 15% to 25% range . This type of inflammatory arthritis can develop at any age but usually is seen between the ages of 30 and 50 years, with men being affected equally or a little more than are women. Clinical symptoms usually include pain and stiffness of affected joints, > 30 minutes of morning stiffness, and fatigue.
The presentation of joint involvement can vary widely. Five subtypes of arthritis were identified by Moll and Wright in 1973, which included arthritis with predominant distal interphalangeal involvement, arthritis mutilans, symmetric polyarthritis , asymmetric oligoarthritis , and predominant spondylitis . Patients with PsA may also have evidence of spondylitis or sacroiliitis with back pain > 3 months, hip or buttock pain, nighttime pain, or pain that improves with activity but worsens with rest. The cervical spine is more frequently involved than is the lumbar spine in patients with PsA.
Radiograph of the Right Hand and Right Foot
Read Also: Best Bath Soak For Psoriasis
Also Check: Can Drinking Alcohol Cause Psoriasis
If You Think Youve Been Misdiagnosed
Get a second opinion from another rheumatologist or dermatologist. The bright side: Treatment for psoriatic arthritis and rheumatoid arthritis is often the same. For either disease, your doctor may prescribe a non-steroidal anti-inflammatory drug such as Motrin, an immunosuppressant like methotrexate, or any number of biologics on the market.
Psoriatic Arthritis Treatment Options
Psoriatic arthritis symptoms can be treated with systemic drugs that affect your whole body. Depending on your unique case of psoriatic arthritis, your dermatologist may prescribe methotrexate, cyclosporine or certain biologics. In some cases, steroid injections can reduce inflammation quickly in an affected joint. At Dermatology Associates of Plymouth Meeting, we may team with a board-certified rheumatologist to treat joint disease linked to psoriatic arthritis.
In addition to these medications or treatment options, whether you are experiencing psoriasis or psoriatic arthritis, your dermatologist may recommend lifestyle changes to help minimize symptoms and flare ups. We always encourage changes such as quitting smoking, drinking less and minimizing stressors which can help with psoriasis and psoriatic arthritis flare ups. With psoriasis and psoriatic arthritis, it is common for symptoms to come and go, but it is important to continue taking medication and undergoing treatments recommended by your dermatologist.
If you are struggling to manage your plaque psoriasis or psoriatic arthritis, schedule an appointment today. Our team of board-certified dermatologists are experts in treating all types of psoriasis and can develop a personalized treatment plan based on your unique background and needs.
Recent Posts
Don’t Miss: Best Treatment For Psoriasis On Head
Can Psoriatic Arthritis Affect Other Parts Of The Body
Having psoriatic arthritis can put you at risk of developing other conditions and complications around the body.
The chances of getting one of these are rare. But its worth knowing about them and talking to your doctor if you have any concerns.
Eyes
Seek urgent medical attention if one or both of your eyes are red and painful, particularly if you have a change in your vision. You could go to your GP, an eye hospital, or your local A& E department.
These symptoms could be caused by a condition called uveitis, which is also known as iritis. It involves inflammation at the front of the eye.
This can permanently damage your eyesight if left untreated.
Other symptoms are:
- blurred or cloudy vision
- sensitivity to light
- not being able to see things at the side of your field of vision known as a loss of peripheral vision
- small shapes moving across your field of vision.
These symptoms can come on suddenly, or gradually over a few days. It can affect one or both eyes. It can be treated effectively with steroids.
Heart
Psoriatic arthritis can put you at a slightly higher risk of having a heart condition. You can reduce your risk by:
- not smoking
- staying at a healthy weight
- exercising regularly
- eating a healthy diet, thats low in fat, sugar and salt
- not drinking too much alcohol.
These positive lifestyle choices can help to improve your arthritis and skin symptoms.
Talk to your doctor if you have any concerns about your heart health.
Crohns disease
Non-alcoholic fatty liver disease