What Does Nail Psoriasis Look Like
Nail psoriasis can affect your fingernails and toenails and will often manifest in these ways:
- Discoloration. Your nails are starting to brown, yellow or turn completely white.
- Damaged nail surface. You will notice lines, cracks, pits, holes or ridges. Basically, any nail surface that isnt smooth.
- Lifted nails. With nail psoriasis, white debris can begin to form under your nail, pushing it up and away from your skin. This is usually painful.
- Thinning or thickening texture. If your nails feels brittle or too thick, this can be the buildup of psoriatic skin cells under the nails, or it can be a fungal infection that can more easily invade the already-lifted nail. You will need a culture to determine the best treatment.
- Nail separation. Again, pretty painful. Depending on the severity of your nail psoriasis, your nail may start to separate itself from the nail bed.
Read Also: First Line Treatment For Psoriasis
Biologics For Scalp Psoriasis Reviews :
Jennifer Wasser : Biologics truly gave me my life back. I just decided either not take any meds and be miserable and depressed all of the time, or do it so that the quality of life would improve for me. I take Cosentyx along with Acitretin. The 2 of them are my miracle drugs. Yes the side effects can be much at times, but I am now able to work again, and do many more things with my daughter that I wasnt able to before. I suffer from Pustular Psoriasis. My hands and feet were horrible. Here is a before and after.
Kim Keeley : I know so many have commented but I feel like I should too. I had it BAD on my scalp, just like that. I lost a bunch of hair and had bald spots on my head. It would just bleed, it was so gross. This was during taking methotrexate and humira. I then stopped those and started otezla. It worked amazing! I did it for 10 months and the depression side effects got to me, had to stop.
Now on Cosentyx. Its only been 3 weeks so I cant say much but I havent had a huge flair up inbetween switching which I was deathly afraid of. Its worth a try. Just know what side effects there are and be cognitive of them. I didnt realize the depression got to me on otezla until many people commented on how I wasnt myself. Love to you!
What Are The Side Effects Of Taking A Biologic
Each PsA biologic is different. Each has its own potential side effects.
However, there are also similarities in this class of drugs. The most common side effect for all biologics is an increased risk of unusual, or opportunistic, infections.
In addition, TNF-alpha inhibitors may cause new or worsening heart failure.
If you and your doctor decide to try this course of treatment with a biologic, you may experience flu-like symptoms or respiratory infections.
Since biologics are given by injection or via an intravenous solution, you may also experience discomfort where the needle pokes your skin.
Biologics may lead to more serious side effects, such as blood disorders or cancer.
For these reasons, its a good idea to maintain a strong relationship with your doctor that focuses on open communication.
Together, you can talk about and decide on whether a biologic is the right treatment for your psoriatic arthritis.
Biologics are recommended for those living with moderate to severe PsA. But some people arent candidates for biologics.
Thats because the drugs side effects may do more harm than good.
People with compromised immune systems or active infections shouldnt take biologics for their PsA. These drugs suppress the immune system and can be unsafe if yours is already compromised in some way.
The cost and out-of-pocket expenses for biologics can also be a barrier for some people.
Read Also: How Does Guttate Psoriasis Start
Acrodermatitis Continua Of Hallopeau
This type of pustular psoriasis is rare. It causes pus-filled bumps on the fingertips, toes, or both. The disease can also develop underneath the nails.
Often beginning on one finger or toe, new pus-filled bumps may continue to appear. When this happens, new pustules can develop on more than the fingers and toes. In rare cases, the pus-filled bumps can slowly spread up the arms or legs.
Anyone who has pus-filled bumps over much of the skin needs immediate medical care. When widespread, pustular psoriasis can be life-threatening.
The first choice for treating this type of pustular psoriasis often includes the following.
-
Synthetic vitamin D combined with a strong corticosteroid: This combination is applied to the skin.
-
PUVA: This is a type of light treatment that involves taking a medication called psoralen before getting UVA light treatments on the affected skin.
While the above describes what treatment may be used for each type of pustular psoriasis, your treatment plan may include different medications. Your age, other medical conditions , and general health also play key role in determining which treatment is best for you.
ImageGetty Images
ReferencesFitzpatrick JE. Pustular eruptions. In: Fitzpatrick JE and Aeling JL. Dermatology Secrets. Hanley & Belfus, Inc., Philadelphia, 1996:66-7.
Jeon C, Nakamura M, et al. Generalized pustular psoriasis treated with apremilast in a patient with multiple medical comorbidities. JAAD Case Rep. 2017 3: 495-7.
Study Selection And Data Extraction
Three reviewers independently conducted publication selection . Any discrepancies were resolved by an additional reviewer . Studies were categorized based on the morphology of palmoplantar lesions. Study characteristics and subject characteristics were extracted using a standardized data abstraction form designed for this review. Efficacy outcomes were recorded in Table Table1,1, defined as a 50% reduction in the PPP Area and Severity Index if available, otherwise a 75% reduction in PPASI or an Investigator Global Assessment score of 0/1 was used. If two biologics were studied in one study, both were described in Tables 1, ,2,2, ,33 and and44 under the category of the primary biologic that was studied, but the efficacy data of both biologics were used to calculate the summary of clinical improvement outcomes in Table 5. Due to the heterogeneity of outcome measures, outcomes were reported as described by the authors of each publication.
Hyperkeratotic palmoplantar psoriasis, efficacy and safety of biologic agents
Pustular palmoplantar psoriasis, efficacy and safety of biologic agents
BIW Twice weekly, d/c discontinued DM diabetes mellitus, TB tuberculosis, PPD purified protein derivative, HCV hepatitis C
Don’t Miss: How Does Otezla Work For Psoriasis
Who Can Take Biosimilars
All biologics, including biosmilars, are typically prescribed for people with more advanced disease, including individuals with moderate-to-severe psoriasis and active PsA. But each of the three approved biosimilars are indicated for different groups within this population.
You should not take biosimilars if:
- Your immune system is significantly compromised
- You have an active infection
Screening for tuberculosis or other infectious diseases is required before starting treatment with all biologics, including biosimilars.
Read Also: What Is Psoriasis Of The Skin
Enhancing Healthcare Team Outcomes
Palmoplantar psoriasis is best managed by an interprofessional team that also includes the nurse and pharmacist. There is no cure for this disorder and at some point, drug treatment is required. The constant itching and pain and results in a poor quality of life, hence, healthcare workers should take steps to reduce triggers and educate patients on medication compliance. In addition, patients should be encouraged to discontinue smoking. The pharmacist should emphasize the importance of medication compliance. A wound care nurse should educate the patient on the importance of skincare.
The outcomes for most patients with palmoplantar psoriasis are guarded relapses are common and eventually most patients require the potent biological agents, which have their own adverse reactions.
Read Also: Hair Loss Due To Psoriasis
Skyrizi Is A Biologic That Was Approved For The Treatment Of Moderate
What is Skyrizi?
Skyrizi was approved by the FDA in April 2019 for the treatment of moderate-to-severe plaque psoriasis in adults. Skyrizi was approved by the FDA in January 2022 for the treatment of active psoriatic arthritis in adults.
For both plaque psoriasis and PsA, Skyrizi is given by injection under the skin at week 0 and week 4, and then every 12 weeks afterwards.
To learn more, please visit the Skyrizi website.
Best Buologic For Pustular Psoriasis
CLIENT: .Ehm..noits very sudden.
HYPNOTIST: Its very sudden?
CLIENT: Hm
HYPNOTIST: Alright. Now youre in the bath there, youve just become aware of this rash coming up. And youve discovered that Grandads got cancer. But youre only 7, so Im not quite sure whether that really is enough to worry you or not. But something is troubling you. Something perhaps just a day or two before this rash first appeared thats in your mind. And its a big worry, its a worry that youve carried for many years, even to adulthood.
So Im going to pick up your hand and drop it into your lap, and whatever that worry is will come very clearly in your mind, but youll still be in that bath in your mind. Stay relaxed, watch that happen. 1,2,3. Now what is it thats troubling you Helen?
CLIENT: They didnt tell me, I heard them.
HYPNOTIST: You heard them? Now who did you hear? Who did you hear? Thatsalright, you can let those feelings come out. Who did you hear then?
CLIENT: Mum and dad.
HYPNOTIST: And what did you hear them say?
CLIENT: That he was dying of cancer.
HYPNOTIST: Is that Grandad?
HYPNOTIST: So you knew that he was dying?
CLIENT: I dont think I was meant to know.
HYPNOTIST: No, but you overheard them?
CLIENT: Hm
HYPNOTIST: Alright. Obviously I can see that it worried you a lot because you knew what that meant didnt you?
CLIENT: Hm
CLIENT:.Yes.
HYPNOTIST: Did this rash just come along perhaps a day or two after you overheard mum and dad talking?
CLIENT: Mm
CLIENT: No.
Recommended Reading: What Is Psoriasis Skin Condition
Can Biosimilars Be Used With Other Treatments
It is important to tell your health care provider about all treatments, medicines, vitamins or supplements that you are taking.
Like all biologics, biosimilars can be used with other treatment options including topicals and phototherapy. The biologics Enbrel, Humira and Remicade are shown to be safe and effective when taken with methotrexate. This means that their biosimilars, including Erelzi, Amjevita, and Inflectra, may be safe and effective when taken with methotrexate.
- With Inflectra being the biosimilar to Remicade, its use in combination with phototherapy may increase the risk for skin cancer.
- No drugs that interact with biologics should be combined with their respective biosimilars.
What Treatments Are Available For Nail Psoriasis
There are many treatments for nail psoriasis. Your treatment plan may include one or more of the following.Treatment you apply to the nails: This can be helpful for mild or early nail psoriasis. Nails grow slowly, so youll need to apply these treatments for several months, often once or twice a day. Because nail psoriasis can be stubborn, you may need to use more than one treatment. Sometimes, two medicines are combined to give you a faster response.
Treatment that you apply to your nails includes the follow.
-
A potent or very potent corticosteroid: This can be helpful for most signs and symptoms of nail psoriasis. Its safe to use this medicine once or twice a day for up to nine months.
-
Calcipotriol: In one study, researchers found this to be as effective as a potent corticosteroid at treating the buildup beneath the nail.
-
Tazarotene: This treatment can be especially helpful for treating pitting, a separating nail, and discoloration.
If you need stronger treatment, your dermatologist may recommend treatment given in a dermatologist office or clinic. This treatment may include one of the following.
Psoriasis medicine that can help clear the skin and nails includes:
-
A biologic
Read Also: Severe Scalp Psoriasis Home Remedies
Also Check: Which Treatment Is Better For Psoriasis Homeopathy Or Allopathy
How Is Pustular Psoriasis Different
Pustular psoriasis looks different to plaque psoriasis, although plaque and pustular psoriasis can coexist or one may follow the other. The main distinguishing feature of pustular psoriasis is the appearance of pus spots surrounded by or on top of areas of red skin. This does not mean there is infection present. The spots simply show that the skin has been invaded by white blood cells. The person is not infected and neither are they contagious in any way.
Pustular psoriasis flare-ups can be triggered by some medicines, irritating substances on the skin, ultraviolet light overdoses, pregnancy, systemic steroids , infections or emotional stress.
> > > Best Psoriasis Cure Available
3. To help safeguard the skin, the immune system release chemicals that can cause nerves to itch and blood vessels to dilate to prepare the skin for a sudden rush of immune cells
4. When the immune cells arrive at the scene, most work to kill off the pathogens causing the distress, but a few capture some of the invaders and take them back to the heart of the immune system, where other soldier cells are produced in a way to recognize and attack the invading cells on contact
5. Inflammation is the bodys way of opening blood vessels to allow more soldier cells to rush to the battlefield.
While this entire process is completely normal, people with psoriasis tend to overproduce these soldier cells when the body feels threatened. This overabundance of killer immune cells can actually be dangerous to the skin since they begin to attack good cells along with the bad ones.
While it is great to finally understand the impact an improperly working immune system can have on your skin and cause psoriasis more research is needed to pinpoint the exact cause for the over-firing of the cell messages. What Is the Best Biologic for Pustular Psoriasis
Read Also: Narrow Band Uvb Light For Psoriasis
Establishing Treatment Goals In Gpp
Treatment goals in GPP are not well defined due to the rarity of the disease, its heterogeneous symptoms, and the lack of consistent treatment guidelines and therapeutic monitoring strategies. Clinically relevant treatment goals for GPP flares involve the cessation of pustulation and the resolution of erythema and edema. Several treatment goals can be proposed based on the recent advances in our understanding of disease pathogenesis and the development of novel, effective biologics . Proposed treatment goals can be divided into immediate and long term.
Fig. 2
Treatment goals in patients with GPP. GPP is a systemic disease with manifestations that affect several organs. Treatment goals should focus on improving skin-related symptoms and systemic inflammation. GPP generalized pustular psoriasis
How Was Tnf Defined As A Good Target For Therapy
TNF is an important host defence molecule. It helps protect from many stresses including intracellular infection. Hence, it was not considered by most immunologists or rheumatologists to be an important part of the pathogenesis of autoimmune disease. However, on the basis of the hypothesis of Marc Feldmann in 1983 , published with Franco Bottazzos group , and rapidly validated using Graves thyroid disease tissue, in 1985, Ravinder Maini and Marc Feldmann set about systematically exploring the role of cytokines in RA.
1983: a new hypothesis for autoimmunity .
This project was a natural collaboration, since both of us previously studied immune cell supernatants and were impressed by their potency. At the time, their molecular nature was unknown andwith the techniques available at the timeunknowable but the molecular biological revolution of the mid to late 1970s led to the cloning of cDNAs reflecting cytokine mRNAs and these tools permitted specific evaluation of cytokine production in diseased tissue sites. One of the most accessible tissue disease sites is the joints, just under the skin, and this facilitated our progress. Biopsies and larger operative samples and occasionally synovial fluid were available for research, and by miniaturization, it was possible to evaluate which pro-inflammatory cytokines were produced by cells in the RA joint as judged by their mRNA expression .
You May Like: How Effective Is Light Therapy For Psoriasis
Successful Treatment Of Refractory Palmoplantar Pustular Psoriasis With Apremilast: A Case Series
- 1Department of Dermatology, University of Lübeck, Lübeck, Germany
- 2Lübeck Institute of Experimental Dermatology, University of Lübeck, Lübeck, Germany
- 3Institute and Comprehensive Center for Inflammation Medicine, University of Lübeck, Lübeck, Germany
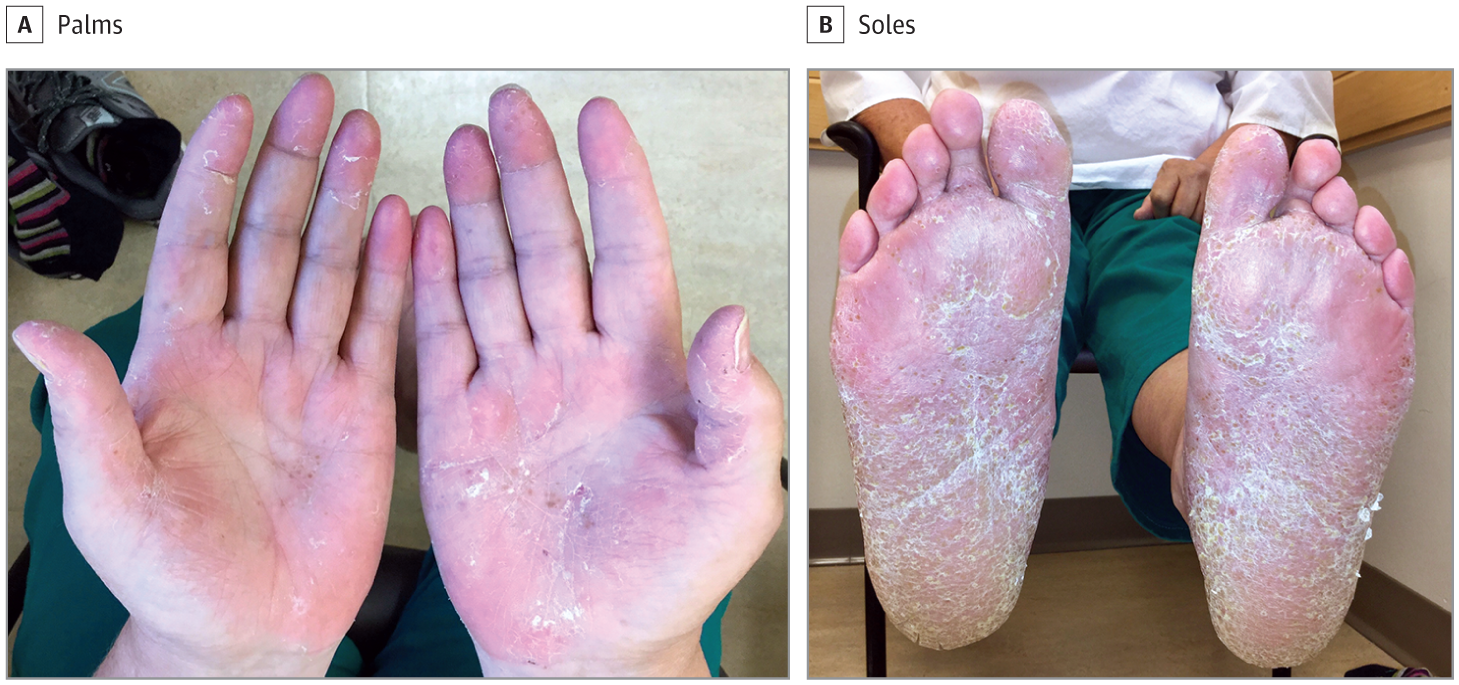
Introduction: Palmoplantar pustular psoriasis is a debilitating inflammatory skin disorder of the palms and soles that poses a high burden on affected patients. Satisfactory treatment response is rarely achieved using current treatment options, little is known about the potential benefit of the PDE4 inhibitor apremilast in the treatment of refractory PPPP patients. We aimed to evaluate the use of apremilast in PPPP patients.
Patients and Methods: Six patients, four with severe physician global assessment = 3 on a scale of 04 and two with very severe treatment-refractory PPPP , were included in this study. Five patients had concomitant psoriatic arthritis . Prior to apremilast administration, topical corticosteroids, psoralen-UVA and multiple systemic oral and biologic anti-inflammatory treatments were insufficient to improve their skin condition or had to be discontinued due to adverse events. Apremilast was commenced in all patients with clinical follow-up over 18 months.
Apremilast may be a promising treatment option for refractory and severely affected PPPP patients. Our observation, however, requires further validation.
What Are The Main Signs And Symptoms Of Ppp
The main sign of PPP is patches of very red or dark skin on the palms of the hands or soles of the feet, covered with small pustules. These pustules are filled with fluid which often gives them a yellow or cream colour, and they may dry up and turn brown or crusty after they have burst. The red or darkened skin around the pustules is often thick and flaky, and is often prone to cracking. Because of this, PPP can be painful, and can make walking or using the hands difficult.
As with other types of psoriasis, PPP can be anything from mild to severe, and can wax and wane.
Don’t Miss: Scalp Psoriasis Cause Hair Loss