What Causes Psoriasis And Psoriatic Arthritis
While no one knows the exact cause of psoriasis or PsA, experts believe that a faulty immune system is partly to blame. Specifically, the immune system attacks healthy skin cells and joints, causing the inflammation, swelling, and pain characteristic of psoriatic disease.
Genetics plays a part, too: Often will have other family members with psoriatic disease, says Dr. Haberman. In fact, roughly 40 percent of people with PsA have at least one close family member with psoriasis or psoriatic arthritis. Research is still ongoing, however, and its not clear whether having a family history of psoriasis alone increases PsA risk.
Obesity is also a common risk factor for people with psoriasis and PsA. According to a 2019 study in the journal Medicine, roughly 40 percent of people with psoriasis are obese. While it is unknown why obesity is so strongly linked to psoriatic diseases, we do know that obesity is associated with the production of inflammatory chemicals in the body, says Dr. Haberman. It may be that this underlying inflammatory environment helps predispose the body to the development of psoriasis and PsA, she says.
Other risk factors for psoriasis include:
- Family history
- Viral and bacterial infections
- Stress
- Obesity
- Smoking
- Alcohol consumption
Read more here about psoriatic arthritis risk factors.
Psoriasis And Psoriatic Arthritis: Pathophysiology Therapeutic Intervention And Complementary Medicine
ISBN |
What are VitalSource eBooks?
Routledge & CRC Press eBooks are available through VitalSource. The free VitalSource Bookshelf® application allows you to access to your eBooks whenever and wherever you choose.
- Mobile/eReaders Download the Bookshelf mobile app at VitalSource.com or from the iTunes or Android store to access your eBooks from your mobile device or eReader.
- Offline Computer Download Bookshelf software to your desktop so you can view your eBooks with or without Internet access.
- System requirements for Bookshelf for PC, Mac, IOS and Android etc.»
Most VitalSource eBooks are available in a reflowable EPUB format which allows you to resize text to suit you and enables other accessibility features. Where the content of the eBook requires a specific layout, or contains maths or other special characters, the eBook will be available in PDF format, which cannot be reflowed. For both formats the functionality available will depend on how you access the ebook .
Metabolic Syndrome And Heart Disease
Along with heart disease, psoriasis and PsA are associated with many comorbidities, including metabolic syndrome, inflammatory bowel disease, osteoporosis, fibromyalgia, and depression.
Some studies have shown that people with psoriasis have a particularly high prevalence of developing metabolic syndrome, which is a type of systemic inflammation associated with heart disease, along with obesity, hypertension, diabetes, liver disease, and high levels of fat in the bloodstream, all of which can increase your risk for cardiovascular disease. Risk factors for metabolic syndrome include:
- High blood sugar
- Belly fat and large waist
- Hypertension
Be sure you are getting regular blood tests to screen for metabolic syndrome, particularly if you have hypertension or a large waist circumference. People with psoriasis have a 22 percent to 98 percent higher risk of developing metabolic syndrome, depending on the severity of their psoriasis.
Also Check: Dosage Of Methotrexate For Psoriasis
Symptoms Of Psoriatic Arthritis
The severity of the condition can vary considerably from person to person. Some people may have severe problems affecting many joints, whereas others may only notice mild symptoms in 1 or 2 joints.
There may be times when your symptoms improve and periods when they get worse .
Relapses can be very difficult to predict, but can often be managed with medicine when they do occur.
If You Have Autoimmune Thyroid Disease
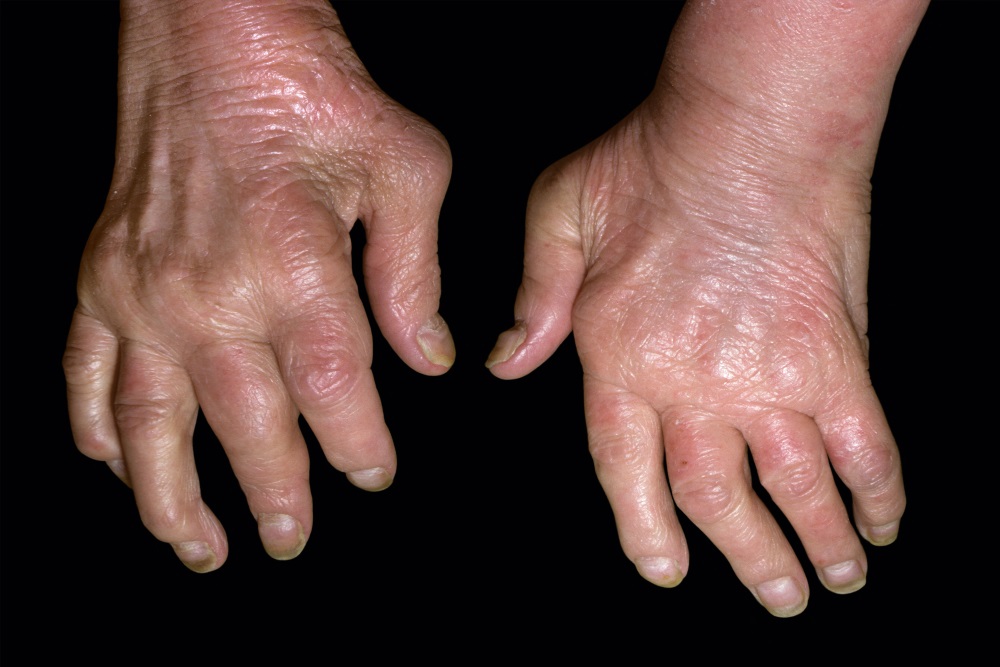
If you have Hashimotos thyroiditis or Graves disease, your risk of developing another autoimmune disease is increased. As a result, its important to become knowledgeable about the common signs and symptoms of other autoimmune conditions. These include fatigue, muscle and joint pain and/or swelling, digestive problems, dry eyes, brain fog and difficulty concentrating, and skin rashes. If you have symptoms that continue after optimal thyroid treatment, you should discuss them with your doctor.
Theres also a caution if you have Graves disease and are being treated with a beta blocker. While most Graves disease patients are not given beta blockers for extended periods, long-term beta blocker use is associated with a significantly increased risk of developing psoriasis.
You May Like: What Is Psoriasis Skin Condition
Psoriatic Arthritis Signs And Symptoms
Early symptoms with psoriatic arthritis are important. People will complain of pain and swelling in their joints hands, feet, wrists, etc. They may have a small patch of psoriasis or have psoriasis covering many areas of the body. There may be complaints of stiffness and fatigue. For example, studies in Toronto showed the year before they were diagnosed, people had reported joint pain, fatigue, and stiffness. Early in the disease, people will often have episodes of worsening of the psoriatic arthritis and then episodes of improvement.
When To Get Medical Advice
See a GP if you have persistent pain, swelling or stiffness in your joints even if you have not been diagnosed with psoriasis.
If you’ve been diagnosed with psoriasis, you should have check-ups at least once a year to monitor your condition. Make sure you let the doctor know if you’re experiencing any problems with your joints.
Read Also: Blue Star Ointment Good For Psoriasis
Enthesitis Treatments For People With Psoriatic Arthritis
Once your enthesitis has been diagnosed, its important that you start receiving right away to prevent permanent joint damage.
Enthesitis typically requires intense treatment courses because the condition is resistant to the disease-modifying antirheumatic drugs used to treat psoriasis. The approach your doctor recommends will usually depend on the severity of your condition. Some mild cases can even be handled with nonsteroidal anti-inflammatory drugs like Advil , but other cases may need biologics or steroids.
Classification Of Psoriatic Arthritis
The simple and highly specific Classification Criteria for Psoriatic Arthritis , developed by a large international study group, has a sensitivity and specificity of 98.7% and 91.4%, respectively. The criteria consist of established inflammatory articular disease with at least 3 points from the following features:
- Current psoriasis
- A history of psoriasis
- A family history of psoriasis
- Dactylitis
- Juxta-articular new-bone formation
- RF negativity
- Nail dystrophy
Read Also: Why Does Sunlight Help Psoriasis
Understanding Remission And Minimal Disease Activity
Psoriatic arthritis disease progression is not inevitable. When your PsA is treated with medications that reduce immune system overactivity, you can reduce your disease activity to a point that its no longer causing significant symptoms or increasing the risk of long-term health issues.
In general, going into remission means that you are no longer showing signs of active disease. Decades ago, remission wasnt conceivable for most people with psoriatic arthritis, but thanks to a proliferation in medication treatment options, getting to remission is a possibility for PsA patients today.
However, going into remission does not mean that you will stay there indefinitely. It is common for PsA symptoms to wax and wane. Even if youve been in remission for a long time and your pain starts coming back and you start flaring more, you may need to change your medication for better control, says Dr. Haberman.
You may also hear the phrase minimal disease activity in conjunction with psoriatic arthritis and remission.
Doctors dont have a clear definition of what it means to be in remission in PsA, but they have defined something called minimal disease activity as a treatment target. This is what your doctor may use to determine whether your PsA disease activity is low enough that you have few symptoms and a low risk of long-term damage.
People are considered to be in minimal disease activity when their scores on five out of these seven criteria are low enough.
How Do Psoriasis And Psa Overlap
For every 10 patients who walk in the door with psoriasis, about three or four of them will eventually get PsA, says Elaine Husni, MD, MPH, vice chair of the department of rheumatic & immunologic diseases at the Cleveland Clinic in Ohio. Most cases almost always start with the skin condition and then within seven to 10 years later, joint pain symptoms start to develop.
However, skin and joint symptoms can develop at the same time and, more rarely, joint symptoms can appear before skin involvement, says Dr. Haberman. While estimates vary, one study showed that up to 3 percent of patients developed joint disease before skin disease, she notes.
In some cases, there may have been skin involvement that went unnoticed or undiagnosed. For example, psoriasis can be sneaky and show up in hidden or private areas like the scalp, intergluteal cleft , belly button, and inside the ear, explains Dr. Husni. Since people dont really examine their scalp or buttocks very often, small psoriasis patches can get missed and delay diagnosis, she says.
Adds Dr. Haberman: You might have a small fleck in your scalp that you just think of as dandruff that is actually psoriasis.
Whats more, people with psoriasis in some of these hidden areas may actually be more prone to PsA. Studies have shown that you may be at higher risk of developing PsA if you have scalp, nail, or inverse psoriasis, says Dr. Haberman.
Read Also: How To Stop Itching From Scalp Psoriasis
How Psoriatic Arthritis Treatment Prevents Disease Progression
The primary way to slow the progression of PsA is through medications that modify the immune system. It may take trial and error to find the treatment that works best for a given patient, notes Dr. Haberman. While we have a lot of medication options for PsA, we dont know which ones a patient will respond to, so sometimes we need to try more than one medication to find the one thats right for that patient, she says.
In addition, medications that have been effective for you can stop working over time. If this happens, your doctor may recommend a medication that works differently say, targets a different part of the immune system to control disease activity.
There are many drugs used to treat PsA. The ones that you will use will depend on the type and severity of symptoms as well as the most problematic areas .
Medications use to treat PsA include:
Experts Arent Sure Why Psoriasis And Psoriatic Arthritis Are Linked
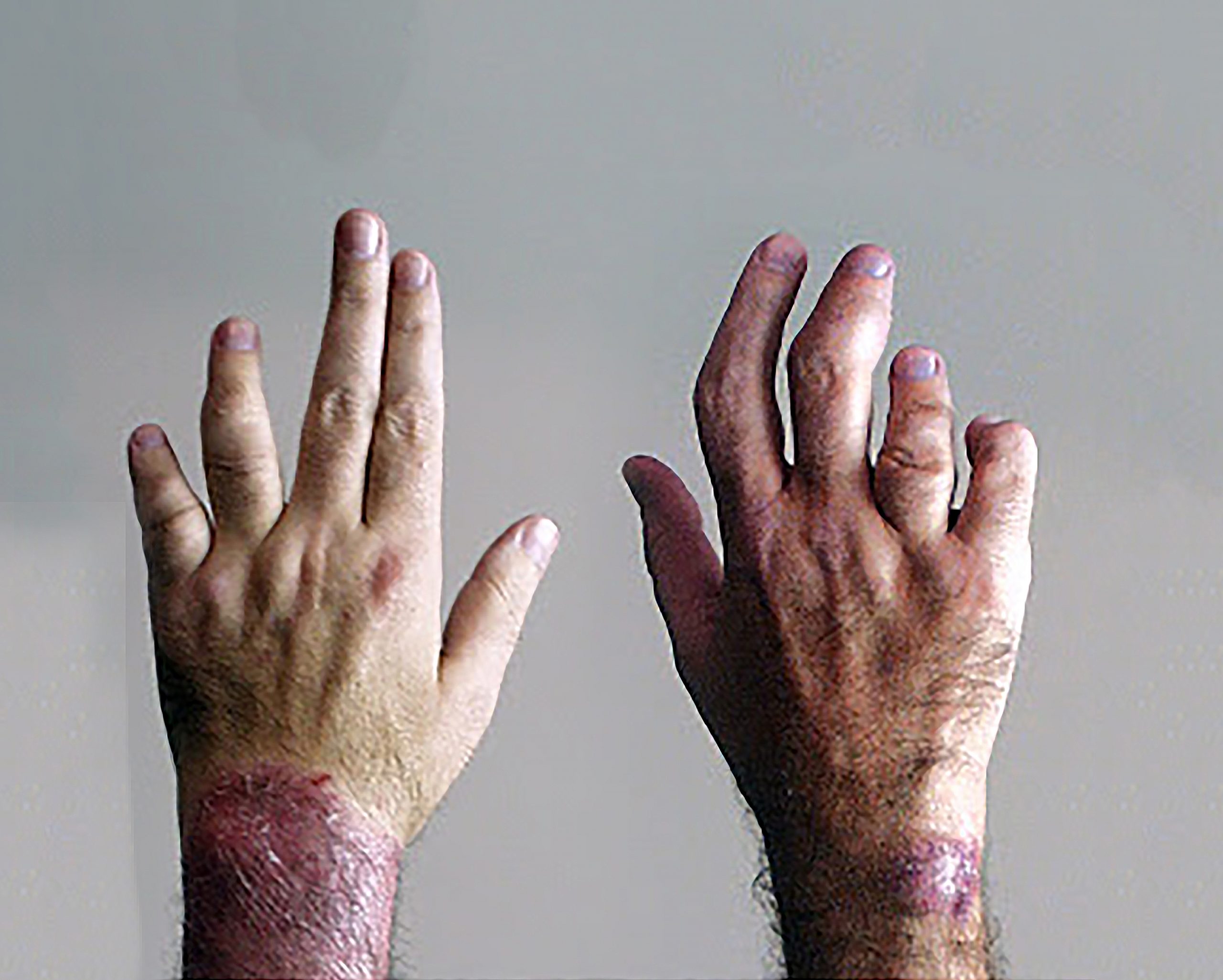
Psoriasis and psoriatic arthritis are clearly connected, but experts dont know why some people develop both conditions. However, genetics appears to be involved. Researchers have pinpointed a family of genes called the human leukocyte antigen complex as a possible contributor to psoriasis and psoriatic arthritis, according to the U.S. National Library of Medicine. People with psoriasis or psoriatic arthritis have HLA genes that are different from people who dont have either condition, according to a May 2021 paper published in The Journal of Rheumatology. And people with psoriasis who have a specific HLA gene mutation are more likely to develop psoriatic arthritis, according to the same paper.
Medical experts also believe that psoriatic arthritis may be inherited. About 40% of people with psoriatic arthritis have a family member with either psoriasis or psoriatic arthritis, according to the U.S. National Library of Medicine.
You May Like: Can Psoriasis Be A Symptom Of Something Else
Psoriasis And Psoriatic Arthritis Overview
Alan Menter, MDSupplements and Featured Publications
Psoriasis and psoriatic arthritis are chronic immune-mediated diseases that primarily affect the skin and joints, respectively these diseases are also associated with high rates of cardiovascular and other comorbidities. Despite over 40 genes proven to be related to the disease, the exact causes of psoriasis and PsA are still to be determined. Recent insights into the underlying pathophysiology of these diseases have revealed novel therapeutic targets. Effective management requires timely diagnosis and initiation of treatment. Yet, both psoriasis and PsA remain underrecognized and undertreated in current clinical practice. Recognizing the true physical, social, and emotional burden of psoriasis and PsA, as well as their associated comorbidities, is the first step to improving the prognosis for affected patients.
Am J Manag Care. 2016 22:S216-S224
PSORIASIS OVERVIEW
Psoriasis is a chronic, multifactorial, immune-mediated skin disease. The characteristic erythematous plaques of psoriasis are often painful and disfiguring, leading to a substantial decrease in quality of life.1 Cardiovascular disease , diabetes, and other autoimmune disorders are common among patients with psoriasis, contributing to the overall burden of disease and increasing healthcare
resource utilization.1
Epidemiology
Immunologic Mechanisms
Genetics of Psoriasis
Environmental triggers
Other immune-mediated diseases
Disease Classification
Mild
Loss Of Significant Joint Mobility
For example, you were able to flex your wrist 60 degrees, and two years later, you lost 50 percent of that range of motion. Its possible to feel okay and still experience loss of range of motion, says Dr. Domingues. But the idea is to prevent joint damage and to make you have less pain. If you have less pain and are still progressing, that means your treatment could be working better.
Don’t Miss: Can You Get Rid Of Psoriasis Forever
Past Research And Achievements In This Area
In 2015, research led by our centre for genetics and genomics at the University of Manchester identified genetic variants associated with psoriatic arthritis, but not with psoriasis or rheumatoid arthritis. This helped to establish psoriatic arthritis as a condition in its own right. The findings could lead to the development of drugs specifically for psoriatic arthritis.
Later in the same year, our TICOPA trial looked at the benefits of early aggressive drug treatment for people with psoriatic arthritis followed by an increase in drug dosage if initial treatment isnt working. The trial found that patients treated this way, required fewer hospital- and community-based services than patients receiving the standard care.
Symptoms Are Often Slow To Show
According to Dr. Fernandez, the majority of people whodevelop psoriatic arthritis have psoriasis first.
Up to 30 percent of people with psoriasis will develop PsA, but that can take an average of 10 to 12 years after the skin disease appears. It is not known exactly why the condition takes so long to appear, he says.
Recommended Reading: Will Losing Weight Help Psoriasis
How To Get The Right Arthritis Diagnosis
There is no single test for psoriatic arthritis, says Azar. Along with a physical exam, youll likely need a series of both imaging procedures and blood tests for a diagnosis, and to rule out other forms of arthritis, such as rheumatoid arthritis or gout.
Theres no one test to diagnose rheumatoid arthritis either, but, as with PsA, blood tests are part of the workup. The presence of autoantibodies in the bloodstream, either rheumatoid factor or cyclic citrullinated peptide antibodies, will suggest an RA diagnosis. These antibodies tend to be less typical in people with psoriatic arthritis, according to an article published in Rheumatic and Musculoskeletal Diseases in August 2018.
As part of the physical exam, the doctor will closely evaluate the affected joints. RA involves the joints in a symmetrical fashion, and often, when rheumatoid factor is very high, there may be nodules under the skin, Azar says. According to the National Rheumatoid Arthritis Society, 20 percent of patients with RA develop these firm lumps.
Psoriatic arthritis, on the other hand, can reveal itself in a variety of ways, affecting a large joint or a single small finger joint of the hand, says Azar.
Another notable difference between the two diseases is bone involvement. RA is characterized by bone loss or erosion near the joint, while PsA is marked by both bone erosion and new bone formation, Azar says. An X-ray or other imaging method can help reveal whats going on.
Psoriasis And Psoriatic Arthritis Treatments Can Make It Easier To Live A Full Life With These Conditions
There are no cures for either disease, but an effective treatment plan can minimize symptoms for both psoriasis and psoriatic arthritis. With psoriasis, doctors generally prescribe treatments that prevent your skin cells from growing too quickly, according to the Mayo Clinic. There are many treatment options for this, including creams, light therapy, or oral or injected medications, the Mayo Clinic explains.
As for psoriatic arthritis, treatments generally focus on controlling inflammation to minimize your joint pain and damage. Your doctor might suggest pharmacological options that target your immune system to lower inflammation, along with exercise or other lifestyle modifications, according to the Mayo Clinic. With each condition, the best treatment depends on your particular situation.
Don’t Miss: Glycerin And Witch Hazel For Psoriasis
Health Initiatives In Psoriasis And Psoriatic Arthritis Consortium European States
01 July 2021
Promoting Early Identification and Improving Outcomes in Psoriatic Arthritis
Psoriatic Arthritis affects at least 30% of people living with Psoriasis and is associated with an increased risk of other comorbidities.
The Health Initiatives in Psoriasis and Psoriatic Arthritis Consortium European States is a study initiative that will contribute greatly and efficiently to enhance the quality of life of persons living with Psoriatic Arthritis . Launched on 1st July 2021, this initiative is a collaboration between European research partners, pharmaceutical companies, SMEs and patient organizations.
The objectives of the HIPPOCRATES are to identify early patients at risk of progression to PsA in order to enable early intervention to prevent the development of PSA. In addition, the initiative aims to define factors that can predict bone/joint damages early. This would support the development of more adapted and personalized treatment strategies with optimized outcomes.
The project includes an integrated approach of patient involvement in the overall consortium with active consultation with people living with Psoriatic disease. Three patient organizations are taking part in the consortium as collaborative or associated partners these include: Group for Research and Assessment of Psoriasis and Psoriatic Arthritis , PARE – EULAR, and EUROPSO led by Europso president, Jan Koren David Trigos and Lars Werner